If you or someone you know is considering a lung transplant, it’s important to have a clear understanding of the process. From the initial evaluation to the post-transplant follow-up care, this article will guide you through the various stages of a lung transplant. We’ll explore the criteria for eligibility, the waiting list, the surgical procedure, and the recovery period. Whether you’re seeking information for yourself or supporting a loved one, this article aims to provide a friendly and informative overview of the lung transplant process.
Understanding the Lung Transplant Process

Overview of Lung Transplant
Lung transplantation is a complex surgical procedure that involves replacing a diseased or failing lung with a healthy lung from a donor. This procedure is typically performed on individuals who have advanced lung diseases that cannot be effectively treated with other medical interventions. Lung transplant offers the possibility of improving the quality of life and extending the lifespan of individuals with severe lung diseases.
Eligibility Criteria for Lung Transplant
Before undergoing a lung transplant, candidates must meet certain eligibility criteria. These criteria take into account various factors to ensure the success of the procedure and the overall well-being of the recipient. Some of the key eligibility criteria include age and general health, underlying lung disease, psychological and social factors, absence of active infection or cancer, and commitment to post-transplant care. A thorough evaluation is conducted to determine if a patient meets these criteria.

Evaluation and Pre-transplant Assessment
The evaluation process for a lung transplant involves a series of medical tests, evaluations, and consultations. The initial consultation provides an opportunity for the transplant team to gather detailed medical history and discuss the potential risks and benefits of the procedure. Medical tests, such as pulmonary function tests, chest imaging, and blood work, are conducted to assess the severity of the lung disease and the overall health of the patient. There is also a psychological and social evaluation to ensure the patient’s ability to cope with the demands of the transplant process. Additionally, a financial assessment is conducted to assess insurance coverage and identify any potential financial barriers.
Organ Procurement and Waiting List
Organ procurement is a crucial step in the lung transplant process. Donor organs can come from deceased individuals who have consented to organ donation or from living donors in the case of lobar lung transplantation. The availability of donor organs depends on the number of registered donors and the allocation system in place. Once a patient is deemed eligible for a lung transplant, they are placed on a waiting list based on the severity of their disease and other priority factors. The waiting time can vary significantly, depending on the availability of suitable organs and the urgency of the patient’s condition.

The Transplant Surgery
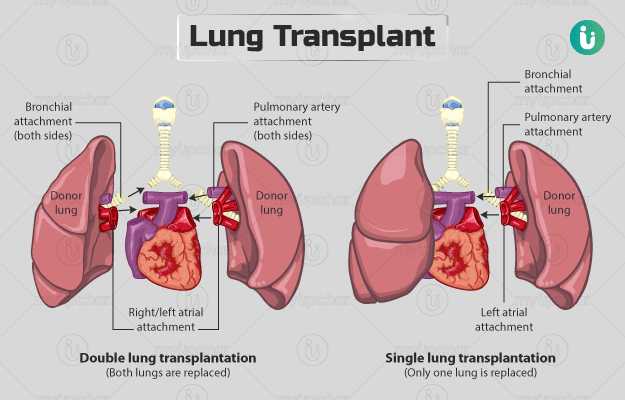
The lung transplant surgery is performed under general anesthesia. The preoperative preparation involves ensuring the patient is in optimal health for the procedure. During the surgery, the surgeon removes the diseased lung and replaces it with a healthy donor lung. The complexity and duration of the surgery depend on various factors, such as whether it is a bilateral or single lung transplant and the condition of the patient’s organs. In some cases, the use of extracorporeal membrane oxygenation (ECMO) may be necessary to support the patient’s lungs before, during, or after the transplant surgery.
Post-transplant Care and Recovery
Following a lung transplant, patients require intensive care and monitoring in the hospital’s intensive care unit (ICU). They may require ventilator support initially to help them breathe until the transplanted lung begins functioning properly. Immunosuppressive medications are initiated to prevent rejection of the transplanted organ. Regular monitoring and infection prevention measures are implemented to identify and manage any potential complications. Rehabilitation and physical therapy are crucial aspects of post-transplant care to aid in the recovery process. Psychological support is also provided to assist patients in adjusting to their new life with a transplanted lung.
Complications and Risks
Despite significant advancements in lung transplantation, complications and risks can still occur. The most common complication is rejection of the transplanted lung, which occurs when the recipient’s immune system recognizes the new organ as foreign and attacks it. Infections and pulmonary complications are also common due to the immunosuppressive medications used to prevent rejection. Graft failure and bronchiolitis obliterans syndrome, a condition characterized by the narrowing of the small airways, are potential long-term risks. Additionally, side effects of immunosuppressive medications and cardiovascular and renal complications should be closely monitored.
Immunosuppression and Anti-rejection Medications
To prevent rejection of the transplanted lung, patients are required to take immunosuppressive medications for the rest of their lives. These medications work by suppressing the immune system’s response to reduce the risk of rejection. Various types of immunosuppressive medications are used, including corticosteroids, calcineurin inhibitors, and antimetabolites. The specific drug regimen is tailored to each patient’s needs and may be adjusted over time. Regular monitoring of drug levels and potential side effects is essential to ensure the medication is effective and well-tolerated.

Follow-up and Long-term Care
Following a successful lung transplant, patients require lifelong follow-up and care. Regular visits to the transplant center are necessary to monitor the function of the transplanted lung, assess medication levels, and detect any signs of rejection or complications. Routine screenings for cancer and infections are conducted as part of long-term care. It is essential for patients to maintain a healthy lifestyle, adhere to medication schedules, and report any changes in their health to their healthcare team promptly. Long-term care is vital for ensuring the longevity of the transplanted lung and the overall well-being of the patient.
Ethical Considerations in Lung Transplantation
Lung transplantation raises various ethical considerations, particularly regarding organ allocation and fairness. The limited availability of donor organs necessitates the development of allocation systems that prioritize patients based on urgency and medical need. Ethical dilemmas may also arise when deciding whether a patient is a suitable candidate for transplantation. Informed consent is crucial in lung transplantation, particularly regarding the potential risks, benefits, and alternatives to the procedure. End-of-life care decisions may also need to be made if a patient’s condition deteriorates. Additionally, the relationship between the organ donor and recipient, and the emotional impact on both parties, raises important ethical considerations.
In conclusion, lung transplantation is a complex process that involves eligibility assessments, evaluations, organ procurement, surgery, and ongoing care. It offers hope for individuals with severe lung diseases, but it also presents risks and challenges. Understanding the lung transplant process is crucial for patients considering transplantation and their families. By being well-informed and actively participating in their care, individuals can navigate the transplantation journey with confidence and achieve the best possible outcomes.