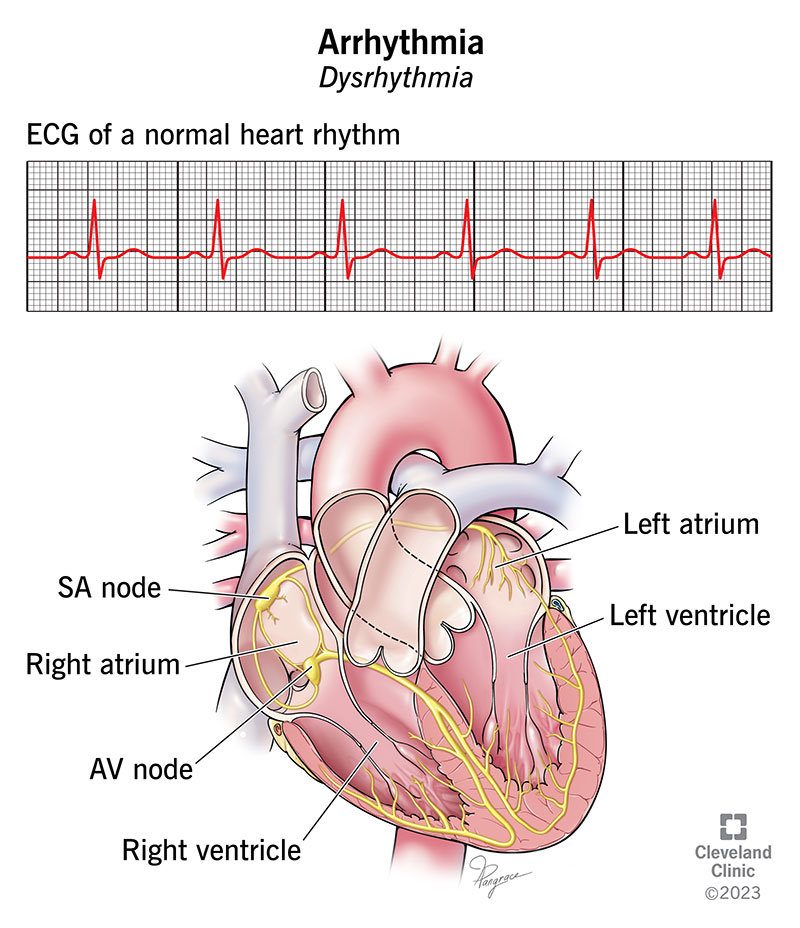
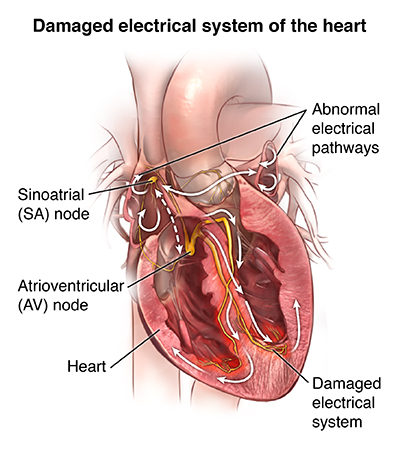
Arrhythmia, a condition characterized by an abnormal heart rhythm, can have a significant impact on one’s overall heart health. From irregular heartbeats to a faster or slower heartbeat than usual, this condition can lead to serious complications if left untreated. In this article, we will explore the various types of arrhythmia, the potential implications they can have on your heart, and the importance of seeking proper medical care to maintain a healthy heart rhythm.
1. Types of Arrhythmia
Arrhythmia refers to an abnormal rhythm of the heart, which can have various types and subtypes. Understanding the different types of arrhythmia is crucial in diagnosing and managing this condition effectively.
1.1 Atrial Fibrillation
Atrial fibrillation is the most common type of arrhythmia and occurs when the upper chambers of the heart (atria) beat irregularly and rapidly. This can lead to poor blood flow, increasing the risk of blood clots and stroke.
1.2 Ventricular Arrhythmia
Ventricular arrhythmia is characterized by abnormal rhythms originating from the lower chambers of the heart (ventricles). This condition can be life-threatening, causing the heart to pump ineffectively and potentially leading to sudden cardiac arrest.
1.3 Supraventricular Arrhythmia
Supraventricular arrhythmia encompasses various abnormal heart rhythms originating from areas above the ventricles. Examples include atrial flutter and paroxysmal supraventricular tachycardia (PSVT).
1.4 Bradycardia
Bradycardia occurs when the heart beats too slowly, depriving the body of adequate blood flow. This can result in symptoms such as fatigue, dizziness, and fainting.
1.5 Tachycardia
Tachycardia refers to a heart rate that is faster than normal. This increased heart rate can be harmless in some cases, but if sustained, it may increase the risk of complications like palpitations and reduced cardiac function.
1.6 Heart Block
Heart block is a condition where the electrical signals in the heart are delayed or blocked, disrupting the normal rhythm. It can range from minor to severe, and treatment may be required to restore normal heart function.
1.7 Premature Contractions
Premature contractions are additional heartbeats that occur before the regular heartbeat, often felt as a skipped or fluttering sensation. While usually harmless, frequent or prolonged premature contractions may require medical attention.
1.8 Sick Sinus Syndrome
Sick sinus syndrome refers to a group of arrhythmias caused by dysfunction of the sinus node, the heart’s natural pacemaker. It can lead to an irregular heart rate, alternating between bradycardia and tachycardia.
1.9 Long QT Syndrome
Long QT syndrome is a rare genetic disorder that affects the heart’s electrical system, causing an abnormal QT interval on an electrocardiogram (ECG). This condition can increase the risk of dangerous arrhythmias and sudden cardiac arrest.
1.10 Wolff-Parkinson-White Syndrome
Wolff-Parkinson-White syndrome is a congenital condition characterized by an extra electrical pathway between the atria and ventricles. This extra pathway can cause rapid heart rates and may require treatment to prevent complications.
2. Causes and Risk Factors
Arrhythmia can arise from various factors and underlying conditions. Understanding the causes and risk factors associated with arrhythmia can help identify potential triggers and guide appropriate treatment approaches.
2.1 Age
As we age, the risk of developing arrhythmia increases. The natural wear and tear on the heart’s electrical system, as well as age-related changes in the heart muscle, can contribute to the development of abnormal heart rhythms.
2.2 Heart Disease
Heart disease, including conditions such as coronary artery disease, heart failure, and previous heart attacks, can significantly increase the risk of arrhythmia. Damage to the heart muscle and impaired blood flow can disrupt the heart’s electrical system.
2.3 High Blood Pressure
Uncontrolled high blood pressure puts excessive strain on the heart, increasing the risk of arrhythmias. The constant elevated pressure can lead to thickening of heart muscle, compromising its ability to maintain a normal rhythm.
2.4 Thyroid Conditions
Thyroid disorders, particularly hyperthyroidism, where the thyroid gland produces excessive hormones, can disrupt the heart’s electrical system and increase the risk of arrhythmia.
2.5 Diabetes
Diabetes, especially when poorly controlled, can contribute to the development of arrhythmias. Uncontrolled blood sugar levels can damage the nerves and blood vessels supplying the heart, affecting its electrical signaling.
2.6 Excessive Alcohol or Caffeine Consumption
Excessive alcohol or caffeine intake can trigger arrhythmias. These substances can interfere with the heart’s electrical signals, causing abnormal rhythms and increasing the risk of complications.
2.7 Smoking
Smoking is a significant risk factor for various heart conditions, including arrhythmias. The chemicals in tobacco smoke can damage the heart muscle, narrow blood vessels, and disrupt the heart’s electrical system.
2.8 Drug or Medication Interactions
Certain medications, both prescription and over-the-counter, can interact with the heart’s electrical system and trigger arrhythmias. It is essential to disclose all medications to healthcare providers to minimize this risk.
2.9 Family History
A family history of arrhythmias or sudden cardiac death can increase an individual’s risk of developing arrhythmia. There may be genetic factors that predispose certain individuals to abnormal heart rhythms.
2.10 Stress and Anxiety
Chronic stress and anxiety can have a detrimental impact on heart health, increasing the risk of arrhythmias. Stress hormones released during periods of heightened anxiety can disrupt the heart’s electrical system.
3. Symptoms
Arrhythmias can cause a range of symptoms, from mild discomfort to severe complications. Recognizing these symptoms is crucial in seeking timely medical attention and appropriate management.
3.1 Palpitations
Palpitations refer to an awareness of the heart beating, often felt as a rapid or irregular heartbeat. This sensation can be unsettling and is a common symptom of arrhythmias.
3.2 Irregular Heartbeat
Arrhythmias can cause an irregular heartbeat, where the intervals between heartbeats are inconsistent. This irregularity can be detected by checking the pulse or during a physical examination by a healthcare professional.
3.3 Chest Pain or Discomfort
Some individuals may experience chest pain or discomfort during episodes of arrhythmia. This pain can vary in severity and may be accompanied by other symptoms.
3.4 Fatigue and Weakness
Arrhythmias can impact the heart’s ability to pump blood effectively, leading to reduced oxygen supply to the body’s tissues. This can result in fatigue and weakness, even with minimal physical exertion.
3.5 Dizziness or Fainting
When an arrhythmia affects blood flow to vital organs, such as the brain, it can cause dizziness or even loss of consciousness (syncope). These symptoms should never be ignored and require immediate medical attention.
3.6 Shortness of Breath
Arrhythmias can contribute to the accumulation of fluid in the lungs, causing shortness of breath and difficulty breathing, especially during physical activity or lying flat.
3.7 Anxiety
Experiencing arrhythmias can cause anxiety and have a significant impact on a person’s mental well-being. The fear of sudden cardiac events and the disruption caused by arrhythmias can lead to anxiety and increased stress levels.
4. Complications
Arrhythmias can lead to various complications, ranging from minor to life-threatening. Understanding these potential complications highlights the importance of early detection and appropriate management.
4.1 Blood Clots
Certain arrhythmias, such as atrial fibrillation, can cause blood to pool and clot within the heart chambers. These blood clots can break loose and travel to other parts of the body, leading to potentially fatal conditions, such as stroke or pulmonary embolism.
4.2 Stroke
Arrhythmias that disrupt blood flow and allow blood clots to form increase the risk of stroke. When a blood clot travels to the brain and blocks a blood vessel, it can cause an ischemic stroke, resulting in permanent damage or death of brain cells.
4.3 Heart Failure
Chronic arrhythmias can weaken the heart muscle, leading to heart failure. When the heart’s pumping function is impaired, it cannot effectively meet the body’s oxygen and nutrient needs, resulting in symptoms such as fatigue, fluid retention, and shortness of breath.
4.4 Sudden Cardiac Death
Certain arrhythmias, such as ventricular fibrillation, can cause sudden cardiac arrest. During this life-threatening event, the heart’s electrical system becomes chaotic, preventing effective pumping and leading to loss of consciousness and, if not promptly treated, death.
4.5 Syncope
Syncope, or fainting, can occur when the brain does not receive enough blood flow due to an arrhythmia. Fainting can have serious consequences, particularly if it occurs without warning or during hazardous activities such as driving.
4.6 Cardiomyopathy
Persistent arrhythmias can lead to structural changes in the heart muscle, resulting in cardiomyopathy. This condition weakens the heart’s pumping ability and can contribute to heart failure and other complications.
4.7 Pulmonary Edema
Arrhythmias that impair the heart’s ability to pump effectively can cause fluid to accumulate in the lungs, resulting in pulmonary edema. This can lead to breathlessness, coughing, and a feeling of suffocation.
4.8 Reduced Quality of Life
Living with arrhythmias can significantly impact an individual’s quality of life. The uncertainty surrounding episodes of arrhythmias, the need for lifestyle modifications, and the potential for complications can cause emotional distress and restrict daily activities.
4.9 Increased Risk of other Heart Conditions
Arrhythmias can increase the risk of developing other heart conditions, such as coronary artery disease and heart failure. Addressing arrhythmias promptly and effectively can help reduce the likelihood of these additional complications.
4.10 Impact on Mental Health
Living with arrhythmias can take a toll on an individual’s mental health. The worry and psychological burden of managing a chronic condition, as well as the impact of symptoms and potentially life-threatening events, can contribute to anxiety, depression, and reduced overall well-being.

5. Diagnosis
Accurate diagnosis of arrhythmias is crucial in determining the most appropriate treatment plan. Healthcare providers employ various diagnostic tools and tests to identify the presence and type of arrhythmia.
5.1 Medical History
Taking a detailed medical history enables healthcare providers to understand an individual’s symptoms, identify potential risk factors, and assess the need for further diagnostic tests. It is essential to provide a thorough account of symptoms, triggers, and any relevant medical conditions.
5.2 Physical Examination
A physical examination can help identify signs of arrhythmias, such as irregular heart sounds, abnormal pulses, or fluid accumulation. Healthcare providers may also listen for a heart murmur and assess overall cardiovascular health.
5.3 Electrocardiogram (ECG)
An electrocardiogram, or ECG, is a primary tool used to diagnose arrhythmias. It records the electrical activity of the heart and can detect irregular heart rhythms, abnormalities, and the overall health of the heart.
5.4 Holter Monitor
A Holter monitor is a portable device worn by the patient for a continuous period, usually 24 to 48 hours. It records the heart’s electrical activity during daily activities, allowing healthcare providers to assess heart rhythm over an extended period.
5.5 Event Recorder
Similar to a Holter monitor, an event recorder is a portable device used to record the heart’s electrical activity for an extended period. However, it is typically used for shorter durations, usually when symptoms occur, allowing individuals to activate the device when symptoms arise.
5.6 Echocardiogram
An echocardiogram utilizes sound waves to create images of the heart’s structure and function. It can help identify underlying structural abnormalities, evaluate the heart’s pumping function, and assess the impact of arrhythmias on cardiac health.
5.7 Stress Test
A stress test, also known as an exercise test, evaluates the heart’s response to physical activity. It can help determine if certain arrhythmias appear or worsen during exertion, providing valuable insights into the heart’s function under stress.
5.8 Electrophysiology Study (EPS)
Electrophysiology studies involve the placement of catheters within the heart to assess its electrical system. This invasive procedure provides detailed information about specific arrhythmias, their origin, and potential treatment options.
5.9 Blood Tests
Blood tests may be conducted to evaluate certain parameters related to heart health, such as levels of electrolytes, thyroid hormones, and cardiac enzymes. These tests can help identify underlying conditions or imbalances contributing to arrhythmias.
5.10 Genetic Testing
In some cases, genetic testing may be recommended to identify inherited arrhythmia syndromes or specific genetic mutations predisposing individuals to abnormal heart rhythms. This testing can assist in tailored treatment plans and identification of familial risks.
6. Treatment Options
The treatment approach for arrhythmias depends on the type, severity, underlying causes, and individual patient factors. Treatment aims to manage symptoms, reduce complications, and improve overall quality of life.
6.1 Lifestyle Changes
Lifestyle modifications are often the first-line approach in managing arrhythmias. These may include quitting smoking, reducing alcohol and caffeine intake, managing stress levels, maintaining a healthy weight, and engaging in regular physical activity.
6.2 Medications
Medications play a crucial role in managing arrhythmias. Antiarrhythmic drugs can help restore and maintain a normal heart rhythm. Other medications may be prescribed to manage underlying conditions contributing to arrhythmias, such as high blood pressure or thyroid disorders.
6.3 Cardioversion
Cardioversion is a procedure that uses controlled electrical shocks or medications to restore a normal heart rhythm in certain types of arrhythmias. This can be done as a planned procedure or in urgent situations when an arrhythmia is life-threatening.
6.4 Catheter Ablation
Catheter ablation involves the insertion of thin, flexible wires (catheters) into the heart to destroy abnormal heart tissue responsible for causing arrhythmias. This procedure aims to eliminate or significantly reduce the occurrence of arrhythmias.
6.5 Implantable Cardioverter-Defibrillators (ICDs)
ICDs are small devices implanted under the skin to monitor heart rhythms and deliver electrical shocks if a life-threatening arrhythmia occurs. ICDs are typically recommended for individuals at high risk of sudden cardiac arrest.
6.6 Pacemakers
Pacemakers are devices implanted under the skin to help regulate the heart’s rhythm. They deliver electrical signals to the heart when it beats too slowly or irregularly, helping to maintain an appropriate heart rate.
6.7 Surgery
Surgical interventions may be considered in certain cases of arrhythmias that do not respond to other treatment modalities. Surgical options can include maze procedures, which create scar tissue to redirect electrical signals, or heart valve repairs/replacements that can improve overall heart function.
6.8 Lifestyle Management
Adopting healthy lifestyle habits is crucial in managing arrhythmias. This includes maintaining a balanced diet, regular exercise, stress management techniques, and getting adequate sleep. Lifestyle management can significantly reduce the severity and frequency of arrhythmias.
6.9 Complementary and Alternative Medicine
Some individuals find relief from arrhythmia symptoms through complementary and alternative approaches. These may include techniques such as acupuncture, yoga, meditation, and herbal supplements. While they may provide symptom relief for some, it is essential to consult with a healthcare professional before initiating any such treatments.
6.10 Clinical Trials
Participating in clinical trials can provide individuals with access to innovative treatments and contribute to the advancement of arrhythmia research. Clinical trials evaluate new medications, procedures, or devices that have shown potential benefits for managing arrhythmias.

7. Prevention
Preventing the occurrence or recurrence of arrhythmias is essential for maintaining optimal heart health. Implementing preventive measures can significantly reduce the risk and severity of arrhythmias.
7.1 Healthy Lifestyle
Adopting a healthy lifestyle is fundamental in preventing arrhythmias. This entails maintaining a balanced diet, limiting alcohol and caffeine consumption, avoiding smoking, and managing stress levels effectively.
7.2 Regular Exercise
Engaging in regular physical activity is crucial for overall heart health. Regular exercise helps maintain a healthy weight, promotes cardiovascular fitness, and reduces the risk of developing heart conditions, including arrhythmias.
7.3 Balanced Diet
A well-balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats provides the necessary nutrients for maintaining heart health. Limiting sugary, processed foods and excessive sodium intake can also help prevent arrhythmias.
7.4 Stress Management
Effective stress management techniques, such as relaxation exercises, meditation, and regular stress-reducing activities, can help prevent stress-related arrhythmias. Finding healthy coping mechanisms is essential for maintaining optimal heart health.
7.5 Avoidance of Triggers
Identifying and avoiding triggers that contribute to arrhythmias is crucial for prevention. These may include excessive alcohol or caffeine consumption, certain medications or substances, and activities or situations that induce anxiety or stress.
7.6 Medication Adherence
If medications have been prescribed to manage underlying conditions or arrhythmias, it is essential to take them as directed by healthcare providers. Adhering to prescribed medication regimens can significantly reduce the risk of arrhythmia recurrence.
7.7 Regular Medical Check-ups
Maintaining regular medical check-ups allows healthcare providers to monitor heart health, identify potential risks, and make necessary adjustments to treatment plans. Routine screening tests and evaluations can help detect arrhythmias early.
7.8 Vaccination
Immunizations, such as receiving the influenza and pneumococcal vaccines, are recommended for individuals with arrhythmias. Preventing infectious diseases can reduce the strain on the heart and minimize the risk of arrhythmia complications.
7.9 Genetic Counseling
In individuals with a known genetic predisposition to arrhythmias, seeking genetic counseling can provide valuable information about the risks, potential treatment options, and family planning considerations. Genetic counseling can help individuals make informed decisions and take proactive steps in managing their conditions.
7.10 Avoidance of Drug or Alcohol Abuse
Illicit drug use and excessive alcohol consumption can significantly increase the risk of developing arrhythmias. Avoiding these substances or seeking appropriate help and treatment for substance abuse is crucial in preventing the onset of arrhythmias.
8. Management of Underlying Conditions
Addressing underlying conditions that contribute to the development or exacerbation of arrhythmias plays a crucial role in effectively managing these abnormal heart rhythms.
8.1 Hypertension
Managing high blood pressure through lifestyle modifications and, if necessary, antihypertensive medication can help reduce the risk of arrhythmias. Regular blood pressure monitoring and adherence to recommended treatment plans are essential.
8.2 Hyperthyroidism
Effective management of hyperthyroidism, such as through medication, radioactive iodine treatment, or surgery, can help restore normal heart function and reduce the risk of arrhythmias associated with this condition.
8.3 Diabetes
Maintaining optimal blood sugar control through lifestyle modifications, medication adherence, and regular monitoring is crucial in managing diabetes-related arrhythmias. Close collaboration with healthcare providers is essential in achieving and maintaining stable blood sugar levels.
8.4 Coronary Artery Disease
Treating underlying coronary artery disease, such as with lifestyle changes, medications, or invasive procedures like angioplasty or bypass surgery, can help improve blood flow to the heart and reduce the risk of arrhythmias.
8.5 Heart Failure
Addressing heart failure through medications, lifestyle adaptations, and, in severe cases, advanced therapies like heart transplantation or mechanical circulatory support, can help reduce the risk of arrhythmias and improve overall heart function.
8.6 Sleep Apnea
Managing sleep apnea, typically through interventions such as continuous positive airway pressure (CPAP) therapy, can help reduce the occurrence of arrhythmias. Restoring normal breathing during sleep minimizes the strain on the heart and improves cardiac rhythm stability.
8.7 Anxiety and Stress
Treating anxiety and stress-related disorders through psychotherapy, medications, or relaxation techniques can help minimize the occurrence of stress-related arrhythmias. Learning healthy coping mechanisms and stress management strategies is crucial for overall heart health.
8.8 Substance Abuse Disorders
Addressing substance abuse disorders through appropriate rehabilitation programs, therapy, and support systems is essential in managing arrhythmias. Sobriety and abstinence from illicit substances significantly reduce the risk of these abnormal heart rhythms.
8.9 Nutritional Deficiencies
Correcting nutritional deficiencies, such as deficiencies in electrolytes like potassium and magnesium, can help restore normal cardiac function and reduce the risk of arrhythmias. Healthcare providers may recommend dietary changes or supplements to address specific deficiencies.
8.10 Hormonal Imbalances
In cases where hormonal imbalances contribute to arrhythmias, treatment options may involve hormone replacement therapy or medications to regulate hormone levels. Close monitoring and collaboration with healthcare providers are necessary for optimal management.

9. Importance of Regular Follow-up
Regular follow-up with healthcare providers is crucial in effectively managing arrhythmias, evaluating treatment efficacy, and preventing complications. This ongoing collaboration ensures appropriate treatment adjustments and comprehensive care.
9.1 Monitoring Symptom Progression
Regular follow-up evaluations allow healthcare providers to monitor symptom progression and identify changes that may require adjustments in treatment plans. This ensures that the most appropriate management strategies are implemented as the condition evolves.
9.2 Medication Adjustments
The effectiveness of medications in managing arrhythmias may change over time. Regular follow-up appointments enable healthcare providers to assess medication efficacy, make necessary adjustments, and explore alternative options if needed.
9.3 Identification of Complications
Regular monitoring helps detect any potential complications related to arrhythmias. Through comprehensive evaluations, healthcare providers can identify signs of blood clots, heart failure, or other adverse events, enabling timely intervention and prevention of serious complications.
9.4 Lifestyle Evaluation
Ongoing assessment of lifestyle habits and behaviors is essential in managing arrhythmias. Follow-up appointments provide an opportunity to discuss the effectiveness of lifestyle modifications, address challenges, and make necessary adjustments to optimize heart health.
9.5 Psychological Support
Living with a chronic condition like arrhythmia can have a significant psychological impact. Regular follow-up allows healthcare providers to offer emotional support, evaluate mental well-being, and refer individuals to appropriate resources for counseling or therapy, if necessary.
9.6 Engagement in Treatment Plan
Maintaining regular follow-up appointments fosters greater engagement in the treatment plan. It allows individuals to actively participate in shared decision-making, ask questions, address concerns, and actively manage their condition alongside the healthcare team.
9.7 Education and Awareness
Follow-up appointments serve as an opportunity for healthcare providers to educate individuals about arrhythmias, treatment options, and lifestyle modifications. Building knowledge and awareness empowers individuals to take charge of their heart health and make informed decisions.
9.8 Prevention of Recurrence
By actively monitoring the effectiveness of treatment interventions, healthcare providers can identify factors contributing to arrhythmia recurrence. Regular follow-up facilitates targeted prevention strategies tailored to each individual’s unique situation, reducing the likelihood of arrhythmia recurrence.
9.9 Collaboration with Healthcare Team
Regular follow-up appointments foster collaboration between individuals and their healthcare team. Open communication enables the sharing of information, enhances treatment coordination, and ensures that all aspects of arrhythmia management are addressed comprehensively.
9.10 Early Intervention
Prompt identification of potential changes, complications, or symptoms during follow-up appointments allows for early intervention. This proactive approach helps prevent the progression of arrhythmias, mitigates the risk of complications, and improves long-term outcomes.
10. Research and Advances
Ongoing research and technological advancements continue to enhance the understanding, diagnosis, and treatment of arrhythmias. Innovations in medical science offer promising avenues for improving the lives of individuals with arrhythmias.
10.1 Pharmacological Innovations
The development of new and improved antiarrhythmic medications aims to enhance treatment efficacy, reduce side effects, and allow for more personalized approaches. Ongoing research explores novel drug targets and delivery systems to optimize arrhythmia management.
10.2 Device Technologies
Advancements in device technologies, such as implantable devices and remote monitoring systems, have revolutionized the management of arrhythmias. Smaller, more efficient devices, along with sophisticated software, enable precise monitoring, better treatment optimization, and improved patient outcomes.
10.3 Novel Surgical Techniques
Innovative surgical techniques, such as minimally invasive procedures and robotic-assisted surgery, continue to evolve in the field of arrhythmia management. These techniques aim to improve treatment outcomes, reduce recovery times, and enhance patient comfort.
10.4 Genetic Studies
Continued research into the genetic basis of arrhythmias has enabled the identification of specific gene mutations associated with certain arrhythmia syndromes. Genetic studies contribute to personalized treatment approaches, genetic counseling, and improved prognostication.
10.5 Stem Cell Research
Stem cell research holds promising potential for regenerative therapies in arrhythmia management. The use of stem cells to repair damaged heart tissue and restore cardiac function offers hope for individuals with arrhythmias and other cardiac conditions.
10.6 Artificial Intelligence in Diagnosis and Management
The application of artificial intelligence (AI) techniques in arrhythmia diagnosis and management is an emerging field. AI algorithms can analyze vast amounts of patient data, aid in accurate arrhythmia detection, and improve treatment decision-making.
10.7 Telemedicine
Telemedicine has gained popularity, especially in the context of arrhythmia management. Remote monitoring systems, virtual consultations, and wearable devices allow for efficient ongoing care, empowering individuals to actively engage in their treatment from the comfort of their homes.
10.8 Wearable Devices
Advancements in wearable devices, such as smartwatches and fitness trackers, provide real-time monitoring capabilities for individuals with arrhythmias. These devices can detect irregular heart rhythms, track physical activity, and transmit data to healthcare providers for evaluation.
10.9 Big Data and Analytics
The use of big data analytics allows for the analysis of vast datasets to identify patterns, risk factors, and treatment outcomes related to arrhythmias. Leveraging data analytics can help improve diagnosis, treatment guidelines, and overall patient care.
10.10 Patient Empowerment through Education and Support
Enhanced patient education and support systems play a critical role in empowering individuals with arrhythmias. Educational resources, support groups, and online communities provide valuable information, emotional support, and encouragement for self-management.
In conclusion, arrhythmias encompass a diverse range of abnormal heart rhythms and can significantly impact an individual’s heart health. Understanding the types, causes, and risk factors associated with arrhythmias is vital in diagnosis, management, and prevention. With advances in research, technology, and treatment options, individuals with arrhythmias can benefit from tailored approaches, improved outcomes, and a better quality of life. Regular follow-up, lifestyle modifications, and proper management of underlying conditions are key components in effectively addressing arrhythmias and minimizing the risk of complications. With ongoing scientific progress, the future holds promising advancements that will continue to transform the landscape of arrhythmia care.