Atrial fibrillation, also known as AFib, is a common heart condition that affects millions of people worldwide. This irregular and often rapid heart rhythm can have a significant impact on overall heart health. In this article, we will explore the causes, symptoms, and potential complications of AFib, as well as the importance of early detection and treatment. So, buckle up and get ready to gain a deeper understanding of this condition and its potential consequences on your heart health.
What is Atrial Fibrillation
Definition
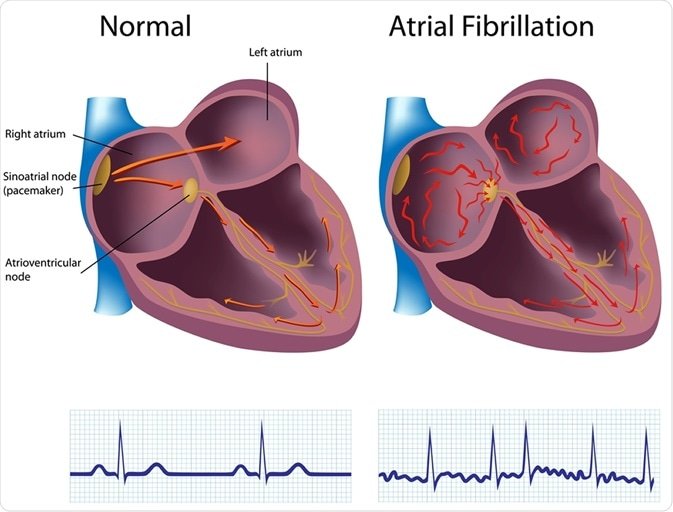
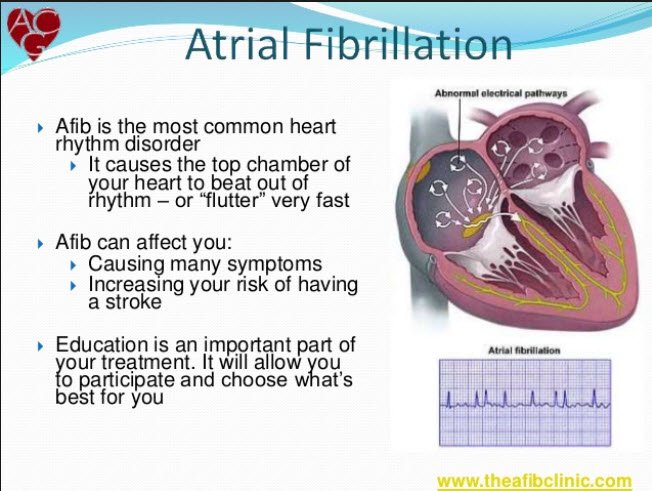
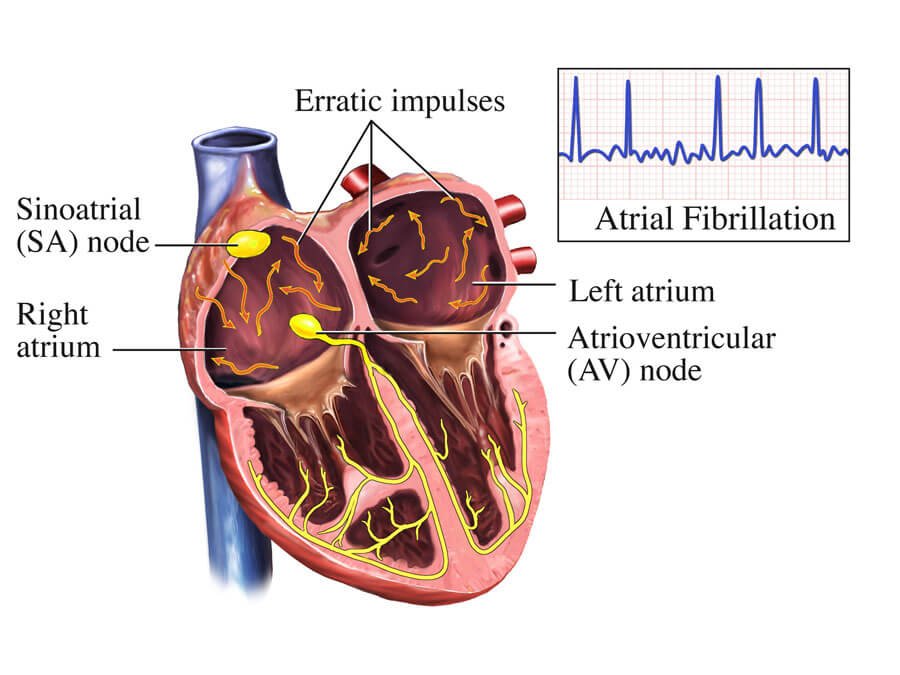
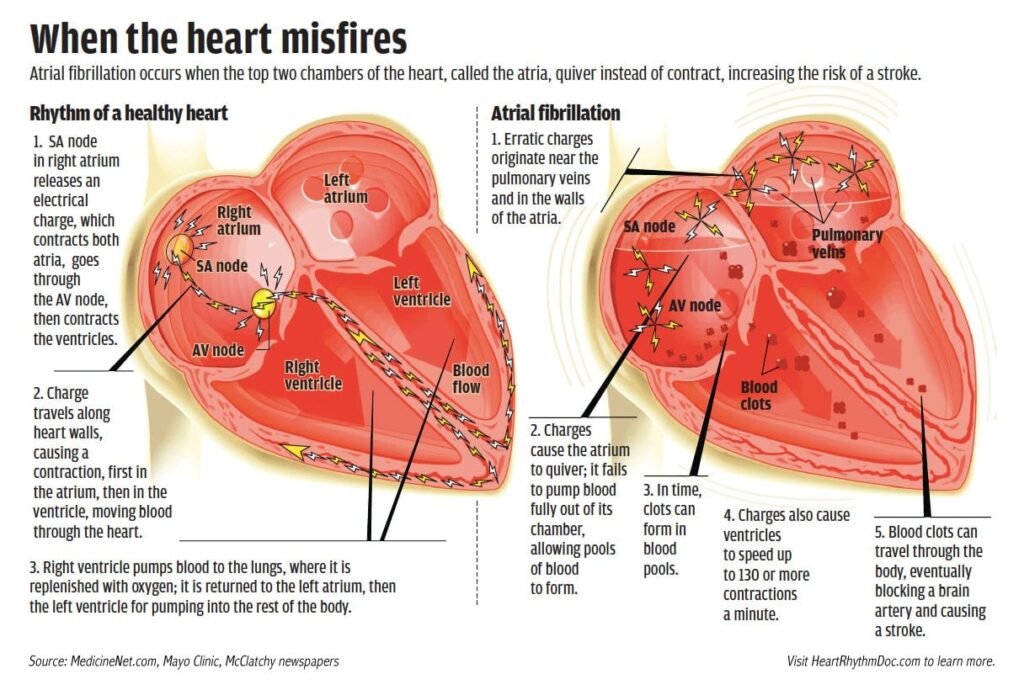
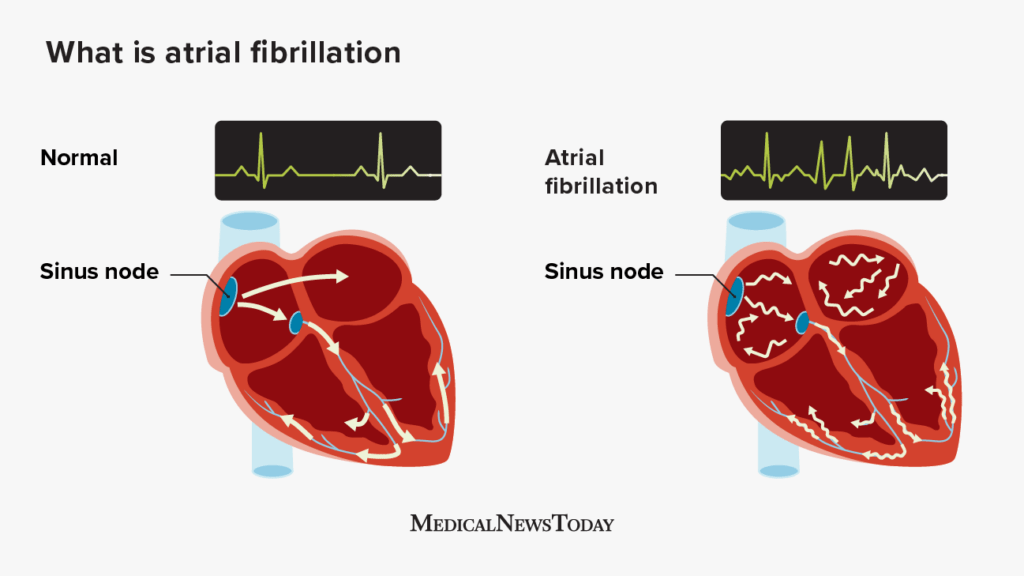
Atrial fibrillation (AFib) is a type of irregular heartbeat that occurs when the upper chambers of your heart (the atria) beat chaotically and out of sync with the lower chambers (the ventricles). In a normal heart rhythm, the electrical signals that control your heartbeat travel in a regular pattern, allowing for efficient and coordinated contraction of the heart muscles. However, in AFib, these signals become disorganized, causing the atria to quiver instead of contracting properly. This can lead to a range of symptoms and complications, affecting the overall health of your heart.
Prevalence
Atrial fibrillation is the most common type of arrhythmia, affecting millions of people worldwide. Its prevalence increases with age, and it is more common in men than in women. According to the American Heart Association, approximately 2.7 million Americans are living with AFib. This number is expected to rise significantly as the population ages. As AFib is an age-related condition, it is important for individuals to be aware of the risk factors and symptoms to ensure timely diagnosis and treatment.
Causes
The exact cause of atrial fibrillation is often unclear, but several factors can contribute to its development. Common causes include:
- High blood pressure: Uncontrolled hypertension can strain the heart and increase the risk of developing AFib.
- Heart diseases: Conditions such as coronary artery disease, heart valve disorders, heart failure, and congenital heart defects can disrupt the normal electrical signals in the heart.
- Age: The risk of AFib increases with age, particularly in individuals over 60 years old.
- Thyroid problems: An overactive or underactive thyroid gland can contribute to the development of AFib.
- Sleep apnea: Obstructive sleep apnea, a condition characterized by interrupted breathing during sleep, has been linked to an increased risk of AFib.
- Chronic conditions: Chronic lung disease, diabetes, obesity, and kidney disease are among the health conditions associated with a higher risk of AFib.
- Alcohol and stimulant use: Excessive alcohol consumption, as well as the use of illicit drugs or stimulants, can trigger episodes of AFib.
It is important to note that in some cases, the exact cause of AFib might remain unknown, despite thorough medical evaluation.
Symptoms of Atrial Fibrillation
Heart Palpitations
One of the most common symptoms of atrial fibrillation is the sensation of a fast, irregular, or pounding heartbeat, also known as heart palpitations. You may feel like your heart is racing or fluttering in your chest. These palpitations can be unsettling and may occur intermittently or persistently. It is important to monitor and report these symptoms to your healthcare provider for proper diagnosis and treatment.
Shortness of Breath
Atrial fibrillation can reduce the heart’s ability to pump blood effectively, leading to inadequate blood flow to the body’s tissues and organs. This can result in shortness of breath, especially during physical exertion or even at rest. You may feel a sense of breathlessness or difficulty catching your breath. If you experience persistent or worsening shortness of breath, it is crucial to seek medical attention promptly.
Fatigue
The irregular and inefficient heartbeat associated with AFib can cause fatigue and low energy levels. You may feel easily tired, even with minimal physical activity or during normal daily tasks. Fatigue can significantly impact your quality of life and overall well-being. Managing your symptoms and seeking appropriate treatment can help alleviate this symptom and improve your energy levels.
Dizziness
In some individuals with atrial fibrillation, the irregular heart rhythm can affect blood flow to the brain, resulting in dizziness or lightheadedness. You may feel unsteady on your feet or have a sensation of spinning or faintness. It is important to be cautious when experiencing dizziness, as it can increase the risk of falls and injuries. Consult with your healthcare provider if you experience frequent or persistent episodes of dizziness.
Diagnosis of Atrial Fibrillation
Medical History and Physical Examination
The diagnosis of atrial fibrillation often begins with a comprehensive medical history review and physical examination. Your healthcare provider will inquire about your symptoms, medical conditions, and any potential triggers or risk factors. They will also listen to your heart with a stethoscope to detect irregular heart sounds, such as abnormal heart rhythms or murmurs.
Electrocardiogram (ECG)
The gold standard test for diagnosing atrial fibrillation is an electrocardiogram (ECG). This non-invasive test measures the electrical activity of your heart and produces a visual representation (electrocardiogram) that shows the patterns and rhythm of your heartbeat. An ECG can identify atrial fibrillation and provide important information about the duration and severity of the condition.
Holter Monitoring
In some cases, atrial fibrillation may be intermittent, making it challenging to capture during a standard ECG. Holter monitoring involves wearing a portable ECG device for 24 to 48 hours to record your heart’s electrical activity continuously. This monitoring method can provide a more comprehensive evaluation of your heart rhythm and help identify any intermittent episodes of AFib that may be missed during a routine ECG.
Event Recorder
Similar to Holter monitoring, an event recorder is a portable device that you can use to record your heart’s electrical activity when you experience symptoms. The device can be worn for a longer period, such as 30 days, and activated whenever you feel palpitations, shortness of breath, or other AFib-related symptoms. This allows your healthcare provider to capture specific episodes of abnormal heart rhythm and assess their underlying causes.
Echocardiogram
An echocardiogram is an ultrasound test that uses sound waves to create detailed images of your heart’s structure and function. This test can evaluate the size, shape, and pumping ability of the heart, as well as detect any structural abnormalities or blood clots. Echocardiography is frequently performed to assess the impact of AFib on the heart and determine the appropriate management or treatment options.
Blood Tests
Blood tests may be ordered as part of the diagnostic process to check for underlying conditions that could contribute to atrial fibrillation or its complications. These tests may include a complete blood count (CBC), thyroid function tests, and specific cardiac biomarkers. Blood samples can provide valuable information about your overall health and identify any potential factors that need to be addressed or managed.
Complications Associated with Atrial Fibrillation
Stroke
One of the most significant complications of atrial fibrillation is an increased risk of stroke. The disorganized electrical signals in the atria can cause blood to pool and form clots. If a clot travels to the brain and blocks a blood vessel, it can result in an ischemic stroke. Individuals with AFib are five times more likely to have a stroke compared to the general population. To minimize this risk, various preventive measures such as anticoagulant medications may be prescribed.
Heart Failure
Atrial fibrillation can lead to a decline in the heart’s pumping capacity over time, increasing the risk of heart failure. Heart failure occurs when the heart cannot pump enough blood to meet the body’s needs. Symptoms of heart failure include shortness of breath, fatigue, swelling in the legs, and fluid retention. Managing AFib through appropriate treatment and lifestyle modifications is crucial for preventing or managing heart failure.
Cardiac Arrest
Although relatively rare, atrial fibrillation can potentially lead to cardiac arrest. In this life-threatening condition, the heart suddenly stops beating effectively, resulting in an immediate loss of consciousness and cessation of vital functions. Prompt medical attention and immediate cardiopulmonary resuscitation (CPR) are essential in such cases. For individuals with known AFib, it is important to follow a treatment plan and be vigilant about managing symptoms to minimize the risk of cardiac arrest.
Blood Clots
The irregular blood flow and pooling of blood in the atria during AFib can increase the likelihood of blood clot formation. These clots can travel through the bloodstream and cause blockages in other organs or blood vessels, leading to various complications. Blood clots can cause deep vein thrombosis (DVT), pulmonary embolism, or other organ-specific conditions. Anticoagulant medications or other preventive measures may be recommended to reduce the risk of blood clots in individuals with AFib.
Treatment Options for Atrial Fibrillation
Medication
Medication is often the first line of treatment for individuals with atrial fibrillation, particularly for managing symptoms and reducing the risk of complications. Antiarrhythmic drugs, such as beta-blockers, calcium channel blockers, and sodium channel blockers, can help regulate heart rhythm and control the heart rate. Anticoagulant medications, such as warfarin or direct oral anticoagulants (DOACs), are commonly prescribed to prevent blood clots and reduce the risk of stroke.
Cardioversion
Cardioversion is a procedure used to restore a normal heart rhythm in individuals with atrial fibrillation. It can be performed using medications or electrical shock (electrical cardioversion). During electrical cardioversion, a controlled electric shock is delivered to the heart through paddles or patches placed on the chest. This shock interrupts the chaotic electrical activity and allows the heart to reset to a normal rhythm. It is often followed by the use of antiarrhythmic medications to maintain a stable heart rhythm.
Catheter Ablation
Catheter ablation is a minimally invasive procedure performed by an electrophysiologist to treat atrial fibrillation. It involves the use of specialized catheters that are threaded through blood vessels to the heart. The catheters deliver radiofrequency energy or extreme cold (cryoablation) to specific areas of the heart that are responsible for the abnormal electrical signals causing AFib. This technique scarifies the tissue, creating a barrier that prevents the irregular electrical signals from being transmitted and thereby restoring a normal heart rhythm.
Surgical Maze Procedure
The surgical maze procedure is a surgical option for individuals with atrial fibrillation who have not responded to other treatment approaches. It involves creating a pattern of scar tissue in the atria using surgical incisions or ablation techniques. This scar tissue disrupts the abnormal electrical pathways, guiding the heart’s electrical activity into a more regular pattern. The surgical maze procedure can be performed as an open-heart surgery or in conjunction with other cardiac surgeries, such as coronary artery bypass grafting.
Pacemaker
In some cases, individuals with atrial fibrillation may require a pacemaker to regulate their heart rhythm. A pacemaker is a small device implanted under the skin near the collarbone, and it uses electrical impulses to keep the heart beating at a regular pace. Pacemakers are commonly used when AFib coexists with other heart rhythm abnormalities, such as bradycardia (a slow heart rate). By maintaining a steady heart rhythm, a pacemaker can help manage AFib symptoms and improve overall heart function.
Lifestyle Modifications for Managing Atrial Fibrillation
Quit Smoking
Smoking is a significant risk factor for the development and progression of atrial fibrillation. The chemicals present in tobacco smoke can damage the heart and blood vessels, leading to increased inflammation and oxidative stress. Quitting smoking can significantly improve heart health and reduce the risk of AFib-related complications. If you are a smoker, consider seeking professional help, using nicotine replacement therapies, or joining support programs to quit smoking.
Limit Alcohol Intake
Excessive alcohol consumption has been associated with an increased risk of developing atrial fibrillation. Alcohol can disrupt the normal electrical activity of the heart and trigger AFib episodes. It is recommended to limit alcohol intake or completely abstain to help manage AFib symptoms and reduce the risk of complications. If you need assistance in reducing or quitting alcohol consumption, reach out to healthcare professionals or support groups specialized in addiction management.
Maintain a Healthy Weight
Being overweight or obese can strain the heart and increase the risk of developing atrial fibrillation. Losing excess weight through a combination of healthy eating and regular exercise can help manage AFib symptoms and improve heart health. Consult with a healthcare professional or registered dietitian to develop a personalized weight loss plan that suits your needs and incorporates balanced nutrition.
Exercise Regularly
Regular physical activity is beneficial for overall cardiovascular health and can help manage atrial fibrillation. Engaging in moderate-intensity aerobic exercises, such as brisk walking, swimming, or cycling, for at least 150 minutes per week can promote heart fitness and reduce the risk of AFib-related complications. It is important to consult with your healthcare provider before starting an exercise program and to follow their recommended guidelines to ensure safety and effectiveness.
Reduce Stress
Stress can trigger AFib episodes and worsen symptoms. Learning and practicing stress management techniques, such as deep breathing exercises, meditation, yoga, or mindfulness, can help alleviate stress levels and promote heart health. Additionally, engaging in activities you enjoy, spending time with loved ones, and maintaining a healthy work-life balance can contribute to better emotional well-being and potentially reduce the frequency or severity of AFib episodes.
Prevention of Atrial Fibrillation
Manage Underlying Health Conditions
Addressing and managing underlying health conditions is crucial for preventing the onset or progression of atrial fibrillation. Conditions such as high blood pressure, diabetes, and thyroid disorders should be carefully monitored and treated to reduce the risk of AFib. Following your healthcare provider’s recommendations for medication management, regular check-ups, and lifestyle modifications can play a pivotal role in maintaining overall heart health.
Control Blood Pressure
High blood pressure is a significant risk factor for atrial fibrillation. It can strain the heart and increase the likelihood of developing arrhythmias. Monitoring blood pressure regularly, taking prescribed medications as directed, and implementing lifestyle modifications, such as reducing salt intake and maintaining a healthy weight, can help control blood pressure levels and reduce the risk of AFib.
Keep Cholesterol in Check
High cholesterol levels can lead to the development of atherosclerosis and increase the risk of heart disease, including atrial fibrillation. Adopting a heart-healthy diet, low in saturated and trans fats, and high in fruits, vegetables, whole grains, and lean proteins can help maintain optimal cholesterol levels. Regular cholesterol screenings and medication management, if necessary, are essential components of a comprehensive preventive strategy.
Eat a Heart-Healthy Diet
A well-balanced, heart-healthy diet can provide essential nutrients, support overall cardiovascular health, and reduce the risk of atrial fibrillation. Emphasize foods rich in fiber, vitamins, and minerals, while limiting the consumption of processed foods, sugary snacks, and saturated fats. Incorporate foods known to have cardiovascular benefits, such as fatty fish (e.g., salmon), nuts, seeds, and whole grains. Consulting with a registered dietitian can help you develop a personalized eating plan tailored to your specific needs and preferences.
Limit Caffeine
Caffeine is a stimulant that can potentially trigger or worsen atrial fibrillation in some individuals. If you notice a correlation between caffeine consumption and AFib episodes, it may be advisable to limit or avoid caffeinated beverages, such as coffee, tea, energy drinks, and certain soft drinks. Monitoring your caffeine intake and assessing its impact on your symptoms can help identify triggers and contribute to better management of atrial fibrillation.
Living with Atrial Fibrillation
Educate Yourself
Learning about atrial fibrillation and its management is crucial for living well with this condition. Understanding the causes, symptoms, treatment options, and potential complications can empower you to make informed decisions and actively participate in your healthcare. Stay updated on the latest research, seek reliable sources of information, and reach out to healthcare professionals for clarification and guidance.
Follow a Treatment Plan
Adhering to a prescribed treatment plan is essential for effectively managing atrial fibrillation. Consistently taking prescribed medications, attending medical appointments, and undergoing recommended tests ensures optimal management of symptoms and reduces the risk of complications. Do not hesitate to consult your healthcare provider if you have concerns or questions about your treatment plan or if you experience any changes in your symptoms.
Manage Stress
Stress can exacerbate atrial fibrillation symptoms and impact your overall well-being. Incorporating stress management techniques into your daily routine can help reduce the frequency and severity of AFib episodes. Explore different methods, such as meditation, deep breathing exercises, or engaging in hobbies that bring you joy and relaxation. Prioritizing self-care and finding healthy outlets to cope with stress can contribute to a better quality of life.
Monitor Your Symptoms
Keeping track of your symptoms and any changes is vital in managing atrial fibrillation. A symptom diary or journal can help you identify potential triggers and patterns, assisting your healthcare provider in making appropriate adjustments to your treatment plan. Note down any palpitations, shortness of breath, fatigue, or other symptoms you experience, along with their duration and severity. Regularly review this information with your healthcare provider during follow-up appointments.
Seek Support
Living with atrial fibrillation can be challenging, both physically and emotionally. Seek support from loved ones, join local or online support groups, or consider counseling or therapy to cope with the impact of AFib on your life. Sharing your experiences, concerns, and successes with others who understand can provide valuable emotional support and help you navigate the ups and downs of living with this condition.
Alternative and Complementary Therapies for Atrial Fibrillation
Acupuncture
Acupuncture, an ancient Chinese healing practice, involves the insertion of thin needles into specific points on the body. Some individuals with atrial fibrillation have reported symptom relief and a reduction in AFib episodes following acupuncture sessions. While the exact mechanisms are still not fully understood, it is believed that acupuncture may help regulate the autonomic nervous system, which plays a role in heart rhythm regulation. If considering acupuncture, consult with a licensed acupuncturist experienced in treating cardiovascular conditions.
Yoga and Meditation
Yoga and meditation are holistic practices that combine physical movements, breathing techniques, and mental focus. Engaging in regular yoga sessions and meditation practice may help manage stress, improve heart rate variability, and enhance overall well-being. Some individuals with atrial fibrillation have found these practices beneficial in reducing AFib symptoms and promoting a sense of calm. However, it is crucial to consult with a qualified instructor to ensure proper technique and safety.
Herbal Supplements
Certain herbal supplements, such as hawthorn, motherwort, and valerian root, have been traditionally used to support heart health and regulate heart rhythm. However, it is important to approach herbal supplements with caution and consult with a healthcare professional before incorporating them into your treatment plan. Herbal supplements may interact with medications or have unintended side effects. It is also important to ensure the quality and safety of the supplements you choose, as not all products on the market are regulated.
Biofeedback
Biofeedback is a technique that allows individuals to gain voluntary control over specific bodily functions. It involves using electronic devices to measure and provide feedback on physiological signals, such as heart rate and blood pressure. Through practice and training, individuals can learn to regulate these functions and potentially influence heart rhythm. Biofeedback may be used as a complementary therapy in the management of atrial fibrillation under the guidance of a trained professional.
Chiropractic Care
Chiropractic care focuses on the diagnosis and treatment of conditions affecting the musculoskeletal system, particularly the spine. Some individuals with atrial fibrillation have reported improvements in symptoms and well-being following chiropractic adjustments. While the exact mechanisms and effectiveness of chiropractic care for AFib are still being studied, it is important to consult with a licensed chiropractor experienced in managing cardiovascular conditions if considering this therapy.
Research and Future Perspectives
Advancements in Medications
Ongoing research and development efforts are dedicated to improving medications for atrial fibrillation management. Various antiarrhythmic drugs and anticoagulant medications are being studied to enhance their efficacy, reduce side effects, and optimize their use in specific patient populations. Additionally, novel therapeutic targets are being explored, and clinical trials are underway to evaluate the safety and effectiveness of new medications for AFib treatment and prevention.
Innovative Treatment Approaches
Non-pharmacological treatment modalities, such as emerging technologies and procedural advancements, are being investigated for atrial fibrillation management. These include techniques such as cryoablation, high-frequency ultrasound, and novel implantable devices designed to modulate heart rhythm. These innovative approaches aim to provide more precise and effective treatments while minimizing risks and improving patient outcomes.
Impact of Wearable Devices
The rise of wearable devices, including smartwatches and fitness trackers, has the potential to transform atrial fibrillation management. These devices can monitor heart rate, detect irregular rhythms, and provide real-time data to individuals and healthcare providers. The integration of advanced algorithms and artificial intelligence enables the early detection and notification of AFib episodes, empowering proactive intervention and timely medical care.
Genetic Studies
Understanding the genetic underpinnings of atrial fibrillation is an active area of research. Genetic studies aim to identify specific genes or gene variants associated with AFib susceptibility, development, and response to treatment. This knowledge can pave the way for personalized medicine approaches, enabling tailored therapies based on an individual’s genetic profile. Additionally, genetic testing may help identify individuals at increased risk of AFib, allowing early interventions and preventive measures.
As researchers continue to deepen their understanding of atrial fibrillation, it is expected that these advancements and future perspectives will contribute to more targeted and effective management strategies, improving the overall outcomes and quality of life for individuals living with AFib.
