Bronchiectasis, a chronic lung condition characterized by the widening and inflammation of the airways, can be a challenging condition to manage. However, there is hope on the horizon with the emergence of new treatment options that aim to improve the quality of life for individuals living with bronchiectasis. This article will take you on a journey as we explore these innovative treatments, from targeted therapies to pulmonary rehabilitation, offering a glimmer of hope for those affected by this debilitating disease. So sit back, relax, and let’s venture into the world of new possibilities in bronchiectasis treatment together.

Overview of Bronchiectasis
Bronchiectasis is a respiratory condition characterized by the abnormal widening and scarring of the airways, leading to a build-up of mucus and recurrent infections. This chronic condition affects the bronchi, which are the large airway passages in the lungs. Bronchiectasis can develop due to various causes, including respiratory infections, genetic disorders, and autoimmune diseases. It can also occur as a result of damage to the airways caused by inhalation of toxic substances or other underlying lung conditions.
Signs and Symptoms
The primary symptoms of bronchiectasis include chronic cough, frequent respiratory infections, and production of large amounts of sputum. Other signs and symptoms that may manifest in individuals with bronchiectasis include shortness of breath, wheezing, chest pain, fatigue, and recurrent pneumonia. These symptoms can vary in intensity and frequency, depending on the severity of the disease and the individual’s overall health.

Diagnostic Methods
To diagnose bronchiectasis, various diagnostic methods are utilized. These may include a thorough medical history assessment, physical examination, and a range of imaging tests. Chest X-rays, computed tomography (CT) scans, and high-resolution CT scans are commonly performed to visualize the airways and assess the extent of damage. Other tests, such as pulmonary function tests and sputum cultures, may be conducted to evaluate lung function and identify potential bacterial infections.
Current Treatment Options
The management of bronchiectasis aims to alleviate symptoms, reduce the frequency of infections, and improve overall lung function. Several treatment options are available and may be used in combination for optimal results.
Medication
Medication plays a crucial role in controlling symptoms and preventing complications in individuals with bronchiectasis. Bronchodilators may be prescribed to relax the airway muscles and improve airflow. Inhaled corticosteroids are commonly used to reduce inflammation in the airways. Antibiotics are also frequently prescribed to treat and prevent bacterial infections that can exacerbate bronchiectasis symptoms.
Chest Physiotherapy
Chest physiotherapy is a technique used to help clear mucus from the lungs and improve breathing. It involves various manual techniques, such as clapping, vibration, and postural drainage, to mobilize the mucus and facilitate its removal from the airways. These techniques can be performed by a healthcare professional or taught to patients for self-management.
Airway Clearance Techniques
Airway clearance techniques are exercises and methods that assist in loosening and clearing mucus from the airways. Examples of such techniques include active cycle of breathing, autogenic drainage, and positive expiratory pressure devices. These techniques are often incorporated into daily routines to minimize mucus accumulation and prevent respiratory infections.
Antibiotics
Antibiotics are key in managing bronchiectasis, particularly in cases where bacterial infections are recurrent. They can help control bacterial growth and reduce inflammation in the airways. Antibiotics may be taken orally, intravenously, or inhaled, depending on the severity of the infection and the individual’s overall health.
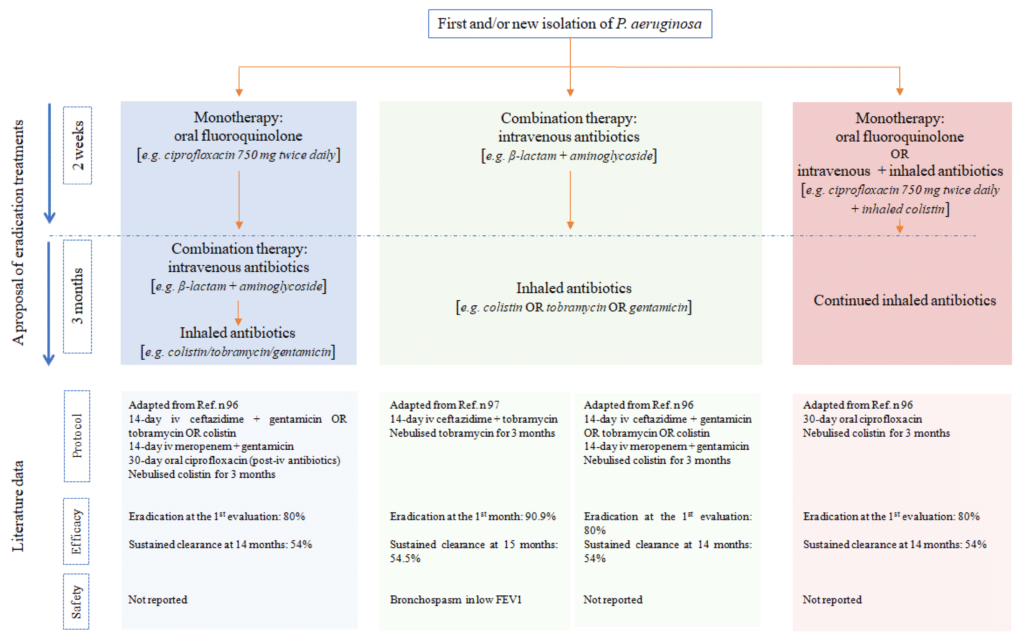
Emerging Therapies
The field of bronchiectasis research is continuously evolving, leading to the development of new and promising treatment options. These emerging therapies aim to target the underlying causes of bronchiectasis and provide more targeted and effective management options.
Mucus Reducing Agents
Mucus reducing agents, such as mucolytics, are being investigated for their potential to improve mucus clearance in individuals with bronchiectasis. These agents work by thinning the mucus, making it easier to expectorate and reducing the risk of mucus blockage in the airways.
Anti-inflammatory Drugs
Inflammation plays a significant role in the progression and exacerbation of bronchiectasis. Therefore, anti-inflammatory drugs are being studied as potential treatments for the condition. By reducing inflammation in the airways, these drugs may help alleviate symptoms and prevent further damage to the bronchi.
Biologic Therapies
Biologic therapies, including monoclonal antibodies and immune-modulating drugs, show promise in the treatment of bronchiectasis. These therapies target specific components of the immune system and aim to modify the immune response, thereby reducing inflammation and the risk of recurrent infections.
Gene Therapy
Gene therapy involves the modification or replacement of defective genes responsible for the development of bronchiectasis. This emerging therapy holds great potential for treating genetic forms of bronchiectasis by addressing the underlying genetic abnormalities.
Role of Nutritional Intervention
Proper nutrition plays a vital role in supporting the management of bronchiectasis. Nutritional interventions can significantly impact an individual’s overall health, immunity, and respiratory function.
Importance of Nutritional Support
Maintaining a balanced diet and obtaining adequate nutrition is crucial for individuals with bronchiectasis. A well-nourished body is better equipped to fight infections, promote tissue repair, and support optimal lung function. Proper nutrition also plays a critical role in preventing malnutrition, which can weaken the immune system and exacerbate symptoms.
Dietary Modifications
Incorporating dietary modifications can be beneficial for individuals with bronchiectasis. Consuming a diet rich in fruits, vegetables, whole grains, and lean proteins can provide essential vitamins, minerals, and antioxidants that support overall health and lung function. Limiting the intake of processed foods, high-sodium foods, and sugary snacks can help manage inflammation and reduce the risk of exacerbations.
Supplements and Vitamins
In some cases, dietary supplements and specific vitamins may be recommended by healthcare professionals to address any nutritional deficiencies and support the management of bronchiectasis. These supplements may include omega-3 fatty acids, vitamin D, and antioxidants, which have been shown to have potential benefits for respiratory health.

Pulmonary Rehabilitation
Pulmonary rehabilitation is a comprehensive program designed to improve the quality of life and overall respiratory function in individuals with lung diseases, including bronchiectasis.
Exercise and Breathing Techniques
Pulmonary rehabilitation programs often include exercise routines tailored to an individual’s abilities and goals. These exercises can help improve lung capacity, strengthen respiratory muscles, and enhance overall physical endurance. Breathing techniques are also taught, allowing individuals to optimize their breathing patterns and manage breathlessness more effectively.
Benefits of Pulmonary Rehabilitation
Engaging in pulmonary rehabilitation programs can offer numerous benefits to individuals with bronchiectasis. These programs have been shown to improve exercise tolerance, reduce breathlessness, enhance disease self-management skills, and boost overall psychological well-being. Participating in pulmonary rehabilitation can also lead to a decreased need for hospitalizations and emergency room visits.
Components of a Rehabilitation Program
A typical pulmonary rehabilitation program for bronchiectasis may consist of various components. These can include exercise training, education on self-management strategies, nutritional counseling, psychological support, and lifestyle modification recommendations. The combination of these components aims to address the multifaceted needs of individuals living with bronchiectasis and improve their overall quality of life.
Surgical Options
In some cases, when other treatment options fail to provide sufficient relief or the disease progresses significantly, surgery may be considered as a viable option for individuals with bronchiectasis.
Lung Volume Reduction Surgery
Lung volume reduction surgery involves the removal of damaged lung tissue, which can alleviate symptoms and improve lung function. This surgical procedure reduces the size of the lungs, allowing healthier lung tissue to function more efficiently.
Bullectomy
A bullectomy is a surgical procedure that involves the removal of large air pockets, or bullae, in the lungs. These bullae can compress healthy lung tissue and impair respiratory function. By removing them, the space in the lungs is freed up, allowing for better airflow and improved lung capacity.
Lung Transplantation
In severe cases of bronchiectasis, lung transplantation may be considered as a last resort treatment option. This procedure involves replacing the damaged lungs with healthy lungs from a donor. Lung transplantation can provide individuals with advanced bronchiectasis a new lease on life, offering improved lung function and an opportunity for a higher quality of life.

Management of Exacerbations
Exacerbations, or acute flare-ups of bronchiectasis symptoms, can significantly impact an individual’s well-being and lung function. Prompt and appropriate management of exacerbations is crucial to alleviate symptoms and prevent further complications.
Recognizing Exacerbations
It is essential for individuals with bronchiectasis to be able to recognize exacerbations and seek medical attention promptly. Common signs of exacerbations include increased respiratory symptoms, changes in sputum color or consistency, fever, and worsening breathlessness. Monitoring symptoms closely and maintaining regular communication with healthcare providers can help identify exacerbations early on.
Treatment with Antibiotics
Exacerbations often result from bacterial infections, and antibiotic therapy plays a vital role in their management. Identifying the specific bacteria causing the exacerbation through sputum cultures allows healthcare providers to prescribe appropriate antibiotics. Timely initiation of antibiotic treatment can help control the infection, reduce inflammation, and alleviate symptoms effectively.
Coping with Exacerbations
Managing exacerbations extends beyond medical treatment. Lifestyle and self-care practices can make a significant difference in coping with exacerbations. Staying hydrated, getting enough rest, practicing good hygiene, and maintaining a nutritious diet are all important during exacerbations. Additionally, seeking emotional support from loved ones, engaging in relaxation techniques, and following respiratory management strategies prescribed by healthcare providers can help individuals navigate exacerbations more effectively.
Complementary Therapies
Complementary therapies are often sought by individuals with bronchiectasis to complement traditional treatments and manage symptoms. While the evidence surrounding the effectiveness of these therapies is limited, some individuals report benefits from their use.
Acupuncture
Acupuncture is an ancient practice that involves the insertion of thin needles into specific points on the body. Some individuals with bronchiectasis have reported improvements in symptoms such as cough and breathlessness following acupuncture treatment. However, more research is needed to determine the effectiveness of acupuncture as a complementary therapy for bronchiectasis.
Herbal Medicine
Herbal medicine, including the use of herbal supplements and teas, is another complementary therapy option explored by individuals with bronchiectasis. Some herbal remedies are believed to have anti-inflammatory properties and may help alleviate symptoms such as cough and mucus production. However, it is important to consult with healthcare professionals before incorporating herbal medicine into bronchiectasis management, as some herbal remedies may interact with medications or have unwanted side effects.
Nutritional Supplements
Certain nutritional supplements, such as omega-3 fatty acids and antioxidants, have gained attention for their potential respiratory benefits. While some individuals with bronchiectasis may experience symptom relief or improved well-being with the use of these supplements, it is crucial to consult with healthcare providers before starting any new supplements. Proper dosing and quality control are necessary to ensure effectiveness and safety.
Telehealth and Remote Monitoring
Advances in technology have opened doors for remote healthcare delivery, facilitating access to healthcare services from the comfort of one’s own home. Telehealth and remote monitoring offer various benefits to individuals with chronic conditions like bronchiectasis.
Benefits of Telehealth
Telehealth allows individuals with bronchiectasis to connect with healthcare providers remotely for consultations, follow-ups, and treatment management. This removes barriers such as travel time and reduces exposure to potential infections in healthcare settings. Telehealth also provides an opportunity for quicker access to healthcare services, particularly during times when in-person visits may be challenging.
Remote Monitoring Devices
Remote monitoring devices, such as wearable sensors and smart devices, enable individuals to track their vital signs and symptoms from home. These devices can provide valuable data to healthcare providers, allowing for timely intervention and adjustment of treatment plans. Monitoring oxygen saturation levels, heart rate, and respiratory functions remotely can help detect early signs of exacerbations and facilitate appropriate medical interventions.
Telemedicine Consultations
Telemedicine consultations involve virtual interactions between individuals with bronchiectasis and their healthcare providers. These consultations can be conducted via video calls or phone calls, allowing for in-depth discussions about symptoms, treatment adjustments, and overall disease management. Telemedicine consultation also offers the convenience of seeking medical advice from the comfort of home, reducing the need for unnecessary trips to healthcare facilities.
Clinical Trials and Research
Ongoing clinical trials and research initiatives play a vital role in advancing the understanding and treatment of bronchiectasis. These endeavors contribute to the development of innovative treatments and strategies that may provide better outcomes for individuals with this condition.
Ongoing Clinical Trials
Several clinical trials are currently underway to evaluate novel treatments and interventions for bronchiectasis. These trials aim to assess the effectiveness and safety of new medications, therapies, and management approaches. Participation in clinical trials not only provides access to potentially groundbreaking treatments but also contributes to the advancement of medical knowledge surrounding bronchiectasis.
Investigational Treatments
Investigational treatments refer to those that are being studied and researched for their potential benefits in bronchiectasis management. These treatments may involve new medications, therapies, or approaches that have shown promise in preliminary studies. Investigational treatments go through rigorous testing and evaluation processes before they can be approved for widespread use.
Future Directions
The future of bronchiectasis treatment holds much promise as advancements continue to be made in the field of respiratory medicine. The development of targeted treatment options, gene therapies, and a better understanding of the underlying mechanisms of bronchiectasis are expected to revolutionize the care and management of this chronic condition. With ongoing research and innovation, the future holds the potential for improved outcomes and a higher quality of life for individuals living with bronchiectasis.
