In today’s article, we’ll explore the intriguing connection between diabetes mellitus and obesity. Diabetes Mellitus, a lifelong chronic condition, affects millions worldwide, causing an imbalance in blood sugar levels. But what if I told you that there is a significant correlation between this condition and obesity? As we delve into this topic, we’ll uncover the intricate relationship between these two health concerns, shedding light on the impact they can have on our overall well-being. Get ready to discover the fascinating link between diabetes mellitus and obesity – it’s a conversation you won’t want to miss out on!
The Link Between Diabetes Mellitus and Obesity
Introduction to Diabetes Mellitus
Diabetes Mellitus, commonly referred to as diabetes, is a chronic metabolic disorder characterized by high blood sugar levels. It occurs when the body either doesn’t produce enough insulin or doesn’t effectively use the insulin it produces. Insulin is a hormone that regulates blood sugar levels and allows glucose to enter the body’s cells to be used as energy.
Definition
Diabetes Mellitus is classified into different types, including Type 1 diabetes, Type 2 diabetes, gestational diabetes, and other less common types. Type 1 diabetes occurs when the immune system mistakenly attacks and destroys the insulin-producing cells in the pancreas. Type 2 diabetes, on the other hand, is the most common form and develops when the body becomes resistant to insulin or doesn’t produce enough insulin to maintain normal blood sugar levels.
Types of Diabetes Mellitus
Type 1 diabetes typically manifests in childhood or adolescence, while Type 2 diabetes is more prevalent in adults, especially those who are overweight or obese. Gestational diabetes affects pregnant women and usually resolves after delivery. Other types of diabetes, such as monogenic diabetes and cystic fibrosis-related diabetes, are less common and have specific underlying causes.
Prevalence and Incidence
According to the International Diabetes Federation (IDF), approximately 463 million adults worldwide had diabetes in 2019, and this number is projected to rise to 700 million by 2045. Type 2 diabetes accounts for about 90% of all diabetes cases. The prevalence of diabetes is increasing globally due to factors such as population growth, urbanization, sedentary lifestyles, and unhealthy eating habits.
Introduction to Obesity
Obesity is a medical condition characterized by excessive body fat accumulation. It is commonly assessed using the body mass index (BMI), calculated by dividing a person’s weight in kilograms by the square of their height in meters. A BMI of 30 or higher is considered obese.
Definition
Obesity is primarily caused by an imbalance between calorie intake and energy expenditure. When the energy consumed from food exceeds the energy expended through physical activity and metabolic processes, the excess energy is stored as fat, leading to weight gain. It is essential to note that obesity is a complex condition influenced by genetic, environmental, and behavioral factors.
Causes
The causes of obesity are multifactorial. Genetic factors play a role, as certain gene variations can predispose individuals to weight gain and obesity. Environmental factors such as the availability of unhealthy food options, sedentary lifestyles, and cultural norms also contribute to the obesity epidemic. Additionally, psychological factors, socioeconomic status, and hormonal imbalances can influence weight gain and obesity.
Prevalence
Obesity has reached epidemic proportions globally, with the World Health Organization (WHO) estimating that over 1.9 billion adults were overweight in 2016, of whom more than 650 million were obese. The prevalence of obesity has more than doubled since 1980.
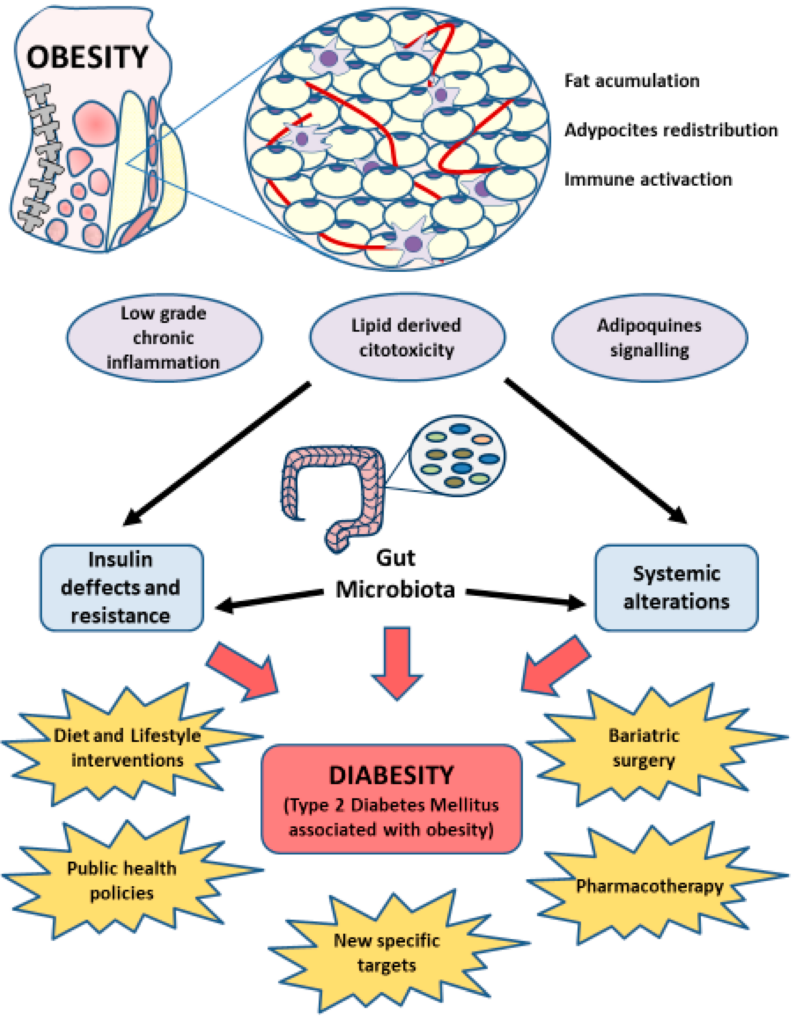
Connection between Obesity and Type 2 Diabetes
There is a strong correlation between obesity and the development of Type 2 diabetes. Obesity increases the risk of developing insulin resistance, a condition in which the body’s cells fail to respond properly to the effects of insulin. This leads to elevated blood glucose levels and, eventually, diabetes.
Increased Insulin Resistance
Adipose tissue, commonly known as body fat, produces substances called adipokines that can interfere with insulin signaling. In obesity, the increased secretion of adipokines promotes systemic inflammation and impairs insulin sensitivity in various tissues, including muscle, liver, and adipose tissue itself. The accumulation of fat in these tissues can disrupt the normal metabolic processes and contribute to insulin resistance.
Elevated Blood Glucose Levels
Insulin resistance in obesity results in an inadequate uptake of glucose by the body’s cells. As a result, blood glucose levels remain elevated, leading to a condition known as hyperglycemia. Over time, this chronic hyperglycemia can damage organs and tissues throughout the body, resulting in the complications associated with diabetes.
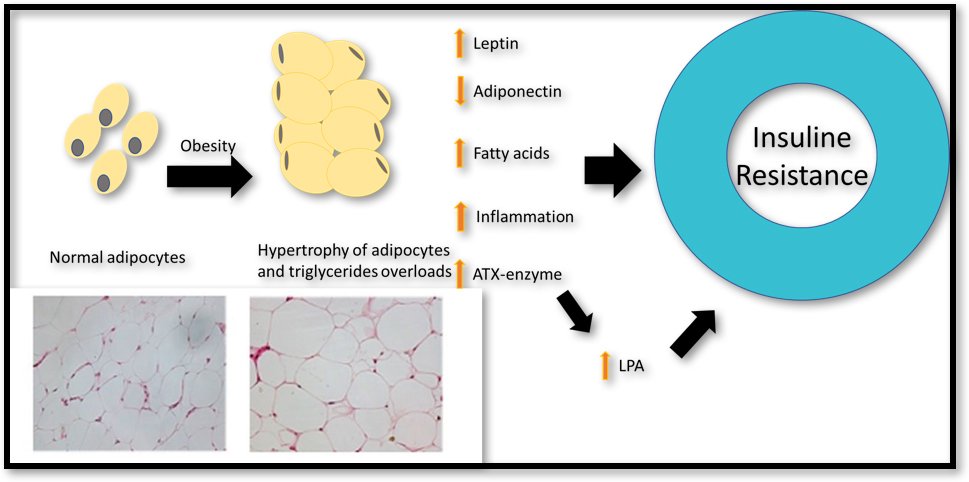
Role of Adipose Tissue
Adipose tissue is not merely a passive energy storage site but an active endocrine organ that secretes numerous hormones and signaling molecules. In obesity, increased adipose tissue mass releases excessive amounts of free fatty acids into the bloodstream. These free fatty acids can promote insulin resistance and impair the function of insulin-producing cells in the pancreas. Moreover, the adipose tissue can produce pro-inflammatory cytokines, which contribute to chronic low-grade inflammation, further exacerbating insulin resistance and diabetes risk.

Obesity as a Risk Factor for Diabetes Mellitus
Obesity is a significant risk factor for the development of Type 2 diabetes. Multiple studies have established a robust association between obesity, as measured by BMI, and the risk of developing diabetes.
Body Mass Index and Diabetes Risk
Research has consistently shown that higher BMI levels are associated with an increased risk of developing Type 2 diabetes. The risk of diabetes rises progressively with increasing BMI. Individuals with obesity, defined as having a BMI of 30 or higher, have a significantly higher risk of developing diabetes compared to those with a normal BMI.
Central Obesity and Diabetes Risk
Central obesity, characterized by excess fat accumulation around the waist and abdomen, has been linked to a higher risk of diabetes compared to generalized obesity. The distribution of body fat plays a crucial role in the development of insulin resistance and diabetes. Individuals with a higher waist circumference or waist-to-hip ratio are at a greater risk of developing diabetes, even if their overall BMI may be within the normal range.
Dose-response Relationship
The relationship between obesity and diabetes follows a dose-response pattern. As the severity and duration of obesity increase, the risk of developing diabetes also rises. Weight gain over time contributes to the development and progression of insulin resistance and diabetes. However, even modest weight loss can have significant benefits in reducing diabetes risk and improving glycemic control.
Mechanisms Linking Obesity and Diabetes Mellitus
Several mechanisms have been proposed to explain the link between obesity and the development of diabetes.
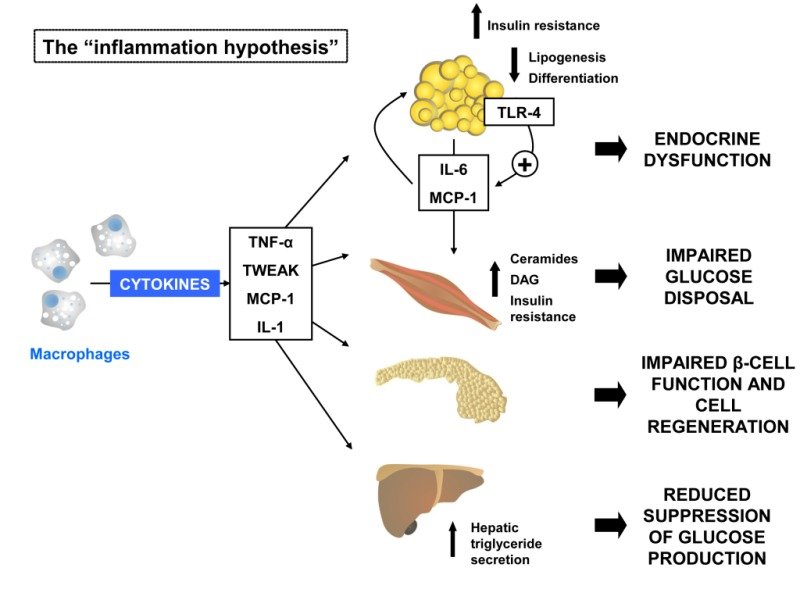
Chronic Inflammation
Obesity is characterized by a state of chronic low-grade inflammation. Adipose tissue releases pro-inflammatory cytokines and other inflammatory molecules that contribute to systemic inflammation. This chronic inflammation can impair insulin signaling and promote insulin resistance, increasing the risk of developing diabetes.
Adipokines and Insulin Resistance
Adipokines, hormones secreted by adipose tissue, can modulate insulin sensitivity. In obesity, the balance of adipokines shifts, leading to an increased production of pro-inflammatory adipokines such as tumor necrosis factor-alpha (TNF-alpha) and interleukin-6 (IL-6). These adipokines can disrupt insulin signaling pathways and impair glucose uptake, contributing to insulin resistance.
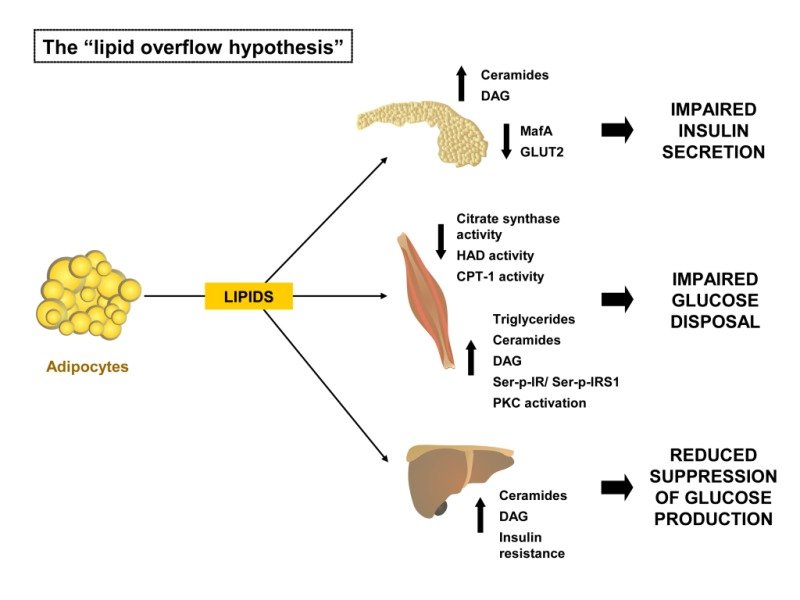
Dyslipidemia and Insulin Resistance
Obesity is often accompanied by dyslipidemia, an abnormal lipid profile characterized by elevated levels of triglycerides and LDL cholesterol, along with decreased levels of HDL cholesterol. Dyslipidemia can interfere with insulin signaling and contribute to insulin resistance, further increasing the risk of diabetes.
Impact of Weight Loss on Diabetes Management
Weight loss has been found to have numerous beneficial effects on the management of diabetes.
Weight Loss and Glycemic Control
Losing weight can significantly improve glycemic control in individuals with Type 2 diabetes. Weight loss reduces insulin resistance, allowing better glucose uptake by the cells and reducing the reliance on exogenous insulin or oral medications to control blood sugar levels. Studies have shown that modest weight loss of 5-10% of initial body weight can lead to clinically meaningful improvements in glycemic control.
Benefits on Insulin Sensitivity
Weight loss improves insulin sensitivity, enabling the body to effectively utilize insulin. With improved insulin sensitivity, the risk of complications associated with diabetes, such as heart disease and kidney damage, is also reduced. Weight loss achieved through lifestyle modifications, such as dietary changes and increased physical activity, has been shown to have lasting effects on insulin sensitivity.
Improvements in Cardiovascular Risk Factors
Obesity and diabetes are both major risk factors for cardiovascular disease. Weight loss can lead to improvements in various cardiovascular risk factors, including blood pressure, cholesterol levels, and markers of inflammation. These improvements can significantly reduce the risk of cardiovascular complications in individuals with diabetes.
Obesity and Gestational Diabetes Mellitus
Gestational diabetes mellitus (GDM) is a type of diabetes that is diagnosed during pregnancy. Obesity is a significant risk factor for the development of GDM.
Increased Risk during Pregnancy
Obesity increases the risk of developing GDM during pregnancy. The excess body fat and increased insulin resistance associated with obesity can interfere with glucose metabolism, leading to elevated blood sugar levels. Pregnant women who are obese are at a higher risk of developing GDM compared to those with a healthy weight.
Impact on Mother and Baby
GDM can have adverse effects on both the mother and the baby. Uncontrolled high blood sugar levels during pregnancy can increase the risk of complications such as preeclampsia, cesarean delivery, and gestational hypertension. The baby may be at risk of macrosomia (excessive birth weight), birth trauma, and an increased likelihood of developing obesity and Type 2 diabetes later in life.
Prevention and Management
Maintaining a healthy weight before and during pregnancy is crucial in reducing the risk of developing GDM. Lifestyle modifications, including healthy eating, regular physical activity, and weight management, should be encouraged as part of prenatal care. Close monitoring of blood sugar levels and appropriate medical management can help control GDM and minimize its associated complications.
Clinical Implications and Recommendations
The link between obesity and diabetes has significant clinical implications and warrants a comprehensive approach to prevention and management.
Screening and Diagnosis Strategies
Routine screening for diabetes and prediabetes should be implemented, especially in individuals with risk factors such as obesity. Assessing BMI, waist circumference, and other anthropometric measures can help identify individuals at high risk of developing diabetes. Early diagnosis enables timely intervention and lifestyle modifications to prevent or manage diabetes effectively.
Integrated Diabetes and Obesity Management
Given the strong association between diabetes and obesity, management strategies should target both conditions simultaneously. Lifestyle modifications, including a balanced diet, regular physical activity, and behavior change techniques, form the cornerstone of integrated diabetes and obesity management. Pharmacotherapy and bariatric surgery may be considered in select cases where lifestyle interventions alone are inadequate.
Lifestyle Modifications
Promoting healthy lifestyle habits is essential in preventing and managing both obesity and diabetes. Encouraging regular physical activity, adopting a balanced diet rich in fruits, vegetables, whole grains, and lean proteins, and promoting weight management can help individuals reduce their risk of developing diabetes. Lifestyle modifications should be tailored to the individual’s needs, preferences, and cultural context, ensuring long-term adherence and sustainable outcomes.
Conclusion
The link between diabetes mellitus and obesity is undeniable. Obesity increases the risk of developing Type 2 diabetes through various mechanisms, including insulin resistance and elevated blood glucose levels. Managing obesity is crucial in preventing the onset of diabetes and improving glycemic control in individuals already diagnosed with diabetes. Integrated approaches that address both conditions concurrently, along with comprehensive lifestyle modifications, are key to reducing the burden of diabetes and obesity on individuals and healthcare systems worldwide.