Congratulations on your pregnancy! As you embark on this exciting journey, it is important to be aware of the potential impact that diabetes mellitus can have on both you and your baby. Diabetes mellitus, a chronic condition characterized by high blood sugar levels, requires special attention during pregnancy to ensure a healthy outcome for both mother and child. This article will provide you with valuable information and insights on managing diabetes mellitus during pregnancy, empowering you to make informed decisions and take necessary precautions for a successful and joyful pregnancy.
Prevalence of Diabetes Mellitus in Pregnancy
Diabetes Mellitus is a chronic condition that affects millions of people worldwide. During pregnancy, the prevalence of diabetes mellitus, including gestational diabetes mellitus (GDM) and pre-existing diabetes mellitus, increases significantly. This article aims to provide a comprehensive overview of diabetes mellitus in pregnancy, including risks, diagnosis, management, care during pregnancy, and long-term implications for both the mother and the baby.
Gestational Diabetes Mellitus (GDM)
Gestational diabetes mellitus (GDM) refers to the development of diabetes during pregnancy in women who did not previously have diabetes. It is estimated that GDM affects approximately 7% of all pregnancies. This condition occurs when the body is unable to produce enough insulin to meet the increased demands during pregnancy. GDM usually resolves after delivery, but it increases the risk of developing type 2 diabetes later in life.
Pre-existing Diabetes Mellitus
Pre-existing diabetes mellitus refers to diabetes that existed before pregnancy. This can include type 1 diabetes, type 2 diabetes, or other forms of diabetes. Women with pre-existing diabetes mellitus require careful management of their blood sugar levels to ensure a healthy pregnancy. It is essential for these women to have optimal blood glucose control before conception to reduce the risk of complications during pregnancy.
Risks and Complications
Both GDM and pre-existing diabetes mellitus pose risks and complications for both the mother and the baby. It is crucial to be aware of these risks and take appropriate measures to minimize them.
Maternal Risks
For the mother, poorly controlled diabetes during pregnancy increases the risk of developing high blood pressure, preeclampsia, and the need for a cesarean section. Women with diabetes are also more prone to urinary tract infections and may experience difficulties in wound healing after delivery. Additionally, poorly controlled diabetes can lead to diabetic ketoacidosis, a life-threatening condition characterized by high blood sugar levels and the presence of ketones in the urine.
Fetal Risks
Uncontrolled diabetes during pregnancy can have severe consequences for the baby. Elevated blood sugar levels in the mother can affect the baby’s development and increase the risk of birth defects, such as heart and neural tube defects. These babies are also more likely to have macrosomia (large birth weight), which can increase the risk of birth injuries during delivery. Furthermore, infants born to mothers with diabetes are at a higher risk of developing metabolic syndrome and type 2 diabetes later in life.
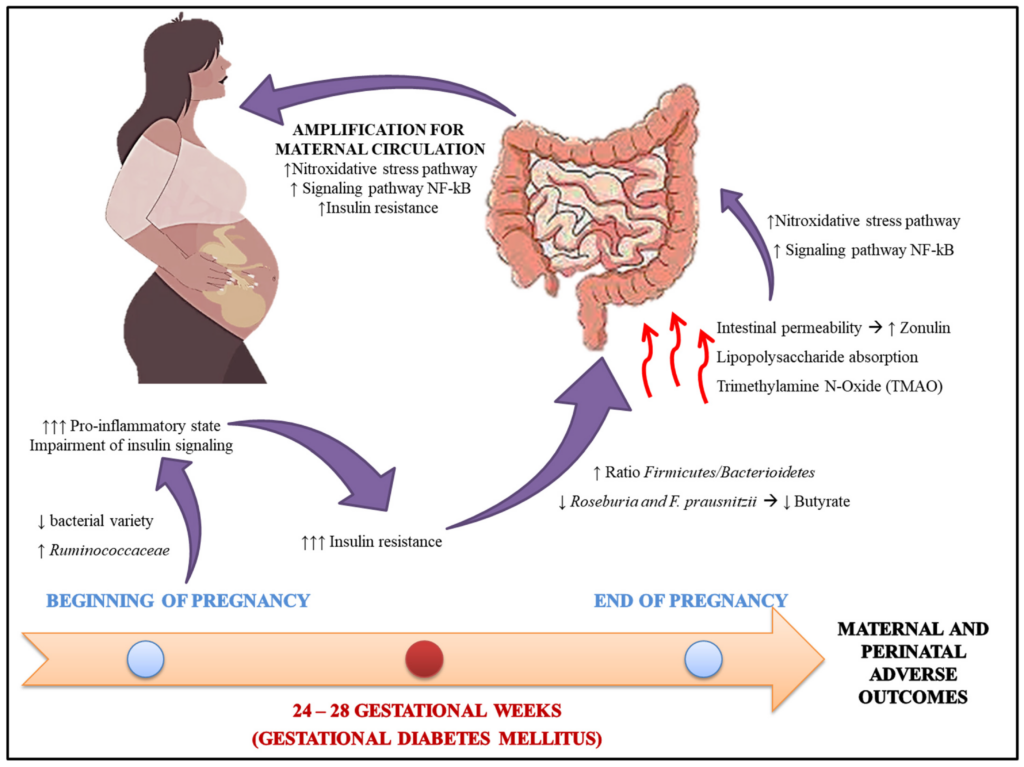
Screening and Diagnosis
Early detection and diagnosis of diabetes during pregnancy are essential for appropriate management and reducing the risk of complications. Several screening and diagnostic tests are available.
Oral Glucose Tolerance Test (OGTT)
The oral glucose tolerance test (OGTT) is commonly used to screen for gestational diabetes mellitus. This test involves having the woman drink a solution containing a specific amount of glucose, followed by blood samples at regular intervals to measure how the body processes the sugar. Abnormal results on the OGTT indicate the need for further testing to confirm the diagnosis of GDM.
Glycated Hemoglobin (HbA1c) Testing
Glycated hemoglobin (HbA1c) testing provides an indication of average blood sugar levels over the past two to three months. This test is typically used to diagnose pre-existing diabetes mellitus. A higher HbA1c level suggests poorer blood glucose control.
Blood Glucose Monitoring
Regular blood glucose monitoring is crucial for women with diabetes during pregnancy. This involves checking blood sugar levels using a glucose meter multiple times throughout the day. It helps in determining the effectiveness of diabetes management strategies and making adjustments as necessary.
Urine Testing
Urine testing for the presence of glucose and ketones can provide additional information about blood sugar control. Ketones in the urine indicate that the body is breaking down fat for energy instead of glucose, suggesting inadequate insulin levels.
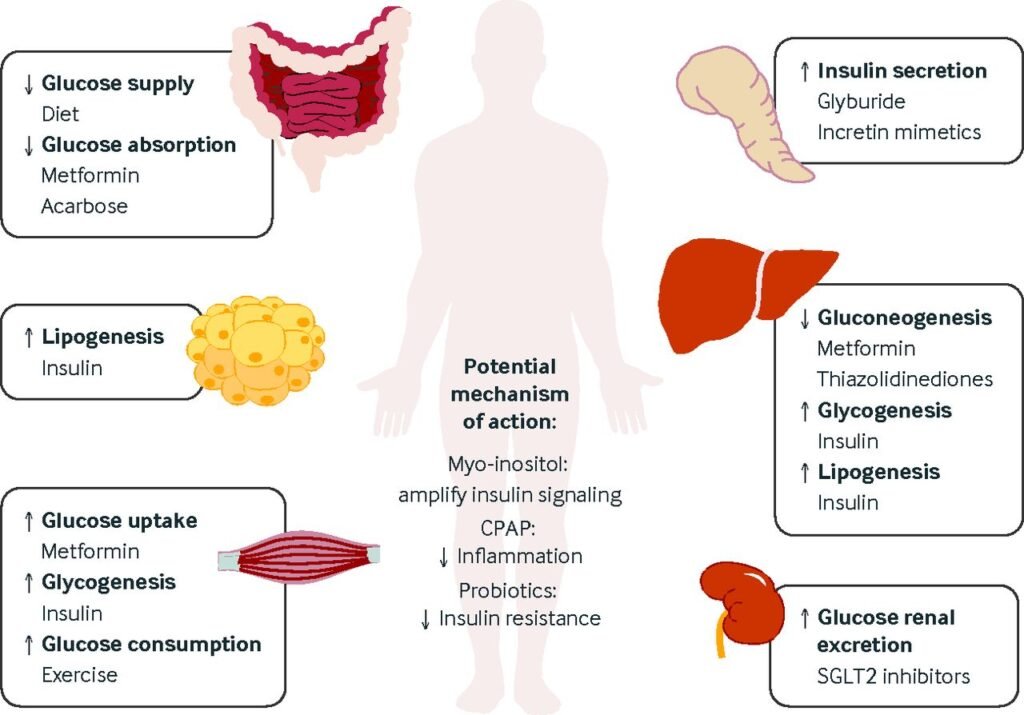
Management of Diabetes Mellitus during Pregnancy
Effective management of diabetes mellitus during pregnancy is essential to ensure the well-being of both the mother and the baby. A multidisciplinary approach involving healthcare professionals, including obstetricians, endocrinologists, dieticians, and diabetes educators, is typically employed.
Medical Management
Medical management of diabetes during pregnancy may involve medication adjustments, such as increasing insulin doses or switching to insulin therapy if previously on oral medications. Regular check-ups with healthcare providers help monitor blood sugar levels and adjust the treatment plan as needed.
Dietary Management
A healthy, balanced diet is crucial for managing diabetes during pregnancy. Women are advised to consume a variety of nutrient-rich foods while avoiding excessive carbohydrates and sugars. Dieticians can provide personalized meal plans and guidance to help women make appropriate food choices.
Physical Activity
Regular physical activity is beneficial for managing blood sugar levels and overall health during pregnancy. Low-impact exercises, such as walking or swimming, are generally recommended. However, it is essential to consult with healthcare providers before starting or continuing an exercise routine during pregnancy.
Insulin Therapy
Insulin therapy is often necessary for women with pre-existing diabetes mellitus or poorly controlled gestational diabetes mellitus. Insulin is safe to use during pregnancy and helps regulate blood sugar levels. Different types of insulin may be prescribed, including long-acting and rapid-acting insulin, depending on individual needs.
Continuous Glucose Monitoring
In some cases, continuous glucose monitoring (CGM) may be recommended. CGM involves wearing a sensor that measures glucose levels in the interstitial fluid continuously. This provides real-time data and alerts for better blood sugar control.
Self-Monitoring of Blood Glucose
Self-monitoring of blood glucose levels at home is an essential tool for managing diabetes during pregnancy. Regular monitoring helps women identify patterns and make appropriate adjustments to their diet, physical activity, and insulin doses.
Regular Check-ups and Monitoring
Frequent check-ups and monitoring throughout pregnancy are crucial for assessing the well-being of both the mother and the baby. Healthcare providers will monitor blood sugar levels, fetal growth, and any potential complications. Regular ultrasound scans and non-stress tests may be performed to assess fetal development and well-being.

Antenatal Care for Women with Diabetes
Antenatal care for women with diabetes involves a comprehensive approach to ensure optimal pregnancy outcomes. This care is typically provided by a team of healthcare professionals, including obstetricians, endocrinologists, dieticians, and diabetes educators.
Multidisciplinary Approach
A multidisciplinary approach is essential for managing diabetes during pregnancy. This team-based approach ensures that all aspects of care, including medical management, dietary advice, and lifestyle modifications, are effectively addressed.
Optimal Blood Glucose Control
Maintaining optimal blood glucose control is a primary goal of antenatal care for women with diabetes. Regular monitoring, medication adjustments, and lifestyle modifications are employed to achieve and maintain target blood sugar levels.
Fetal Surveillance
Regular fetal surveillance, including ultrasound scans and non-stress tests, is performed to assess the baby’s growth and well-being. This helps identify any potential complications and guides appropriate management decisions.
Monitoring Blood Pressure
Hypertension is a common complication in women with diabetes during pregnancy. Regular monitoring of blood pressure is important to detect and manage high blood pressure promptly.
Assessment of Fetal Growth
Monitoring and assessing fetal growth is crucial for identifying any abnormalities or deviations from the expected growth pattern. Ultrasound measurements can provide valuable information about the baby’s size and development.
Screening for Gestational Hypertension
Women with diabetes are at an increased risk of developing gestational hypertension, a condition characterized by high blood pressure during pregnancy. Regular screenings help identify this condition early and initiate appropriate management.
Labor and Delivery Care
Labor and delivery care for women with diabetes requires close monitoring and careful management to ensure the safety of both the mother and the baby.
Induction of Labor
In some cases, labor may be induced to prevent complications associated with diabetes, such as macrosomia or prolonged pregnancy. The timing of induction is determined based on various factors, including blood glucose control, fetal growth, and maternal well-being.
Mode of Delivery
The mode of delivery for women with diabetes is determined on an individual basis. Vaginal delivery is generally preferred if blood sugar levels are well controlled, and there are no other complications. However, for women with poorly controlled diabetes or other complications, a cesarean section may be recommended.
Intrapartum Blood Glucose Management
During labor, blood glucose levels are closely monitored. Insulin may be administered as needed to maintain stable blood sugar levels. Careful management of blood glucose during labor helps prevent any adverse outcomes for both the mother and the baby.
Postpartum Care
Postpartum care is an essential component of managing diabetes after delivery. It focuses on monitoring blood glucose levels, promoting breastfeeding, and providing contraception options.
Blood Glucose Monitoring
Blood glucose monitoring continues after delivery to ensure that blood sugar levels return to normal. Women with gestational diabetes mellitus may need additional testing to confirm the resolution of diabetes. Postpartum follow-up with healthcare providers is essential to address any ongoing diabetes management needs.
Breastfeeding and Diabetes
Breastfeeding is encouraged for women with diabetes, as it provides numerous health benefits for both the mother and the baby. Breastfeeding can help with postpartum weight loss and may improve blood sugar control in women with diabetes. It is important to work closely with healthcare providers to ensure optimal breastfeeding practices and monitor blood sugar levels during this time.
Contraception
Contraception options should be discussed with healthcare providers to prevent unintended pregnancies. Some forms of contraception may be more suitable for women with diabetes, considering their individual health needs.
Long-term Implications for the Mother
Having diabetes during pregnancy can have long-term implications for the mother’s health and well-being. It is important to be aware of these potential risks and take appropriate measures to mitigate them.
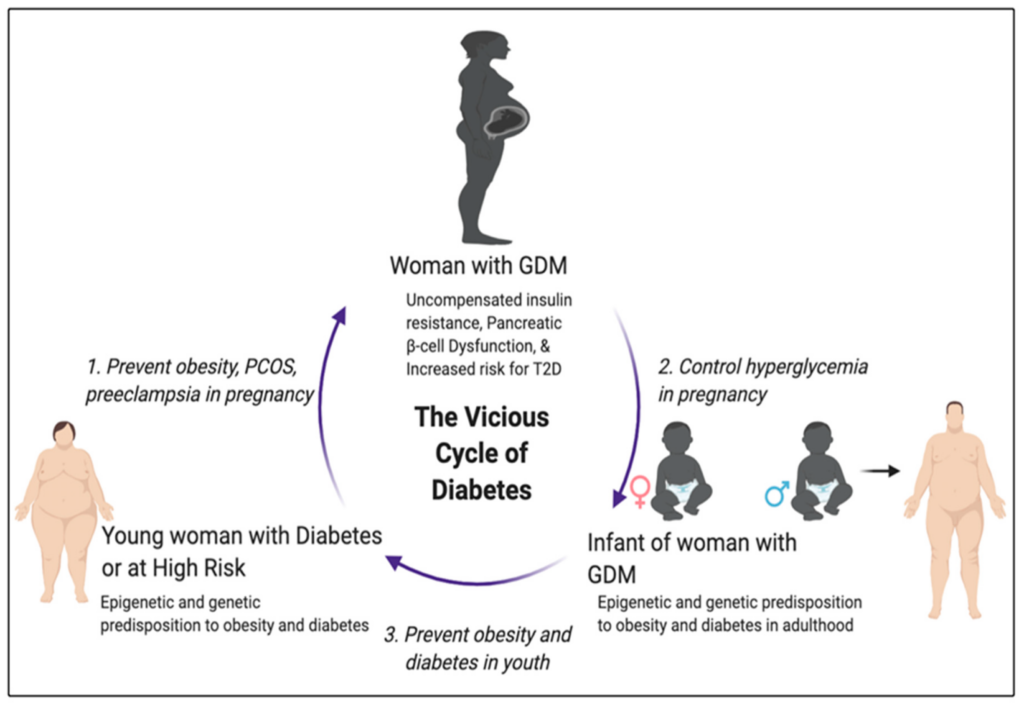
Risk of Developing Type 2 Diabetes
Women who have had gestational diabetes mellitus have an increased risk of developing type 2 diabetes later in life. Regular screenings and lifestyle modifications, such as healthy eating and regular exercise, can help reduce this risk.
Prevention and Lifestyle Changes
Lifestyle changes, including maintaining a healthy weight, engaging in regular physical activity, and making nutritious food choices, can help prevent the development of type 2 diabetes. Women with a history of diabetes during pregnancy should work closely with healthcare providers to implement these preventive measures.
Long-term Implications for the Baby
Babies born to mothers with diabetes during pregnancy may face long-term health implications. It is important to understand these potential risks and take appropriate measures to minimize them.
Risk of Developing Type 2 Diabetes
Children born to mothers with diabetes are at an increased risk of developing type 2 diabetes later in life. It is crucial to promote a healthy lifestyle for these children, including regular physical activity and a balanced diet, to reduce this risk.
Childhood Obesity
Children born to mothers with diabetes are more likely to develop childhood obesity. This can further increase the risk of numerous health problems, including diabetes and cardiovascular diseases. Implementing healthy habits early in life can help prevent obesity and its associated complications.
Metabolic Syndrome
Metabolic syndrome, a cluster of conditions that increase the risk of heart disease, stroke, and diabetes, is more common in individuals born to mothers with diabetes during pregnancy. Early screening and appropriate lifestyle interventions can help reduce the likelihood of developing metabolic syndrome.
Conclusion
Diabetes mellitus during pregnancy, whether gestational or pre-existing, requires careful management and monitoring to ensure the well-being of both the mother and the baby. Timely screening, appropriate medical and dietary management, and regular antenatal care are essential for optimal pregnancy outcomes. Long-term follow-up and preventive measures are also important to address any potential risks for the mother and the baby. By taking proactive measures and working closely with healthcare providers, women with diabetes can have successful pregnancies and minimize potential complications.