Celiac Disease is a condition that affects millions of people worldwide, yet diagnosing it can often be complicated. Understanding the key aspects of Celiac Disease diagnosis is crucial not only for those who suspect they may have the condition, but also for healthcare professionals looking to accurately identify and treat patients. In this article, you will learn everything you need to know about Celiac Disease diagnosis, from the common symptoms to the various testing methods available. So, whether you are personally affected by Celiac Disease or simply curious about the topic, let’s explore the ins and outs of diagnosing this often misunderstood condition.

What is Celiac Disease?
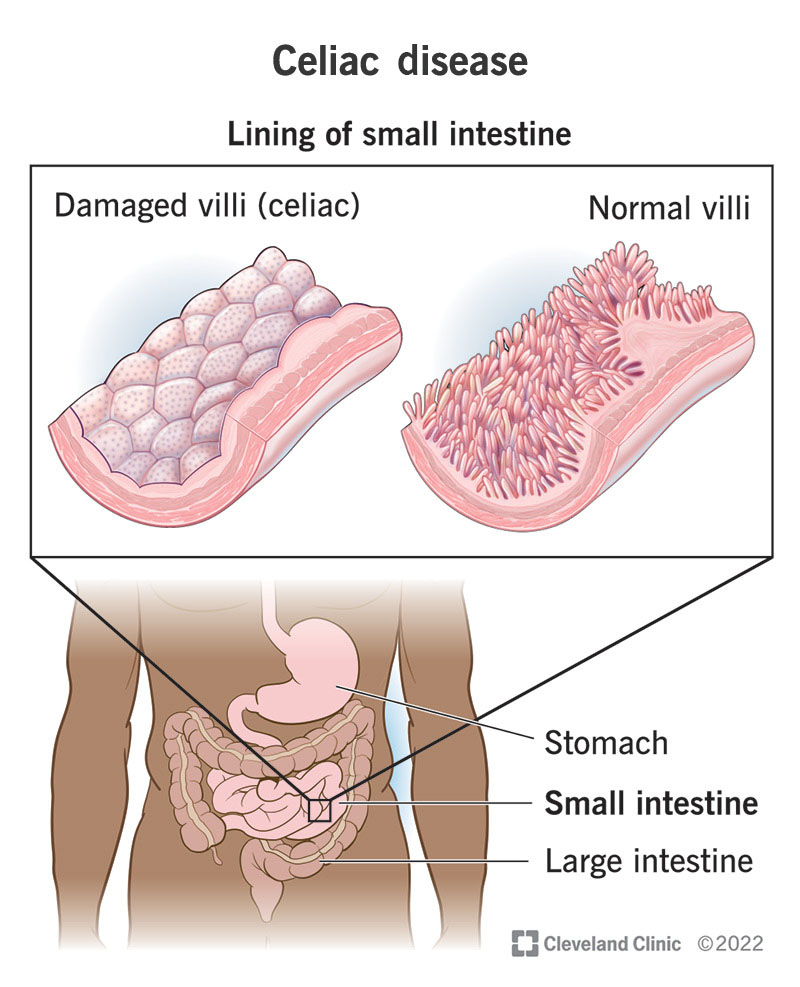
Celiac disease is a chronic autoimmune disorder that affects the small intestine. When individuals with celiac disease consume gluten, a protein found in wheat, barley, and rye, their immune system responds by attacking the lining of the small intestine. Over time, this immune response can lead to damage and inflammation in the small intestine, preventing the absorption of nutrients from food. This damage to the small intestine can result in a wide range of symptoms and long-term health complications if left untreated.
Definition of Celiac Disease
Celiac disease is defined as an immune-mediated disorder that is triggered by the ingestion of gluten. It is important to note that celiac disease is not the same as a gluten intolerance or sensitivity. While individuals with a gluten intolerance may experience similar symptoms, they do not have the same autoimmune response and resulting damage to the small intestine. Celiac disease is a lifelong condition that requires strict adherence to a gluten-free diet.
Causes of Celiac Disease
The exact cause of celiac disease is not fully understood, but it is believed to be a combination of genetic and environmental factors. Certain genes, specifically the human leukocyte antigen (HLA) genes, are associated with an increased risk of developing celiac disease. However, not everyone with these genes will develop the condition. Environmental factors, such as the introduction of gluten into the diet, may also play a role in triggering the immune response in susceptible individuals.
Symptoms of Celiac Disease
The symptoms of celiac disease can vary widely from person to person, and some individuals may experience no symptoms at all. Common symptoms of celiac disease include gastrointestinal issues such as diarrhea, abdominal pain, bloating, and constipation. Other symptoms may include fatigue, unexplained weight loss, anemia, skin rash, and delayed growth in children. It is important to note that the symptoms of celiac disease can be similar to those of other conditions, which can make diagnosis challenging.

Prevalence and Risk Factors
Celiac disease is estimated to affect approximately 1% of the global population. It can occur at any age, from infancy to adulthood. Certain populations, such as individuals with a family history of celiac disease or other autoimmune disorders, are at a higher risk of developing the condition. Additionally, individuals with certain genetic factors, such as specific HLA genes, are also at an increased risk.
Testing for Celiac Disease
If you suspect you may have celiac disease, it is important to consult a healthcare professional for proper testing and diagnosis. There are several different methods used to diagnose celiac disease, including blood tests, genetic testing, intestinal biopsy, and other diagnostic approaches. The choice of testing method may vary depending on individual circumstances and the preferences of the healthcare provider.

When to Consider Testing
Testing for celiac disease should be considered if you are experiencing symptoms that may be indicative of the condition, or if you have a family history of celiac disease or other autoimmune disorders. It is important to continue consuming gluten prior to testing, as a gluten-free diet can affect the accuracy of the results. However, if you have already eliminated gluten from your diet, it may be necessary to reintroduce it for a period of time before testing.
Blood Tests
Blood tests are commonly used to screen for celiac disease. These tests measure the levels of certain antibodies in the blood that are indicative of an immune response to gluten. The most common blood tests for celiac disease include deamidated gliadin peptide (DGP) antibodies, tissue transglutaminase (tTG) antibodies, and endomysial antibodies (EMA). In addition, a total immunoglobulin A (IgA) test may be performed to assess for IgA deficiency, which can affect the accuracy of other blood tests.

Genetic Testing
Genetic testing for celiac disease involves analyzing DNA samples to identify specific HLA genes associated with an increased risk of developing the condition. This type of testing can be useful in certain situations, such as when there is uncertainty regarding the diagnosis or for family members of individuals with celiac disease. It is important to note that genetic testing alone cannot diagnose celiac disease, as not all individuals with the associated genes will develop the condition.
Intestinal Biopsy
An intestinal biopsy is considered the gold standard for diagnosing celiac disease. During this procedure, a small sample of tissue is taken from the lining of the small intestine and examined for signs of damage or inflammation. This procedure is typically performed using an endoscope, a thin tube with a camera on the end, which is inserted through the mouth and into the small intestine. The sample is then sent to a laboratory for analysis.
Other Diagnostic Methods
In addition to blood tests and intestinal biopsy, there are other diagnostic methods that may be used to assess for celiac disease or gluten sensitivity. Serologic tests for gluten sensitivity can help identify individuals who may experience symptoms similar to celiac disease but do not have the characteristic immune response. Elimination diets and food diaries can also be useful in identifying specific food triggers and determining if gluten is causing symptoms. Capsule endoscopy and cross-contamination testing are additional methods that may be used in certain cases.
The Importance of Diagnosis
Diagnosing celiac disease is essential in order to properly manage the condition and prevent long-term health complications. Without a diagnosis, individuals with celiac disease may continue to consume gluten, resulting in ongoing damage to the small intestine. Additionally, celiac disease is associated with an increased risk of developing other autoimmune disorders and certain types of cancer, making early diagnosis and intervention crucial for long-term health.
Long-Term Health Risks
If left untreated, celiac disease can lead to a range of long-term health complications. The chronic inflammation and damage to the small intestine can result in malabsorption of nutrients, leading to deficiencies in vitamins, minerals, and other essential nutrients. This can result in a variety of health issues, including osteoporosis, anemia, infertility, and neurological disorders. Managing celiac disease through a gluten-free diet can help reduce the risk of these long-term complications.
Avoiding Gluten
The primary treatment for celiac disease is strict adherence to a gluten-free diet. This means avoiding all sources of gluten, including wheat, barley, and rye, as well as any products that may contain hidden sources of gluten. Reading food labels carefully and seeking out gluten-free alternatives is essential for individuals with celiac disease. It is important to note that even small amounts of gluten can cause damage to the small intestine, so cross-contamination must be avoided.
Monitoring for Associated Conditions
Individuals with celiac disease are at increased risk for developing other autoimmune disorders, such as type 1 diabetes, thyroid disease, and rheumatoid arthritis. Regular monitoring for these associated conditions is important to ensure early detection and treatment. Additionally, individuals with celiac disease may also be at a higher risk for certain types of cancer, particularly lymphoma and adenocarcinoma of the small intestine. Regular screenings and check-ups with healthcare professionals are important for ongoing monitoring.
Family Screening and Genetic Counseling
Celiac disease has a strong genetic component, so it is important for family members of individuals with the condition to undergo screening. Even in the absence of symptoms, individuals with the associated genes may be at an increased risk of developing celiac disease in the future. Genetic counseling can also be beneficial in helping individuals and their families understand the risks, implications, and management strategies associated with celiac disease.
Differential Diagnosis
Distinguishing celiac disease from other conditions can sometimes be challenging, as the symptoms can overlap with other gastrointestinal disorders. Some of the conditions that need to be considered in the differential diagnosis include wheat allergy, non-celiac gluten sensitivity, irritable bowel syndrome, and inflammatory bowel disease. Proper evaluation and testing by a healthcare professional are essential in order to differentiate between these conditions and ensure accurate diagnosis.
Potential Challenges in Diagnosis
Diagnosing celiac disease can present several challenges due to the variability of symptoms and the potential for atypical presentations. While some individuals may experience the classic gastrointestinal symptoms, others may have more subtle symptoms or even no symptoms at all. Additionally, symptoms of celiac disease can overlap with other disorders, which can make diagnosis more difficult. In some cases, there may also be a delay in diagnosis, which can result in ongoing damage and complications.
Seeking Professional Medical Advice
If you suspect you may have celiac disease, it is important to seek professional medical advice from a gastroenterologist or another healthcare professional specializing in celiac disease. These professionals have the knowledge and expertise to properly evaluate your symptoms, order the necessary tests, and provide a comprehensive diagnosis. Collaborating with a registered dietitian who specializes in celiac disease can also be beneficial in developing a personalized gluten-free diet plan and navigating the challenges of living with the condition.
Multidisciplinary Approach
Celiac disease is a complex condition that can impact multiple aspects of an individual’s health and well-being. Therefore, a multidisciplinary approach to diagnosis and management is often recommended. This may involve collaborating with various healthcare professionals, such as gastroenterologists, dietitians, allergists, and psychologists, to ensure comprehensive care. Regular follow-up care and ongoing communication with healthcare providers are vital for maintaining optimal health and managing the condition effectively.
In conclusion, diagnosing celiac disease involves a combination of medical evaluation, testing, and collaboration with healthcare professionals. Early diagnosis and intervention are crucial for preventing long-term health complications and improving quality of life. If you suspect you may have celiac disease, it is important to consult a healthcare professional who can guide you through the diagnostic process and provide the necessary support and resources for managing the condition. Remember, you are not alone in this journey, and there are healthcare professionals and resources available to help you navigate the challenges of living with celiac disease.