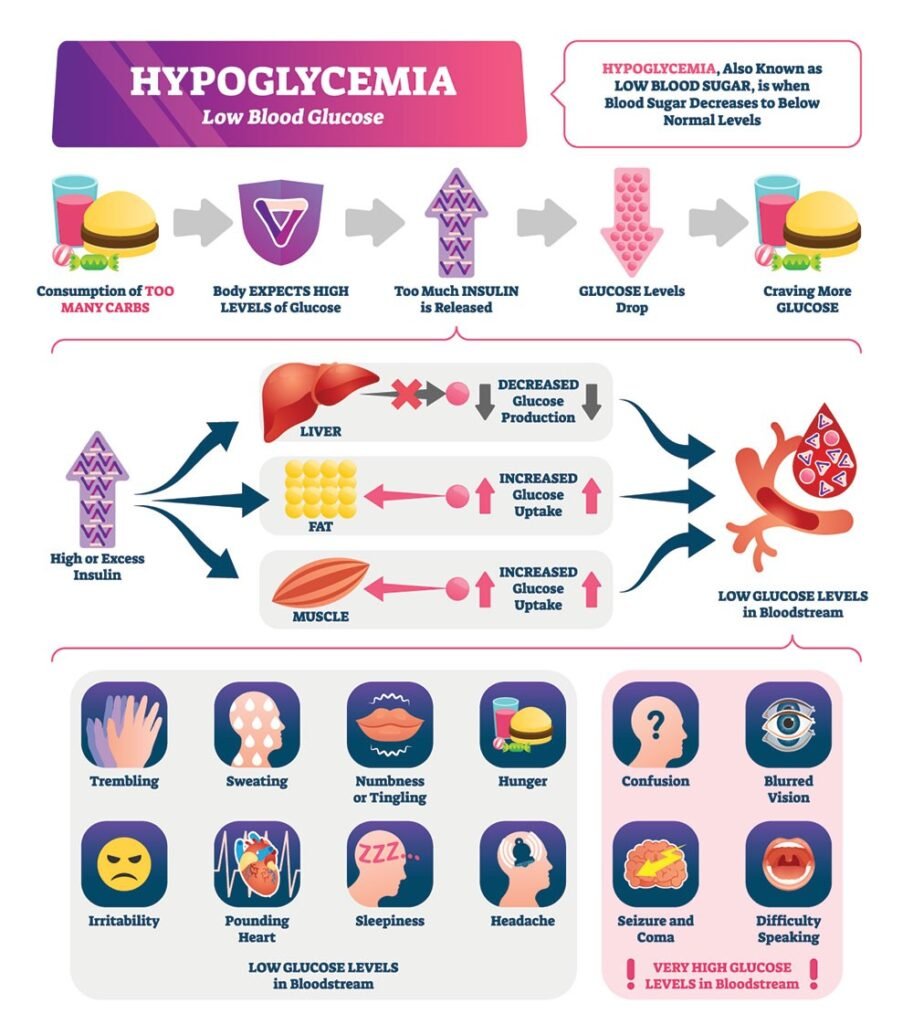
Pregnancy is an incredible journey, but for those with gestational diabetes, managing blood sugar levels can be a challenge. In this article, you will discover effective strategies to lower blood sugar during pregnancy. From adopting a healthy diet to incorporating exercise into your routine, these simple yet powerful tips will help you maintain stable blood sugar levels and ensure a healthier pregnancy for both you and your baby. So, let’s explore these practical steps and make this beautiful phase of your life even more enjoyable and worry-free.
Maintain a Balanced Diet
During pregnancy, it is crucial to maintain a balanced diet to effectively manage blood sugar levels. This means consuming a variety of nutrient-rich foods that provide essential vitamins and minerals for both you and your baby. Here are some key points to keep in mind when it comes to maintaining a balanced diet during pregnancy:
Consume Complex Carbohydrates
Complex carbohydrates are an excellent choice for managing blood sugar levels. These carbohydrates are digested slowly, causing a gradual rise in blood sugar instead of a sudden spike. Incorporate foods like whole grains, legumes, and vegetables into your meals to ensure a steady release of energy throughout the day.
Include Lean Protein in Each Meal
Including lean protein sources in your meals is essential for managing blood sugar levels during pregnancy. Consuming lean proteins such as chicken, fish, tofu, and beans can help stabilize blood sugar levels and keep you feeling satiated for longer periods. Aim to include a palm-sized portion of protein with each meal to maintain a balanced diet.
Choose Healthy Fats
Contrary to popular belief, not all fats are bad for you. Including healthy fats, such as avocados, nuts, and olive oil, in your diet can aid in blood sugar control during pregnancy. Healthy fats are digested slowly and can help keep you feeling full, preventing overeating and blood sugar spikes.
Eat Plenty of Fiber
Fiber plays a vital role in maintaining stable blood sugar levels during pregnancy. Foods rich in fiber, such as fruits, vegetables, and whole grains, can slow down the absorption of sugar into your bloodstream. Aim to incorporate fiber into each meal to promote healthy blood sugar levels and overall digestive health.
Avoid Sugary Foods and Beverages
When managing blood sugar levels during pregnancy, it is crucial to minimize your intake of sugary foods and beverages. These can cause sudden spikes in blood sugar, leading to complications for both you and your baby. Instead, opt for healthier alternatives like fresh fruits, unsweetened beverages, and low-sugar snacks to satisfy your cravings without affecting your blood sugar levels.
Portion Control
In addition to maintaining a balanced diet, portion control is key to managing blood sugar levels during pregnancy. It helps to keep your meals balanced and prevents overeating, which can cause blood sugar spikes. Here are some tips to help you practice portion control:
Use a Smaller Plate
Using a smaller plate can trick your brain into thinking you’re consuming a larger portion. This psychological trick can prevent overconsumption and aid in portion control. By visually filling up a smaller plate, you’ll feel satisfied without overeating.
Measure Food Portions
Measuring your food portions can give you a better understanding of serving sizes and help you control your carbohydrate intake. Invest in measuring cups and a food scale to accurately portion your meals and snacks. This will allow you to keep track of your carbohydrate consumption and ensure you’re staying within the recommended limits.
Avoid Overeating
During pregnancy, it can be tempting to indulge in large portions or give in to cravings. However, overeating can lead to blood sugar spikes and unnecessary weight gain. To avoid overeating, try to listen to your body’s hunger and fullness cues. Eat until you feel comfortably satisfied, rather than until you feel overly full.
Eat Regularly throughout the Day
To maintain stable blood sugar levels, it’s essential to eat regularly throughout the day. Instead of having three large meals, aim for five to six smaller meals/snacks spread out evenly. This approach can help prevent extreme hunger and stabilize your blood sugar levels.

Monitor Carbohydrate Intake
Monitoring your carbohydrate intake is a crucial aspect of managing blood sugar levels during pregnancy. Carbohydrates directly impact blood sugar levels, so it’s important to make informed choices and keep track of your intake. Here are some strategies to help you monitor your carbohydrate consumption:
Learn to Read Food Labels
Reading food labels can provide valuable information about the carbohydrate content of packaged foods. Pay attention to the total carbohydrate count per serving, including both sugars and fiber. Look for foods that are lower in added sugars and higher in fiber to make healthier choices that won’t cause significant blood sugar spikes.
Track Carbohydrate Consumption
Keeping track of your carbohydrate consumption can help you stay within your recommended limits and maintain stable blood sugar levels. Consider using a food diary or a smartphone app to log your meals and calculate your carb intake. This will allow you to identify patterns, make adjustments if necessary, and communicate effectively with your healthcare provider.
Space Out Carbohydrate Intake
Instead of consuming a large amount of carbohydrates in one meal, try to space out your intake throughout the day. This approach helps prevent blood sugar spikes and provides a more consistent source of energy. Distribute your carbohydrate intake evenly across your meals and snacks to maintain stable blood sugar levels.
Focus on Low Glycemic Index Foods
Opting for low glycemic index (GI) foods can help regulate blood sugar levels during pregnancy. Low GI foods are digested and absorbed more slowly, resulting in a slower rise in blood sugar levels. Examples of low GI foods include whole grains, legumes, non-starchy vegetables, and most fruits. Incorporating these foods into your diet can contribute to stable blood sugar control.
Exercise Regularly
Regular exercise is beneficial for everyone, including pregnant women with gestational diabetes. It helps to improve insulin sensitivity, manage blood sugar levels, and promote overall health and well-being. Here are some important considerations when it comes to exercising during pregnancy:
Consult with Your Healthcare Provider
Before starting or continuing any exercise routine during pregnancy, it’s essential to consult with your healthcare provider. They can provide personalized advice based on your specific situation and ensure that exercise is safe for you and your baby.
Choose Suitable Exercises
Not all exercises are suitable for pregnant women, especially those with gestational diabetes. Opt for low-impact activities that minimize stress on your joints, such as walking, swimming, and prenatal yoga. These exercises can help improve cardiovascular health, maintain muscle tone, and manage blood sugar levels.
Engage in Moderate Physical Activity
Engaging in moderate-intensity physical activity for at least 150 minutes per week is recommended for pregnant women with gestational diabetes. Moderate-intensity exercises, such as brisk walking or swimming, elevate your heart rate and promote better blood sugar control. Aim for 30 minutes of exercise on most days of the week, but remember to listen to your body and rest when needed.
Incorporate Strength Training
Including strength-training exercises in your fitness routine can be highly beneficial during pregnancy. Strength training helps build muscle mass, improves insulin sensitivity, and supports overall body strength. Consult with a certified prenatal fitness instructor to learn safe and effective strength-training exercises that are appropriate for your stage of pregnancy.
Walk After Meals
Taking a short walk after meals can help lower blood sugar levels by increasing insulin sensitivity. Research shows that even a 10 to 15-minute walk after a meal can significantly improve glucose metabolism. So, make it a habit to go for a leisurely stroll after lunch or dinner to help keep your blood sugar levels in check.

Stay Hydrated
Maintaining proper hydration is essential for overall health and blood sugar management during pregnancy. Here are some recommendations to ensure you stay hydrated:
Drink Plenty of Water
Water is the best choice for hydration during pregnancy, regardless of whether or not you have gestational diabetes. Aim to drink at least eight cups (64 ounces) of water per day or more if you’re exercising or in a hot climate. Staying properly hydrated can help prevent dehydration and support optimal blood sugar control.
Avoid Sugary Beverages
Sugary beverages, such as soda, fruit juices, and sweetened teas, can cause blood sugar spikes and contribute to unnecessary weight gain. It’s best to avoid these beverages altogether or consume them in moderation. Instead, opt for water, unsweetened herbal tea, or infused water with fresh fruits and herbs as a refreshing and hydrating alternative.
Limit Caffeine Intake
While moderate caffeine intake is generally considered safe during pregnancy, it’s important to be mindful of your consumption. High levels of caffeine can have adverse effects on blood sugar control and may also impact your sleep quality. Limit your intake of caffeinated beverages like coffee, tea, and energy drinks, and opt for decaffeinated versions when possible.
Manage Stress Levels
Managing stress is crucial for overall well-being during pregnancy, especially when dealing with gestational diabetes. Chronic stress can negatively impact blood sugar levels and the body’s ability to respond to insulin. Here are some strategies to help you manage stress levels effectively:
Practice Relaxation Techniques
Incorporating relaxation techniques into your daily routine can help reduce stress and promote better blood sugar control. Try deep breathing exercises, meditation, guided imagery, or gentle stretching to help calm your mind and alleviate stress. You can also explore prenatal yoga classes or relaxation-focused prenatal exercise programs for additional support.
Get Adequate Rest and Sleep
Getting enough rest and quality sleep is essential for managing stress and maintaining optimal health. Aim for at least seven to eight hours of uninterrupted sleep per night. Establish a relaxing bedtime routine, create a comfortable sleep environment, and prioritize restorative rest to support your overall well-being.
Engage in Activities That Bring Joy
Engaging in activities that bring you joy and relaxation can help reduce stress and improve blood sugar control. Whether it’s pursuing a hobby, spending time with loved ones, reading a book, or listening to music, make sure to prioritize self-care and carve out time for activities that bring you happiness during pregnancy.
Seek Support from Loved Ones
Having a strong support system is crucial when managing gestational diabetes and the associated stress. Lean on your loved ones for emotional support, understanding, and encouragement. Share your concerns and challenges with them, and don’t hesitate to seek professional help if needed. Support groups or counseling services can provide additional guidance and assistance.

Medication and Insulin
Depending on your blood sugar control, your healthcare provider may prescribe medication or insulin to manage gestational diabetes effectively. Here are some key points to keep in mind regarding medication and insulin:
Follow Your Healthcare Provider’s Instructions
It is essential to follow your healthcare provider’s instructions regarding medication and insulin usage. They will prescribe the appropriate medication or insulin therapy based on your specific needs. It’s important to understand the dosage, timing, and any potential side effects associated with your medication or insulin regimen.
Take Medications as Prescribed
Consistency is crucial when taking medications or insulin for gestational diabetes. Take your prescribed medications or administer insulin injections exactly as instructed by your healthcare provider. Set reminders or use an alarm to ensure you adhere to your medication schedule and maintain stable blood sugar control.
Monitor Blood Sugar Levels Regularly
Regularly monitoring your blood sugar levels is essential when taking medication or insulin for gestational diabetes. Your healthcare provider will provide guidance on how often and when to test your blood sugar using a glucometer. This information will help you and your healthcare provider track your progress and make necessary adjustments to your treatment plan.
Learn How to Self-Administer Insulin
If insulin therapy is required, your healthcare provider will teach you how to self-administer insulin injections properly. It’s important to learn the correct technique to ensure accurate dosage and minimize discomfort. Follow your provider’s instructions closely and ask any questions you may have to ensure your confidence in self-administration.
Adjust Insulin Dosages as Required
As your pregnancy progresses and your blood sugar levels change, adjustments to your insulin dosage may be necessary. Consult with your healthcare provider if you notice any significant changes in your blood sugar levels or experience symptoms of hypo- or hyperglycemia. They will guide you on adjusting your insulin dosage to maintain stable blood sugar control.
Regular Blood Sugar Monitoring
Regular blood sugar monitoring is a crucial aspect of managing gestational diabetes effectively. Here’s what you need to keep in mind:
Use a Glucometer
A glucometer is a device that allows you to check your blood sugar levels at home. Your healthcare provider will guide you on how to use it accurately. With regular monitoring, you can track your blood sugar levels and understand how different foods, activities, and medications impact your readings.
Check Blood Sugar Levels at Recommended Times
Your healthcare provider will provide specific guidelines on when to check your blood sugar levels. Typically, blood sugar readings may be required upon waking (fasting), before meals, after meals, and before bedtime. Follow your provider’s instructions closely to remain diligent in monitoring your blood sugar levels.
Keep a Log of Readings
Maintaining a log of your blood sugar readings is beneficial for both you and your healthcare provider. It helps identify trends, patterns, and potential triggers that affect your blood sugar control. Use a notebook, smartphone app, or any other tracking tool to record your readings, along with the date, time, and any relevant notes.
Discuss Results with Your Healthcare Provider
Regularly discuss your blood sugar readings with your healthcare provider to assess your progress and make any necessary adjustments to your treatment plan. Open communication is vital to ensure you’re consistently managing your blood sugar levels effectively and maintaining optimal health for you and your baby.
Make Necessary Adjustments
Based on your blood sugar readings and discussions with your healthcare provider, adjustments may be required in terms of your diet, exercise routine, or medication/insulin dosage. Stay proactive, ask questions, and be open to making any necessary modifications to better manage your blood sugar levels.

Regular Prenatal Care
Attending regular prenatal care appointments is crucial for maintaining healthy blood sugar levels during pregnancy. Here’s why:
Attend Scheduled Doctor’s Appointments
During pregnancy, you will have regular appointments with your doctor or healthcare provider. Attend these appointments as scheduled to monitor your overall health, pregnancy progress, and blood sugar control. Regular check-ups allow your healthcare provider to detect any changes or complications early on and provide necessary guidance and support.
Communicate Your Concerns and Challenges
Prenatal care appointments offer an opportunity to discuss any concerns or challenges you may be facing regarding blood sugar management. Share your experiences, symptoms, or difficulties with your healthcare provider openly and honestly. They can provide reassurance, answer any questions you may have, and offer tailored advice to address your specific needs.
Receive Proper Guidance and Support
Regular prenatal care ensures that you receive proper guidance and support in managing gestational diabetes. Your healthcare provider can offer valuable insights on nutrition, exercise, medication, insulin, and overall diabetes management during pregnancy. Their expertise and support can significantly contribute to your ability to maintain stable blood sugar levels and have a healthy pregnancy.
Educate Yourself
Educating yourself about gestational diabetes and its management is empowering. Here are some steps you can take to expand your knowledge:
Attend Nutrition and Gestational Diabetes Classes
Attending nutrition and gestational diabetes classes can provide valuable information and guidance on managing blood sugar levels during pregnancy. These classes are often offered by healthcare providers, hospitals, or community organizations and cover topics such as meal planning, carbohydrate counting, label reading, and healthy lifestyle habits. Take advantage of these educational resources to enhance your understanding of gestational diabetes and make informed choices.
Learn about Dietary Modifications
Understanding dietary modifications specific to gestational diabetes can help you make healthier food choices and manage blood sugar levels effectively. Educate yourself about portion sizes, carbohydrate counting, and glycemic index to optimize your diet. Consult with a registered dietitian or nutritionist who specializes in gestational diabetes for personalized advice and meal planning.
Understand the Importance of Blood Sugar Control
Gaining an understanding of the importance of blood sugar control during pregnancy empowers you to take charge of your health and make necessary lifestyle changes. Knowing the potential risks and complications associated with uncontrolled gestational diabetes can motivate you to maintain stable blood sugar levels and follow your healthcare provider’s recommendations diligently.
Stay Informed About Potential Complications
Staying informed about potential complications related to gestational diabetes is essential for both you and your baby’s well-being. Educate yourself about conditions such as preeclampsia, preterm birth, and macrosomia (large-for-gestational-age baby) that can be associated with uncontrolled gestational diabetes. Awareness of these risks can help you stay motivated to manage your blood sugar levels effectively and reduce the likelihood of complications.
In conclusion, managing blood sugar levels during pregnancy is crucial for the health and well-being of both you and your baby. By maintaining a balanced diet, practicing portion control, monitoring carbohydrate intake, exercising regularly, staying hydrated, managing stress levels, following medication and insulin instructions, monitoring blood sugar regularly, attending regular prenatal care appointments, and educating yourself about gestational diabetes, you can effectively lower blood sugar during pregnancy and have a healthy and successful pregnancy journey. Remember to communicate openly with your healthcare provider, seek support from loved ones, and prioritize self-care to ensure a positive outcome for you and your baby.