Meningococcal Disease, a severe bacterial infection, can have devastating consequences if not identified and treated promptly. This article provides an overview of the symptoms and diagnosis of this illness, aiming to help you recognize the signs and symptoms early on. By understanding the key indicators and seeking immediate medical attention, you can ensure timely intervention and potentially save lives.
Overview
Meningococcal Disease is a potentially serious bacterial infection caused by Neisseria meningitidis, a bacterium that can cause meningitis and septicemia. Meningitis is the inflammation of the membranes surrounding the brain and spinal cord, while septicemia is a bloodstream infection. This disease can progress rapidly and lead to life-threatening complications if not treated promptly. It is important to be aware of the prevalence, transmission, symptoms, diagnosis, complications, vaccine, treatment, prevention, and control of meningococcal disease.
Prevalence and Transmission
Meningococcal disease is distributed worldwide but varies in its prevalence depending on geographical region and population groups. It is most common in sub-Saharan Africa during the dry season, known as the “meningitis belt.” In other regions, sporadic cases and outbreaks can occur.
Transmission of the bacteria occurs through respiratory droplets, direct contact with an infected person’s saliva or nasal discharge, or close contact with contaminated items. Crowded living conditions, such as college dormitories or military barracks, can increase the risk of transmission. The bacteria can colonize the throat or nasal passages without causing symptoms.
Symptoms
Initial Symptoms
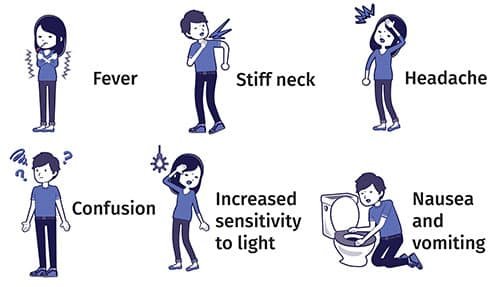
The initial symptoms of meningococcal disease can resemble those of the flu or a common viral infection. They may include sudden onset of fever, headache, stiff neck, and a rash. However, unlike a viral infection, the symptoms can progress rapidly and become severe.
Severe Symptoms
As the disease progresses, severe symptoms may develop. These may include high fever, intense headache, nausea, vomiting, sensitivity to light, confusion, and seizures. The rash associated with meningococcal disease may start as small, pink or purple spots, which can quickly develop into larger bruises. This rash does not disappear when pressed with a glass, indicating a medical emergency.
Signs in Newborns and Infants
Newborns and infants with meningococcal disease may exhibit different signs and symptoms. These can include fever, irritability, poor feeding, lethargy, and high-pitched crying. They may also have a bulging fontanelle, which is the soft spot on the top of the baby’s head.
Diagnosis
Medical History and Physical Examination
To diagnose meningococcal disease, the healthcare provider will start by taking a detailed medical history and conducting a thorough physical examination. The emphasis is on identifying risk factors, recent exposure to someone with meningococcal disease, and symptoms suggestive of the illness.
Lumbar Puncture
A lumbar puncture, also known as a spinal tap, is a common diagnostic test for meningococcal disease. During this procedure, a sample of cerebrospinal fluid (CSF) is obtained by inserting a needle into the lower back. The CSF is then tested for the presence of bacteria and other abnormalities.
Blood Tests
Blood tests can help confirm the diagnosis of meningococcal disease by detecting the presence of bacteria in the bloodstream or indicating an inflammatory response. These tests include blood cultures, complete blood count (CBC), and C-reactive protein (CRP) levels.
Imaging
In some cases, imaging tests such as a computed tomography (CT) scan or magnetic resonance imaging (MRI) may be performed to evaluate the extent of complications, such as brain swelling or abscess formation.
Complications
Meningitis
Meningitis is one of the most common complications of meningococcal disease. It can lead to inflammation of the brain and spinal cord, causing long-term neurological damage, hearing loss, and even death if not promptly treated. Prompt recognition of symptoms and initiation of treatment is crucial to prevent these complications.
Septicemia
Septicemia, also known as blood poisoning, occurs when the bacteria invade the bloodstream. This can lead to severe sepsis, organ failure, and in some cases, limb loss. Immediate medical attention is necessary to prevent life-threatening complications.
Other Complications
Meningococcal disease can also result in various other complications, such as pneumonia, arthritis, myocarditis (inflammation of the heart), and pericarditis (inflammation of the lining around the heart). These complications can have long-term effects on an individual’s health and require appropriate management.
Vaccine
Types of Meningococcal Vaccines
Several vaccines are available for the prevention of meningococcal disease. They can protect against different serogroups (types) of Neisseria meningitidis. The most common types include MenACWY, MenB, MenC, and MenACWY-TT. Each vaccine is designed to induce an immune response against specific serogroups.
Vaccine Schedule
The recommended vaccine schedule for meningococcal disease depends on several factors, including age, risk factors, and country-specific guidelines. Vaccinations are typically given during infancy, adolescence, and early adulthood. Booster doses may be necessary to maintain immunity.
Effectiveness and Side Effects
Meningococcal vaccines have shown high effectiveness in preventing meningococcal disease. They provide protection against the targeted serogroups and reduce the risk of complications. Common side effects are generally mild, such as injection site reactions, low-grade fever, and fatigue. Serious side effects are rare.

Treatment
Hospitalization
Meningococcal disease requires immediate medical attention, and most cases require hospitalization. In the hospital, the infected person can receive appropriate care, monitoring, and treatment to prevent complications. Isolation precautions are implemented to avoid further transmission.
Antibiotics
Antibiotics, such as ceftriaxone or cefotaxime, are the mainstay of treatment for meningococcal disease. These medications help eliminate the bacteria from the body and prevent the progression of the disease. Close monitoring of the patient’s response to antibiotics is essential.
Supportive Care
Supportive care is also crucial to manage the symptoms and complications associated with meningococcal disease. This may include pain relief, fever management, intravenous fluids, and respiratory support. Treatment plans are tailored to the individual’s specific needs.
Prevention and Control
Isolation and Quarantine
Isolation precautions are essential to prevent the spread of meningococcal disease. Infected individuals are isolated in healthcare settings, and close contacts are monitored for symptoms and offered prophylactic antibiotics when necessary. Prompt identification and isolation of cases can minimize the risk of transmission.
Contact Tracing
Contact tracing is a critical component of controlling meningococcal disease. Healthcare providers identify and follow up with individuals who have had close contact with an infected person. Close contacts are assessed for symptoms, offered prophylactic antibiotics, and educated on the signs and symptoms of the disease.
Health Education and Awareness
Health education and awareness play a vital role in preventing meningococcal disease. It is essential to educate the public about the disease, its symptoms, transmission, and the importance of vaccination. Encouraging good respiratory hygiene practices and early healthcare-seeking behavior can help control the spread of the disease.

Epidemiology
Global Burden
Meningococcal disease remains a global public health concern. It can occur in sporadic cases or lead to outbreaks, primarily affecting vulnerable populations. Each year, thousands of cases are reported worldwide, resulting in significant morbidity and mortality.
At-Risk Population
Certain populations are at higher risk of developing meningococcal disease. These include infants, adolescents, college students living in dormitories, military recruits, individuals with compromised immune systems, and those traveling to regions with a high prevalence of the disease.
Outbreaks
Outbreaks of meningococcal disease can occur in various settings, such as schools, college campuses, and military installations. These outbreaks often necessitate a swift public health response, including mass vaccination campaigns, contact tracing, and heightened surveillance.
Research and Future Directions
Development of New Vaccines
Ongoing research aims to develop new vaccines that provide broader protection against multiple serogroups of Neisseria meningitidis. These innovative vaccines may offer long-lasting immunity and simplify vaccination schedules, contributing to the control of meningococcal disease.
Improved Diagnostic Tools
Advancements in diagnostic tools, such as rapid molecular tests, can help healthcare providers promptly identify and distinguish meningococcal disease from other infections with similar symptoms. These tools aid in early intervention and appropriate treatment.
Public Health Interventions
Public health interventions, including comprehensive vaccination programs, improved surveillance systems, and targeted awareness campaigns, continue to enhance prevention and control efforts. Collaborative efforts between healthcare professionals, policymakers, and researchers are crucial for reducing the burden of meningococcal disease.
Conclusion
Meningococcal disease is a serious bacterial infection that can have devastating consequences if not detected and treated promptly. Understanding the prevalence, transmission, symptoms, diagnosis, complications, vaccine, treatment, prevention, and control measures is essential in mitigating the impact of this disease. By maintaining high vaccination rates, promoting awareness, and implementing effective public health strategies, we can work together to reduce the burden of meningococcal disease worldwide and protect our communities.
