If you have ever experienced pain, you know how it can be intrusive and overwhelming. Pain management is crucial to ensure optimal patient comfort and recovery. In this article, we will explore the vital role of nurses in effective pain management. From assessing pain levels to implementing appropriate interventions, nurses play a key role in providing comfort and relief to patients. Let’s delve into the essential nursing considerations and management techniques that can make a significant difference in patients’ overall well-being.

Assessment of Pain
Patient history
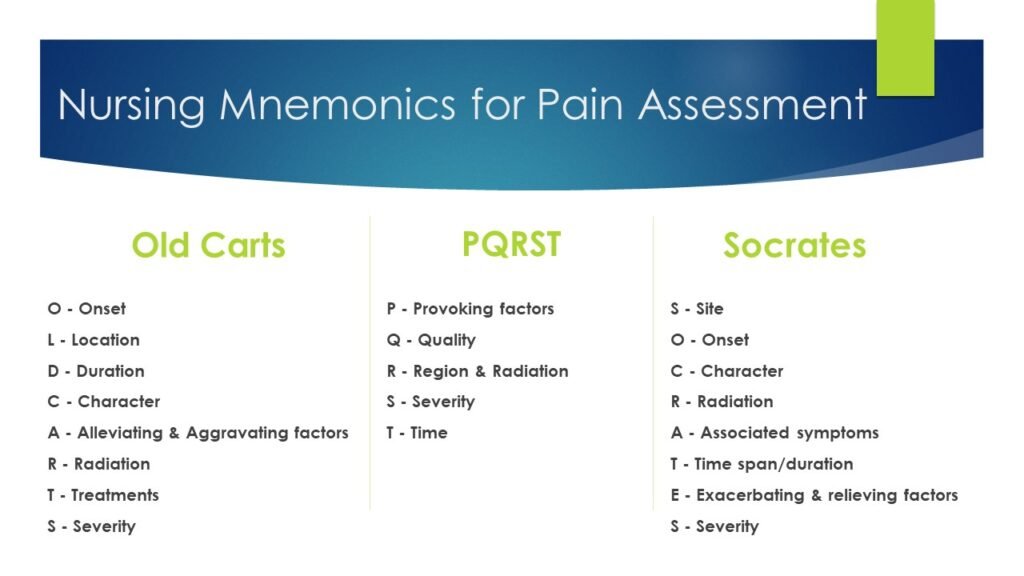
When assessing a patient’s pain, it is crucial to gather their history. This includes determining the onset, location, intensity, and quality of the pain. Understanding the patient’s medical history, past and current treatments, and any underlying conditions is also essential in developing an effective pain management plan. Additionally, it is important to consider psychosocial factors such as anxiety, depression, and stress, as these can significantly impact pain perception and management.
Observation and physical examination
Observation and physical examination play a vital role in pain assessment. Visual cues such as facial expressions, body language, and restlessness can provide valuable insights into the intensity and location of pain. Additionally, palpation and other physical examination techniques can help identify underlying causes of pain, such as inflammation or muscle spasms. It is crucial for nurses to be observant and attentive to these details to accurately assess and address the patient’s pain.
Assessment tools
To further enhance pain assessment, various assessment tools can be utilized. Tools such as the Numeric Rating Scale (NRS), Visual Analog Scale (VAS), and Wong-Baker FACES Pain Rating Scale are commonly used to quantify pain intensity. These tools allow patients to self-report their pain levels, providing a standardized measure for healthcare professionals to assess and monitor pain over time. Additionally, tools like the Pain Assessment in Advanced Dementia (PAINAD) scale can be used in patients with cognitive impairments who may have difficulty verbalizing their pain.
Use of Pharmacological Interventions
Medication administration
Pharmacological interventions are often necessary to manage pain effectively. Medications can be administered orally, intravenously, transdermally, or through various other routes depending on the patient’s condition and the urgency of pain relief. Different medications may be prescribed, including opioids, nonsteroidal anti-inflammatory drugs (NSAIDs), acetaminophen, and adjuvant medications such as antidepressants or anticonvulsants. Nurses play a crucial role in administering these medications safely and ensuring proper dosing and timing.
Routes of administration
The choice of medication administration route depends on factors such as the patient’s condition, the urgency of pain relief, and the patient’s ability to tolerate oral medications. Intravenous (IV) administration is commonly used for acute pain management, providing rapid and reliable pain relief. Oral medications, on the other hand, are effective for chronic pain management and can be self-administered by the patient at home. Transdermal patches and topical medications offer localized relief for specific areas of pain, such as joint or muscle pain.
Dose titration
Dose titration involves adjusting the dosage of medication based on the individual patient’s response and ongoing pain assessment. The goal is to find the minimum effective dose that provides adequate pain relief while minimizing side effects. Nurses closely monitor the patient’s response to medication, assessing for pain relief, adverse effects, and signs of medication tolerance or dependence. By collaboratively working with the patient and healthcare team, nurses can ensure the optimal balance between pain management and the patient’s safety and well-being.
Non-Pharmacological Interventions
Therapeutic positioning
Therapeutic positioning involves placing the patient in specific positions to alleviate pain and discomfort. For example, elevating the legs can relieve lower back pain, while side-lying positions can help alleviate pressure on specific body parts. Proper positioning ensures optimal comfort and support, promoting overall relaxation and pain relief for the patient.
Heat and cold therapy
Heat and cold therapy are non-pharmacological interventions that can provide effective pain relief. Applying heat, such as through hot packs or warm baths, helps relax muscles, increase blood circulation, and alleviate pain associated with muscle spasms or stiffness. Cold therapy, on the other hand, can reduce inflammation, numb pain, and decrease swelling. Ice packs, cold compresses, and cold baths are commonly used methods for cold therapy.
Massage and touch
Massage and touch therapies can have significant benefits in pain management. Gentle massages can help relax muscles, improve blood circulation, and promote the release of endorphins, which act as natural painkillers. Additionally, touch therapy, such as holding a patient’s hand or providing comforting hugs, can help reduce anxiety, increase feelings of emotional support, and alleviate pain perception.
Distraction techniques
Distraction techniques can effectively divert a patient’s attention from pain, reducing pain perception and improving overall comfort. Nurses can engage patients in activities such as listening to music, watching movies, playing games, or engaging in conversation to distract them from their pain. This can be especially useful for pediatric patients who may have difficulty understanding and managing their pain.
Patient Education and Empowerment
Pain education
Patient education is crucial in pain management, as it empowers patients to actively participate in their own care. Nurses should provide patients with information about the nature of their pain, potential treatment options, and self-management techniques. Educating patients about pain medications, potential side effects, and the importance of adhering to prescribed regimens can also help improve pain management outcomes.
Self-management techniques
Empowering patients with self-management techniques gives them the tools to effectively manage their pain outside of the healthcare setting. This may include teaching patients relaxation techniques, guided imagery, breathing exercises, or mindfulness practices. Encouraging patients to keep a pain diary or utilize pain tracking apps can also help them identify patterns and triggers, allowing for better pain management strategies.

Collaborative Approach in Pain Management
Interdisciplinary team communication
Pain management requires a collaborative approach involving various healthcare professionals. Effective communication and teamwork among nurses, physicians, pharmacists, physical therapists, and other specialists are crucial for providing comprehensive care. Regular interdisciplinary meetings and clear communication channels ensure that everyone is involved in the decision-making process and the patient’s pain management plan is coordinated and effective.
Multidimensional assessment
Pain is a complex experience that involves physical, psychological, and social factors. To provide holistic care, nurses must conduct a multidimensional assessment that addresses all aspects of the patient’s pain experience. This may involve collaborating with psychologists, social workers, and spiritual care providers to assess and address the psychosocial aspects of pain. By taking a comprehensive approach, healthcare professionals can develop individualized pain management plans tailored to the patient’s unique needs.
Maintaining continuity of care
Pain management is an ongoing process that requires consistency and continuity of care. Nurses play a crucial role in ensuring that the patient’s pain management plan is consistently implemented across healthcare settings. This involves effective handoff communication during patient transfers, providing clear documentation of the pain management plan, and ensuring that patients have access to necessary pain medications and resources beyond the hospital or clinical setting.
Cultural Considerations
Cultural beliefs and practices influencing pain perception and expression
Culture plays a significant role in how individuals perceive and express pain. Some cultures may value stoicism and discourage overt expression of pain, while others may encourage more vocalization and emotional expression. It is essential for nurses to be aware of these cultural differences and adapt their approach accordingly. Taking the time to understand a patient’s cultural background and beliefs can help in developing an individualized pain management approach that respects their cultural values.
Culturally sensitive care
Providing culturally sensitive care involves tailoring pain management strategies to align with a patient’s cultural beliefs, values, and preferences. This may involve utilizing traditional healing practices, involving family members in the decision-making process, or using culturally appropriate pain assessment tools. By acknowledging and incorporating cultural considerations, nurses can foster trust, promote effective communication, and ultimately improve pain management outcomes for their patients.

Special Considerations in Pediatric Pain Management
Assessment challenges in children
Assessing pain in children can be challenging due to their limited verbal communication skills and varying developmental stages. To effectively assess pain in pediatric patients, nurses often rely on a combination of self-report scales, behavioral observation, and physiological indicators. Utilizing age-appropriate pain assessment tools and involving parents or caregivers in the assessment process can help ensure accurate pain evaluation in children.
Age-appropriate pain scales
Different age groups require different pain assessment tools to ensure accurate and reliable results. The Wong-Baker FACES Pain Rating Scale is commonly used with younger children, allowing them to choose a facial expression that corresponds to their level of pain. Older children and adolescents may use numeric rating scales or visual analog scales, which involve rating pain on a scale from 0 to 10 or using a line to indicate pain intensity. Utilizing these age-appropriate pain scales enhances communication and helps healthcare professionals better understand and manage pediatric pain.
Geriatric Pain Management
Physiological changes in aging
As individuals age, they may experience physiological changes that can influence pain perception and management. Age-related changes in sensory stimuli, metabolism, and the central nervous system can affect how older adults experience and interpret pain. Additionally, comorbidities, polypharmacy, and cognitive impairments can further complicate pain management in geriatric patients. Nurses must be attentive to these physiological changes and tailor pain management strategies accordingly.
Polypharmacy considerations
Polypharmacy, the use of multiple medications, is common among older adults due to the management of multiple chronic conditions. However, the use of multiple medications can increase the risk of adverse effects, drug interactions, and medication-related problems. When managing pain in geriatric patients, nurses must carefully assess and consider the patient’s current medication regimen to avoid potential complications. Collaboration with physicians and pharmacists is essential in optimizing pain management while minimizing the risks associated with polypharmacy.
Comorbidity management
Geriatric patients often have multiple comorbidities, such as arthritis, diabetes, or cardiovascular disease, which can complicate pain management. Nurses need to take a holistic approach when caring for older adults, considering the impact of these comorbidities on pain perception, medication choices, and potential interactions. Understanding the interplay between multiple chronic conditions allows nurses to develop comprehensive pain management plans that address the individual needs and minimize the risks associated with comorbidities.

Pain Management in Palliative Care
Goals of palliative care
Palliative care focuses on providing relief from pain and other symptoms associated with serious illness. The primary goals of palliative care are to improve the quality of life, promote comfort, and offer emotional and psychological support to patients and their families. Nurses in palliative care settings play a crucial role in assessing and managing pain, collaborating with the interdisciplinary team, and ensuring the patient’s comfort and dignity throughout their journey.
Opioid use and titration
Opioids play a significant role in managing moderate to severe pain in palliative care. Nurses must carefully monitor and titrate opioid doses to provide adequate pain relief while minimizing side effects such as sedation or respiratory depression. Regular assessment of pain intensity, opioid side effects, and the patient’s overall condition is essential in ensuring effective pain management within the palliative care setting.
Psychological support
Palliative care patients often experience significant psychological and emotional distress, including anxiety, depression, and fear. Nurses must provide emotional support, active listening, and counseling to address these concerns. Collaborating with psychologists or social workers can further enhance the psychological support provided to patients and their families. By addressing both physical and psychological aspects of pain, nurses in palliative care settings contribute to the overall well-being and comfort of patients and their loved ones.
Ethical and Legal Considerations
Informed consent
In the realm of pain management, obtaining informed consent is essential when administering certain medications or performing procedures. Nurses must ensure that patients fully understand the purpose, risks, benefits, and alternatives of the proposed treatment plan. Informed consent involves open communication, ensuring the patient’s autonomy and right to make decisions about their own care. It is the nurse’s responsibility to provide the necessary information and answer any questions or concerns the patient may have.
Pain medication contracts
Pain medication contracts, also known as opioid contracts or pain management agreements, are commonly used in pain management to outline the responsibilities and expectations of both the healthcare provider and patient. These contracts help establish clear guidelines for medication use, periodic drug testing, expectations regarding adherence to the prescribed regimen, and steps for discontinuing or modifying treatment if necessary. Nurses must effectively communicate and educate patients about these contracts to ensure compliance and safe medication management.
