In this article, you will gain a deeper understanding of hyperglycemic medications and their importance in managing diabetes. Whether you or a loved one are affected by this condition, it is crucial to comprehend these medications and their role in controlling blood sugar levels. From oral medications to injectables, we will explore the various types of hyperglycemic medications and their benefits in helping individuals lead a healthier and more balanced life. So, let’s dive into the world of hyperglycemic medications and equip ourselves with knowledge that can make a positive impact on our well-being.
Understanding Hyperglycemic Medications
If you have been diagnosed with diabetes or pre-diabetes, you may have been prescribed hyperglycemic medications to help manage your condition. These medications are vital for controlling blood glucose levels and preventing complications associated with high blood sugar. In this article, we will dive into the world of hyperglycemic medications, exploring the different types of oral medications, insulin therapies, their administration, monitoring blood glucose levels, managing side effects and risks, incorporating lifestyle changes, and choosing the right medication for your unique needs.

Oral Medications
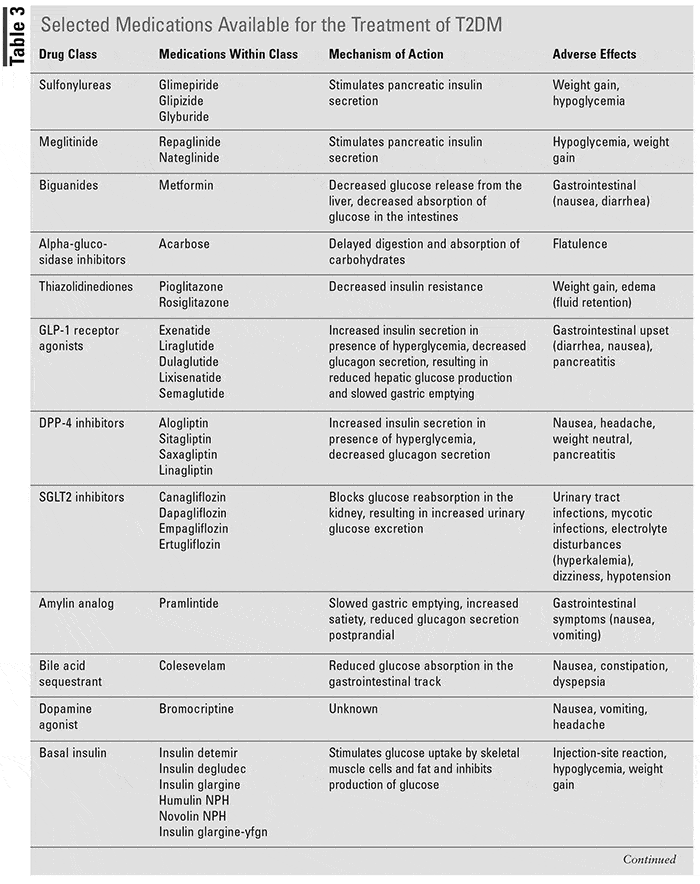
Oral hyperglycemic medications are commonly prescribed for individuals with type 2 diabetes. These medications work by helping the body use insulin more effectively or by stimulating the pancreas to produce more insulin. There are several classes of oral medications, each with its unique mode of action. Some common classes include sulfonylureas, biguanides, meglitinides, thiazolidinediones, DPP-4 inhibitors, and SGLT-2 inhibitors.
Sulfonylureas and meglitinides help stimulate insulin secretion from the pancreas, while biguanides like metformin reduce glucose production in the liver, increase insulin sensitivity, and decrease sugar absorption in the intestines. Thiazolidinediones improve insulin sensitivity in the body’s cells. DPP-4 inhibitors and SGLT-2 inhibitors have different mechanisms of action, targeting specific enzymes or transporters involved in glucose regulation.
Insulin Therapies
For individuals with type 1 diabetes or more advanced cases of type 2 diabetes, insulin therapy is necessary. Insulin is a hormone that allows the body’s cells to take in glucose, thus lowering blood sugar levels. There are various types of insulin, classified based on their onset, peak, and duration of action. Rapid-acting insulin starts working within minutes, peaks in about an hour, and lasts for a few hours. Short-acting insulin typically takes effect within 30 minutes, peaks in 2-3 hours, and lasts for around 5-8 hours. Intermediate-acting insulin has a slower onset, peaks around 4-12 hours, and lasts for up to 24 hours. Long-acting insulin has a slow and steady release, providing a basal level of insulin for a more extended period.
Insulin therapy can be delivered through multiple methods, including traditional injections using a syringe, insulin pens, and insulin pumps. The choice of insulin type and delivery method depends on various factors, such as individual preference, lifestyle, and blood glucose control goals. Your healthcare provider will work with you to determine the most suitable insulin therapy for your needs.

Medication Administration
Proper medication administration is crucial for ensuring the efficacy of hyperglycemic medications. If you are on oral medications, it is important to take them as prescribed by your healthcare provider. Some medications may need to be taken with food, while others should be taken on an empty stomach. It is essential to follow these instructions to maximize their effectiveness.
For individuals on insulin therapy, precise insulin administration is essential. Your healthcare provider will guide you on the necessary steps to measure and inject insulin accurately. It is crucial to rotate injection sites to prevent lipohypertrophy or the buildup of fatty tissue. Additionally, regular follow-ups with your healthcare provider will help fine-tune your insulin regimen and ensure optimal blood glucose control.
Side Effects and Risks
Like any medication, hyperglycemic medications can have side effects and associated risks. Common side effects of oral medications include gastrointestinal issues like nausea, upset stomach, diarrhea, and a metallic taste in the mouth. These side effects are usually temporary and diminish as your body adjusts to the medication. However, if they persist or worsen, it is important to consult your healthcare provider.
Insulin therapy can also have side effects, such as hypoglycemia (low blood sugar) or injection-site reactions like redness, itching, or swelling. It is important to be aware of the signs and symptoms of hypoglycemia, such as shakiness, dizziness, sweating, confusion, and rapid heartbeat. Prompt treatment with glucose or a fast-acting carbohydrate is essential to raise blood sugar levels quickly.
Monitoring Blood Glucose Levels
Regular monitoring of blood glucose levels is essential for effective diabetes management. This helps you understand how well your medications are working and allows you to make necessary adjustments in consultation with your healthcare provider. Monitoring can be done using a blood glucose meter, which measures blood sugar levels from a small drop of blood obtained by pricking your fingertip. Continuous glucose monitoring (CGM) systems are also available, providing real-time data on blood glucose levels throughout the day.
Maintaining a blood glucose log can be helpful in identifying patterns and trends in your blood sugar levels, making it easier to adjust your medications and make lifestyle changes accordingly. Consistent monitoring and communication with your healthcare provider are key to achieving optimal blood glucose control.
Combination Therapies
In some cases, individuals may require a combination of oral medications or a combination of oral medications and insulin therapy to achieve adequate blood glucose control. Combination therapies allow for a more customized approach tailored to individual needs. Your healthcare provider will assess your specific situation and create a treatment plan that may include multiple medications or a combination of medications and insulin.
Combination therapies should always be discussed with your healthcare provider. They will guide you on the appropriate dosage, timing, and potential side effects of each medication. It is important to understand how these medications may interact and work together to manage your blood glucose effectively.

Hypoglycemia Management
Hypoglycemia, or low blood sugar, can occur as a side effect of hyperglycemic medications, particularly insulin. It is crucial to be prepared and know how to manage hypoglycemia. Always keep a source of fast-acting carbohydrates, such as glucose tablets, fruit juice, or hard candy, readily available. If you experience symptoms of hypoglycemia, it is important to act promptly by consuming these carbohydrates to raise your blood sugar back to normal levels.
It is also important to inform your loved ones, friends, and colleagues about your condition and how they can assist you in case of a severe hypoglycemic episode. Wearing a medical identification bracelet or necklace can provide crucial information to emergency responders in case of an emergency.
Lifestyle Changes
Alongside medication, making certain lifestyle changes is essential for effective diabetes management. Regular physical activity, a healthy diet, managing stress, and getting enough sleep are all factors that can positively impact blood glucose control.
Engaging in regular exercise, such as brisk walking, swimming, cycling, or strength training, can help improve insulin sensitivity and lower blood sugar levels. A balanced diet that includes a variety of fruits, vegetables, whole grains, lean proteins, and healthy fats can contribute to overall health and better blood glucose control. Managing stress through relaxation techniques such as deep breathing exercises, meditation, or engaging in hobbies can also help maintain stable blood sugar levels. Lastly, ensuring adequate sleep is vital, as sleep deprivation can affect insulin sensitivity and lead to increased blood sugar levels.
Choosing the Right Medication
When it comes to choosing the right hyperglycemic medication, there are several factors to consider. Your healthcare provider will assess your medical history, overall health, blood glucose levels, and individual preferences to determine the most appropriate medication for you. Factors such as the medication’s effectiveness, safety, potential side effects, cost, and ease of administration will all be taken into account.
It is important to have open and honest communication with your healthcare provider, discussing any concerns or questions you may have about your medication. They are there to support you on your diabetes management journey and find the optimal treatment plan for your unique situation.
Conclusion
Hyperglycemic medications play a vital role in managing and controlling blood glucose levels for individuals with diabetes. Whether it be oral medications or insulin therapies, proper administration, monitoring, and lifestyle changes are all essential for effective diabetes management. By working closely with your healthcare provider, staying informed, and actively participating in your treatment plan, you can achieve optimal blood glucose control and lead a healthier, happier life. Remember, you are not alone in this journey, and your healthcare team is here to support you every step of the way.
