In the exciting field of pediatric oncology, significant progress has been made in the treatment of Acute Myeloid Leukemia (AML) in children. Recent advances have brought about promising therapies and improved outcomes for young patients battling this aggressive form of leukemia. From targeted therapies to innovative immunotherapies, researchers are dedicated to finding better and more effective ways to combat AML in children, offering hope and the potential for a brighter future.
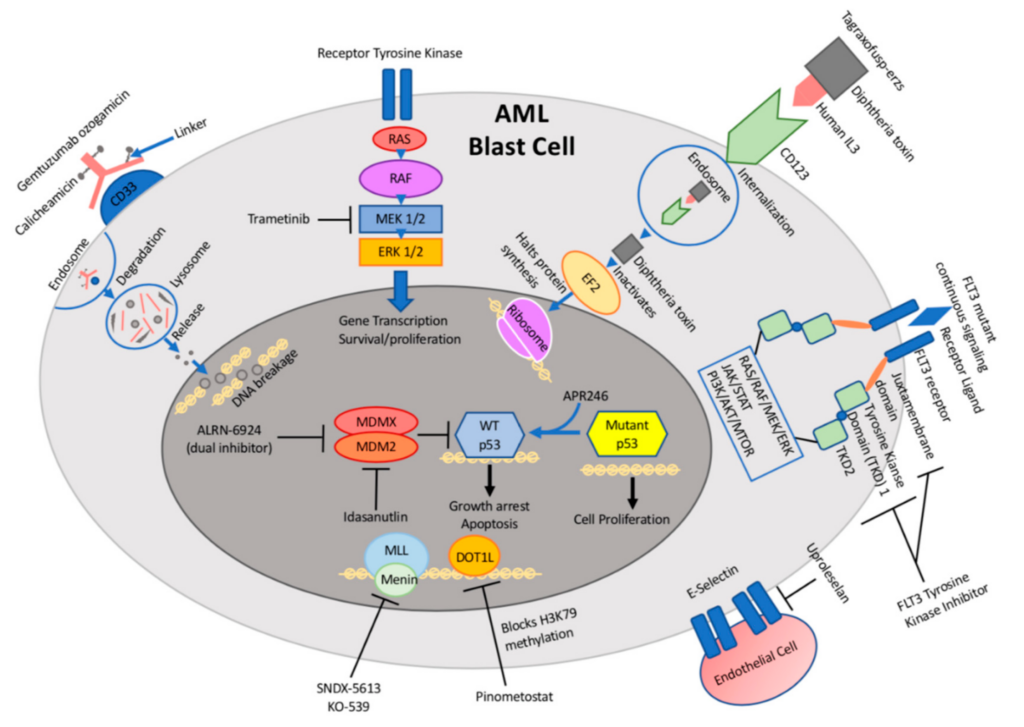
Recent Advances in Acute Myeloid Leukemia Treatment for Children
Acute Myeloid Leukemia (AML) is a type of cancer that affects the bone marrow and blood. While it can occur in people of any age group, it is most commonly seen in children. Over the years, significant progress has been made in the treatment of AML in children. This article aims to explore the recent advances in AML treatment, focusing on various modalities that have shown promising results.
Immunotherapy
Immunotherapy is a revolutionary treatment approach that harnesses the power of the immune system to fight cancer. It has transformed the landscape of cancer treatment, including AML in children. Immunotherapy involves the use of various techniques to stimulate and enhance the body’s natural defense mechanisms against cancer cells.
Introduction to Immunotherapy
Immunotherapy encompasses a wide range of treatments. One approach involves the use of checkpoint inhibitors, which are drugs that unleash the natural ability of the immune system to recognize and destroy cancer cells. Another breakthrough in immunotherapy is CAR-T cell therapy, where immune cells are genetically modified to specifically target and eliminate cancer cells.
Checkpoint Inhibitors
Checkpoint inhibitors work by blocking certain proteins that prevent immune cells from attacking cancer cells. These drugs help activate the immune system, allowing it to recognize and destroy leukemia cells more effectively. While checkpoint inhibitors are extensively researched and approved for various adult cancers, their use in pediatric AML is still under investigation, with promising results in preliminary studies.
CAR-T Cell Therapy
CAR-T cell therapy is a personalized treatment approach that involves modifying a patient’s own immune cells to target cancer cells. T cells, a type of immune cell, are genetically engineered to express chimeric antigen receptors (CARs) on their surface. These CARs are designed to recognize specific proteins found in leukemia cells, leading to their destruction. CAR-T cell therapy has shown remarkable success in some cases of pediatric AML, offering new hope for patients who have not responded to traditional treatments.
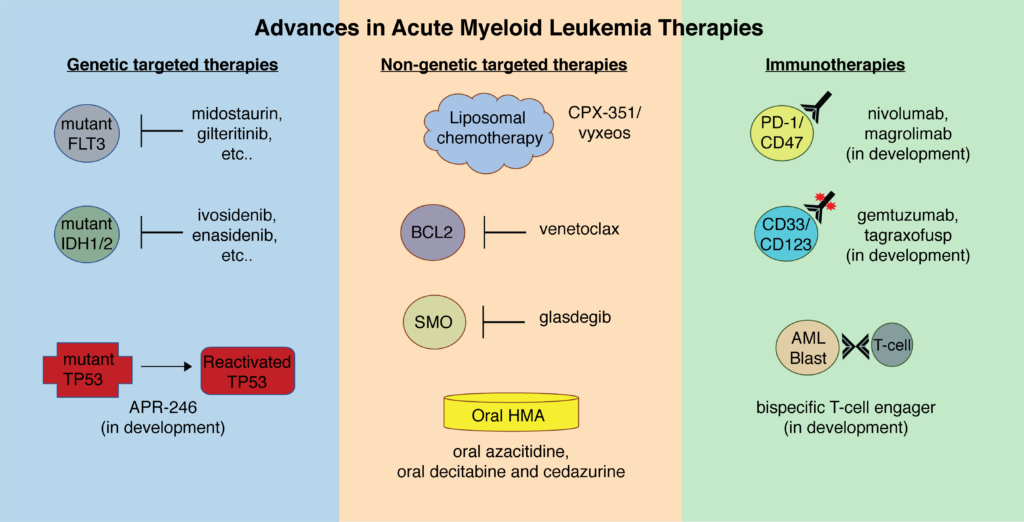
Targeted Therapy
Targeted therapy is an approach that focuses on specific molecular alterations or genetic mutations driving the growth and survival of cancer cells. By targeting these abnormalities, targeted therapy drugs can inhibit cancer cell growth while sparing healthy cells, leading to more effective treatment with fewer side effects.
FLT3 Inhibitors
One of the most significant advancements in targeted therapy for pediatric AML is the development of FLT3 inhibitors. FLT3 is a protein that plays a crucial role in the growth and survival of leukemia cells. Inhibition of FLT3 with targeted therapies has shown promising results, particularly in patients with FLT3-activating mutations.
IDH Inhibitors
IDH inhibitors target mutations in the IDH1 and IDH2 genes, which are commonly found in AML. These inhibitors work by blocking the abnormal function of mutant IDH proteins, thereby inhibiting the growth of leukemia cells. Clinical trials have shown encouraging outcomes in patients with IDH mutant AML, leading to the approval of IDH inhibitors for AML treatment.
KIT Inhibitors
KIT inhibitors are targeted therapies that aim to inhibit abnormal activation of the KIT protein, which is implicated in certain subtypes of AML, particularly pediatric AML with core-binding factor (CBF) rearrangements. By blocking the activity of the KIT protein, these inhibitors can impede leukemia cell proliferation and promote their elimination.
Chemotherapy
Chemotherapy has long been the standard of care in AML treatment and continues to play a crucial role in the management of pediatric AML. It involves the use of powerful drugs to kill leukemia cells and prevent their further growth and division.
Induction Chemotherapy
Induction chemotherapy is the initial phase of treatment aimed at achieving remission, which refers to the absence of leukemia cells in the bone marrow. It involves the administration of intensive chemotherapy regimens over a few weeks. The goal is to eliminate the majority of leukemia cells and restore normal blood cell production.
Consolidation Chemotherapy
Consolidation chemotherapy follows induction therapy and is aimed at eradicating any remaining leukemia cells that may not be detectable under the microscope. This phase often involves several cycles of chemotherapy to ensure complete remission and reduce the risk of relapse.
Intensification Chemotherapy
Intensification chemotherapy refers to a more aggressive approach to treatment designed to further reduce the burden of leukemia cells and prevent relapse. This phase may consist of high-dose chemotherapy, sometimes with additional drugs or stem cell transplantation.
Maintenance Chemotherapy
Maintenance chemotherapy is a prolonged treatment phase that aims to sustain remission and minimize the risk of relapse. It usually involves lower-dose chemotherapy for an extended period, typically several months to years, depending on the risk profile of the patient.
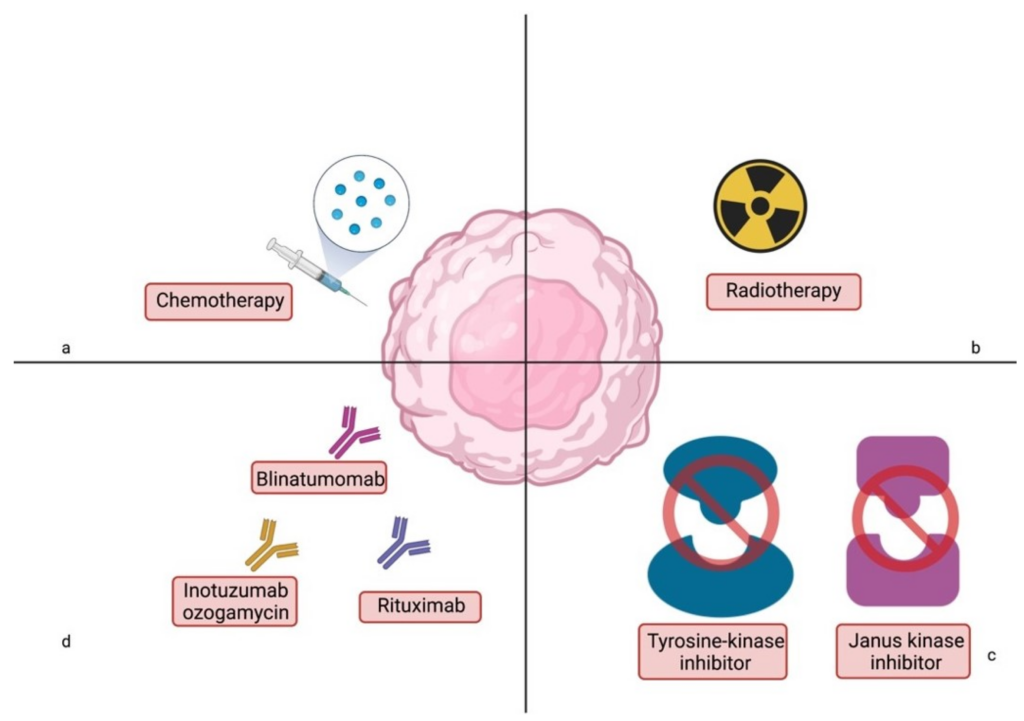
Stem Cell Transplantation
Stem cell transplantation, also known as bone marrow transplantation, offers a potential cure for pediatric AML. It involves replacing the diseased bone marrow with healthy stem cells obtained from a donor (allogeneic) or the patient themselves (autologous) after intensive chemotherapy or radiation to destroy leukemia cells.
Allogeneic Stem Cell Transplantation
Allogeneic stem cell transplantation involves using stem cells from a matched sibling donor or an unrelated donor. This approach offers the advantage of the graft-versus-leukemia effect, where the immune cells from the donor can recognize and eliminate residual leukemia cells. However, it carries the risk of graft-versus-host disease, a complication where the donor immune cells attack healthy tissues.
Autologous Stem Cell Transplantation
Autologous stem cell transplantation utilizes the patient’s own stem cells, usually collected and stored prior to high-dose chemotherapy. After the elimination of leukemia cells using intensive therapies, the stored stem cells are infused back into the patient’s bloodstream to regenerate the bone marrow. This approach removes the risk of graft-versus-host disease but may have a higher relapse rate.
Reduced-Intensity Stem Cell Transplantation
Reduced-intensity stem cell transplantation aims to reduce the toxicity associated with conventional high-dose chemotherapy and radiation. It involves using lower-intensity conditioning regimens to prepare the patient’s body for the donor stem cells. This approach is particularly useful for patients who may be older or have underlying health concerns that limit their tolerance for intensive conditioning.
Supportive Care
Supportive care plays a critical role in the comprehensive management of pediatric AML. It focuses on minimizing treatment-related complications, improving quality of life, and providing holistic support to children and their families throughout the treatment journey.
Management of Infections
Infections are a significant concern for children undergoing AML treatment, as chemotherapy can weaken the immune system. Vigilant monitoring for signs of infection and prompt initiation of appropriate antibiotics are essential. In addition, preventative strategies, such as vaccinations and prophylactic antibiotics, may be employed to reduce the risk of infections.
Red Blood Cell Transfusions
Children with AML often develop anemia, where the levels of healthy red blood cells are low. Red blood cell transfusions can help alleviate symptoms like fatigue and shortness of breath, improving overall well-being and quality of life.
Platelet Transfusions
AML treatment can cause a decrease in platelet levels, leading to an increased risk of bleeding. Platelet transfusions are administered to restore platelet counts and prevent bleeding complications. Close monitoring of platelet levels is essential to ensure timely transfusions when necessary.
Antifungal Prophylaxis
Children with AML are susceptible to fungal infections due to the prolonged use of immunosuppressive therapy. Antifungal prophylaxis may be administered to reduce the risk of fungal infections and their associated complications.
Pain Management
AML and its treatment can cause pain and discomfort in children. Effective pain management strategies, including medications and non-pharmacological approaches, are essential to ensure the well-being and comfort of young patients.

Minimal Residual Disease Detection
Minimal residual disease (MRD) refers to the presence of small amounts of leukemia cells that may remain after treatment in patients who are in remission. MRD detection has become increasingly relevant in AML treatment as it provides valuable information about the risk of relapse and helps guide treatment decisions.
Techniques for Detection
Several techniques can be employed to detect MRD, including flow cytometry, polymerase chain reaction (PCR), and next-generation sequencing (NGS). These methods enable the sensitive assessment of residual leukemia cells at a molecular level, offering insights into disease burden and potential relapse risks.
Importance of MRD Monitoring
MRD monitoring allows healthcare providers to identify patients who may be at higher risk of relapse. By closely monitoring MRD levels over time, treatment can be personalized and intensified to prevent relapse and improve long-term outcomes.
Impact on Treatment Decisions
MRD detection has emerged as a critical tool for guiding treatment decisions in pediatric AML. Patients with persistent MRD may benefit from additional therapies such as stem cell transplantation or targeted agents. Conversely, patients with low or undetectable MRD levels may be candidates for less intensive treatment, minimizing the risk of unnecessary toxicities.
Precision Medicine
Precision medicine aims to tailor treatment approaches to the unique characteristics of each patient, considering factors such as genetic mutations, molecular profiles, and individual responses to therapies. In recent years, precision medicine has shown promising results in the treatment of pediatric AML.
Molecular Profiling
Molecular profiling involves analyzing the genetic and molecular characteristics of leukemia cells to identify specific mutations or alterations. This information helps guide treatment decisions and identify potential targeted therapies that can effectively inhibit the abnormal pathways driving cancer growth.
Targeted Therapies Based on Genetic Mutations
Precision medicine has paved the way for targeted therapies that specifically address the genetic mutations driving AML in children. By matching targeted therapies to the specific molecular alterations present in individual patients, treatment outcomes can be significantly improved.
Clinical Trials
Clinical trials play a vital role in advancing the field of pediatric AML treatment. These studies provide opportunities to explore new treatments, improve existing therapies, and evaluate the efficacy and safety of novel interventions.
Importance of Clinical Trials
Clinical trials offer access to innovative treatment approaches and help shape the future of AML treatment for children. Participation in clinical trials allows patients to receive cutting-edge therapies that may not be available through standard treatment protocols.
Recent Advances in Clinical Trials
The field of pediatric AML has witnessed significant progress through clinical trials. New treatment strategies, including immunotherapy, targeted therapies, and precision medicine approaches, are being evaluated in clinical trial settings, with encouraging preliminary results. These trials hold promise for improved outcomes and survival rates for children with AML.
Side Effects Management
The treatment of pediatric AML can cause various side effects that impact the child’s well-being and quality of life. Effectively managing these side effects is crucial to ensure the best possible treatment experience.
Novel Strategies for Relapse Prevention
Relapse is a significant concern in AML, and preventing relapse is of utmost importance in achieving long-term remission. Innovative therapeutic strategies are being explored to prevent relapse, such as immune-based therapies, targeted therapies for specific mutations, and combination treatments aimed at eradicating residual leukemia cells more effectively.
Post-Remission Therapies
Post-remission therapies are employed to consolidate the gains achieved during initial treatment and further reduce the risk of relapse. These therapies may include reduced-intensity chemotherapy, targeted therapies, or stem cell transplantation, depending on the patient’s risk profile and specific clinical characteristics.
Recent advances in the treatment of pediatric AML have brought about remarkable improvements in outcomes and revolutionized the approach to care. Immunotherapy, targeted therapy, chemotherapy, stem cell transplantation, and precision medicine have all contributed to enhanced treatment strategies. Clinical trials continue to drive innovation in the field, offering hope for further progress and better long-term outcomes for children with AML. With a multi-modal approach that includes supportive care and side effect management, the comprehensive management of pediatric AML has significantly improved, providing renewed hope for patients and their families.
Watch This Video Below
Related Terms About Recent Advances in Acute Myeloid Leukemia Treatment for Children
Acute Lymphoblastic Leukemia Treatment In Child, Acute Lymphoblastic Leukemia Treatment Side Effects, Acute Myeloid Leukemia Chemotherapy Side Effects, Acute Myeloid Leukemia Chemotherapy Survival Rate, Acute Myeloid Leukemia Child Survival Rate, Acute Myeloid Leukemia Treatment Side Effects, Acute Myeloid Leukemia Treatment Strategy, Acute Myeloid Leukemia Treatment Study, Acute Myeloid Leukemia Treatment Success, Acute Myeloid Leukemia Treatment Success Rate