If you’ve been struggling with joint pain, you’re not alone. Dealing with discomfort in your joints can be frustrating and impact your daily life. However, there are ways to manage joint pain and find relief. In this article, we’ll explore some helpful tips and strategies that can make a significant difference in minimizing your discomfort. Whether you’re looking for lifestyle changes, exercises, or natural remedies, we’ve got you covered. Say goodbye to the limitations imposed by joint pain and get ready to regain control of your life.
Overview of Joint Pain
Joint pain refers to discomfort, aching, or soreness in any of the body’s joints. It can affect any part of the body where two or more bones meet, such as the knees, hips, shoulders, and wrists. Joint pain can range from mild to severe and can be temporary or chronic. It is a common problem that can occur at any age and may be accompanied by swelling, stiffness, and limited mobility.
What is joint pain?
Joint pain, also known as arthralgia, can be caused by a variety of factors. It occurs when the structures around the joint, including the bones, ligaments, tendons, and muscles, are affected. Common causes of joint pain include injury, inflammation, infection, autoimmune diseases (such as rheumatoid arthritis), wear and tear of cartilage (such as osteoarthritis), and other underlying medical conditions.
Common causes of joint pain
There are several common causes of joint pain:
- Osteoarthritis: This is the most common form of arthritis and occurs when the protective cartilage that cushions the ends of bones wears down over time.
- Rheumatoid arthritis: An autoimmune disorder in which the body’s immune system mistakenly attacks the joints, causing inflammation and pain.
- Gout: A form of arthritis caused by the buildup of uric acid crystals in the joints, leading to sudden and severe pain, often in the big toe.
- Injury: Joint pain can be the result of acute or chronic injuries, such as fractures, sprains, strains, or dislocations.
- Bursitis: Inflammation of the bursae, small fluid-filled sacs that cushion the joints, can cause joint pain.
- Tendinitis: Inflammation of the tendons, which connect muscles to bones, can result in joint pain.
- Infections: Joint pain can be a symptom of various types of infections, including viral, bacterial, or fungal infections.
- Fibromyalgia: A chronic disorder characterized by widespread musculoskeletal pain, fatigue, and tender points.
- Lupus: An autoimmune disease that can affect multiple organs, including the joints, causing inflammation and pain.
Signs and symptoms of joint pain
The signs and symptoms of joint pain can vary depending on the underlying cause and the specific joint affected. Common symptoms associated with joint pain may include:
- Pain or discomfort in the affected joint(s)
- Swelling or inflammation
- Stiffness and decreased range of motion
- Redness or warmth around the joint
- Joint instability or locking
- Muscle weakness or imbalances
- Difficulty performing daily activities or tasks requiring joint mobility
It is important to consult a healthcare professional for an accurate diagnosis and appropriate treatment options if you experience persistent or worsening joint pain.
Diagnosing Joint Pain
When you visit a healthcare professional for joint pain, they will typically perform a thorough medical history and physical examination to gather information about your symptoms, previous injuries, and overall health. This initial assessment helps in identifying potential underlying causes of the joint pain and guides further diagnostic testing or the need to consult a specialist.
Medical history and physical examination
During the medical history interview, your healthcare provider may ask specific questions about your joint pain, such as when it started, how long it has been present, the severity, any associated symptoms, and any factors that seem to worsen or alleviate the pain. They may also ask about your medical history, including any previous injuries, surgeries, or conditions that may contribute to the joint pain.
Following the medical history, a physical examination of the affected joint(s) and other relevant body systems will be conducted. This examination helps evaluate the joint’s range of motion, any swelling or tenderness, muscle strength, and overall joint stability. Your healthcare provider may also perform specific maneuvers or tests to further assess the joint’s integrity and function.
Diagnostic tests
In addition to the medical history and physical examination, your healthcare provider may order diagnostic tests to help identify the cause of your joint pain. These tests can include:
- X-rays: X-ray imaging can provide detailed pictures of the bones and identify any structural abnormalities, fractures, or signs of arthritis.
- Magnetic Resonance Imaging (MRI): This imaging technique uses magnetic fields to create detailed images of the soft tissues, such as cartilage, tendons, and ligaments, providing a more comprehensive view of the joint’s internal structures.
- Ultrasound: Ultrasound imaging uses sound waves to create real-time images of the joint and surrounding soft tissues. It can help detect fluid buildup, inflammation, or other abnormalities.
- Blood tests: Blood tests, such as complete blood count (CBC), erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), and specific autoimmune markers, can help assess inflammation levels and identify autoimmune or infectious causes of joint pain.
- Joint aspiration: In some cases, a small sample of fluid may be drawn from the affected joint using a needle for further evaluation. This procedure can help diagnose infections, gout, or other conditions causing joint inflammation.
- Other specialized tests: Depending on the suspected underlying cause, your healthcare provider may order additional tests, such as computed tomography (CT) scans, bone scans, or joint arthroscopy, to gather more detailed information about the joint.
Consulting a specialist
If the initial evaluation and diagnostic tests do not provide a clear diagnosis or if the joint pain persists despite conservative management, your healthcare provider may refer you to a specialist, such as a rheumatologist, orthopedic surgeon, or physical therapist. These healthcare professionals have specialized knowledge and expertise in diagnosing and managing joint-related conditions and can provide tailored treatment options and recommendations based on your specific needs.

Tips for Preventing Joint Pain
While joint pain can be a common and challenging issue, there are several preventive measures you can take to reduce the risk of joint pain and maintain joint health. Incorporating these tips into your lifestyle can contribute to your overall well-being and help promote healthy joints.
Maintain a healthy weight
Maintaining a healthy weight is crucial for joint health, as excess weight can put added stress on the joints, leading to increased wear and tear. By maintaining a healthy weight through a balanced diet and regular exercise, you can help reduce the strain on your joints, especially weight-bearing joints like the knees and hips.
Exercise regularly
Regular exercise is essential for maintaining joint health and flexibility. Engaging in low-impact exercises, such as swimming, cycling, and walking, can help strengthen the muscles around the joints, improve range of motion, and promote joint stability. It is important to consult with a healthcare professional or a certified fitness trainer to develop an exercise routine tailored to your specific needs and capabilities.
Avoid repetitive movements
Repetitive movements, such as constant typing or gripping activities, can put stress on the joints and increase the risk of developing joint pain or conditions like carpal tunnel syndrome. Whenever possible, take breaks, vary your tasks, and practice proper ergonomics to minimize the strain on your joints.
Wear appropriate footwear
Wearing appropriate footwear that provides adequate support and cushioning is crucial for joint health, especially for weight-bearing joints like the knees and feet. Look for shoes that fit properly, have shock-absorbing soles, and offer good arch support. Avoid high heels or shoes with insufficient padding, as they can increase the risk of joint pain and other foot-related problems.
Practice good posture
Maintaining good posture is essential for reducing stress on your joints, especially in the spine, neck, and shoulders. Be mindful of your posture while sitting, standing, or performing daily activities, and make adjustments as needed to ensure proper alignment of your joints. Incorporating exercises and stretches that promote posture and core strength, such as yoga or Pilates, can also be beneficial.
Lifestyle Changes to Manage Joint Pain
Joint pain can significantly impact daily activities and quality of life. While medical interventions and therapies play a crucial role in managing joint pain, certain lifestyle changes can also help alleviate symptoms and improve overall well-being.
Manage stress levels
Chronic stress can contribute to inflammation and exacerbate joint pain. Implementing stress management techniques, such as deep breathing exercises, meditation, or engaging in hobbies or activities that you enjoy, can help reduce stress levels and promote relaxation, which can positively impact joint pain management.
Get enough sleep
Adequate and quality sleep is essential for the body’s healing and repair processes, including joint health. Establish a regular sleep routine, create a comfortable sleep environment, and prioritize getting seven to eight hours of uninterrupted sleep each night. If joint pain disrupts your sleep, consider using pillows or support cushions to relieve pressure on the affected joints.
Eat a balanced diet
A healthy and balanced diet rich in nutrients can support joint health and reduce inflammation. Include foods high in omega-3 fatty acids, such as fatty fish (salmon, mackerel), flaxseeds, chia seeds, and walnuts, as these have anti-inflammatory properties. Additionally, incorporate plenty of fruits, vegetables, whole grains, lean proteins, and low-fat dairy products to provide essential vitamins, minerals, and antioxidants that support overall joint health.
Use assistive devices
Assistive devices can help alleviate joint stress and reduce pain during daily activities. For example, using a cane, crutches, or a walker can provide support and stability for weight-bearing joints. Utilizing ergonomic tools, such as jar openers or reachers, can reduce joint strain and improve functionality. Consult with an occupational therapist or healthcare professional for personalized recommendations on assistive devices based on your specific needs.
Apply hot and cold therapy
Hot and cold therapy techniques can provide temporary relief from joint pain. Applying a hot pack or taking a warm shower can help relax muscles and increase blood flow to the affected area, reducing stiffness and promoting healing. On the other hand, using a cold pack or ice wrapped in a towel can numb the area and reduce inflammation and swelling. Alternate between hot and cold therapy for the desired effect, and always use a barrier (towel or cloth) between the skin and the heat or cold source to prevent skin damage.
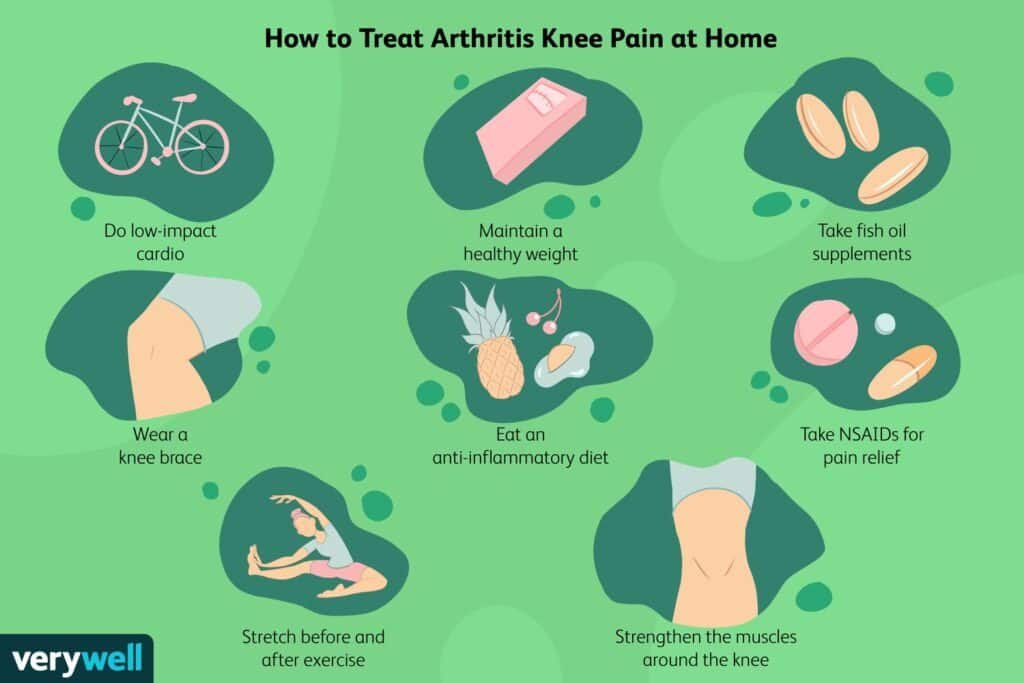
Home Remedies for Joint Pain Relief
In addition to lifestyle changes, several home remedies can provide temporary relief from joint pain. These remedies can be used as complementary therapies alongside medical treatments, but it is important to consult with a healthcare professional before trying any new treatments, especially if you have underlying medical conditions or take medications.
Apply topical creams and ointments
Topical creams and ointments containing ingredients like menthol, capsaicin, or salicylates can provide localized relief from joint pain. These products work by numbing the area or by promoting blood flow, reducing inflammation, and providing a soothing sensation. Follow the instructions on the product packaging and consult a healthcare professional if you have any concerns or allergies.
Use over-the-counter pain relievers
Over-the-counter (OTC) pain relievers, such as acetaminophen or nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen, can help reduce joint pain and inflammation. When using OTC medications, it is important to follow the recommended dosage and instructions and consult with a healthcare professional if you have any underlying medical conditions or take other medications that may interact with these drugs.
Try natural supplements
Certain natural supplements have been suggested to provide relief from joint pain. Glucosamine and chondroitin are commonly used supplements that may help reduce symptoms of joint pain and slow down the progression of certain joint conditions. However, the evidence is mixed, and it is important to consult with a healthcare professional before starting any new supplements, as they may interact with other medications or medical conditions.
Apply heat compresses
Applying a heat compress, such as a warm towel or a heating pad, to the affected joint can help relax muscles, improve blood circulation, and temporarily alleviate joint pain. Ensure that the heat is not too intense to avoid burns or skin damage. Limit the application of heat to around 20 minutes at a time and use caution if you have reduced sensation or are unable to sense temperature changes normally.
Take warm baths
Soaking in a warm bath with added Epsom salts or essential oils can provide relaxation and temporary pain relief for achy joints. The warm water helps relax muscles and increase blood flow to the joints, reducing stiffness and promoting recovery. Ensure the water is not too hot to avoid burns, and monitor the time spent in the water to prevent dehydration or lightheadedness.
Medications for Joint Pain
In some cases, medications may be prescribed to manage joint pain, particularly when lifestyle modifications and home remedies are insufficient. The choice of medication depends on the underlying cause, severity of pain, and individual factors. It is important to consult with a healthcare professional before starting or changing any medications, as they can have potential side effects or interact with other medications.
Nonsteroidal anti-inflammatory drugs (NSAIDs)
NSAIDs, such as ibuprofen, naproxen, or aspirin, are commonly used medications to reduce joint pain and inflammation. They work by inhibiting prostaglandins, substances that contribute to inflammation and pain. NSAIDs are available over-the-counter or in higher strengths by prescription, and their use should be monitored, especially if you have a history of gastrointestinal or cardiovascular conditions.
Corticosteroids
Corticosteroids, such as prednisone or cortisone, are powerful anti-inflammatory medications that may be prescribed to manage severe joint pain or inflammation. They are usually administered orally, by injection into the joint (intra-articular), or applied topically as creams or ointments. Corticosteroids should be used under the guidance of a healthcare professional, as they have potential side effects, particularly with long-term use.
Disease-modifying antirheumatic drugs (DMARDs)
DMARDs are a class of medications commonly used in the treatment of autoimmune diseases like rheumatoid arthritis. They work by suppressing the immune system to reduce inflammation and slow down the progression of joint damage. DMARDs can take several weeks to months to produce noticeable effects and should be closely monitored by a healthcare professional due to potential side effects, such as liver or kidney toxicity.
Analgesics
Analgesics, such as acetaminophen, provide pain relief without reducing inflammation. They are commonly used for mild to moderate joint pain and can be purchased over-the-counter. Analgesics can be a suitable option for individuals who cannot tolerate NSAIDs or have health conditions that may interact or restrict the use of other pain medications.
Biologic response modifiers
Biologic response modifiers, also known as biologic drugs or biologics, are a relatively newer class of medications used to manage joint pain, primarily in autoimmune diseases like rheumatoid arthritis or psoriatic arthritis. These medications target specific molecules in the immune system to reduce inflammation and slow down joint damage. Biologics are typically administered by injection or infusion and require regular monitoring due to potential side effects.

Physical Therapy for Joint Pain
Physical therapy plays a significant role in the management of joint pain and can help improve joint function, reduce pain, and enhance overall quality of life. A physical therapist, following a comprehensive evaluation, can develop an individualized treatment plan that may include various modalities and exercises based on the specific joint affected and the underlying cause.
Range-of-motion exercises
Range-of-motion exercises aim to maintain or improve the joint’s full range of motion by stretching and moving it in various directions. These exercises help prevent joint stiffness and improve joint flexibility, allowing for better functional mobility. A physical therapist can guide you through specific exercises targeting the affected joint(s), ensuring safety and effectiveness.
Strengthening exercises
Strengthening exercises focus on improving muscle strength around the joint, which helps support and stabilize the joint and reduces additional stress. These exercises can be tailored to the individual’s needs and may include resistance training, weightlifting, or exercises using resistance bands. A physical therapist can guide you in performing appropriate exercises that target the muscles supporting the affected joint(s) without exacerbating pain.
Low-impact aerobic exercises
Low-impact aerobic exercises are beneficial for joint health, cardiovascular fitness, and overall well-being. Activities such as walking, biking, swimming, or using an elliptical machine involve rhythmic, low-impact movements that minimize stress on the joints while improving cardiovascular endurance. A physical therapist can help you incorporate these exercises into your routine, ensuring proper form and intensity.
Manual therapy techniques
Manual therapy techniques, performed by a physical therapist or other trained healthcare professional, involve specialized hands-on techniques to improve joint mobility, reduce muscular tension, and alleviate pain. These techniques may include joint mobilization, soft tissue mobilization, or manual stretching. Manual therapy can provide immediate pain relief and improve joint function, especially when used in conjunction with other therapy approaches.
Splinting or bracing
Splinting or bracing can provide additional support and stability to the affected joint during activities or rest, depending on the specific joint and condition. Splints or braces can help protect the joint, reduce pain, and minimize further damage or degeneration. A physical therapist or orthopedic specialist can recommend appropriate splints or braces and provide instructions on their application and usage.
Alternative Treatments for Joint Pain
In addition to conventional medical treatments and physical therapy, several alternative treatments may offer relief from joint pain. These approaches are considered as complementary therapies and should be used under the guidance of trained healthcare professionals.
Acupuncture
Acupuncture is an ancient Chinese therapy that involves the insertion of thin needles into specific points on the body to stimulate energy flow and promote healing. It is believed to help reduce pain and inflammation, improve joint function, and release endorphins, the body’s natural painkillers. Acupuncture should be performed by a licensed acupuncturist who can assess your condition and tailor the treatment accordingly.
Massage therapy
Massage therapy involves the manipulation of soft tissues, such as muscles and tendons, to improve blood circulation, reduce muscle tension, and promote relaxation. It can help reduce joint pain, increase joint mobility, and improve overall well-being. Seek a licensed massage therapist with experience in joint-related conditions to ensure appropriate techniques and safety precautions.
Chiropractic care
Chiropractic care focuses on the diagnosis, treatment, and prevention of disorders of the musculoskeletal system, particularly the spine. Chiropractors use manual techniques, such as spinal adjustments or manipulations, to correct misalignments and improve joint function. Chiropractic care may be beneficial for certain joint-related conditions, but it is important to consult with a licensed chiropractor and inform them about your specific joint pain issues.
Herbal medicine
Herbal medicine, also known as botanical medicine or herbalism, involves the use of plant-based remedies to treat various ailments. Certain herbs, such as turmeric, ginger, boswellia, and devil’s claw, have been traditionally used for their potential anti-inflammatory and pain-relieving properties. However, it is important to consult with a healthcare professional or an experienced herbalist before incorporating any herbal supplements or remedies, as they may interact with medications or have potential side effects.
Meditation and relaxation techniques
Meditation and relaxation techniques, such as deep breathing exercises, mindfulness, or guided imagery, can help reduce stress, promote relaxation, and potentially alleviate joint pain. These techniques focus on redirecting attention and promoting a sense of calmness, which can positively impact pain perception and overall well-being. Consider seeking guidance from a meditation instructor or participating in meditation programs or classes to learn and practice these techniques effectively.

Surgical Options for Joint Pain
In cases where conservative treatments have been unsuccessful or the joint damage is severe, surgical interventions may be recommended to alleviate joint pain and restore function. Surgical options vary depending on the affected joint, the underlying condition, and the individual’s specific needs and circumstances. It is important to consult with an orthopedic surgeon or a healthcare professional to determine the most appropriate surgical approach.
Arthroscopy
Arthroscopy is a minimally invasive surgical procedure used to diagnose and treat joint problems. It involves inserting a thin, flexible tube with a small camera (arthroscope) through small incisions in the joint to visualize the joint structures. Arthroscopy allows for the removal of damaged cartilage, loose bodies, or repair of torn ligaments or tendons, thereby relieving joint pain and improving function.
Joint replacement surgery
Joint replacement surgery, also known as arthroplasty, involves removing the damaged joint surfaces and replacing them with artificial components made of metal, plastic, or ceramic. This surgical procedure is commonly performed for severe joint pain and limited joint mobility due to conditions like osteoarthritis or rheumatoid arthritis. Joint replacement surgery can significantly relieve joint pain and improve overall joint function and mobility.
Joint fusion
Joint fusion, also known as arthrodesis, involves permanently fusing the joint surfaces together to create a stable, pain-free joint. This surgical procedure is typically performed for joints severely damaged by conditions like arthritis or trauma. Joint fusion eliminates joint pain but significantly limits joint movement and mobility. It is usually considered for joints that do not require a wide range of motion for everyday activities.
Joint resurfacing
Joint resurfacing is a surgical procedure that involves reshaping the damaged joint surfaces while preserving most of the natural joint structures. This procedure is commonly used for joints affected by conditions like osteoarthritis or avascular necrosis. Joint resurfacing aims to alleviate joint pain, improve joint function, and delay or avoid a total joint replacement, particularly in younger patients.
Osteotomy
Osteotomy is a surgical procedure that involves cutting and repositioning the bones around a joint to redistribute the weight-bearing forces, relieve joint pain, and improve alignment. This procedure is commonly performed for joint conditions affecting the lower extremities, such as osteoarthritis of the knee or hip. Osteotomy aims to delay the need for joint replacement surgery and can be beneficial for younger patients with localized joint damage.
Supportive Resources for Joint Pain
Living with joint pain can be physically and emotionally challenging. Engaging with supportive resources can provide valuable information, emotional support, and practical advice for individuals dealing with joint pain.
Joining support groups
Support groups for individuals with joint pain or specific joint-related conditions can provide a sense of community, understanding, and shared experiences. These groups, whether in-person or online, offer opportunities to connect with others facing similar challenges, share information, and learn from each other’s experiences. Ask your healthcare provider or search online for local support groups or online communities related to your specific condition.
Seeking emotional support
Dealing with chronic joint pain can take a toll on mental and emotional well-being. It is important to seek emotional support from family, friends, or professionals who can provide understanding, empathy, and encouragement. Consider talking to a counselor, therapist, or psychologist experienced in chronic pain management to help process emotions, develop coping strategies, and improve overall mental well-being.
Finding online resources
The internet provides a wealth of information on joint pain, including reputable websites, blogs, and forums dedicated to joint health and management. These online resources can provide helpful tips, educational materials, and the latest developments in joint pain management. However, it is important to critically evaluate the information and consult with a healthcare professional for personalized advice and recommendations.
Consulting patient advocacy organizations
Patient advocacy organizations are dedicated to supporting individuals with specific medical conditions or diseases, including joint-related conditions. These organizations provide valuable resources, educational materials, and advocacy efforts to promote patient rights and raise awareness about joint pain conditions. Reach out to relevant patient advocacy organizations related to your specific condition for support, information, and potential networking opportunities.
Medical insurance and financial assistance
Managing joint pain can involve various medical treatments, therapies, and medications, which can incur significant healthcare costs. It is important to understand your medical insurance coverage and benefits to ensure access to necessary treatments and medications. Additionally, explore financial assistance programs, foundations, or grants that may provide support for individuals with joint pain or specific joint-related conditions.
In conclusion, joint pain is a common problem that can have a significant impact on daily activities and overall quality of life. While there are various causes of joint pain, many preventive measures, lifestyle changes, home remedies, medical treatments, physical therapy, and alternative therapies can help manage joint pain and improve joint function. It is important to consult with a healthcare professional for an accurate diagnosis, personalized treatment plan, and ongoing support to effectively manage joint pain and enhance overall well-being.