You may have heard of insulin resistance, a condition that affects the body’s ability to respond to the hormone insulin. But what exactly are the risk factors associated with insulin resistance, and how can you take precautions to prevent it? In this article, we will explore the various factors that can increase your chances of developing insulin resistance, and provide practical steps you can take to protect yourself from this potentially serious health condition. So, let’s delve into the world of insulin resistance and arm ourselves with knowledge and precautionary measures to maintain a healthy and balanced lifestyle.

Risk Factors for Insulin Resistance
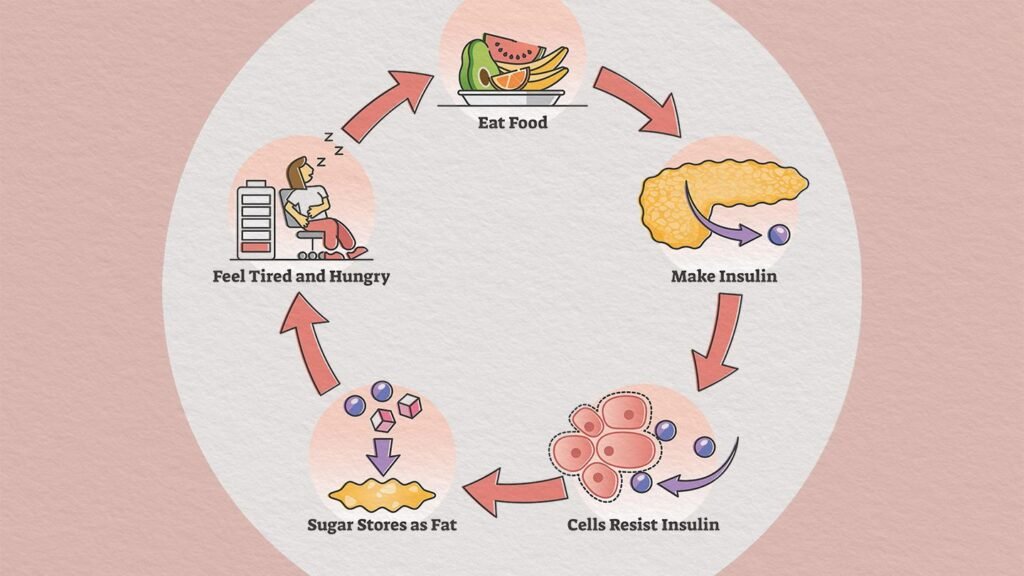
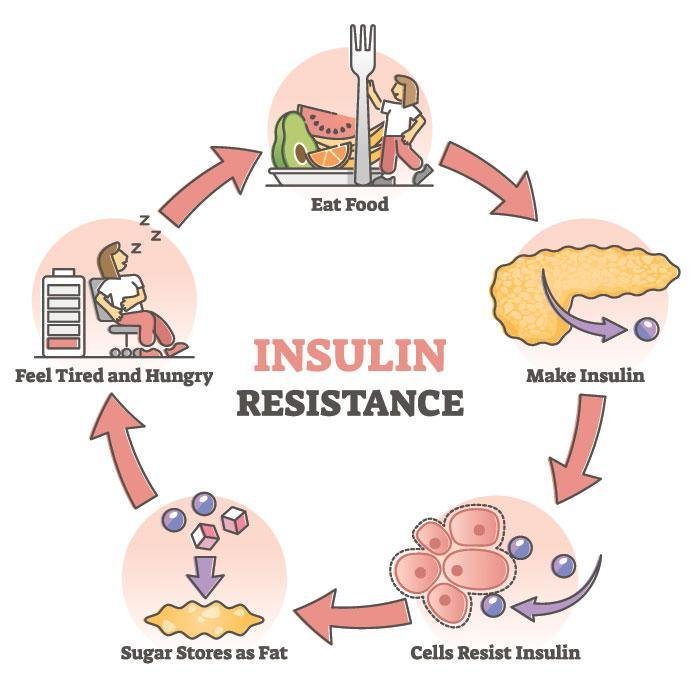
Insulin resistance is a condition in which the body’s cells become resistant to the effects of insulin, resulting in elevated blood sugar levels. It is a precursor to type 2 diabetes and can increase the risk of developing various other health issues. While there is no single cause for insulin resistance, there are several risk factors that can contribute to its development. By understanding these risk factors, you can take necessary precautions to reduce your chances of developing insulin resistance and its associated complications. Let’s explore some of the key risk factors in detail.
Obesity
Obesity is a major risk factor for insulin resistance. Excessive accumulation of body fat, especially around the abdominal area, can disrupt insulin function. Individuals with obesity often have higher levels of free fatty acids in their blood, which interfere with insulin’s ability to regulate blood sugar levels. Body Mass Index (BMI) and abdominal obesity are two important parameters used to assess the risk of insulin resistance associated with obesity.
BMI is a measure of body fat based on height and weight. A BMI of 30 or higher is considered obese, and individuals falling into this category are at a greater risk of developing insulin resistance. Additionally, abdominal obesity, characterized by excess fat around the waistline, is particularly detrimental in terms of insulin resistance. The accumulation of visceral fat in the abdominal area promotes inflammation and the release of inflammatory molecules, which further worsen insulin resistance.

Family History
Your family history plays a significant role in determining your risk of developing insulin resistance. If one or both of your parents have type 2 diabetes or insulin resistance, you are more likely to develop these conditions yourself. This is partly due to genetic factors, as certain genes can influence how your body processes and responds to insulin. However, it’s essential to remember that genetics are not the sole determining factor, and lifestyle choices can also influence the development of insulin resistance.
Having a family history of insulin resistance or type 2 diabetes should serve as a reminder to be proactive in adopting a healthy lifestyle. By maintaining a healthy weight, eating a balanced diet, and engaging in regular physical activity, you can mitigate the impact of genetic predispositions.
Physical Inactivity
Leading a sedentary lifestyle is strongly associated with insulin resistance. Lack of exercise and prolonged periods of sitting or inactivity can contribute to insulin resistance over time. Physical activity helps to improve insulin sensitivity and aids in maintaining a healthy weight. When you engage in regular exercise, your muscles use glucose as fuel, which helps to regulate blood sugar levels and reduce the strain on insulin-producing cells.
You don’t need to become a professional athlete to combat insulin resistance. Simple lifestyle changes such as walking, cycling, or participating in any form of physical activity for at least 150 minutes per week can make a significant difference. Incorporating exercise into your daily routine, such as taking the stairs instead of the elevator or going for a brisk walk during your lunch break, can also help counteract the effects of physical inactivity.
Unhealthy Diet
A poor diet can have a significant impact on your risk of developing insulin resistance. Consuming an excessive amount of sugar, fat, and lacking fiber in your diet can contribute to weight gain and disrupt insulin function. High sugar intake, especially from sugary beverages and processed foods, leads to rapid spikes in blood sugar levels, putting a strain on the body’s insulin response.
Similarly, a diet rich in unhealthy fats, such as saturated and trans fats, can promote insulin resistance. These fats contribute to inflammation and interfere with insulin signaling pathways. On the other hand, a diet low in fiber reduces satiety and can lead to overeating, weight gain, and insulin dysregulation.
To reduce your risk of developing insulin resistance, focus on consuming a well-balanced diet rich in whole grains, lean proteins, fruits, vegetables, and healthy fats. Limit your intake of sugary and processed foods, opt for healthier cooking methods such as baking, grilling, or steaming, and choose complex carbohydrates over refined ones.
Age
Age is an inevitable risk factor for insulin resistance. As we get older, our body’s ability to produce and utilize insulin becomes less efficient. This is attributed to natural changes that occur with aging, such as decreased muscle mass, increased fat mass, and alterations in hormone levels. Middle-aged or older adults are more likely to develop insulin resistance compared to younger individuals.
However, aging doesn’t mean you’re destined to develop insulin resistance. By adopting a healthy lifestyle early on and addressing any other risk factors you may have, you can significantly reduce the impact of aging on insulin function. Regular exercise, a balanced diet, and maintaining a healthy weight are particularly crucial for older adults to manage and prevent insulin resistance.
Polycystic Ovary Syndrome (PCOS)
Polycystic ovary syndrome (PCOS) is a hormonal disorder that affects many women of reproductive age. It is characterized by hormonal imbalances, irregular periods, and the presence of small cysts on the ovaries. PCOS can increase the risk of insulin resistance and type 2 diabetes due to the higher levels of insulin the body produces to compensate for the reduced effectiveness of the hormone.
The exact connection between PCOS and insulin resistance is not fully understood, but it is believed that hormonal imbalances disrupt insulin signaling pathways. This results in excess insulin in the bloodstream, leading to insulin resistance. Additionally, insulin resistance itself contributes to further hormone imbalances in PCOS, creating a vicious cycle.
If you have been diagnosed with PCOS, it is essential to work closely with your healthcare provider to manage and monitor your insulin resistance. Treatment options may include lifestyle modifications, such as healthy eating and regular exercise, as well as medication to regulate hormone levels and improve insulin sensitivity.
Gestational Diabetes
Gestational diabetes is a form of diabetes that occurs during pregnancy. Women who have had gestational diabetes are at an increased risk of developing insulin resistance and type 2 diabetes later in life. Hormonal changes during pregnancy can impair insulin function, leading to elevated blood sugar levels. If not properly managed, gestational diabetes can have health implications for both the mother and the baby.
A history of gestational diabetes should serve as a red flag for monitoring your insulin resistance levels in the future. Regular check-ups with your healthcare provider are crucial to assess your risk and take appropriate precautions. Lifestyle modifications, such as maintaining a healthy weight, eating a balanced diet, and engaging in regular exercise, play a significant role in preventing or managing insulin resistance following gestational diabetes.
Certain Medications
Some medications can increase the risk of developing insulin resistance. Glucocorticoids, often prescribed for inflammatory conditions, can interfere with insulin’s ability to regulate blood sugar levels. Similarly, antiretroviral drugs used in the treatment of HIV can contribute to insulin resistance. Anti-psychotic medications, frequently prescribed for mental health conditions, have also been associated with an increased likelihood of developing insulin resistance.
If you are taking any of these medications, it is essential to discuss the potential risks with your healthcare provider. They can help you monitor your insulin sensitivity and provide guidance on managing the effects of these medications. It’s important to note that the benefits of these medications often outweigh the potential risks of insulin resistance, so it is essential to strike a balance between managing your condition and minimizing additional health risks.
Regularly Check Blood Pressure and Cholesterol Levels
Aside from the specific risk factors mentioned above, it is crucial to monitor and manage other health conditions that can increase the risk of insulin resistance. High blood pressure and abnormal cholesterol levels are commonly associated with insulin resistance and can further contribute to cardiovascular disease. By regularly checking your blood pressure and cholesterol levels, you can identify any abnormalities and take appropriate action.
Maintaining healthy blood pressure and cholesterol levels is essential in preventing complications associated with insulin resistance and type 2 diabetes. If you have already been diagnosed with high blood pressure or elevated cholesterol, it’s important to follow your healthcare provider’s recommendations for medication, lifestyle modifications, and dietary changes. By addressing these risk factors, you can effectively reduce your chances of developing insulin resistance and improve your overall health.
Implement Lifestyle Changes
Preventing or managing insulin resistance ultimately comes down to making positive lifestyle changes. By adopting healthy habits, you can significantly reduce your risk of developing insulin resistance and its associated complications. Here are a few key lifestyle modifications to consider:
- Maintain a healthy weight: Losing excess weight, particularly around the abdominal area, can improve insulin sensitivity and reduce the risk of insulin resistance.
- Eat a well-balanced diet: Focus on consuming nutrient-rich foods, including whole grains, lean proteins, fruits, vegetables, and healthy fats. Limit your intake of processed and sugary foods.
- Engage in regular physical activity: Aim for at least 150 minutes of moderate-intensity exercise per week. Find activities you enjoy and incorporate them into your daily routine.
- Avoid prolonged periods of inactivity: Take regular breaks from sitting and incorporate movement into your day, such as stretching or short walks.
- Monitor your blood pressure and cholesterol levels: Regularly check these vital signs and follow your healthcare provider’s recommendations for maintaining healthy levels.
- Take medications as prescribed: If you are on any medications that may increase the risk of insulin resistance, follow your healthcare provider’s directions and communicate any concerns or side effects.
- Seek support: Consider joining support groups or seeking guidance from healthcare professionals to help you make and sustain positive changes.
By taking these precautions and implementing lifestyle changes, you can significantly reduce your risk of developing insulin resistance. Remember, it’s never too late to start prioritizing your health. Start small and gradually incorporate healthier habits into your daily life. Your body will thank you for it in the long run.