Sleep disorders can have a significant impact on a person’s overall health and well-being, and as a nurse, it is essential to be aware of the various nursing considerations and management strategies for these conditions. This article will provide you with valuable insights and practical guidance on how to support individuals with sleep disorders, including assessment and monitoring techniques, medication administration, and lifestyle modifications. By understanding the unique challenges faced by those struggling with sleep disorders, you can play a vital role in promoting better sleep and improving the quality of life for your patients.
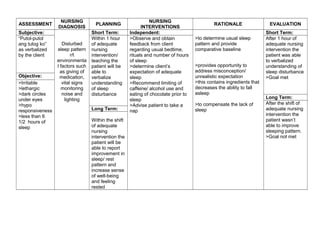
1. Types of Sleep Disorders
Sleep disorders are conditions that disrupt the normal sleep patterns of individuals, leading to difficulties in falling asleep, staying asleep, or experiencing restorative sleep. There are various types of sleep disorders that can affect individuals of all ages. It is essential to understand these different types to provide appropriate care and intervention.
1.1 Insomnia
Insomnia is one of the most common sleep disorders. It is characterized by difficulty falling asleep, staying asleep, or waking up too early and not being able to fall back asleep. Insomnia can be caused by various factors, including stress, anxiety, depression, medical conditions, or certain medications.
1.2 Sleep Apnea
Sleep apnea is a sleep disorder characterized by episodes of interrupted breathing during sleep. It can be caused by either a blockage in the airway (obstructive sleep apnea) or a failure of the brain to initiate breathing (central sleep apnea). Sleep apnea can lead to excessive daytime sleepiness, fatigue, and an increased risk of cardiovascular diseases if left untreated.
1.3 Narcolepsy
Narcolepsy is a neurological disorder that affects the brain’s ability to regulate sleep-wake cycles. Individuals with narcolepsy experience excessive daytime sleepiness, sudden episodes of sleep, and cataplexy (sudden loss of muscle tone triggered by emotions). The exact cause of narcolepsy is unknown, but it is believed to involve genetic and environmental factors.
1.4 Restless Leg Syndrome
Restless Leg Syndrome (RLS) is a condition characterized by an uncontrollable urge to move the legs, usually accompanied by uncomfortable sensations. Symptoms commonly occur when individuals are at rest, such as during sleep or prolonged periods of inactivity. RLS can significantly disrupt sleep and lead to daytime fatigue.
1.5 Circadian Rhythm Disorders
Circadian rhythm disorders occur when an individual’s internal body clock is misaligned with the external environment. This can result in difficulties falling asleep or waking up at desired times. Common examples of circadian rhythm disorders include jet lag, shift work sleep disorder, and delayed sleep phase syndrome.
1.6 Parasomnias
Parasomnias are a group of sleep disorders that involve abnormal movements, behaviors, emotions, perceptions, or dreams during sleep. Examples of parasomnias include sleepwalking, sleep talking, night terrors, and sleep-related eating disorder. These disorders can cause disruption to both the individual experiencing them and their sleep partners.
1.7 Sleepwalking
Sleepwalking, also known as somnambulism, is a parasomnia characterized by complex movements or behaviors during sleep. Sleepwalkers are often unaware of their actions and may perform activities such as walking, talking, or even driving a vehicle while asleep.
1.8 REM Sleep Behavior Disorder
REM Sleep Behavior Disorder (RBD) is a parasomnia characterized by the loss of muscle atonia during REM (rapid eye movement) sleep. This results in individuals acting out their dreams, which can be violent or dangerous. RBD can often be an early indicator of neurological conditions such as Parkinson’s disease.
1.9 Nightmares and Night Terrors
Nightmares are vivid, disturbing dreams that evoke strong emotions, often causing individuals to awaken abruptly. Night terrors, on the other hand, are intense episodes of fear or dread during sleep, accompanied by behaviors such as crying, screaming, or flailing. Both nightmares and night terrors can significantly disrupt sleep and lead to distress.
1.10 Sleep Disorders Related to Medical Conditions
Certain medical conditions can also contribute to the development of sleep disorders. These may include chronic pain, respiratory disorders (such as asthma or chronic obstructive pulmonary disease), neurological disorders (such as epilepsy or Alzheimer’s disease), or mental health disorders (such as depression or anxiety).
2. Common Symptoms of Sleep Disorders
Recognizing the symptoms of sleep disorders is crucial for their identification and management. While the specific symptoms may vary depending on the type of sleep disorder, there are several common signs to be aware of.
2.1 Difficulty Falling Asleep
Individuals with sleep disorders often experience difficulty falling asleep, despite feeling tired. They may toss and turn in bed, have racing thoughts, or feel restless and unable to relax.
2.2 Difficulty Staying Asleep
Waking up frequently during the night or having trouble staying asleep is another common symptom. Sleep disruptions can result from sleep apnea, restless leg syndrome, or other conditions leading to fragmented sleep.
2.3 Excessive Daytime Sleepiness
Feeling excessively tired or drowsy during the day, even after a full night’s sleep, is a significant symptom of a sleep disorder. Excessive daytime sleepiness can impact daily functioning, productivity, and overall quality of life.
2.4 Fatigue or Lack of Energy
Sleep disorders can often leave individuals feeling fatigued or lacking energy, even after an adequate amount of sleep. This persistent tiredness can affect physical, mental, and emotional well-being.
2.5 Impaired Concentration and Memory
Sleep deprivation and recurrent sleep disruptions can impair concentration, memory, and cognitive function. Individuals may have difficulty focusing, making decisions, or remembering information.
2.6 Mood Disturbances
Sleep disorders can contribute to mood disturbances, including irritability, frustration, anxiety, or depression. Mood swings and heightened emotional reactivity may be observed.
2.7 Irritability
Sleep deprivation and poor sleep quality can lead to irritability, often expressed as increased sensitivity to noise, light, or other environmental factors. Irritability may cause difficulties in personal and professional relationships.
2.8 Decreased Performance and Productivity
Sleep disorders can impact an individual’s performance and productivity, both at work and in daily activities. Difficulties in concentration, alertness, and memory can hinder overall performance levels.
2.9 Physical Symptoms
Sleep disorders may manifest with physical symptoms such as headaches, muscle aches, gastrointestinal disturbances, increased susceptibility to illnesses, or changes in appetite.
2.10 Impaired Quality of Life
Sleep disorders can significantly diminish an individual’s quality of life, affecting their ability to engage in enjoyable activities, maintain social relationships, and function optimally in daily life.

3. Assessment and Diagnosis
Proper assessment and diagnosis of sleep disorders are essential to develop appropriate treatment plans. Healthcare professionals, including nurses, play a crucial role in gathering information and facilitating the diagnostic process.
3.1 Sleep History
Obtaining a comprehensive sleep history is an essential component of the assessment process. The sleep history should include information about sleep patterns, duration of sleep, sleep environment, sleep-related symptoms, and any factors that may impact sleep quality.
3.2 Physical Examination
A physical examination may help identify underlying medical conditions contributing to sleep disorders. It can involve assessing vital signs, respiratory function, neurological function, and physical signs such as obesity or enlarged tonsils.
3.3 Sleep Diary
A sleep diary is a useful tool for individuals to track their sleep patterns and symptoms over a designated period. Sleep diaries can provide valuable insights into sleep quality, duration, and potential triggers.
3.4 Polysomnography
Polysomnography is a comprehensive sleep study conducted in a sleep laboratory. It involves recording brain waves, eye movement, muscle activity, heart rate, and other physiological parameters during sleep. Polysomnography can assist in diagnosing various sleep disorders, especially sleep apnea and narcolepsy.
3.5 Multiple Sleep Latency Test (MSLT)
The Multiple Sleep Latency Test measures how quickly an individual falls asleep during daytime nap opportunities. It is often conducted following an overnight polysomnography to evaluate excessive daytime sleepiness and help diagnose narcolepsy.
3.6 Epworth Sleepiness Scale
The Epworth Sleepiness Scale is a questionnaire used to assess an individual’s daytime sleepiness by asking them to rate their likelihood of falling asleep in various situations. It provides a subjective measure of excessive daytime sleepiness.
3.7 Mental Health Assessment
Mental health assessments can help identify any underlying psychological or psychiatric conditions that may contribute to sleep disturbances. Assessments may include evaluating mood, anxiety levels, and the presence of any mental health disorders.
3.8 Sleep Disorders Screening Tools
Specific screening tools, such as the Insomnia Severity Index or Stop-Bang questionnaire, can aid in the initial screening and identification of specific sleep disorders. These tools can provide a standardized measure and guide further assessment.
3.9 Differential Diagnosis
Differential diagnosis involves ruling out other potential causes of sleep disturbances that may mimic sleep disorders. This process helps ensure accurate diagnosis and appropriate treatment interventions.
3.10 Collaborative Assessments
In complex cases, interdisciplinary collaboration may be necessary for a comprehensive assessment. Collaboration with specialists such as sleep physicians, psychologists, and other healthcare professionals can provide valuable insights and enhance the accuracy of the diagnosis.
4. Nursing Interventions for Sleep Disorders
As crucial members of the healthcare team, nurses play an integral role in the management of sleep disorders. Nursing interventions aim to provide support, education, and strategies to promote healthy sleep habits and improve overall sleep quality.
4.1 Sleep Hygiene Education
Sleep hygiene education involves providing individuals with information and strategies to optimize their sleep routines and habits. This includes promoting consistent sleep schedules, creating a sleep-conducive environment, and establishing relaxing bedtime rituals.
4.2 Relaxation Techniques
Nurses can teach patients various relaxation techniques that can aid in falling asleep and reducing anxiety or stress-related sleep disturbances. These techniques may include deep breathing exercises, progressive muscle relaxation, guided imagery, or mindfulness meditation.
4.3 Cognitive Behavioral Therapy for Insomnia (CBT-I)
CBT-I is a psychological therapy that addresses the underlying thoughts, beliefs, and behaviors contributing to insomnia. Nurses can provide elements of CBT-I, such as sleep restriction therapy, stimulus control therapy, and cognitive restructuring, to help individuals improve their sleep quality.
4.4 Continuous Positive Airway Pressure (CPAP) Therapy
For individuals with obstructive sleep apnea, CPAP therapy is a common treatment approach. Nurses can educate patients on the proper use and maintenance of CPAP machines, ensure mask fitting, and provide ongoing support to promote adherence to therapy.
4.5 Medication Management
Nurses may play a role in medication management for sleep disorders, under the guidance of healthcare providers. This may involve providing education about medication options, proper administration, potential side effects, and monitoring treatment effectiveness.
4.6 Assistive Devices
Assistive devices, such as adjustable beds, orthopedic pillows, or white noise machines, can help improve sleep quality for individuals with specific sleep disorders or physical conditions. Nurses can assess the need for such devices and facilitate their acquisition or use.
4.7 Referrals to Specialists
In complex cases or when underlying medical or psychological conditions are present, nurses can facilitate referrals to specialists such as sleep physicians, psychiatrists, psychologists, or physical therapists. These specialists can provide additional expertise and interventions to optimize sleep outcomes.
4.8 Follow-up and Monitoring
Nurses can play an important role in follow-up and monitoring of individuals with sleep disorders. This includes assessing treatment progress, evaluating the effectiveness of interventions, addressing concerns or side effects, and making appropriate adjustments to the care plan.
4.9 Implementation of Sleep Environment Modifications
Nurses can collaborate with individuals to identify and modify any environmental factors that may interfere with sleep quality. This may involve minimizing noise, adjusting lighting, regulating temperature, and creating a comfortable sleep environment.
4.10 Family Education and Support
Sleep disorders can affect not only the individuals experiencing them but also their families or caregivers. Nurses can provide education and support to family members, helping them understand the impact of sleep disorders and strategies to assist their loved ones in improving their sleep outcomes.
5. Collaboration with the Interdisciplinary Team
Successful management of sleep disorders often requires collaboration with a diverse group of healthcare professionals. Nurses can actively participate and contribute to interdisciplinary teamwork to ensure holistic care for individuals with sleep disorders.
5.1 Physician
Physicians, particularly sleep medicine specialists, play a key role in the diagnosis, treatment, and ongoing management of sleep disorders. Nurses collaborate with physicians to share assessment findings, discuss treatment plans, and provide ongoing updates regarding patients’ progress.
5.2 Respiratory Therapist
Respiratory therapists are essential in the management of sleep disorders such as sleep apnea. Nurses collaborate with respiratory therapists to ensure appropriate referral, assessment, and support in the provision of respiratory interventions, including the use of CPAP machines.
5.3 Psychiatrist or Psychologist
Psychiatrists or psychologists can provide valuable insights and interventions for individuals with sleep disorders related to mental health conditions. Nurses collaborate with psychiatrists or psychologists to ensure a comprehensive approach to treatment, incorporating both psychological and physiological aspects.
5.4 Neurologist
Neurologists specialize in the diagnosis and management of sleep disorders with neurological origins, such as narcolepsy or RBD. Nurses collaborate with neurologists to facilitate referrals, coordinate care, and implement appropriate interventions based on neurology recommendations.
5.5 Sleep Specialist
Sleep medicine specialists are experts in the field of sleep disorders and can provide specialized knowledge and interventions. Nurses collaborate with sleep specialists to ensure accurate diagnosis, appropriate treatment plans, and ongoing support for individuals with complex sleep disorders.
5.6 Physical Therapist
Physical therapists may be involved in the management of sleep disorders, particularly those associated with musculoskeletal or physical conditions. Nurses collaborate with physical therapists to develop individualized exercise programs and provide recommendations for improving sleep quality.
5.7 Social Worker
Social workers can provide valuable support, counseling, and resources for individuals with sleep disorders, particularly those involving psychosocial challenges. Nurses collaborate with social workers to address social determinants of health, facilitate access to community resources, and provide emotional support to individuals and their families.
5.8 Dietitian
Dietitians can contribute to the management of sleep disorders by providing dietary recommendations that promote optimal sleep. Nurses collaborate with dietitians to address any nutrition-related factors that may impact sleep quality or contribute to sleep disturbances.
5.9 Occupational Therapist
Occupational therapists can assist individuals with sleep disorders in developing routines, environmental modifications, and relaxation strategies to improve sleep outcomes. Nurses collaborate with occupational therapists to incorporate sleep-related interventions into individuals’ daily activities and support occupational therapy goals.
5.10 Pharmacist
Pharmacists play a crucial role in medication management for sleep disorders. Nurses collaborate with pharmacists to ensure accurate medication administration, monitor medication interactions or side effects, and provide education regarding appropriate pharmaceutical interventions.
6. Considerations for Special Populations
Sleep disorders can vary in their presentation and management across different population groups. Nurses need to consider specific considerations when caring for special populations to ensure individualized care and optimal outcomes.
6.1 Pediatrics
Sleep disorders in children require specialized assessment and management. Nurses working with pediatric populations must consider age-specific factors such as growth and development, presence of sleep-related disorders unique to childhood (e.g., night terrors, sleepwalking), and the impact of sleep disorders on the child’s overall well-being and academic performance.
6.2 Geriatrics
Older adults may experience changes in sleep patterns and increased prevalence of sleep disorders. Nurses caring for geriatric populations should consider age-related physiological changes, comorbid conditions, polypharmacy, and the potential impact of sleep disorders on cognitive function, falls, and quality of life.
6.3 Pregnant Women
Pregnancy can introduce unique sleep challenges due to hormonal changes, physical discomfort, and psychological factors. Nurses working with pregnant women should provide education on sleep positions, relaxation techniques, and strategies to alleviate common sleep disturbances during pregnancy.
6.4 Shift Workers
Individuals working non-traditional shifts, such as night shifts or rotating shifts, are at an increased risk of sleep disorders. Nurses should consider the impact of disrupted circadian rhythms, potential safety hazards, and strategies to optimize sleep health for shift workers.
6.5 Individuals with Mental Health Disorders
Sleep disorders and mental health disorders often coexist. Nurses caring for individuals with mental health disorders should be aware of the bidirectional relationship between sleep and mental health, assess sleep disturbances, and collaborate with mental health professionals to provide comprehensive care.
6.6 Individuals with Comorbid Medical Conditions
Many medical conditions, such as cardiovascular diseases, respiratory disorders, and chronic pain, can contribute to the development of sleep disorders. Nurses working with individuals with comorbid conditions should consider the potential impact of these conditions on sleep and collaborate with healthcare providers to manage sleep disturbances effectively.
6.7 Individuals with Substance Use Disorders
Substance use disorders, including alcohol or drug dependence, can profoundly affect sleep patterns and lead to the development of sleep disorders. Nurses caring for individuals with substance use disorders should address substance abuse treatment, provide education on sleep hygiene, and offer appropriate interventions to improve sleep outcomes.
6.8 Individuals with Developmental Disabilities
Individuals with developmental disabilities may experience unique sleep challenges due to cognitive, sensory, or physical impairments. Nurses working with individuals with developmental disabilities should identify any sleep disturbances, address specific support needs, and develop individualized interventions to promote healthy sleep habits.
6.9 Individuals with Neurological Disorders
Neurological disorders such as Parkinson’s disease, epilepsy, or stroke can significantly impact sleep quality and contribute to the development of sleep disorders. Nurses caring for individuals with neurological disorders should collaborate with neurologists, occupational therapists, and other specialists to assess sleep disturbances and integrate appropriate interventions into the care plan.
6.10 Individuals with Chronic Pain Management
Chronic pain can significantly disrupt sleep and lead to the development of sleep disorders. Nurses should work closely with individuals managing chronic pain to identify pain-related sleep disturbances, implement pain management strategies, and provide education on sleep hygiene techniques to improve sleep quality.
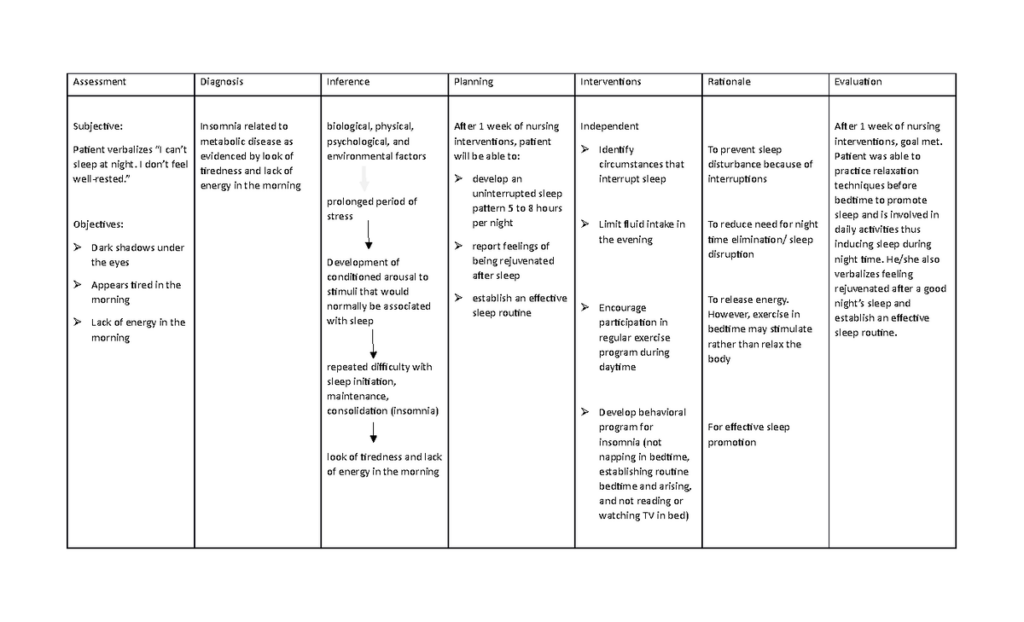
7. Ethical and Legal Considerations
When caring for individuals with sleep disorders, nurses must adhere to ethical and legal principles to ensure the delivery of safe, patient-centered care.
7.1 Confidentiality and Privacy
Nurses must maintain patient confidentiality and privacy when collecting, documenting, and discussing sensitive information related to sleep disorders. Respect for individuals’ privacy rights is fundamental in promoting trust and maintaining professional boundaries.
7.2 Informed Consent
Informed consent is essential when providing treatments or interventions for sleep disorders. Nurses should ensure individuals receive clear and comprehensive information about proposed interventions, potential risks, benefits, and alternative options before giving their consent.
7.3 Patient Autonomy
Respecting patient autonomy is crucial when assisting individuals with sleep disorders in decision-making processes. Nurses should empower individuals to actively participate in their care and support their choices regarding treatment options, sleep environment modifications, or lifestyle changes.
7.4 End-of-Life Care
In cases where individuals with sleep disorders are receiving end-of-life care, nurses must provide compassionate support, symptom management, and holistic care. Ethical considerations surrounding end-of-life decisions should be respected, and interdisciplinary collaboration is vital to ensure comfort and quality of life for the individual and their families.
7.5 Documentation and Communication
Accurate and thorough documentation is essential when caring for individuals with sleep disorders. Nurses should ensure that all assessments, interventions, patient responses, and communication with other healthcare professionals are appropriately documented to maintain continuity of care and legal accountability.
7.6 Ethical Dilemmas
Nurses may encounter ethical dilemmas in the care of individuals with sleep disorders, particularly when balancing patient autonomy, privacy, and safety concerns. In such situations, ethical principles should guide decision-making, and nurses should consult with colleagues, ethics committees, or supervisors as needed.
7.7 Legal Implications
Nurses must be knowledgeable about legal implications related to the management of sleep disorders. This includes understanding regulations regarding the administration of medications, certification requirements for specific interventions (e.g., CPAP), and legal responsibilities surrounding patient safety and informed consent.
7.8 Professional Boundaries and Ethics
Maintaining professional boundaries and ethical conduct is essential when caring for individuals with sleep disorders. Nurses should prioritize patient welfare, practice within their scope of practice, engage in ongoing professional development, and seek supervision or guidance as needed to ensure ethical care delivery.
7.9 Cultural Considerations
Culture influences individuals’ beliefs, practices, and perceptions regarding sleep and sleep disorders. Nurses should consider cultural factors when providing care, such as respecting cultural sleep practices, addressing cultural stigma associated with sleep disorders, and providing culturally sensitive education.
7.10 Duty of Care
Nurses have a legal and ethical duty to provide competent and compassionate care to individuals with sleep disorders. This includes recognizing and addressing sleep disturbances promptly, advocating for necessary interventions, and coordinating care to promote optimal sleep outcomes and overall well-being.
8. Education and Health Promotion Strategies
Education and health promotion are vital components of managing sleep disorders. Nurses can play a critical role in creating awareness, providing education, and implementing various strategies to promote healthy sleep habits and overall sleep health.
8.1 Public Awareness Campaigns
Nurses can initiate and participate in public awareness campaigns to educate communities about the importance of healthy sleep and the impact of sleep disorders on overall health. These campaigns can involve disseminating information through various channels, organizing community events, or collaborating with local organizations.
8.2 Community Talks and Workshops
Conducting community talks and workshops can provide valuable platforms for nurses to educate individuals and families about sleep disorders, sleep hygiene practices, and strategies for improving sleep quality. These sessions can be customized to address specific population groups, such as schools, workplaces, or community centers.
8.3 Health Fairs and Exhibitions
Participating in health fairs and exhibitions can allow nurses to interact directly with individuals, providing information, screening tools, and educational materials related to sleep disorders. This avenue can help raise awareness, provide on-the-spot education, and facilitate connections to healthcare resources.
8.4 Collaboration with Schools and Universities
Collaborating with schools and universities provides an opportunity for nurses to educate students, teachers, and parents about the importance of healthy sleep habits for academic success and overall well-being. Nurses can conduct workshops, provide educational materials, and recommend strategies to optimize sleep among students.
8.5 Support Groups
Facilitating support groups for individuals with sleep disorders and their families can help create a sense of community and provide a platform for sharing experiences, coping strategies, and emotional support. Nurses can organize support groups within healthcare settings or collaborate with community organizations to establish dedicated groups.
8.6 Online Resources and Education Materials
Developing and disseminating online resources and educational materials can help reach a wider audience. Nurses can contribute to the creation of evidence-based websites, blogs, or fact sheets that provide information, tips, and tools related to sleep disorders and healthy sleep practices.
8.7 Professional Development and Continuing Education
Nurses should engage in ongoing professional development and continuing education to stay current with sleep disorder management best practices. They can attend workshops, conferences, or online courses focused on sleep disorders, sleep medicine, or related nursing interventions.
8.8 Integration in Nursing Curriculum
Sleep disorders can be integrated into nursing curricula to ensure that future nurses receive education on the identification and management of sleep disorders. Incorporating relevant content into undergraduate and graduate nursing programs can help prepare nurses to deliver quality care to individuals with sleep disorders.
8.9 Research and Evidence-Based Practice
Nurses can contribute to the advancement of knowledge and evidence-based practice by participating in or conducting research related to sleep disorders. This can involve research on nursing interventions, outcomes measurement, or exploring novel approaches in sleep disorder management.
8.10 Advocacy for Sleep Health
Nurses can advocate for the importance of sleep health within healthcare systems, policy-making organizations, and public health initiatives. By raising awareness of sleep disorders, promoting policy changes, and advocating for equitable access to sleep disorder management resources, nurses can help improve sleep outcomes on a broader scale.

9. Evaluation and Outcomes
Evaluation of sleep disorder management is essential to gauge the effectiveness of interventions and ensure optimal outcomes for individuals. Nurses can employ various evaluation strategies to assess the progress, satisfaction, and overall impact of sleep disorder management.
9.1 Monitoring Sleep Patterns and Quality
Continuously monitoring sleep patterns and quality is crucial to assess the effectiveness of interventions. This may involve tracking sleep duration, sleep efficiency, the number of awakenings, or the severity of symptoms using tools such as sleep diaries or actigraphy.
9.2 Assessing Symptom Improvement
Regularly assessing symptom improvement is vital in evaluating the effectiveness of interventions. Nurses can use standardized assessment tools or patient self-reports to measure changes in symptoms such as difficulty falling asleep, daytime sleepiness, or quality of sleep.
9.3 Patient Satisfaction and Compliance
Assessing patient satisfaction and compliance with prescribed treatments is essential for evaluating the overall experience and effectiveness of sleep disorder management. Surveys, interviews, or feedback forms can help gather patient perspectives and identify areas for improvement.
9.4 Quality of Life Measures
Assessing changes in an individual’s quality of life can provide valuable insights into the impact of sleep disorder management. Nurses can use validated questionnaires or measures to evaluate changes in areas such as daily functioning, mood, cognitive ability, or overall well-being.
9.5 Collaboration and Communication Feedback
Regular collaboration and communication with interdisciplinary team members contribute to the effectiveness of sleep disorder management. Nurses can gather feedback from colleagues, specialists, and patients to evaluate the quality of collaboration, identify areas for improvement, and enhance communication processes.
9.6 Objective Assessment Tools
Objective assessment tools, such as polysomnography or actigraphy, can provide quantitative data on sleep parameters and assist in evaluating treatment effectiveness. The interpretation of objective assessment results should be done in collaboration with sleep medicine specialists or other experts.
9.7 Identifying Areas for Improvement
Regular evaluation helps identify areas for improvement in sleep disorder management. Nurses can assess the effectiveness of interventions, patient education materials or resources, collaborative processes, and the overall care environment to make necessary adjustments.
9.8 Reflections and Lessons Learned
Reflection and learning from experiences in sleep disorder management can contribute to ongoing improvement. Nurses can engage in self-reflection, participate in case discussions, or seek supervision to identify lessons learned and apply them to future practice.
9.9 Effectiveness of Implemented Interventions
Evaluation should focus on determining the effectiveness of implemented interventions in improving sleep outcomes. Objective data, patient reports, and interdisciplinary input can contribute to understanding which interventions are most successful and inform future practice.
9.10 Long-term Outcomes
Evaluating long-term outcomes of sleep disorder management is crucial to understanding the sustainability and durability of interventions. Nurses should consider long-term follow-up, assess maintenance of treatment effects, and identify any emerging concerns or needs that may arise over time.
10. Conclusion
Sleep disorders can significantly impact individuals’ well-being and overall quality of life. Nurses, with their expertise in patient care, play a crucial role in the assessment, management, and education associated with sleep disorders. By understanding the different types of sleep disorders, recognizing common symptoms, collaborating with interdisciplinary teams, and employing effective nursing interventions, nurses can provide comprehensive care and support to individuals with sleep disorders. Additionally, promoting education, developing health promotion strategies, adhering to ethical and legal principles, and evaluating outcomes contribute to improving sleep health outcomes on an individual and community level.
