Hey there! Have you ever wondered what goes on inside a child’s brain when they are diagnosed with a brain tumor? In this article, we will be exploring the intricate world of brain tumors in children. From understanding the different types to exploring the symptoms and treatment options, we’ll take a closer look at this complex issue. So, grab a cup of coffee and get ready to learn more about the fascinating world of understanding brain tumors in children!
Types of Brain Tumors in Children
Medulloblastomas
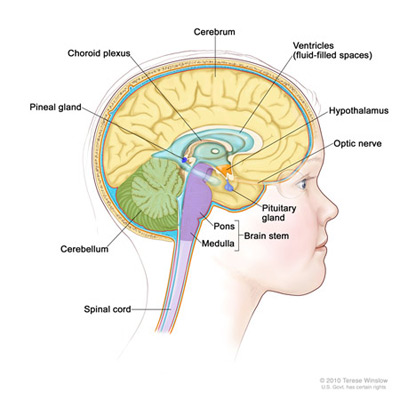
Medulloblastomas are one of the most common types of brain tumors in children. They typically originate in the cerebellum, which is the part of the brain responsible for balance and coordination. These tumors usually grow fast and can spread to other parts of the brain or spinal cord.
Astrocytomas
Astrocytomas are tumors that form from astrocytes, which are star-shaped cells that support the nerve cells in the brain. There are different types of astrocytomas, ranging from low-grade (slow-growing) to high-grade (fast-growing). The location and size of the tumor determine the symptoms and treatment options.
Ependymomas
Ependymomas are tumors that develop from the cells lining the ventricles or central canal of the spinal cord. They are most often found in children and can occur in different areas of the brain, including the fourth ventricle. The growth rate of ependymomas varies, and they can cause symptoms such as headaches, nausea, and balance problems.
Craniopharyngiomas
Craniopharyngiomas are tumors that develop near the pituitary gland, which is located at the base of the brain. These tumors are usually noncancerous but can cause problems by pressing on nearby structures. Craniopharyngiomas commonly occur in children and adolescents and can affect hormone production and growth.
Causes and Risk Factors
Genetic factors
Some brain tumors in children can be caused by genetic factors, such as certain inherited syndromes. Examples of syndromes associated with an increased risk of brain tumors include neurofibromatosis type 1 and 2, Li-Fraumeni syndrome, and tuberous sclerosis. Genetic counseling and testing may be recommended for families with a history of these syndromes.
Radiation therapy
Children who have received radiation therapy to the head, especially at a young age, have a higher risk of developing brain tumors later in life. This includes children who have undergone radiation treatment for previous cancers, such as leukemia. Close monitoring and follow-up care are crucial for those who have undergone radiation therapy.
Certain medical conditions
Certain medical conditions, such as neurofibromatosis type 1 and 2 mentioned earlier, increase the risk of brain tumors in children. Other conditions that may be associated with an increased risk include tuberous sclerosis, Li-Fraumeni syndrome, and von Hippel-Lindau disease. Regular check-ups and screenings are important for early detection in these cases.
Unknown causes
In some cases, the exact cause of brain tumors in children remains unknown. Research is ongoing to better understand the factors that contribute to the development of these tumors. It is important to remember that most children with these tumors do not have a family history or known risk factors.
Symptoms and Signs
Headaches
Headaches are a common symptom of brain tumors in children. These headaches are often persistent, dull, and worsen over time. They may be accompanied by other symptoms such as vomiting, changes in vision, or sensitivity to light. It is essential to pay attention to the frequency, severity, and pattern of headaches in children.
Nausea and vomiting
Nausea and vomiting are common symptoms of brain tumors, particularly when they affect the part of the brain responsible for coordinating balance and movement. These symptoms may worsen in the morning or after physical activities. If your child experiences frequent or unexplained episodes of nausea and vomiting, it is important to seek medical attention.
Balance problems
Brain tumors can disrupt the normal functioning of the cerebellum, leading to balance problems and coordination difficulties. Children may experience unsteady gait, clumsiness, and difficulty with everyday activities that require fine motor skills. These symptoms can significantly impact a child’s quality of life and should be assessed by a healthcare professional.
Seizures
Seizures, which are sudden and uncontrollable electrical disturbances in the brain, can occur in children with brain tumors. The type and severity of seizures can vary, with some children experiencing focal seizures (limited to a specific part of the body) and others having generalized seizures that cause loss of consciousness. If a child experiences seizures, prompt medical evaluation is necessary.
Behavioral changes
Brain tumors can cause various behavioral changes in children. These changes may manifest as irritability, mood swings, unusual sleep patterns, and difficulty concentrating or paying attention. It is important for parents and caregivers to communicate any noticeable changes in a child’s behavior to healthcare professionals to help with diagnosis and treatment.
Diagnosis and Testing
Medical history and physical examination
When evaluating a child for a possible brain tumor, a healthcare professional will start by taking a detailed medical history and performing a thorough physical examination. The medical history may include questions about the child’s symptoms, any family history of brain tumors or related conditions, and the timeline of symptom progression.
Neurological examination
A neurological examination assesses the child’s nervous system function. This includes evaluating reflexes, muscle strength, coordination, and sensory perception. Abnormal findings may indicate the presence of a brain tumor and help guide further diagnostic tests.
Imaging tests
Imaging tests, such as magnetic resonance imaging (MRI) and computed tomography (CT) scans, are essential for visualizing brain tumors. These tests provide detailed images of the brain and help determine the size, location, and characteristics of the tumor. Additional specialized imaging techniques, such as functional MRI and positron emission tomography (PET) scans, may be used to gather more specific information.
Biopsy or surgery
To confirm the diagnosis of a brain tumor and gather additional information about its type and grade, a biopsy may be performed. During a biopsy, a small sample of the tumor is removed for laboratory analysis. In some cases, surgery may be necessary to remove part or all of the tumor, which can also provide diagnostic information.
Treatment Options
Surgery
Surgery is often the first treatment option for brain tumors in children. The goals of surgery may include removing as much of the tumor as possible, relieving symptoms, and obtaining a tissue sample for diagnosis. The extent and type of surgery depend on factors such as the tumor’s size, location, and characteristics.
Radiation therapy
Radiation therapy uses high-energy beams to kill or slow the growth of cancer cells. It is commonly used after surgery to target any remaining tumor cells. In certain cases, radiation therapy may be used as the primary treatment if surgery is not feasible or to shrink the tumor before surgery.
Chemotherapy
Chemotherapy involves using drugs to kill cancer cells or slow their growth. It can be administered orally, intravenously, or directly into the cerebrospinal fluid. Chemotherapy may be used before or after surgery, in combination with radiation therapy, or as the main treatment for tumors that cannot be surgically removed.
Targeted drug therapy
Targeted drug therapy involves using drugs that specifically target certain molecules or pathways involved in the growth and spread of cancer cells. These drugs can block tumor growth or inhibit blood vessel formation within the tumor. Targeted therapy may be used in combination with other treatments or as a maintenance therapy.
Prognosis and Survival Rates
Survival rates by tumor type
The prognosis and survival rates for children with brain tumors vary depending on various factors, including the type and grade of the tumor, the age of the child, and the effectiveness of treatment. While some types of brain tumors have high survival rates, others may have lower rates. It is important to remember that each case is unique, and prognosis should be discussed with the child’s healthcare team.
Long-term effects and quality of life
Children who undergo treatments for brain tumors may experience long-term effects that can affect their quality of life. These effects may include cognitive impairments, learning difficulties, hormonal imbalances, and physical limitations. Supportive care and rehabilitation play a vital role in mitigating these effects and helping children reach their full potential.
Supportive Care and Rehabilitation
Psychosocial support
A child’s diagnosis of a brain tumor can have a significant impact on their emotional well-being and that of their families. Psychosocial support, including counseling, support groups, and access to mental health services, is crucial in providing emotional support and helping families cope with the challenges they may face.
Physical and occupational therapy
Physical and occupational therapy are important components of rehabilitation for children with brain tumors. These therapies aim to improve physical function, mobility, and independence. Physical therapy focuses on strengthening muscles and improving coordination, while occupational therapy helps children regain skills necessary for everyday activities.
Special education services
Children with brain tumors may require additional educational support to address any learning difficulties or cognitive impairments resulting from their condition or treatment. Special education services can provide tailored instruction, accommodations, and support to help children succeed academically and overcome any challenges they may face.
Research and Advances
Advancements in treatment
Ongoing research and clinical trials continue to drive advancements in the treatment of brain tumors in children. Researchers are exploring new targeted therapies, immunotherapies, and innovative surgical techniques to improve outcomes and reduce treatment side effects. These advancements offer hope for more effective and less invasive treatment options in the future.
Clinical trials and experimental therapies
Clinical trials are research studies that evaluate new treatments, interventions, or diagnostic procedures for brain tumors. Participation in clinical trials may provide access to experimental therapies that are not yet widely available. Families are encouraged to discuss the possibility of clinical trials with their healthcare team to explore additional treatment options.

Coping Strategies for Children and Families
Emotional support
Coping with a brain tumor diagnosis can be emotionally challenging for both children and their families. Seeking emotional support from healthcare professionals, counseling services, support groups, and other families going through similar experiences can provide reassurance, guidance, and a safe space to express emotions and concerns.
Coping techniques for children
Children with brain tumors may benefit from learning and using coping techniques to manage their emotions and reduce stress. These techniques can include mindfulness exercises, relaxation techniques, creative outlets such as art or music therapy, and age-appropriate discussions about their condition.
Support groups
Joining support groups for children and families affected by brain tumors can provide a sense of community and understanding. These groups offer opportunities to share experiences, exchange information, and find support from others who are going through similar challenges. Support groups may be available in person or online.
Prevention and Early Detection
Regular check-ups and screenings
Regular check-ups and screenings are important for early detection and monitoring of brain tumors in children. Routine visits with healthcare providers allow for the identification of any concerning symptoms, timely referrals for further evaluation, and appropriate screening tests if necessary.
Awareness of risk factors
Awareness of risk factors, such as previous radiation therapy or a family history of brain tumors or related genetic conditions, can help in the early detection and management of brain tumors in children. Caregivers should communicate any relevant family history or known risk factors to healthcare professionals.
Genetic counseling
Families with a history of brain tumors or related genetic conditions may benefit from genetic counseling. Genetic counselors can assess the risk of inherited conditions and provide information about genetic testing and potential preventive measures. Early identification of high-risk individuals allows for proactive monitoring and interventions.