If you’ve ever experienced a sudden, intense pain in your upper abdomen, you may be familiar with acute pancreatitis. This condition, characterized by inflammation of the pancreas, can be incredibly painful and potentially life-threatening. But fear not, because, in this article, we’ll break down the causes, symptoms, and treatment options for acute pancreatitis. By the end, you’ll have a better understanding of this condition and be equipped with the knowledge to seek the necessary medical attention if needed. So, let’s get started!

Causes of Acute Pancreatitis
Acute pancreatitis can have various causes. Understanding these causes is important in order to prevent or manage the condition effectively.
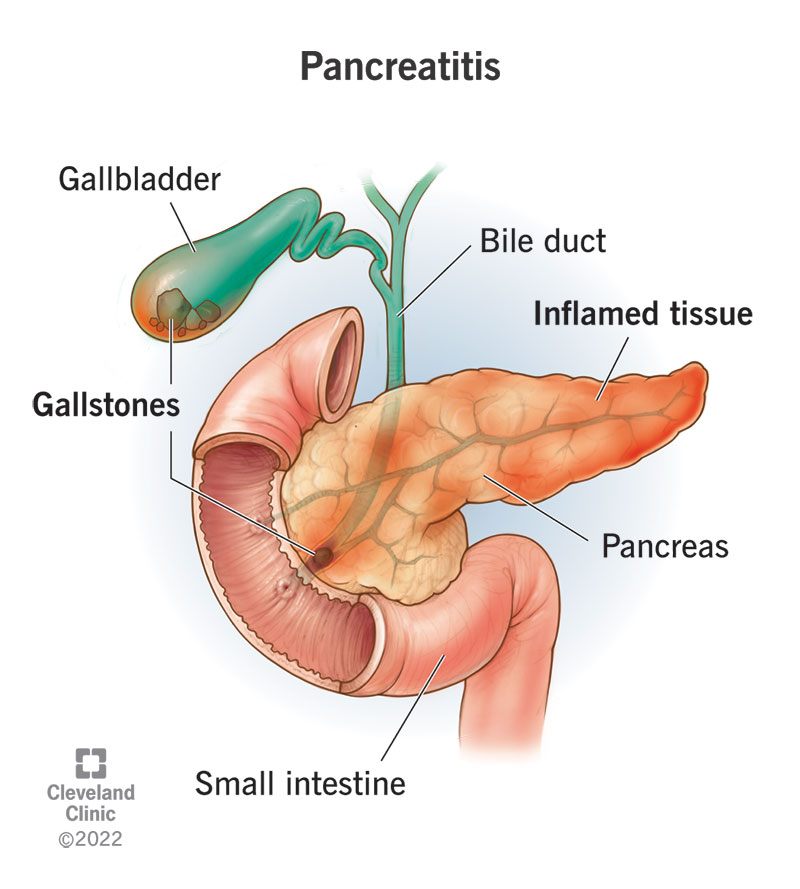
Gallstones
One of the common causes of acute pancreatitis is the presence of gallstones. When these small, hard deposits develop in the bile duct, they can block the passage of digestive enzymes from the pancreas into the small intestine. This can lead to inflammation and damage to the pancreas.
Alcohol consumption
Excessive alcohol consumption is another significant factor that can trigger acute pancreatitis. Alcohol can irritate the pancreas, leading to inflammation and a sudden bout of the condition. It is important to note that not everyone who consumes alcohol excessively will develop pancreatitis, but the risk increases with heavy and prolonged use.
High levels of triglycerides
Elevated levels of triglycerides, a type of fat found in the blood, can also contribute to the development of acute pancreatitis. When triglyceride levels are too high, they can clog the blood vessels in the pancreas, restricting blood flow and causing inflammation.
Infections
Certain infections, such as viral infections like mumps or bacterial infections like pneumonia, can also cause acute pancreatitis. These infections can directly affect the pancreas, leading to inflammation and the onset of the condition.
Medications
Certain medications, although rare, can also be a cause of acute pancreatitis. Examples include certain antibiotics, diuretics, and drugs used for chemotherapy. If you are taking any medications and experience symptoms of pancreatitis, it is important to consult with your healthcare provider.
Injury or trauma to the pancreas
Injury or trauma to the pancreas, such as a car accident or a severe blow to the abdomen, can result in acute pancreatitis. The physical trauma can disrupt the normal functioning of the pancreas, causing it to become inflamed.
Genetic factors
Genetics can play a role in the development of acute pancreatitis. Certain inherited conditions, such as hereditary pancreatitis or cystic fibrosis, can increase the risk of pancreatitis. If you have a family history of these conditions, it is important to be mindful of the symptoms and seek medical attention if needed.
Autoimmune conditions
In some cases, the body’s immune system can mistakenly attack the pancreas, leading to acute pancreatitis. Autoimmune conditions such as lupus or rheumatoid arthritis can increase the risk of this immune response and subsequent inflammation of the pancreas.
Recurring episodes of acute pancreatitis
Experiencing multiple episodes of acute pancreatitis can also contribute to the development of the condition. Each episode can cause further damage to the pancreas, increasing the likelihood of future episodes and the potential for long-term complications.
Cystic fibrosis
Cystic fibrosis, a genetic disorder that primarily affects the lungs and digestive system, can also lead to the development of acute pancreatitis. The condition causes the production of thick and sticky mucus, which can obstruct the pancreatic ducts and trigger inflammation.
Symptoms of Acute Pancreatitis
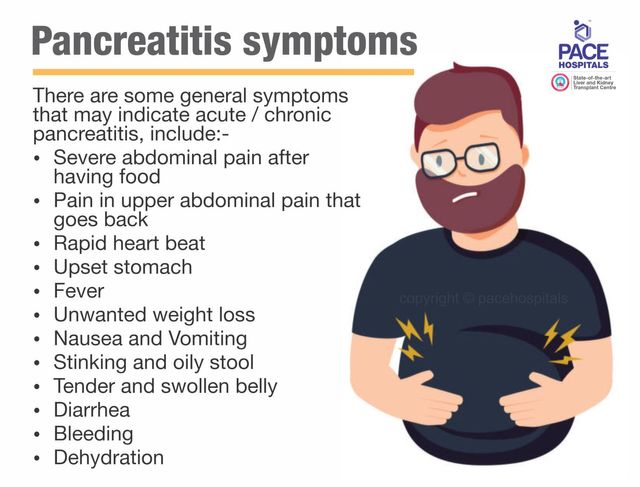
Recognizing the symptoms of acute pancreatitis is essential for early diagnosis and treatment. If you experience any of the following symptoms, it is important to seek immediate medical attention.
Severe abdominal pain
One of the hallmark symptoms of acute pancreatitis is severe abdominal pain. This pain is usually located in the upper abdomen and can radiate to the back. It is often described as persistent and can worsen after eating.
Nausea and vomiting
Nausea and vomiting are common symptoms accompanying acute pancreatitis. These symptoms can be persistent and may not provide relief.
Fever
Fever can also be present in cases of acute pancreatitis. The body’s immune system responds to the inflammation in the pancreas by increasing its temperature to fight off possible infections.
Rapid pulse
During an episode of acute pancreatitis, the heart may beat faster than usual. This increased heart rate, known as tachycardia, is a response to the body’s inflammatory processes.
Swollen and tender abdomen
The abdomen may become swollen and tender to the touch during an acute pancreatitis episode. This is a result of the inflammation and irritation of the pancreas, which can extend to surrounding tissues.
Back pain
The severe abdominal pain associated with acute pancreatitis often radiates to the back. This back pain can be persistent and worsen with movement.
Loss of appetite
Due to the pain and discomfort, individuals with acute pancreatitis may experience a loss of appetite. This can lead to unintentional weight loss if the condition persists.
Indigestion
Indigestion, characterized by a feeling of fullness, bloating, or discomfort after eating, is another symptom that can accompany acute pancreatitis.
Unexplained weight loss
Unintentional weight loss can occur with acute pancreatitis, as the body may have difficulty absorbing nutrients properly due to the inflammation and disruption of normal pancreatic function.
Jaundice
Jaundice, characterized by yellowing of the skin and eyes, can occur in cases where acute pancreatitis affects the bile duct. This can happen when the obstruction of the pancreatic duct leads to the backflow of bile into the bloodstream.
Diagnosis of Acute Pancreatitis
To diagnose acute pancreatitis, healthcare providers may use a combination of physical examinations and medical tests.
Physical examination
During a physical examination, the healthcare provider will examine the abdomen for tenderness, bloating, or swelling. They may also check for signs of yellowing of the skin and eyes, and assess the patient’s overall condition.
Blood tests
Blood tests, including amylase and lipase levels, can help determine if there are elevated levels of these enzymes. In cases of acute pancreatitis, these pancreatic enzymes may be elevated due to the damage to the pancreas.
Imaging tests (ultrasound, CT scan, MRI)
Imaging tests may be recommended to visualize the pancreas and its surrounding structures. An ultrasound, CT scan, or MRI can provide detailed images that help identify any abnormalities or inflammation in the pancreas.
Endoscopic retrograde cholangiopancreatography (ERCP)
In some cases, an ERCP may be performed to evaluate the pancreatic and bile ducts. This procedure uses a flexible tube with a camera at the end to examine the ducts and, if necessary, perform interventions such as removing gallstones or placing stents.
Biopsy
In rare cases, a biopsy of the pancreas may be performed to confirm the diagnosis and rule out other conditions. This involves taking a small tissue sample from the pancreas for analysis under a microscope.
Complications of Acute Pancreatitis
Acute pancreatitis can lead to various complications, some of which can be serious and require additional medical intervention.
Pancreatic pseudocysts
During an episode of acute pancreatitis, fluid and tissue debris can accumulate, forming a pseudocyst. These cysts can cause persistent abdominal pain and may require drainage if they become large or infected.
Infection
The inflammation and disruption of the pancreas can increase the risk of infection. In severe cases, bacteria can invade the pancreas or the pseudocysts, leading to an infection that requires immediate medical attention.
Pancreatic necrosis
In some instances, the blood vessels in the pancreas can become damaged, causing tissue death or necrosis. This can contribute to the formation of infected pseudocysts and increase the risk of complications.
Respiratory problems
Acute pancreatitis can affect the respiratory system, leading to complications such as pleural effusion (fluid buildup around the lungs) or acute respiratory distress syndrome (ARDS). These respiratory problems can be life-threatening and require intensive care.
Diabetes
Damage to the pancreas from acute pancreatitis can disrupt the production and release of insulin, leading to the development of diabetes. Long-term management of blood sugar levels may be necessary for individuals who develop diabetes as a complication of acute pancreatitis.
Malnutrition
Persistent inflammation and disruption of the pancreas can interfere with the digestion and absorption of nutrients, leading to malnutrition. This can result in weight loss, weakness, and nutrient deficiencies.
Acute Pancreatitis Treatment
The treatment approach for acute pancreatitis typically involves a combination of medical interventions and lifestyle changes.
Hospitalization
Moderate to severe cases of acute pancreatitis usually require hospitalization. This allows healthcare providers to closely monitor the patient’s condition and provide necessary treatments.
Pain management
Severe abdominal pain is a common symptom of acute pancreatitis. Medications such as analgesics may be prescribed to help manage the pain effectively.
Intravenous fluids
To prevent dehydration and help the pancreas recover, intravenous (IV) fluids may be administered. These fluids contain essential electrolytes and nutrients that the body needs to heal.
Nasogastric tube
In some cases, a nasogastric tube may be placed to remove excess stomach contents and relieve pressure on the pancreas. This can help with nausea and vomiting and allow the pancreas to rest.
Antibiotics
If an infection is present or suspected, antibiotics may be prescribed to help fight off the infection and prevent it from spreading.
Nutritional support
Maintaining proper nutrition is crucial for individuals with acute pancreatitis. If oral intake is difficult, a temporary feeding tube or total parenteral nutrition (TPN) may be recommended to ensure adequate nutrient intake.
Gallbladder removal
If gallstones are the underlying cause of acute pancreatitis, surgical removal of the gallbladder (cholecystectomy) may be necessary to prevent future episodes.
Endoscopic or surgical drainage of pseudocysts
Large or infected pseudocysts may need to be drained either endoscopically or surgically. This helps relieve pain, prevent infection, and promote the healing of the pancreas.
Pancreatic enzyme replacement therapy
In cases where the pancreas is not producing sufficient digestive enzymes, pancreatic enzyme replacement therapy (PERT) may be prescribed. This involves taking oral enzymes to aid in the digestion and absorption of nutrients.
Lifestyle changes (diet, quitting alcohol)
To prevent recurrent episodes of acute pancreatitis, lifestyle changes are often recommended. This may include adopting a low-fat diet, quitting alcohol consumption, and maintaining a healthy weight through regular exercise.
Prevention of Acute Pancreatitis
While not all cases of acute pancreatitis can be prevented, certain measures can help reduce the risk of developing the condition.
Maintaining a healthy weight
Obesity is a risk factor for acute pancreatitis. By maintaining a healthy weight through proper diet and regular exercise, individuals can reduce their risk of developing the condition.
Eating a balanced diet
Following a balanced diet, rich in fruits, vegetables, lean proteins, and whole grains, can help support overall pancreas health and reduce the risk of developing pancreatitis.
Moderating alcohol consumption
Excessive alcohol consumption is a known risk factor for acute pancreatitis. By moderating alcohol intake or avoiding it altogether, individuals can significantly reduce their risk.
Regular exercise
Engaging in regular physical activity not only helps maintain a healthy weight but also improves overall health and reduces the risk of various conditions, including acute pancreatitis.
Avoiding smoking
Smoking is not only harmful to overall health but can also increase the risk of pancreatitis. Quitting smoking can have a positive impact on pancreas health and overall well-being.
Managing underlying medical conditions
If you have any underlying medical conditions, such as high triglyceride levels or autoimmune disorders, it is important to work closely with your healthcare provider to manage these conditions effectively. This can help minimize the risk of acute pancreatitis.
Avoiding triggers (certain medications, high-fat diets)
If you have a history of acute pancreatitis, it is important to avoid triggers that can worsen the condition. This may include certain medications known to cause pancreatitis or high-fat diets that can strain the pancreas.

Recurrent Acute Pancreatitis
In some cases, individuals may experience recurrent episodes of acute pancreatitis. This can be challenging and requires comprehensive management.
Causes of recurrent acute pancreatitis
The causes of recurrent acute pancreatitis can vary from person to person. It may be due to ongoing gallstone issues, alcohol consumption, or other underlying factors. Identifying and addressing these causes is important in managing recurrent episodes.
Diagnosis and treatment of recurrent acute pancreatitis
Healthcare providers will conduct a thorough evaluation to determine the underlying causes of recurrent acute pancreatitis. Treatment options may involve a combination of lifestyle changes, medication adjustments, or further interventions, such as surgery or endoscopic procedures.
Complications of recurrent acute pancreatitis
Recurrent acute pancreatitis poses an increased risk of complications compared to single episodes. These complications can include the development of chronic pancreatitis, pancreatic insufficiency, and an increased risk of developing pancreatic cancer. Close monitoring and follow-up with healthcare providers are crucial to minimize these risks.
Children and Acute Pancreatitis
While acute pancreatitis is more commonly seen in adults, children can also develop this condition. The causes, symptoms, and treatment of acute pancreatitis in children may have some differences compared to adults.
Causes of acute pancreatitis in children
In children, some of the common causes of acute pancreatitis include trauma or injury to the pancreas, genetic factors, certain medications, infections, and underlying medical conditions like cystic fibrosis.
Symptoms and diagnosis in children
The symptoms of acute pancreatitis in children may be similar to those seen in adults, including severe abdominal pain, nausea, vomiting, and fever. However, young children may have difficulty expressing their symptoms, making it important for parents and healthcare providers to closely monitor any signs of distress. Diagnosis in children may involve a combination of physical examinations, blood tests, and imaging studies.
Treatment options for children
The treatment of acute pancreatitis in children is similar to that in adults. Hospitalization, pain management, intravenous fluids, and nutritional support may be necessary. In some cases, interventions such as endoscopic procedures or surgeries may be required to address specific complications.
Long-term effects and complications
Children who have had acute pancreatitis may require long-term follow-up and monitoring. It is important to manage any identified underlying causes, such as genetic conditions or metabolic disorders, to prevent recurrent episodes and minimize the risk of complications.

When to Seek Medical Help
While mild cases of acute pancreatitis may resolve on their own with home care measures, certain situations warrant immediate medical attention.
Severe abdominal pain that does not improve
If you are experiencing severe abdominal pain that does not improve or becomes progressively worse, it is important to seek medical help right away. This could be a sign of a serious complication or a severe flare-up of pancreatitis.
Persistent vomiting
Persistent vomiting, especially if accompanied by other symptoms such as severe abdominal pain or inability to keep any food or fluids down, requires medical attention. This could indicate dehydration or an obstructed digestive system.
Fever above 102°F (38.9°C)
If you have a high fever along with other symptoms suggestive of acute pancreatitis, medical evaluation is necessary. Fever can indicate an infection or inflammation that requires prompt treatment.
Signs of dehydration
Signs of dehydration, including excessive thirst, dry mouth, dark urine, or dizziness, should not be ignored. Acute pancreatitis can lead to dehydration, and prompt medical intervention is crucial to prevent complications.
Difficulty breathing
If you are experiencing difficulty breathing or shortness of breath along with other symptoms of acute pancreatitis, it is important to seek immediate medical help. Respiratory complications can occur, and swift intervention is necessary.
Yellowing of the skin or eyes
Jaundice, which is characterized by yellowing of the skin and eyes, can indicate a possible bile duct obstruction related to acute pancreatitis. This requires urgent medical evaluation and intervention.
Unexplained weight loss
Unintentional weight loss is a concerning symptom and may indicate underlying issues related to the pancreas or digestive system. If you are experiencing unexplained weight loss along with other symptoms, it is important to consult with a healthcare professional.
Worsening symptoms
If your symptoms worsen despite home care measures or if you are experiencing new or concerning symptoms, it is advisable to seek medical help. Proper evaluation and medical intervention can prevent complications or address any underlying issues.
Acute pancreatitis is a serious condition that requires prompt medical attention. Understanding the causes, symptoms, and treatment options is crucial for early detection and management. By adopting a healthy lifestyle, managing underlying medical conditions, and seeking timely medical help, individuals can reduce the risk of developing acute pancreatitis and its complications. Always consult with a healthcare professional for personalized advice and treatment.
Watch This Video Below
Related Terms About Understanding Acute Pancreatitis
Acute Pancreatitis Scoring System, Explain Acute Pancreatitis, How Do You Fix Acute Pancreatitis, Understanding Acute Pancreatitis, What Happens In Acute Pancreatitis, What Makes Acute Pancreatitis Worse