So you want to know more about liver cancer? You’ve come to the right place! In this article, we will explore the ins and outs of liver cancer, providing you with a comprehensive understanding of this disease. From its causes and risk factors to its symptoms and treatment options, we’ve got you covered. So, sit back, relax, and let’s dive into the world of liver cancer!
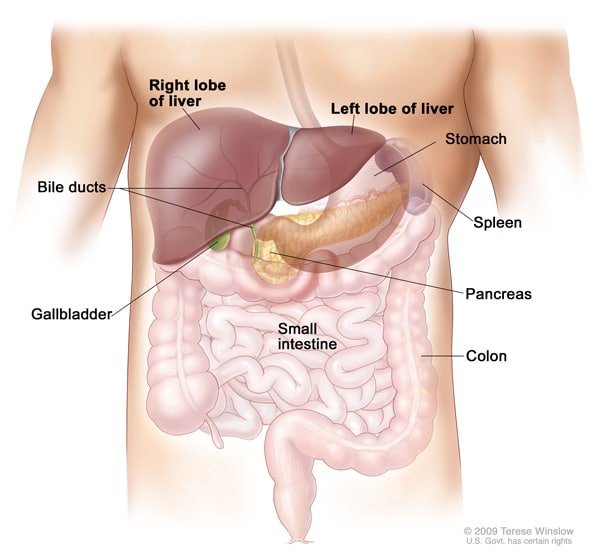
Overview of Liver Cancer
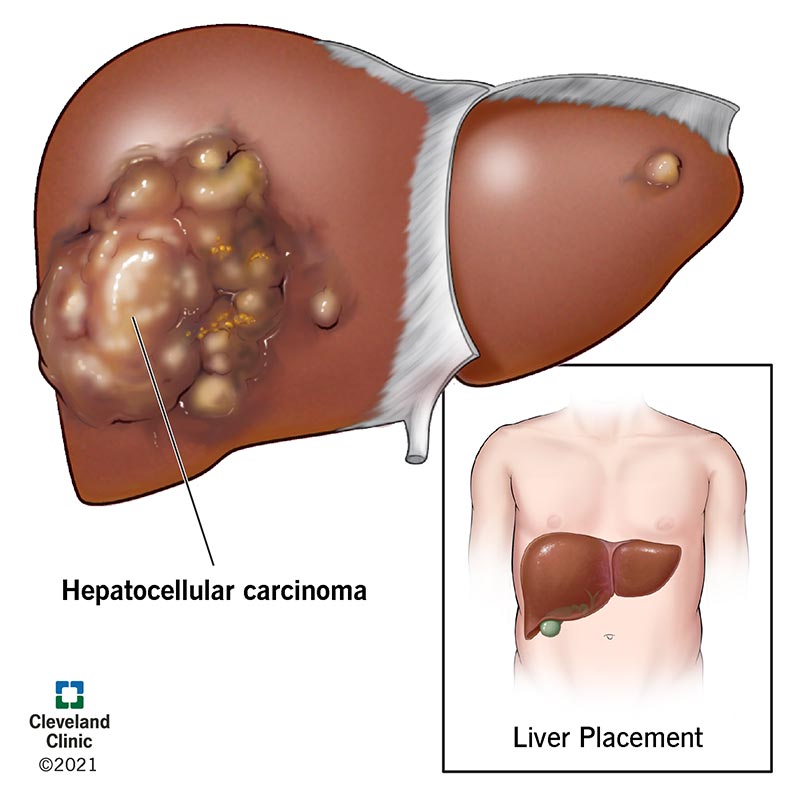
Liver cancer, also known as hepatic cancer, is a condition that starts in the cells of the liver. There are several types of liver cancer, including hepatocellular carcinoma (HCC), intrahepatic cholangiocarcinoma (ICC), and hepatoblastoma. HCC is the most common type of liver cancer and accounts for the majority of cases.
Types of Liver Cancer
-
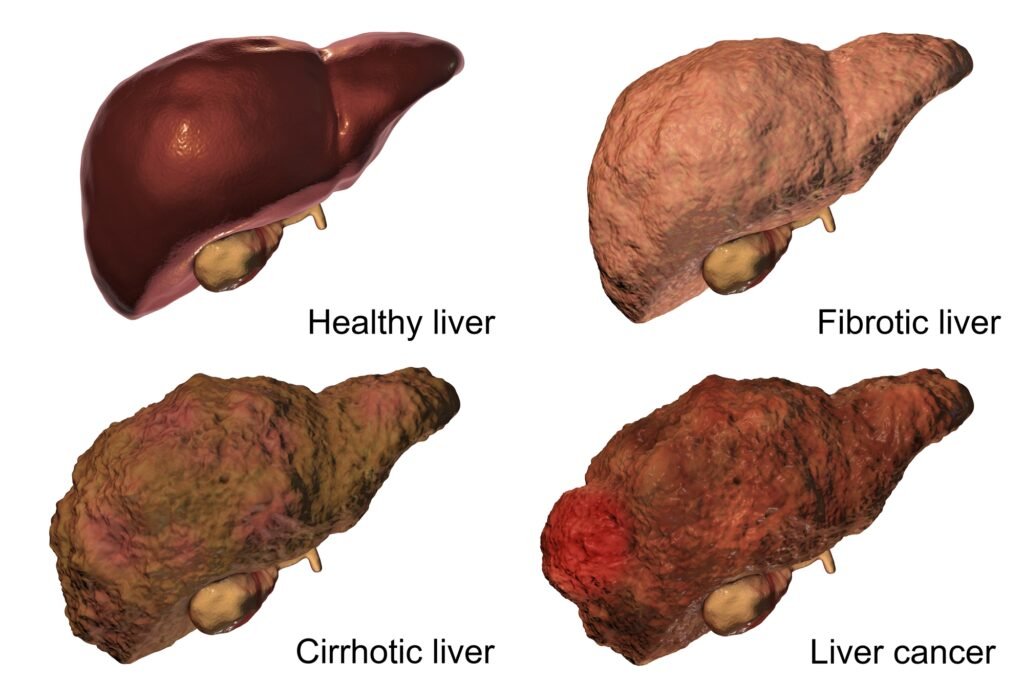
Hepatocellular Carcinoma (HCC): This type of liver cancer originates in the main type of liver cells called hepatocytes. HCC is usually associated with liver cirrhosis, which is often caused by chronic hepatitis B or C infection, excessive alcohol consumption, or non-alcoholic fatty liver disease.
-
Intrahepatic Cholangiocarcinoma (ICC): ICC begins in the bile ducts within the liver. While less common than HCC, ICC is often diagnosed at a later stage and tends to have a poorer prognosis.
-
Hepatoblastoma: This is a rare liver cancer that primarily affects children under the age of 5. It is usually treated with a combination of surgery, chemotherapy, and sometimes liver transplantation.
Causes and Risk Factors
Liver cancer can arise from various factors and risk factors. Some common causes and risk factors include:
-
Chronic viral infections: Chronic infections with hepatitis B or C viruses significantly increase the risk of developing liver cancer. These viruses can cause long-term liver inflammation and damage, which can eventually lead to the development of cancer.
-
Excessive alcohol consumption: Heavy and long-term alcohol consumption can damage the liver and increase the risk of liver cancer. Alcohol-related liver disease, such as alcoholic hepatitis and cirrhosis, can contribute to the development of liver cancer.
-
Non-alcoholic fatty liver disease: Accumulation of fat in the liver has been associated with an increased risk of liver cancer. This condition is often linked to obesity, type 2 diabetes, and metabolic syndrome.
-
Obesity and diabetes: These conditions are closely linked to the development of fatty liver disease and can increase the risk of liver cancer. This connection is thought to be due to the accumulation of fat in the liver and the development of chronic inflammation.
-
Certain genetic conditions: Certain inherited genetic conditions, such as hereditary hemochromatosis, Wilson’s disease, and alpha-1 antitrypsin deficiency, can increase the risk of liver cancer.
-
Exposure to aflatoxins: Aflatoxins are toxins produced by a type of mold called Aspergillus flavus. Prolonged exposure to aflatoxins, often through contaminated food, can increase the risk of liver cancer.
Signs and Symptoms
Liver cancer may not cause noticeable symptoms in its early stages. As the cancer progresses, the following signs and symptoms may occur:
- Unexplained weight loss
- Loss of appetite
- Abdominal pain or tenderness
- Jaundice (yellowing of the skin and eyes)
- Fatigue or weakness
- Nausea and vomiting
- Swelling in the abdomen
- Enlarged liver or a lump in the abdomen
- Easy bruising or bleeding
It is essential to note that these symptoms can also be caused by other conditions, so it is crucial to consult a healthcare professional for an accurate diagnosis.
Diagnosis
If liver cancer is suspected, various diagnostic tests and procedures may be conducted to confirm the diagnosis. These may include:
-
Imaging tests: Ultrasound, computed tomography (CT) scan, magnetic resonance imaging (MRI), or positron emission tomography (PET) scan can help visualize the liver and detect any abnormalities or tumors.
-
Blood tests: Blood tests can help evaluate liver function and detect specific tumor markers, such as alpha-fetoprotein (AFP) and des-gamma-carboxy prothrombin (DCP).
-
Biopsy: A tissue sample from the liver may be obtained through a needle biopsy or during surgery. The sample is then examined under a microscope to determine if there are cancer cells present.
-
Other diagnostic procedures: Additional tests, such as angiography or laparoscopy, may be performed to gather more information about the extent of the cancer.
Treatment Options for Liver Cancer
The treatment options for liver cancer may vary depending on the stage of the cancer, the location of the tumor, and the overall health of the individual. Common treatment options include:
Surgery
Surgical removal of the tumor is often the preferred treatment option if the cancer is confined to the liver and has not spread. The types of surgical procedures may include:
- Hepatectomy: Removal of a portion of the liver containing the tumor.
- Liver transplant: In certain cases, liver transplantation may be an option for individuals with early-stage liver cancer.
Ablation and Embolization Therapies
These minimally invasive procedures target and destroy cancer cells within the liver. Ablation therapies use heat (radiofrequency ablation) or extreme cold (cryoablation) to destroy the tumor. Embolization therapies involve blocking the blood supply to the tumor using tiny particles or beads.
Radiation Therapy
Radiation therapy uses high-energy beams to target and destroy cancer cells. It may be used as a primary treatment option or in combination with other treatments, such as surgery or chemotherapy.
Chemotherapy
Chemotherapy involves the use of drugs to kill cancer cells. It can be administered orally or intravenously and may be given before or after surgery, or in advanced cases, to slow the progression of the cancer.
Targeted Therapy
Targeted therapy relies on medications that specifically target certain molecules or pathways involved in the growth of cancer cells. These therapies can be particularly effective in individuals with specific genetic mutations or abnormalities in their tumor cells.
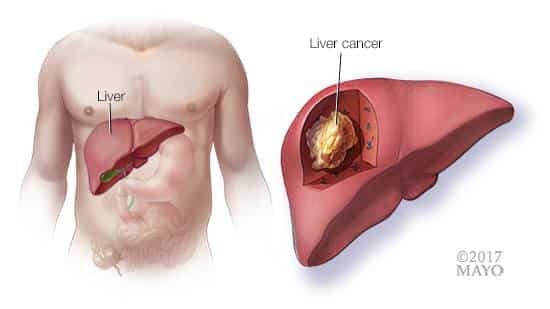
Prevention and Early Detection of Liver Cancer
While not all cases of liver cancer can be prevented, there are steps individuals can take to reduce their risk and promote early detection:
Preventive Measures
-
Vaccination against hepatitis B: Hepatitis B vaccination is crucial in preventing chronic viral infection, which is a significant risk factor for liver cancer. It is recommended for all infants, as well as adults who have not been previously vaccinated.
-
Practice safe sex and avoid the sharing of needles: Hepatitis B and C, as well as other sexually transmitted infections, can increase the risk of liver cancer. Using barrier methods and avoiding the sharing of needles are important preventive measures.
-
Limit alcohol consumption: To reduce the risk of liver cancer and other liver diseases, it is advisable to consume alcohol in moderation or avoid it altogether.
-
Maintain a healthy weight and eat a balanced diet: Obesity and non-alcoholic fatty liver disease increase the risk of liver cancer. Adopting a healthy lifestyle that includes regular physical activity and a balanced diet can help prevent these conditions.
Screening and Early Detection
Regular screening for liver cancer is recommended in individuals at high risk, such as those with chronic viral hepatitis, cirrhosis, or a family history of liver cancer. Screening methods can include imaging tests, blood tests for tumor markers, or a combination of both. Early detection can significantly improve the chances of successful treatment.
Living with Liver Cancer
A diagnosis of liver cancer can be overwhelming, but there are ways to manage the disease and improve quality of life:
Managing Symptoms and Side Effects
Various symptoms and side effects, such as pain, fatigue, nausea, or loss of appetite, can be effectively managed through medications, lifestyle modifications, and complementary therapies. It is essential to communicate with healthcare providers to address any concerns and receive appropriate support.
Supportive Care and Palliative Care
Supportive care focuses on providing relief from symptoms, improving quality of life, and supporting emotional well-being. Palliative care aims to alleviate pain and discomfort for individuals with advanced liver cancer and may be provided alongside curative treatments.
Clinical Trials and Experimental Treatments
Participating in clinical trials can provide access to new and potentially promising treatments for liver cancer. It is important to discuss eligibility and potential benefits with healthcare professionals.
Psychosocial Support and Counseling
Receiving emotional support from loved ones, joining support groups, or seeking counseling services can help individuals cope with the challenges of liver cancer. Emotional well-being is an important aspect of overall health.
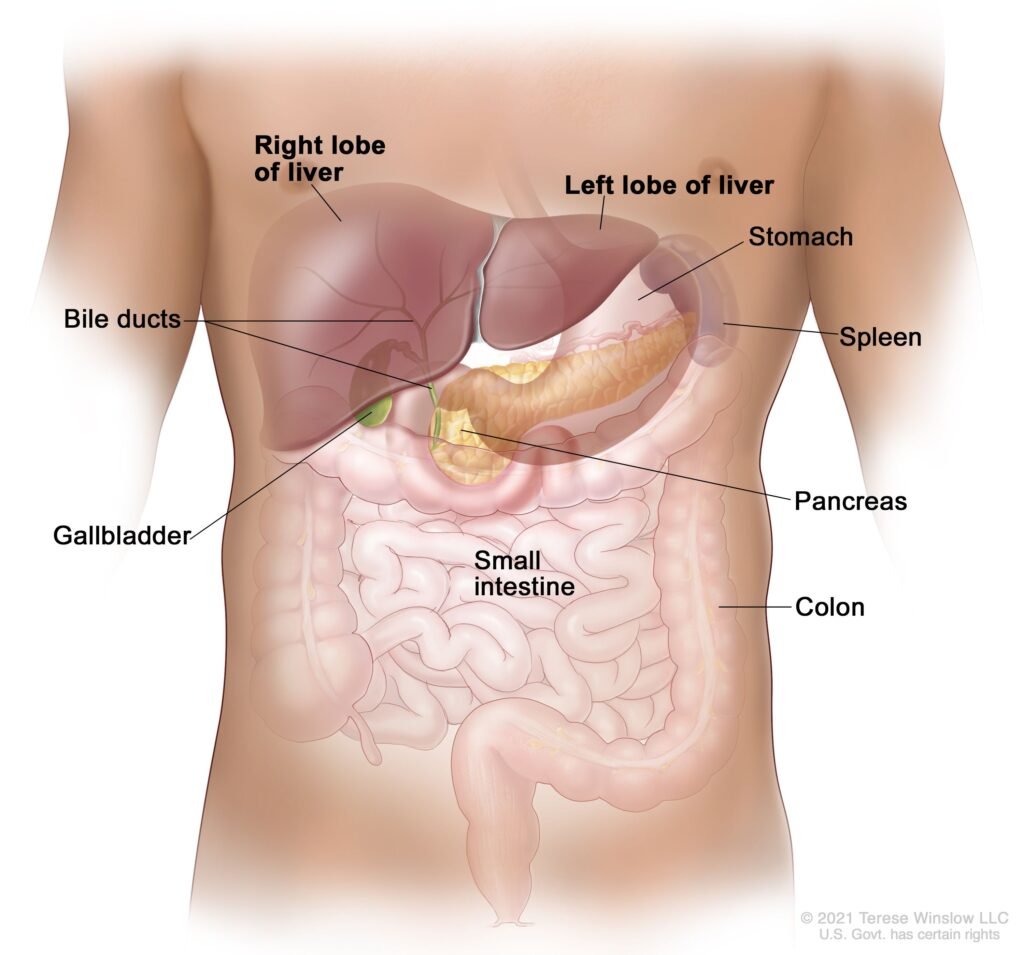
Understanding the Stages of Liver Cancer
The staging of liver cancer is crucial for determining the appropriate treatment options and estimating the prognosis. The four main stages of liver cancer are:
Stage 1: Early Stage
At this stage, the tumor is confined to the liver and has not spread to nearby lymph nodes or distant organs. Surgery or liver transplantation may be viable treatment options.
Stage 2: Localized Cancer
The tumor has grown larger and may have spread to nearby blood vessels or other structures within the liver. Surgical removal of the tumor may still be a viable treatment option.
Stage 3: Advanced Cancer
The cancer has spread to nearby lymph nodes or other adjacent organs, such as the gallbladder or intestines. Treatment options may include surgery, ablation therapies, radiation therapy, or targeted therapy, depending on the extent of the spread.
Stage 4: Metastatic Cancer
At this stage, the cancer has spread to distant organs, such as the lungs or bones. Treatment focuses on managing symptoms, providing palliative care, and improving quality of life.
Frequently Asked Questions about Liver Cancer
What is liver cancer?
Liver cancer is a condition characterized by the uncontrolled growth of abnormal cells in the liver. It can take various forms, such as hepatocellular carcinoma (HCC), intrahepatic cholangiocarcinoma (ICC), or hepatoblastoma.
Who is at risk of developing liver cancer?
Individuals at higher risk include those with chronic viral hepatitis infections (hepatitis B or C), a history of liver cirrhosis, excessive alcohol consumption, obesity, diabetes, certain genetic conditions, or exposure to aflatoxins.
What are the common symptoms of liver cancer?
The common symptoms include unexplained weight loss, loss of appetite, abdominal pain or tenderness, jaundice, fatigue, nausea, vomiting, swelling in the abdomen, and easy bruising or bleeding.
How is liver cancer diagnosed?
Diagnostic procedures include imaging tests (ultrasound, CT scan, MRI, PET scan), blood tests (to evaluate liver function and detect tumor markers), biopsy, and other tests to assess the extent of the cancer.
What are the treatment options for liver cancer?
Treatment options include surgery, liver transplantation, ablation and embolization therapies, radiation therapy, chemotherapy, and targeted therapy. The choice of treatment depends on the stage of the cancer, location, and overall health of the individual.
Can liver cancer be prevented?
While not all liver cancer cases can be prevented, preventive measures include hepatitis B vaccination, safe sex practices, avoiding sharing needles, limiting alcohol consumption, maintaining a healthy weight, and adopting a balanced diet.
What is the prognosis for liver cancer?
The prognosis depends on various factors such as the stage of the cancer, overall health, response to treatment, and individual circumstances. Early detection and treatment can significantly improve the prognosis.
Are there any alternative treatments for liver cancer?
Some individuals may explore alternative or complementary therapies such as herbal remedies, acupuncture, mind-body therapies, dietary modifications, or exercise. It is important to discuss these options with healthcare professionals.
Is liver cancer hereditary?
While most cases of liver cancer are not hereditary, there are certain genetic conditions, such as hereditary hemochromatosis, Wilson’s disease, or alpha-1 antitrypsin deficiency, which can increase the risk of liver cancer.
How can I support a loved one with liver cancer?
Offering emotional support, being a good listener, helping with practical tasks, accompanying them to medical appointments, and encouraging them to engage in activities they enjoy can provide valuable support and comfort for someone with liver cancer.
Understanding the Role of Hepatitis in Liver Cancer
Hepatitis B and Liver Cancer
Chronic infection with hepatitis B is a leading cause of liver cancer worldwide. The virus can cause long-term inflammation, leading to liver cirrhosis and an increased risk of developing liver cancer. Hepatitis B vaccination is crucial in preventing both chronic infection and subsequent liver cancer.
Hepatitis C and Liver Cancer
Chronic hepatitis C infection is another significant risk factor for liver cancer. It can cause liver inflammation and fibrosis, which may progress to cirrhosis and increase the risk of developing liver cancer. Antiviral treatments for hepatitis C can help reduce the risk of liver cancer in infected individuals.
Other Types of Viral Hepatitis
In addition to hepatitis B and C, other types of viral hepatitis, such as hepatitis A, D, and E, can also cause liver inflammation. Although their association with liver cancer may be less common, any chronic inflammation and liver damage can potentially increase the risk of developing liver cancer.
Preventing Hepatitis Infection
Preventing hepatitis infection is a crucial step in reducing the risk of liver cancer. This can be achieved through vaccination, practicing safe sex, avoiding sharing needles, maintaining good personal hygiene, and taking precautions while traveling to regions with high hepatitis prevalence.
Impact of Liver Cancer on the Body
Effects on Liver Function
As liver cancer progresses, it can impact the liver’s ability to perform vital functions, such as filtering toxins, metabolizing nutrients, producing bile, and regulating blood clotting. Impaired liver function can result in symptoms such as jaundice, fluid retention, and general weakness.
Associated Complications
Liver cancer can lead to various complications, including liver failure, ascites (accumulation of fluid in the abdomen), hepatic encephalopathy (brain dysfunction due to liver failure), portal hypertension (high blood pressure in the portal vein), and an increased risk of infections.
Impact on Overall Health and Well-being
Living with liver cancer can have a significant impact on an individual’s overall health and well-being. Fatigue, pain, mood changes, and disruption of daily activities and routines can affect both physical and emotional well-being. It is important to address these concerns and seek support from healthcare professionals and loved ones.
Emotional and Psychological Impact
A diagnosis of liver cancer can lead to various emotional and psychological challenges, such as anxiety, fear, sadness, or depression. Seeking psychological support, such as counseling or therapy, can help individuals cope with these emotional burdens and improve their overall well-being.
Risk Factors for Liver Cancer
Chronic Viral Infections
Chronic infections with hepatitis B or C viruses are major risk factors for liver cancer. Individuals with long-term viral infections should undergo regular monitoring and take necessary precautions to reduce the risk.
Excessive Alcohol Consumption
Heavy and prolonged alcohol consumption can lead to liver cirrhosis, which increases the risk of liver cancer. Limiting or avoiding alcohol consumption is an important step in preventing liver cancer.
Non-alcoholic Fatty Liver Disease
Non-alcoholic fatty liver disease (NAFLD), characterized by the accumulation of fat in the liver, is closely associated with liver cancer. Managing and preventing NAFLD through lifestyle changes, such as weight loss and adopting a healthy diet, can help reduce the risk of liver cancer.
Obesity and Diabetes
Obesity and type 2 diabetes are risk factors for non-alcoholic fatty liver disease, which is associated with an increased risk of liver cancer. Maintaining a healthy weight, engaging in regular physical activity, and managing diabetes can help reduce the risk.
Certain Genetic Conditions
Certain inherited genetic conditions, such as hereditary hemochromatosis, Wilson’s disease, and alpha-1 antitrypsin deficiency, can increase the risk of liver cancer. Regular monitoring and appropriate management of these conditions are crucial.
Exposure to Aflatoxins
Aflatoxins, produced by a type of mold called Aspergillus flavus, can contaminate food, particularly nuts, grains, and legumes. Chronic exposure to aflatoxins increases the risk of liver cancer. Reducing exposure to aflatoxins by storing food properly and consuming fresh, uncontaminated food can help mitigate this risk.
Alternative and Complementary Therapies for Liver Cancer
Herbal Remedies and Supplements
Some individuals with liver cancer may consider using herbal remedies or dietary supplements. However, it is essential to consult with healthcare professionals before trying any alternative therapies, as some herbs or supplements may interact with conventional treatments or have potential side effects.
Acupuncture and Traditional Chinese Medicine
Acupuncture, a traditional Chinese medicine practice, involves inserting thin needles into specific points on the body. It is sometimes used alongside conventional treatments to manage symptoms such as pain, nausea, or fatigue. However, it is important to discuss acupuncture or other traditional Chinese medicine practices with healthcare professionals.
Mind-body Therapies
Mind-body therapies, such as meditation, yoga, or tai chi, can help individuals with liver cancer manage stress, improve their overall well-being, and promote relaxation. These practices can be utilized as complementary approaches alongside standard medical care.
Dietary Modifications and Nutrition
Maintaining a healthy diet and proper nutrition is crucial for individuals with liver cancer. Healthcare professionals, such as dietitians, can provide guidance on a balanced diet that meets the specific nutritional needs of individuals with liver cancer.
Exercise and Physical Activity
Regular exercise and physical activity can have numerous benefits for individuals with liver cancer, including improved physical fitness, reduced fatigue, increased mood, and enhanced overall well-being. It is important to consult healthcare professionals for guidance and recommendations on suitable exercise programs.
In conclusion, liver cancer is a complex disease with various types, causes, and risk factors. Early diagnosis, appropriate treatment, and supportive care can significantly improve outcomes and quality of life for individuals with liver cancer. By understanding the disease, promoting prevention measures, and offering support, we can work together to reduce the burden of liver cancer in communities worldwide.