Have you ever wondered how the influenza virus affects humans and what makes it capable of causing a pandemic? This article aims to provide a comprehensive understanding of the influenza virus and its impact on our bodies. By exploring the various strains, transmission methods, and potential consequences for human health, we can gain valuable insights into tackling this global health challenge. Join us as we delve into the fascinating world of the influenza virus and uncover the key factors behind its ability to cause widespread illness.
What is Influenza?
Definition of influenza
Influenza, commonly known as the flu, is a contagious respiratory illness caused by the influenza virus. It affects the nose, throat, and sometimes the lungs. Influenza can range from mild to severe and can even lead to hospitalization or death in severe cases.
An overview of the influenza virus
The influenza virus belongs to the Orthomyxoviridae family. There are four types of influenza viruses: influenza A, B, C, and D. Influenza A and B viruses are the most common ones that cause seasonal flu outbreaks in humans. Influenza C viruses usually cause mild respiratory infections, while influenza D viruses primarily affect cattle.
Types of influenza viruses
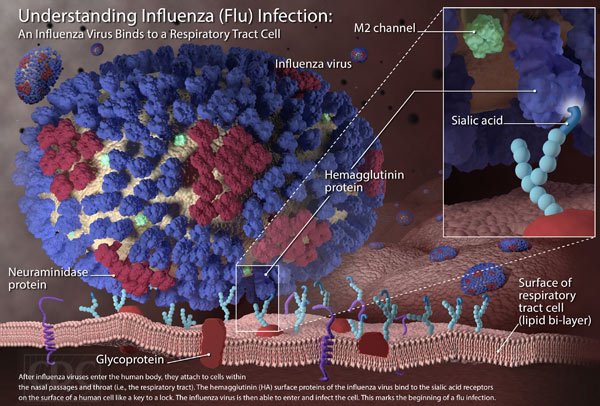
Influenza A viruses are further categorized based on two proteins on the surface of the virus: hemagglutinin (H) and neuraminidase (N). There are numerous subtypes of influenza A viruses, with the most common subtypes responsible for human infections being H1N1 and H3N2. Influenza B viruses, on the other hand, do not have subtypes but are classified into two lineages: B/Yamagata and B/Victoria.
Transmission of Influenza
How influenza spreads
Influenza spreads from person to person through respiratory droplets when an infected individual coughs, sneezes, or talks. These droplets can land in the mouths or noses of people nearby or be inhaled into the lungs. It is also possible to contract the flu by touching surfaces or objects contaminated with the virus and then touching one’s mouth, eyes, or nose.
Common modes of transmission
The most common modes of influenza transmission occur in crowded places such as schools, workplaces, and public transportation where people come into close contact. Additionally, influenza can spread within households, especially when preventive measures like hand hygiene and respiratory etiquette are not practiced consistently.
Factors that contribute to the spread of influenza
Several factors contribute to the spread of influenza. The virus can rapidly spread within communities due to its high infectivity and the ease with which it can be transmitted through close contact. Seasonal variations, such as the winter season when people spend more time indoors, also contribute to the increased transmission of influenza.

Symptoms of Influenza
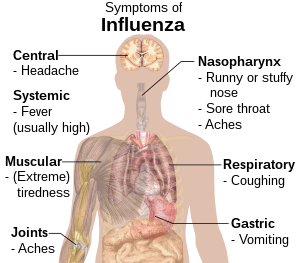
Common symptoms of influenza
Influenza symptoms typically include fever, cough, sore throat, runny or stuffy nose, body aches, headache, fatigue, and sometimes vomiting or diarrhea. These symptoms usually appear suddenly and can vary in severity depending on the individual.
Differences between influenza and common cold
Influenza symptoms can be similar to those of the common cold, but there are some distinguishing characteristics. Influenza symptoms tend to be more severe and have a rapid onset, whereas cold symptoms develop gradually. Additionally, influenza often involves a high fever, body aches, and extreme fatigue, which are less common with a common cold.
Potential complications of influenza
Influenza can lead to various complications, particularly in vulnerable populations such as older adults, young children, pregnant women, and individuals with underlying health conditions. These complications can include pneumonia, bronchitis, sinus infections, ear infections, and worsening of existing chronic conditions.
Diagnosis and Testing
Methods for diagnosing influenza
Influenza can be diagnosed based on the patient’s symptoms and physical examination by a healthcare professional. However, these methods alone may not provide a definitive diagnosis, as other respiratory viruses can cause similar symptoms. Laboratory testing is often necessary to confirm the presence of the influenza virus.
Medical tests used for influenza detection
The most common test used for influenza detection is the rapid influenza diagnostic test (RIDT). This test detects the presence of influenza antigens and provides results within a short period, usually within 15-30 minutes. In cases where a more accurate diagnosis is required, molecular tests like polymerase chain reaction (PCR) tests are performed to directly detect the genetic material of the influenza virus.
Challenges in diagnosing influenza
Diagnosing influenza can be challenging due to the overlapping symptoms with other respiratory viral infections. Rapid diagnostic tests may not always be accurate, and false negatives or positives can occur. Additionally, access to diagnostic testing may vary depending on healthcare settings, leading to potential delays in diagnosis and treatment.
Treatment Options for Influenza
Antiviral medications for influenza
Antiviral medications play a crucial role in the treatment of influenza, especially for individuals at high risk of complications or those with severe illness. The most commonly prescribed antiviral drugs for influenza include oseltamivir (Tamiflu), zanamivir (Relenza), and peramivir (Rapivab). These drugs can help reduce the severity and duration of influenza symptoms if initiated early.
Home remedies and symptom management
In addition to antiviral medications, several home remedies and self-care measures can help manage symptoms and promote recovery from influenza. These include getting plenty of rest, staying hydrated, using over-the-counter pain relievers, and using a humidifier or saline nasal spray to relieve nasal congestion.
Prevention measures during influenza outbreak
Preventing the spread of influenza is essential to protect yourself and others. During an outbreak, it is crucial to practice good hand hygiene by washing hands frequently with soap and water or using hand sanitizer. Covering your mouth and nose with a tissue or your elbow when coughing or sneezing can also help prevent the spread of the virus. Additionally, staying home when you are sick can prevent the transmission of influenza to others.
Vaccination against Influenza
Importance of influenza vaccination
Influenza vaccination is the most effective way to prevent influenza and its complications. Vaccination helps reduce the risk of getting infected, decreases the severity of illness if infection does occur, and lowers the chance of hospitalization or death due to influenza complications. It also plays a crucial role in minimizing the spread of the virus in communities.
Efficiency and effectiveness of influenza vaccines
The efficiency and effectiveness of influenza vaccines can vary depending on factors such as the match between the circulating strains and the vaccine strains, the age and health of individuals, and other environmental factors. On average, influenza vaccines have been shown to reduce the risk of influenza illness by 40-60% in the overall population.
Types of influenza vaccines available
There are several types of influenza vaccines available, including inactivated influenza vaccines (IIVs), recombinant vaccines, live attenuated influenza vaccines (LAIVs), and adjuvanted vaccines. The recommended vaccine types can vary by age group, health conditions, and individual preferences. The annual seasonal influenza vaccine is usually updated to include the strains predicted to circulate during the upcoming flu season.
Influenza and Public Health
Impact of influenza on public health
Influenza has a significant impact on public health globally. It causes substantial morbidity and mortality each year, leading to hospitalizations, loss of productivity, and economic burden. Influenza-related complications can strain healthcare systems, particularly during severe flu seasons or pandemics.
The role of public health measures in influenza control
Public health measures play a crucial role in controlling the spread of influenza. These measures include surveillance and monitoring of influenza activity, promoting vaccination programs, implementing infection prevention and control measures in healthcare settings, and providing public education on preventive measures such as hand hygiene and respiratory etiquette.
Vaccination campaigns and strategies
To maximize the impact of influenza vaccination, public health agencies often conduct vaccination campaigns targeting different populations, such as healthcare workers, older adults, and individuals with underlying health conditions. Strategies may include mass vaccination clinics, workplace vaccination programs, and outreach efforts to ensure access to vaccines for underserved communities.
Risk Groups and Vulnerable Populations
Groups at high risk of severe influenza infection
Certain groups are at higher risk of developing severe influenza infections and experiencing complications. These include young children (especially those younger than 2 years old), adults over the age of 65, pregnant women, individuals with chronic medical conditions (such as asthma, diabetes, or heart disease), and individuals with compromised immune systems.
Special considerations for pregnant women, older adults, and children
Pregnant women, older adults, and children are particularly vulnerable to complications from influenza. Pregnant women are at an increased risk of severe illness and adverse pregnancy outcomes, while older adults may have weakened immune systems that make it harder to fight off the virus. Children, especially those under 5 years old, are more susceptible to influenza and its complications.
Healthcare workers and influenza prevention
Healthcare workers play a crucial role in preventing the spread of influenza. Vaccination is strongly recommended for healthcare workers to protect both themselves and the patients they care for. Additionally, adherence to infection prevention and control practices, such as wearing personal protective equipment, practicing hand hygiene, and staying home when sick, is essential to minimize the risk of transmission in healthcare settings.

Historical Influenza Pandemics
Overview of past influenza pandemics
Throughout history, the world has experienced several severe influenza pandemics. The most notable ones include the 1918 Spanish flu pandemic, the 1957 Asian flu pandemic, the 1968 Hong Kong flu pandemic, and the 2009 H1N1 pandemic. These pandemics resulted in significant morbidity, mortality, and societal disruptions.
Lessons learned from historical pandemics
Historical influenza pandemics have taught us valuable lessons about the importance of preparedness, surveillance, and rapid response. They have highlighted the need for effective communication, early detection of emerging strains, and the development of vaccines and antiviral medications to mitigate the impact of future pandemics.
Comparison between seasonal influenza and pandemics
Seasonal influenza outbreaks occur annually and are caused by different strains of the virus. They usually result in milder illness and affect a significant portion of the population. In contrast, influenza pandemics involve the global spread of a new influenza virus strain to which a large proportion of the population has little or no pre-existing immunity. Pandemics can result in more severe illness and have the potential to cause high mortality rates.
Current and Future Challenges
Evolving nature of influenza viruses
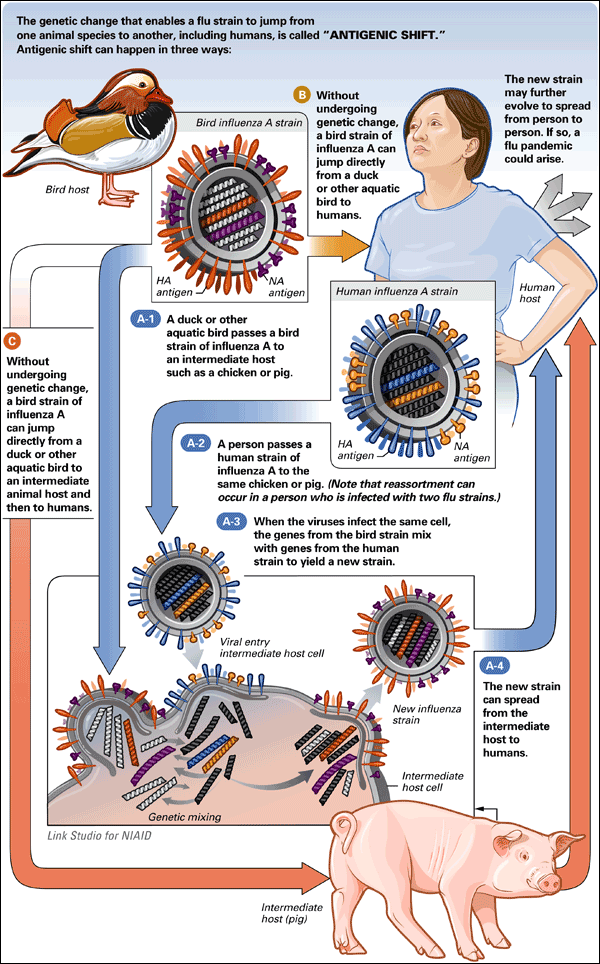
Influenza viruses are constantly evolving, undergoing genetic changes through antigenic drift and antigenic shift. Antigenic drift refers to small changes that accumulate over time, allowing the virus to evade prior immunity and causing seasonal influenza outbreaks. Antigenic shift, on the other hand, occurs when two or more influenza viruses combine their genetic material, leading to the emergence of a novel strain and potentially causing a pandemic.
Global surveillance and monitoring efforts
To tackle the challenges posed by the evolving nature of influenza viruses, global surveillance and monitoring efforts are essential. These efforts involve monitoring the genetic characteristics of circulating influenza strains, tracking influenza activity in different regions, and sharing data and information among international health organizations to inform vaccine development and public health strategies.
Anticipating the next influenza pandemic
Anticipating the next influenza pandemic is a crucial aspect of preparedness. Ongoing research, surveillance, and international collaboration are needed to identify potential pandemic strains, develop vaccines, and implement measures to mitigate the impact. Enhanced public health measures and improved vaccine manufacturing technologies will play a vital role in preventing and responding to future pandemics.
Understanding the Influenza Virus and Its Effects on Humans, Influenza in Human Pandemic