You may have heard of Celiac Disease, a condition that affects the digestive system. But did you know that it can also lead to nutritional deficiencies? This article explores the connection between Celiac Disease and an inadequate intake of essential nutrients, such as iron, calcium, and vitamin B12. Understanding this link is crucial for those with Celiac Disease, as it highlights the importance of maintaining a balanced diet and seeking proper medical guidance to manage the condition effectively. Discover how Celiac Disease can impact your body’s ability to absorb vital nutrients and find out practical tips for ensuring your nutritional needs are met.
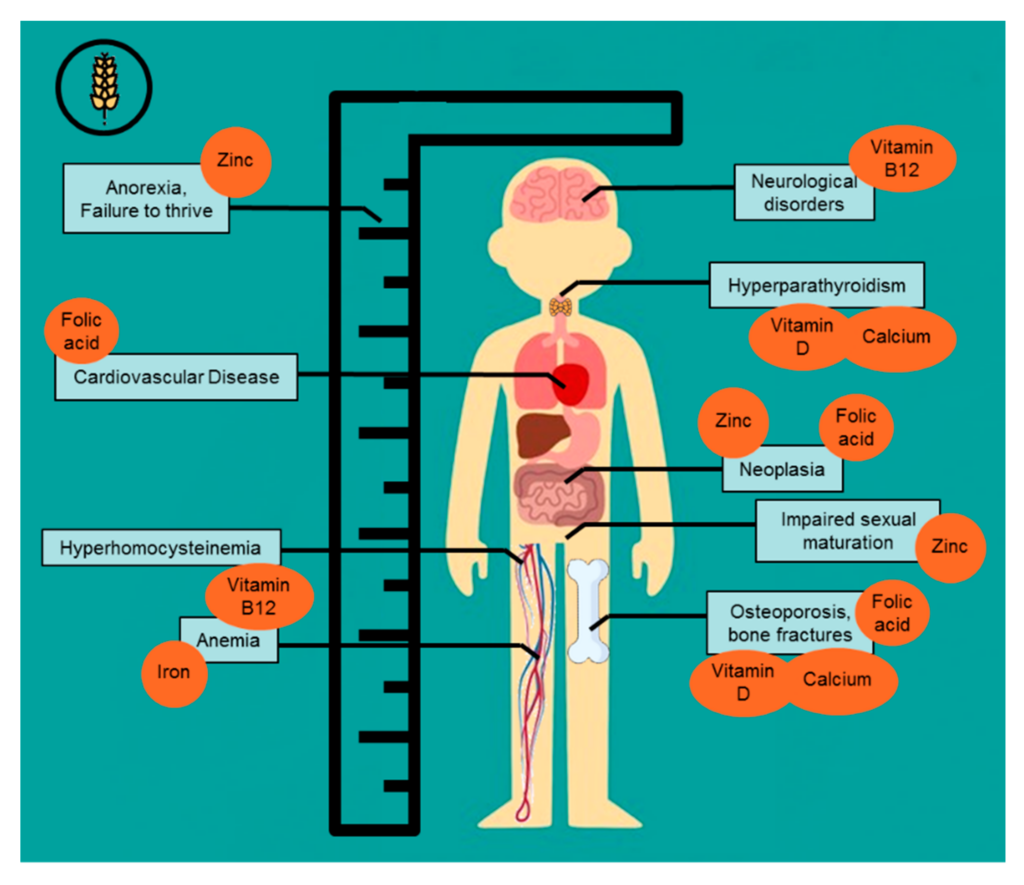
Overview of Celiac Disease
Definition of celiac disease
Celiac disease is a chronic autoimmune disorder that affects the small intestine. It is triggered by the consumption of gluten, a protein found in wheat, barley, and rye. When someone with celiac disease ingests gluten, their immune system responds by attacking the lining of the small intestine, resulting in inflammation and damage to the villi, which are responsible for nutrient absorption. This damage can lead to various nutritional deficiencies and other health complications.
Prevalence and impact on population
Celiac disease is more common than previously thought, affecting approximately 1% of the global population. However, many cases go undiagnosed due to the wide range of symptoms, which can vary greatly from person to person. Celiac disease can affect individuals of any age or background, and it is often diagnosed in childhood. The impact of the disease on an individual’s quality of life can be significant, as it requires adherence to a strict gluten-free diet and can lead to complications if not properly managed.
Causes and triggers of celiac disease
The exact cause of celiac disease is unknown, but it is believed to be a combination of genetic and environmental factors. Certain genes can predispose individuals to develop celiac disease, and the presence of gluten in the diet triggers the immune response. Other factors, such as viral infections, stress, and gut microbiota, may also play a role in the development of the disease.
Symptoms and diagnosis
Celiac disease can manifest with a wide range of symptoms, making it challenging to diagnose. Common symptoms include bloating, diarrhea, abdominal pain, weight loss, fatigue, and skin rashes. However, some individuals may experience no gastrointestinal symptoms at all. Diagnosis typically involves a combination of blood tests to detect specific antibodies, followed by an intestinal biopsy to confirm the presence of villous atrophy.
Treatment and management of celiac disease
The primary treatment for celiac disease is strict adherence to a gluten-free diet. This means avoiding all sources of gluten, including wheat, barley, rye, and contaminated foods. Following a gluten-free diet allows the small intestine to heal and alleviates symptoms. In some cases, additional treatment may be necessary to address complications or nutritional deficiencies. It is crucial for individuals with celiac disease to work closely with healthcare professionals, such as dietitians and gastroenterologists, to ensure proper management and support.
Malabsorption and Nutritional Deficiencies
Mechanism of malabsorption in celiac disease
In celiac disease, the immune system’s response to gluten damages the lining of the small intestine, specifically the villi. These finger-like projections are responsible for absorbing nutrients from food. When the villi are damaged, their surface area decreases, resulting in reduced absorption of nutrients. This malabsorption can lead to various nutritional deficiencies.
Impact of intestinal damage on nutrient absorption
The damage to the villi in celiac disease affects the absorption of several essential nutrients, including iron, vitamin B12, folate, calcium, vitamin D, zinc, magnesium, vitamin K, and vitamin A. The severity of malabsorption can vary from person to person, depending on the extent of intestinal damage. If left untreated, these deficiencies can have a detrimental impact on overall health and well-being.
Types of nutritional deficiencies associated with celiac disease
Celiac disease can lead to various nutritional deficiencies due to malabsorption. Some of the most common deficiencies include iron deficiency anemia, vitamin B12 deficiency, folate deficiency, calcium deficiency, vitamin D deficiency, zinc deficiency, magnesium deficiency, vitamin K deficiency, and vitamin A deficiency. The symptoms and consequences of these deficiencies vary depending on the specific nutrient involved but can range from fatigue and weakness to impaired bone health and compromised immune function.

Iron Deficiency Anemia
Relationship between celiac disease and iron deficiency anemia
Iron deficiency anemia is a common complication of celiac disease. The damaged villi in the small intestine result in impaired iron absorption, leading to low levels of iron in the body. Additionally, gluten-induced inflammation can contribute to iron deficiency by interfering with the body’s ability to utilize iron effectively.
Causes and symptoms of iron deficiency anemia
Iron deficiency anemia occurs when there is a lack of iron available for the body to produce enough healthy red blood cells. In celiac disease, this is primarily a result of malabsorption. Common symptoms of iron deficiency anemia include fatigue, weakness, shortness of breath, pale skin, and rapid heartbeat.
Importance of iron in the body
Iron is an essential nutrient that plays a crucial role in the body. It is necessary for the production of hemoglobin, the protein in red blood cells that transports oxygen throughout the body. Iron also contributes to cellular energy production and supports cognitive function.
Management of iron deficiency anemia in celiac disease
The management of iron deficiency anemia in individuals with celiac disease typically involves addressing the underlying cause, which is malabsorption. This is achieved by following a strict gluten-free diet to allow the small intestine to heal and improve nutrient absorption. Iron supplements may also be prescribed to restore iron levels in the body. Monitoring iron levels regularly and working with healthcare professionals are essential for effective management.
Vitamin B12 Deficiency
Association between celiac disease and vitamin B12 deficiency
Celiac disease can lead to vitamin B12 deficiency due to malabsorption. The damaged small intestine can impair the absorption of vitamin B12 from the diet, resulting in low levels of this vital nutrient in the body. Additionally, the presence of autoimmune conditions, often associated with celiac disease, can also contribute to vitamin B12 deficiency.
Causes and symptoms of vitamin B12 deficiency
Vitamin B12 deficiency occurs when there is a lack of this vitamin in the body. In celiac disease, malabsorption is the primary cause. Vitamin B12 is primarily found in animal-based foods, such as meat, fish, and dairy products, which individuals with celiac disease may avoid due to dietary restrictions. Symptoms of vitamin B12 deficiency may include fatigue, weakness, tingling or numbness in the hands and feet, difficulty walking, memory problems, and mood changes.
Functions and importance of vitamin B12
Vitamin B12 is essential for various bodily functions, including the production of red blood cells, DNA synthesis, and proper nervous system function. It also plays a crucial role in maintaining healthy brain function and a healthy immune system.
Strategies for managing vitamin B12 deficiency in celiac disease
The management of vitamin B12 deficiency in celiac disease primarily involves addressing malabsorption through a gluten-free diet and, if necessary, vitamin B12 supplementation. Dietary sources of vitamin B12, such as fortified foods and supplements, can help restore and maintain adequate levels of this nutrient in the body. Regular monitoring and guidance from healthcare professionals are important for managing vitamin B12 deficiency effectively.

Folate Deficiency
Link between celiac disease and folate deficiency
Celiac disease can lead to folate deficiency due to impaired absorption of this essential vitamin. The damage to the small intestine reduces the surface area available for folate absorption, resulting in low levels of this nutrient in the body. Additionally, the inflammatory response triggered by gluten ingestion can further deplete folate levels.
Causes and symptoms of folate deficiency
Folate deficiency occurs when there is a lack of this vitamin in the body. In celiac disease, malabsorption is the primary cause. Folate is mainly found in foods such as leafy greens, citrus fruits, and legumes, which may be limited in the diet of individuals with celiac disease. Symptoms of folate deficiency can include fatigue, weakness, shortness of breath, headaches, poor concentration, and irritability.
Role of folate in the body
Folate plays a vital role in numerous bodily functions, including DNA synthesis, red blood cell production, and neurological function. It is especially important during periods of rapid growth and development, such as pregnancy.
Approaches for addressing folate deficiency in celiac disease
The management of folate deficiency in individuals with celiac disease involves addressing malabsorption through a gluten-free diet. Including folate-rich foods in the diet, such as leafy greens, citrus fruits, and legumes, can help restore and maintain adequate levels of this nutrient. In some cases, folate supplementation may be necessary to ensure optimal levels. Regular monitoring and guidance from healthcare professionals are crucial for managing folate deficiency effectively.
Calcium and Vitamin D Deficiencies
Relationship between celiac disease and calcium/vitamin D deficiency
Celiac disease can lead to calcium and vitamin D deficiencies due to malabsorption and dietary restrictions. The damaged small intestine reduces the absorption of calcium, while the avoidance of dairy products, a common source of calcium and vitamin D, can further contribute to deficiencies. Additionally, impaired intestinal health can disrupt the conversion of vitamin D to its active form, exacerbating the problem.
Causes and symptoms of calcium and vitamin D deficiencies
Calcium deficiency occurs when there is inadequate calcium intake or absorption in the body. In celiac disease, malabsorption is the primary cause. Common symptoms of calcium deficiency include muscle cramps, numbness, tingling, and weak or brittle bones. Vitamin D deficiency occurs when there is an insufficient level of this vitamin in the body. In celiac disease, impaired absorption and limited dietary intake contribute to low vitamin D levels. Symptoms of vitamin D deficiency can include bone pain, muscle weakness, fatigue, and increased susceptibility to infections.
Importance of calcium and vitamin D for bone health
Calcium and vitamin D are essential for maintaining strong and healthy bones. Calcium provides the structural support for bones, while vitamin D helps the body absorb calcium from the diet. Together, they work in synergy to preserve bone density, prevent bone loss, and reduce the risk of fractures.
Management strategies for calcium and vitamin D deficiencies in celiac disease
The management of calcium and vitamin D deficiencies in individuals with celiac disease involves multiple approaches. Following a gluten-free diet and including alternative sources of calcium, such as leafy greens, nuts, and fortified dairy-free products, can help address calcium deficiency. Adequate sun exposure and dietary sources of vitamin D, such as fatty fish and fortified foods, can help alleviate vitamin D deficiency. In some cases, healthcare professionals may recommend calcium and vitamin D supplementation to ensure optimal levels. Regular monitoring and guidance are essential for effective management.
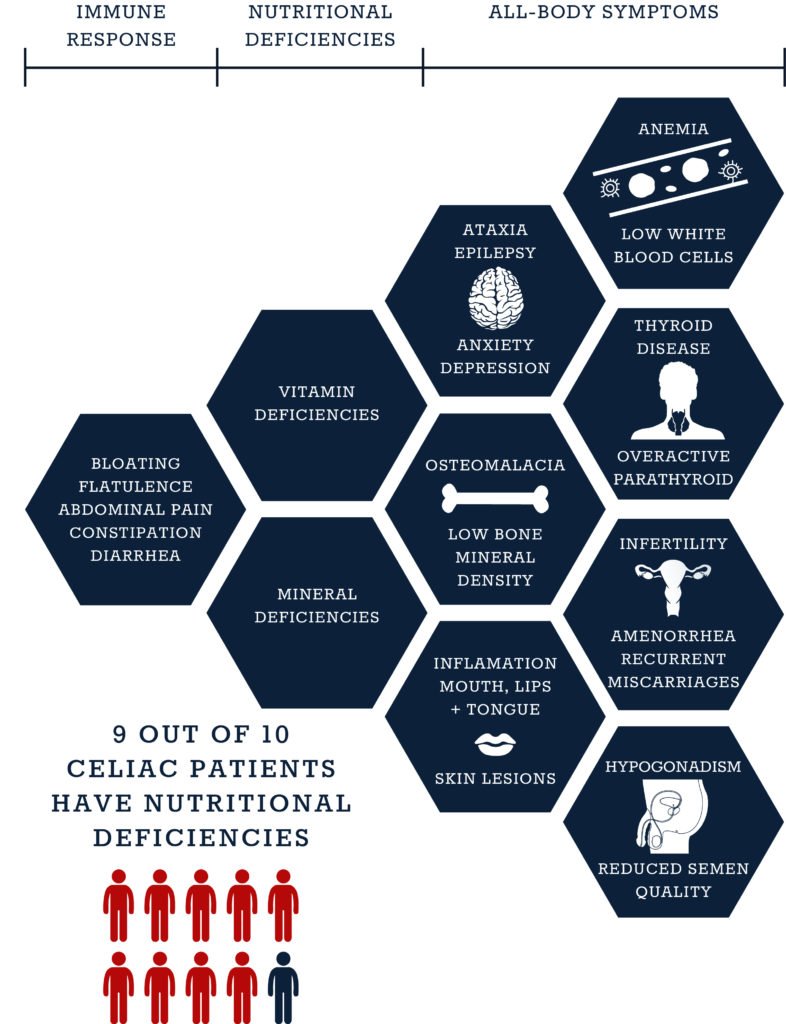
Zinc and Magnesium Deficiencies
Association between celiac disease and zinc/magnesium deficiencies
Celiac disease can lead to deficiencies in zinc and magnesium due to malabsorption and dietary limitations. The damaged small intestine impairs the absorption of these essential minerals, while a gluten-free diet can restrict food sources rich in zinc and magnesium.
Causes and symptoms of zinc and magnesium deficiencies
Zinc deficiency occurs when there is inadequate intake or absorption of this mineral in the body. In celiac disease, malabsorption is the primary cause. Symptoms of zinc deficiency can include slow wound healing, impaired immune function, hair loss, skin rashes, and loss of appetite. Magnesium deficiency occurs when there is insufficient magnesium in the body. Celiac disease can lead to magnesium deficiency due to impaired absorption. Symptoms of magnesium deficiency can include muscle cramps, weakness, fatigue, and irregular heartbeat.
Functions of zinc and magnesium in the body
Zinc and magnesium play crucial roles in numerous bodily functions. Zinc is involved in immune function, DNA synthesis, wound healing, and taste perception. Magnesium is essential for energy metabolism, nerve function, muscle relaxation, and maintaining healthy bones.
Approaches to addressing zinc and magnesium deficiencies in celiac disease
The management of zinc and magnesium deficiencies in individuals with celiac disease primarily involves addressing malabsorption through a gluten-free diet and ensuring adequate intake of these minerals. Including food sources rich in zinc, such as seafood, meat, and legumes, and magnesium, such as whole grains, nuts, and seeds, is important. In some cases, supplementation may be necessary to achieve optimal levels. Regular monitoring and guidance from healthcare professionals are essential for managing zinc and magnesium deficiencies effectively.
Vitamin K Deficiency
Link between celiac disease and vitamin K deficiency
Celiac disease can lead to vitamin K deficiency due to malabsorption and decreased production of vitamin K by gut bacteria. The damaged small intestine impairs the absorption of vitamin K, while the disruption of the gut microbiota in celiac disease can further decrease the production of this vitamin.
Causes and symptoms of vitamin K deficiency
Vitamin K deficiency occurs when there is inadequate intake or absorption of this vitamin in the body. In celiac disease, both malabsorption and reduced production contribute to vitamin K deficiency. Symptoms can include excessive bleeding or bruising, prolonged clotting time, and an increased risk of hemorrhage.
Importance of vitamin K for blood clotting and bone health
Vitamin K is essential for blood clotting, as it activates certain proteins involved in the clotting process. Additionally, vitamin K plays a role in bone health by aiding in the mineralization of bone tissue. It helps ensure sufficient calcium is deposited in the bones, contributing to their strength.
Management strategies for vitamin K deficiency in celiac disease
The management of vitamin K deficiency in individuals with celiac disease involves addressing malabsorption through a gluten-free diet and ensuring adequate intake of this vitamin. Dietary sources of vitamin K include leafy greens, broccoli, and fermented foods. In some cases, healthcare professionals may recommend vitamin K supplementation to restore and maintain optimal levels. Regular monitoring and guidance are important for effective management.

Vitamin A Deficiency
Association between celiac disease and vitamin A deficiency
Celiac disease can lead to vitamin A deficiency due to impaired absorption and limited dietary intake. The damaged small intestine results in reduced absorption of vitamin A, while avoidance of foods rich in vitamin A, such as liver, eggs, and dairy products, can further contribute to deficiencies.
Causes and symptoms of vitamin A deficiency
Vitamin A deficiency occurs when there is insufficient intake or absorption of this vitamin in the body. In celiac disease, both malabsorption and dietary restrictions can contribute to low levels of vitamin A. Symptoms can include vision problems, dry skin, poor night vision, increased susceptibility to infections, and impaired growth.
Functions and importance of vitamin A
Vitamin A plays a crucial role in various bodily functions. It is essential for maintaining healthy vision, promoting proper immune function, supporting growth and development, and contributing to healthy skin and mucous membranes.
Approaches for managing vitamin A deficiency in celiac disease
The management of vitamin A deficiency in individuals with celiac disease primarily involves addressing malabsorption through a gluten-free diet and ensuring adequate intake of vitamin A from alternative food sources. It is important to include foods rich in beta-carotene, a precursor of vitamin A, such as orange and yellow vegetables, leafy greens, and fruits. In some cases, healthcare professionals may recommend vitamin A supplementation to restore and maintain optimal levels. Regular monitoring and guidance are essential for managing vitamin A deficiency effectively.
Conclusion
In conclusion, celiac disease is a chronic autoimmune disorder that can result in various nutritional deficiencies due to malabsorption and dietary restrictions. Iron deficiency anemia, vitamin B12 deficiency, folate deficiency, calcium and vitamin D deficiencies, zinc and magnesium deficiencies, vitamin K deficiency, and vitamin A deficiency are common deficiencies seen in individuals with celiac disease. These deficiencies can have significant impacts on overall health and well-being, affecting energy levels, bone health, immune function, and more. Early diagnosis and appropriate dietary management are crucial in mitigating these deficiencies and preventing further complications. Healthcare professionals, including dietitians and gastroenterologists, play a vital role in assessing and addressing nutritional deficiencies, providing guidance and support to individuals with celiac disease. By working together, individuals with celiac disease can effectively manage their condition and maintain optimal health.
