Imagine a world where pediatric brain tumors no longer pose a threat to the well-being of our children. Thanks to groundbreaking advancements in research, that world is one step closer to becoming a reality. In this article, we will explore the latest discoveries and innovations surrounding pediatric brain tumors, shedding light on the hope they bring to families and medical professionals alike. With a focus on improving treatment options, early detection, and overall survivability, these advancements have the potential to transform the lives of countless young patients and their loved ones. So buckle up and get ready to embark on a journey through the exciting realm of pediatric brain tumor research.
Advancements in Research for Pediatric Brain Tumors
Introduction to Pediatric Brain Tumors
Pediatric brain tumors are a devastating diagnosis affecting children of all ages. These tumors are abnormal growths of cells or tissues within the brain that can interfere with normal brain function. While brain tumors in children are relatively rare, they remain the leading cause of cancer-related deaths in this age group. Due to their delicate nature and the unique challenges they present, research into pediatric brain tumors is crucial to improve diagnosis, treatment, and long-term outcomes for these young patients.
Current Challenges in Pediatric Brain Tumor Research
Research into pediatric brain tumors faces several challenges. First and foremost, the rarity of these tumors makes it difficult to collect sufficient data and develop comprehensive research studies. Additionally, the complexity and heterogeneity of brain tumors in children pose unique challenges in understanding their underlying biology and developing effective treatment strategies. Moreover, the impact of these tumors on a child’s developing brain and their long-term outcomes further complicate the research process. Despite these challenges, significant advancements have been made in recent years, providing hope for improved outcomes for pediatric brain tumor patients.
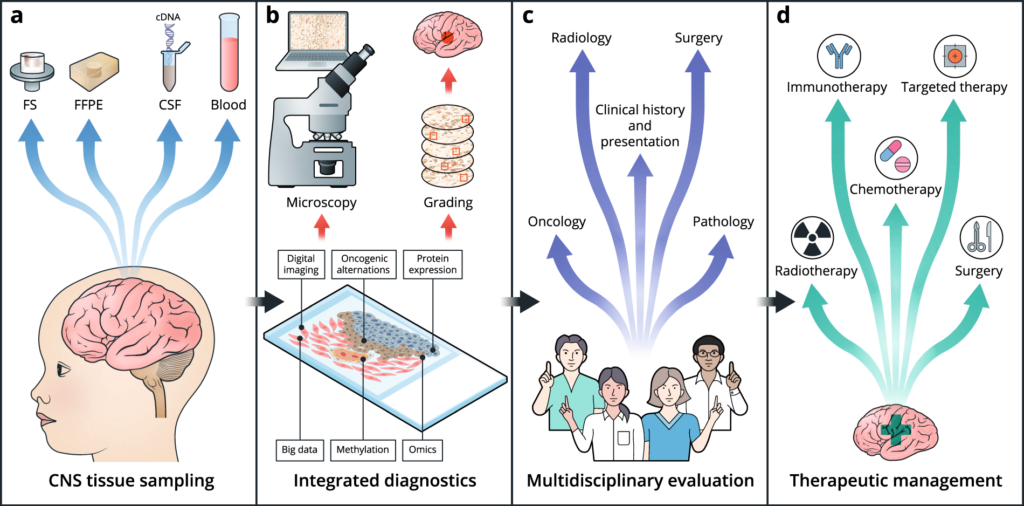
Diagnostic Advances
In recent years, there have been significant advancements in the diagnosis of pediatric brain tumors. Improved imaging techniques, such as magnetic resonance imaging (MRI), allow for more precise visualization of the tumor and its characteristics. This helps in accurately identifying the type and location of the tumor, aiding in the development of personalized treatment plans. Additionally, molecular profiling techniques, such as next-generation sequencing, enable researchers to analyze the genetic alterations within the tumor cells. This information aids in the diagnosis, prognosis, and identification of potential therapeutic targets for individual patients.
Treatment Options
The treatment of pediatric brain tumors typically involves a multimodal approach, including surgery, radiation therapy, and chemotherapy. Recent advancements in treatment options have led to improved outcomes for young patients. Advances in surgical techniques, such as image-guided resections and minimally invasive approaches, have enhanced the precision and safety of tumor removal. Radiation therapy has also seen significant progress with the development of proton therapy, which selectively delivers radiation to the tumor while minimizing damage to healthy surrounding tissues. Chemotherapy protocols have become more tailored and targeted, reducing side effects and increasing treatment efficacy.
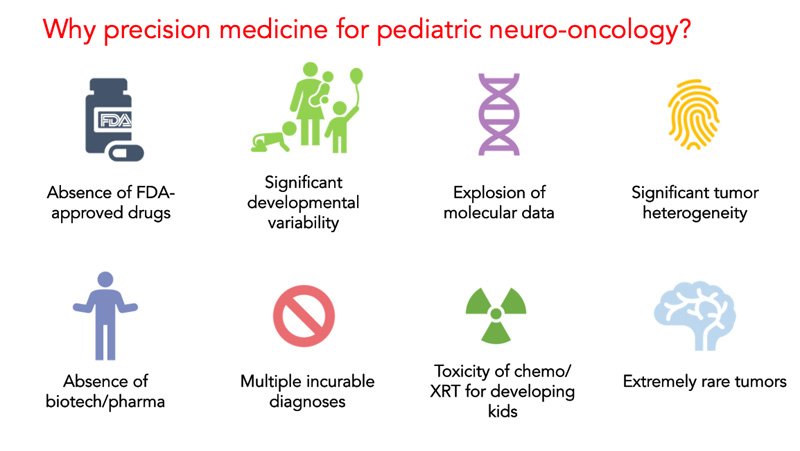
Targeted Therapy
Targeted therapy is a promising approach in the treatment of pediatric brain tumors. This therapeutic strategy aims to disrupt specific molecular pathways that drive tumor growth, while sparing healthy cells. Recent research has identified various genetic mutations and alterations in pediatric brain tumors, paving the way for targeted therapies. Drugs targeting specific genetic abnormalities, such as BRAF inhibitors for BRAF-mutant tumors, have shown promising results. Targeted therapy holds great potential in providing effective and personalized treatment options for pediatric brain tumor patients.
Immunotherapy
Immunotherapy has emerged as an exciting field in cancer treatment, including pediatric brain tumors. This approach harnesses the body’s immune system to fight against cancer cells. Several immunotherapeutic strategies, such as immune checkpoint inhibitors and chimeric antigen receptor (CAR) T-cell therapy, have shown promise in clinical trials for certain types of pediatric brain tumors. Immunotherapy offers a novel and potentially less toxic treatment option, particularly for patients with aggressive or recurrent tumors. Ongoing research in this field aims to further refine these treatments and expand their application in pediatric brain tumor care.
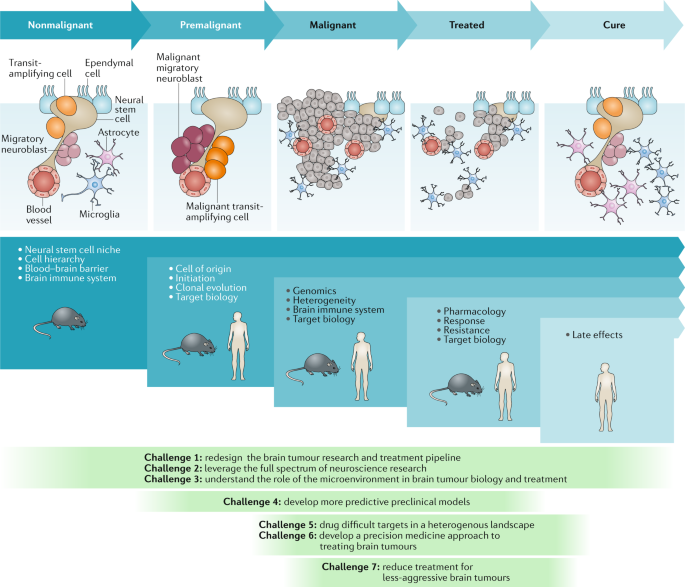
Radiation Therapy
Radiation therapy plays a crucial role in the treatment of pediatric brain tumors, but its impact on the developing brain poses significant challenges. Recent advancements in radiation therapy techniques aim to maximize treatment efficacy while minimizing long-term side effects. Proton therapy, for example, delivers radiation more precisely, reducing radiation exposure to healthy brain tissue. Additionally, techniques like fractionated stereotactic radiation therapy allow for targeted and localized tumor treatment, minimizing damage to surrounding tissues. These advancements in radiation therapy improve treatment outcomes and significantly reduce the long-term neurocognitive effects of therapy for pediatric brain tumor patients.
Surgical Innovations
Surgery remains a vital component in the treatment of pediatric brain tumors. Recent surgical innovations have revolutionized the field and improved patient outcomes. Image-guided surgeries, which use advanced imaging techniques during the operation, enable surgeons to precisely locate and remove tumors while minimizing damage to surrounding healthy tissue. Minimally invasive surgical approaches, such as endoscopic resections, have also gained popularity, reducing the need for extensive open surgeries and leading to quicker recoveries. Further developments in surgical techniques, coupled with advancements in imaging technology, continue to enhance the safety and effectiveness of surgical interventions for pediatric brain tumors.

Precision Medicine
Precision medicine is an innovative approach that tailors treatment plans based on an individual’s unique genetic makeup, tumor characteristics, and overall health. This personalized approach to medicine has the potential to revolutionize the treatment of pediatric brain tumors. By analyzing the genetic and molecular profiles of tumor cells, doctors can identify specific mutations and alterations that drive tumor growth. This information allows for the selection of targeted therapies, minimizing unnecessary treatments and reducing the risk of side effects. The integration of precision medicine into pediatric brain tumor care holds significant promise in improving treatment outcomes and maximizing long-term quality of life for young patients.
Psychosocial Support for Pediatric Brain Tumor Patients
The diagnosis and treatment of a pediatric brain tumor not only impact the physical health of the child but also have profound emotional and psychosocial effects on the patient and their families. Providing comprehensive psychosocial support is an essential aspect of pediatric brain tumor care. Research into pediatric psychosocial support has focused on developing interventions to address the unique emotional and social needs of young patients and their families. Programs offering counseling, support groups, and child-friendly play areas in hospitals aim to improve coping strategies, reduce anxiety, and enhance the overall well-being of pediatric brain tumor patients and their families.
In conclusion, advancements in research for pediatric brain tumors have transformed the landscape of diagnosis and treatment options. Improved diagnostic techniques, such as advanced imaging and molecular profiling, allow for more accurate and personalized diagnoses. Treatment options have expanded with the development of targeted therapies and immunotherapies, offering new hope for young patients. Additionally, advancements in radiation therapy and surgical innovations have improved treatment efficacy while minimizing long-term side effects. The integration of precision medicine and the focus on comprehensive psychosocial support further enhance care for pediatric brain tumor patients. As research continues to progress, the future holds great promise for improved outcomes and increased survival rates for children battling brain tumors.