Imagine living in a world where memories become fragmented and reality becomes distorted. In this captivating article, we will explore the complexities of diagnosing and managing Dementia with Lewy Bodies, a progressive neurodegenerative disorder that affects millions of individuals worldwide. Delve into the intricacies of this condition as we navigate the challenges faced by both patients and their loved ones. Discover the latest advancements in medical treatments and caregiving techniques that strive to bring comfort and understanding to those affected by this debilitating disease.
Definition and Overview
What is Dementia with Lewy Bodies?
Dementia with Lewy Bodies (DLB) is a progressive neurodegenerative disorder that affects cognitive function, behavior, and movement. It is the third most common form of dementia, after Alzheimer’s disease and vascular dementia. DLB is characterized by the presence of abnormal protein deposits, called Lewy bodies, in the brain. These deposits disrupt the normal functioning of brain cells, leading to the symptoms associated with the disease.
Symptoms and Characteristics
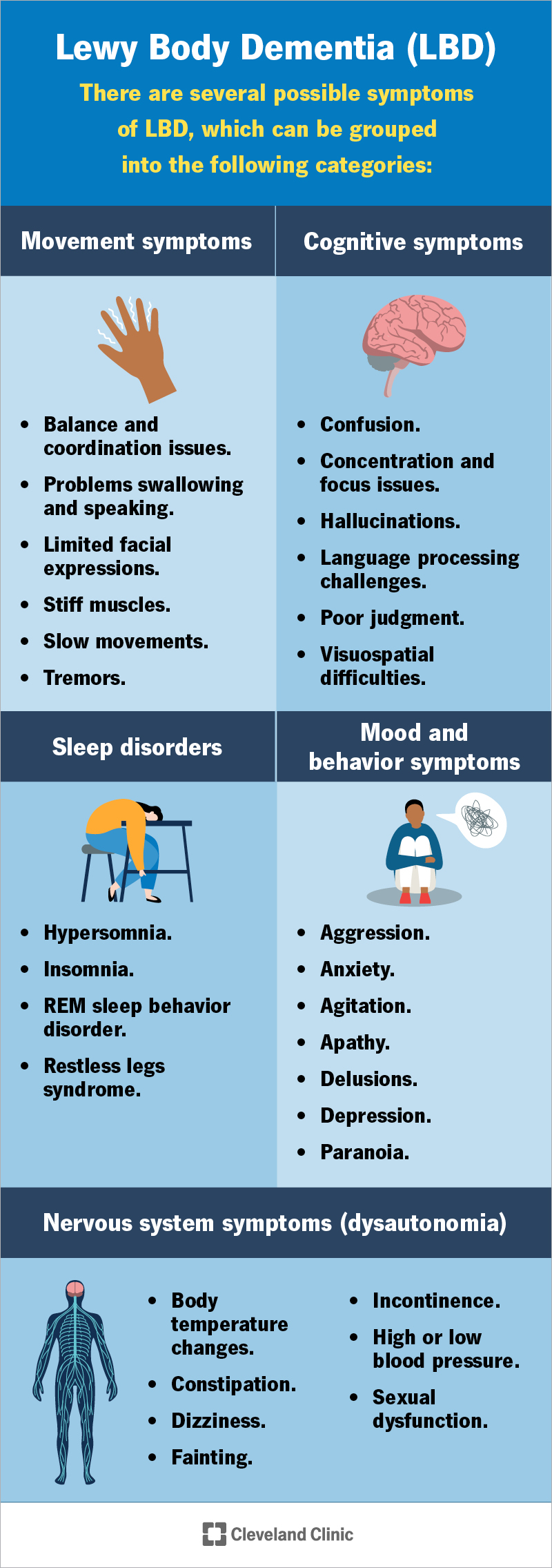
DLB is characterized by a range of symptoms that can vary in severity and presentation from person to person. The hallmark features of DLB include cognitive decline, visual hallucinations, and motor symptoms similar to those seen in Parkinson’s disease. Other common symptoms include fluctuations in attention and alertness, REM sleep behavior disorder, severe sensitivity to neuroleptic medications, and autonomic dysfunction. The combination of these symptoms can have a significant impact on a person’s ability to function independently and maintain a good quality of life.
Prevalence and Risk Factors
The exact prevalence of DLB in the general population is difficult to determine due to variations in diagnostic criteria and challenges in accurately identifying cases. However, it is estimated that DLB accounts for around 15% of all dementia cases. The risk of developing DLB increases with age, and it is more common in men than women. Additionally, there may be genetic factors that contribute to the development of DLB, although further research is needed to fully understand these associations.
Diagnosis
Clinical Evaluation
Diagnosing DLB requires a comprehensive clinical evaluation that takes into account the person’s medical history, symptoms, and physical examination. The evaluation typically involves a thorough assessment of cognitive function, including memory, language, and executive function. The presence of visual hallucinations, motor symptoms, and autonomic dysfunction is also important in the diagnostic process. In addition to cognitive and physical assessments, evaluating psychiatric and behavioral symptoms is crucial for accurate diagnosis.
Diagnostic Criteria
To facilitate consistent diagnosis, several sets of diagnostic criteria have been developed for DLB. The most widely used criteria are the “McKeith criteria,” which include core clinical features, suggestive clinical features, and supportive features. The core clinical features include fluctuating cognition with pronounced variations in attention and alertness, recurrent visual hallucinations, and spontaneous parkinsonism. Suggestive and supportive features help to further support the diagnosis and exclude other conditions with similar symptoms.
Distinguishing Dementia with Lewy Bodies from Other Disorders
Differentiating DLB from other dementias and movement disorders can be challenging due to overlapping symptoms. Distinguishing features of DLB include the early onset of cognitive decline, prominent visual hallucinations, rapid eye movement (REM) sleep behavior disorder, and marked fluctuations in cognition and alertness. Additionally, the presence of parkinsonism, such as bradykinesia, rigidity, and postural instability, is a distinguishing characteristic of DLB compared to other dementias. Neuroimaging and other diagnostic tests can also help in the differentiation process.
Neuroimaging and Laboratory Tests
Neuroimaging techniques, such as magnetic resonance imaging (MRI) and positron emission tomography (PET), can provide valuable information in the diagnosis of DLB. These tests can help identify structural and functional changes in the brain that are characteristic of DLB, such as the presence of Lewy bodies and reduced dopamine transporter activity. While neuroimaging is not required for the diagnosis of DLB, it can be useful in supporting the clinical evaluation. Laboratory tests, such as blood tests and cerebrospinal fluid analysis, may also be performed to rule out other potential causes of cognitive impairment and to support the diagnosis of DLB.

Medical Management
Multidisciplinary Approach
The management of DLB typically involves a multidisciplinary approach, with a team of healthcare professionals working together to address the various aspects of the disease. This may include neurologists, psychiatrists, geriatricians, nurses, occupational therapists, and social workers. Each member of the team plays a crucial role in evaluating and managing the symptoms of DLB and providing support and guidance to both the person with DLB and their caregivers.
Pharmacological Interventions
There are currently no medications specifically approved for the treatment of DLB. However, certain medications can be prescribed to manage the individual symptoms associated with DLB. Cholinesterase inhibitors, such as donepezil, rivastigmine, and galantamine, may be used to improve cognitive function and reduce behavioral symptoms. Parkinson’s medications, such as levodopa, can help alleviate motor symptoms. Antipsychotic medications should be used with caution in individuals with DLB due to their potential to worsen symptoms and increase the risk of adverse effects.
Non-Pharmacological Interventions
Non-pharmacological interventions play a crucial role in managing the symptoms and improving the quality of life of individuals with DLB. These interventions may include cognitive stimulation activities, such as puzzles and memory games, to help maintain cognitive function. Reminiscence therapy, which encourages the recall of past events and experiences, can enhance well-being and communication. Reality orientation techniques, such as using calendars and familiar objects, can help individuals with DLB stay oriented to their surroundings.
Symptom Management
Addressing the various symptoms associated with DLB is an important aspect of medical management. Visual hallucinations may be managed through environmental adaptations to reduce triggers, such as covering mirrors or using low-lighting. Sleep disturbances, including REM sleep behavior disorder, can be addressed through various approaches, including medication adjustments and environmental modifications. Comprehensive symptom management aims to improve the person’s overall well-being and minimize the impact of the symptoms on their daily life.
Monitoring and Adjustments
The management of DLB is an ongoing process that requires regular monitoring and adjustments to the treatment plan. Regular follow-up appointments with the healthcare team are essential to assess the individual’s response to medications, monitor for any side effects, and make necessary adjustments based on changes in symptoms. Open communication between the person with DLB, their caregivers, and the healthcare team is key to ensuring the management plan is tailored to meet the individual’s specific needs.
Cognitive and Behavioral Interventions
Cognitive Stimulation
Cognitive stimulation activities are designed to enhance cognitive function, maintain mental abilities, and improve overall well-being in individuals with DLB. These activities may include puzzles, memory games, arts and crafts, and group discussions. Cognitive stimulation can help maintain cognitive skills, improve attention and concentration, and provide a sense of accomplishment. These activities can be incorporated into daily routines and adjusted to the individual’s abilities and preferences.
Reminiscence Therapy
Reminiscence therapy involves engaging individuals with DLB in discussions and activities that encourage the recall of past events and experiences. This therapy can be facilitated through the use of photographs, personal mementos, music, and reminiscing about important life events. Reminiscence therapy can help improve mood, build rapport and connection, and provide a sense of identity and purpose for individuals with DLB.
Reality Orientation
Reality orientation techniques involve providing clear and consistent information about time, place, and person to help individuals with DLB maintain a sense of reality and orientation. This may include using calendars, clocks, labels, and familiar objects to reinforce the person’s awareness of their surroundings and the current time. Reality orientation techniques can be particularly helpful for individuals who experience confusion and disorientation as a result of their cognitive decline.
Validation Therapy
Validation therapy focuses on empathetically acknowledging and validating the emotions and experiences of individuals with DLB, even if they may not be based in reality. This approach aims to reduce distress and agitation and promote a sense of connection and understanding. Validation therapy involves active listening, empathy, and validation of the person’s feelings rather than attempting to correct or redirect their thoughts.
Behavioral Management Techniques
The management of behavioral symptoms associated with DLB involves using a range of behavioral management techniques. These techniques may include establishing a consistent routine, providing clear and simple instructions, redirecting attention to more appropriate activities, and creating a calm and structured environment. Behavior management techniques should be tailored to the individual’s specific needs and preferences, and may be adapted as the disease progresses.

Physical and Environmental Strategies
Promoting Safety and Independence
Promoting safety and independence is an important aspect of managing DLB. This may involve modifying the environment to reduce fall risks, such as removing trip hazards and installing grab bars and handrails. Providing adequate lighting and removing clutter can also help individuals with DLB navigate their surroundings safely. Assistive devices, such as walking aids and mobility aids, can support independence and reduce the risk of falls. Regular physical exercise and encouraging functional activities can help maintain physical strength and coordination.
Adaptive Equipment and Assistive Devices
Adaptive equipment and assistive devices can help individuals with DLB overcome physical limitations and maintain their independence. These devices may include mobility aids, such as canes or walkers, to support balance and prevent falls. Other assistive devices, such as grab bars, raised toilet seats, and shower chairs, can facilitate activities of daily living and improve safety. The selection and use of adaptive equipment and assistive devices should be guided by the individual’s specific needs and abilities.
Optimizing Physical Functioning
Optimizing physical functioning in individuals with DLB involves a combination of regular physical exercise, rehabilitation interventions, and environmental adaptations. Physical exercise can help improve muscle strength, balance, and coordination, reducing the risk of falls. Rehabilitation interventions, such as physical therapy and occupational therapy, can assess and address specific motor and functional limitations. Environmental adaptations, such as modifying furniture height or using adaptive utensils, can improve independence in daily activities.
Addressing Emotional and Psychosocial Needs
Psychosocial Support
Addressing the emotional and psychosocial needs of individuals with DLB is essential for their overall well-being. Psychosocial support may include individual counseling, psychotherapy, or group therapy sessions. These interventions can provide individuals with DLB with a safe space to express their emotions, process their experiences, and learn coping strategies. The support of a mental health professional can also be beneficial for caregivers, who may experience emotional distress and burnout.
Education and Counseling
Education and counseling are crucial components of the management of DLB, both for the individuals with the disease and their caregivers. Education about DLB, its symptoms, and progression can help individuals and their families understand and prepare for the challenges ahead. Counseling can provide guidance and support in managing the psychosocial impacts of the disease, such as grief, anxiety, and adjustment difficulties. Regular communication between healthcare professionals and individuals with DLB and their caregivers is key to ensure appropriate education and counseling are provided throughout the course of the disease.
Support Groups
Support groups offer individuals with DLB and their caregivers the opportunity to connect with others who are facing similar challenges. These groups provide a supportive environment where experiences, concerns, and strategies can be shared. Support groups can offer emotional support, practical advice, and a sense of community. They can also provide access to information about resources and services that may be beneficial in managing DLB.
End-of-Life Planning
End-of-life planning involves discussing and documenting an individual’s wishes and preferences for their care, should they reach a point where they are no longer able to make decisions for themselves. These discussions may include topics such as medical treatment preferences, resuscitation measures, and the appointment of a healthcare proxy or power of attorney. End-of-life planning should be done in consultation with healthcare professionals and legal advisors to ensure that all legal and ethical considerations are taken into account.

Caregiver Support and Training
Respite Care
Respite care provides temporary relief for caregivers by offering short-term assistance in the care of individuals with DLB. Respite care can take various forms, such as in-home respite, where a trained caregiver provides relief in the person’s own residence, or facility-based respite, where the person temporarily stays in a residential care facility. Respite care gives caregivers the opportunity to take a break, attend to their own needs, and reduce the risk of burnout.
Education and Training
Education and training programs can provide caregivers with the knowledge and skills needed to provide effective care for individuals with DLB. These programs may cover topics such as understanding DLB and its symptoms, communication techniques, behavior management strategies, and self-care for caregivers. Education and training can empower caregivers to better navigate the challenges of caring for someone with DLB, improve their ability to provide appropriate support, and enhance their overall well-being.
Supportive Services
Supportive services, such as home care assistance, meal delivery, and transportation services, can provide practical support to caregivers and individuals with DLB. These services aim to reduce the caregiving burden and help individuals with DLB maintain their independence and quality of life. Supportive services can be tailored to the specific needs of each individual and may be adjusted as the disease progresses.
Legal and Financial Planning
Advance Directives
Advance directives are legal documents that outline an individual’s preferences for medical treatment and end-of-life care. These documents provide instructions to healthcare professionals and family members regarding the person’s wishes should they become unable to communicate or make decisions for themselves. Advance directives may include a living will, which outlines specific medical treatments the person does or does not want, and a durable power of attorney for healthcare, which designates a trusted individual to make healthcare decisions on their behalf.
Long-Term Care Planning
Long-term care planning involves making arrangements for the future care needs of individuals with DLB. This may include planning for potential residential or nursing home care, identifying suitable care facilities, and exploring financing options. Long-term care planning should be done in consultation with healthcare professionals, social workers, and financial advisors to ensure that the individual’s care needs and preferences are met while also considering their financial resources and eligibility for assistance programs.
Power of Attorney
A power of attorney is a legal document that designates someone to make financial and legal decisions on behalf of an individual with DLB. This document can help ensure that the person’s financial and legal affairs are managed appropriately, even if they become unable to make decisions or communicate their preferences. The power of attorney should be created with the assistance of a qualified attorney to ensure that it meets legal requirements and addresses all necessary considerations.

Clinical Research and Future Directions
Current Studies on Dementia with Lewy Bodies
There is ongoing research aimed at further understanding and improving the diagnosis and management of DLB. Current studies may include investigations into the underlying causes of DLB, the development of more accurate diagnostic tests, and the exploration of potential disease-modifying treatments. Clinical trials may also be conducted to evaluate the safety and efficacy of new medications and interventions for DLB. Participating in research studies can provide individuals with DLB and their caregivers with opportunities to contribute to scientific knowledge and potentially receive novel treatments or interventions.
Emerging Treatment Approaches
Emerging treatment approaches for DLB may involve targeting specific pathological features of the disease, such as Lewy body accumulation or abnormal protein processing. These approaches may include the development of drugs that can dissolve or prevent the accumulation of Lewy bodies, immunotherapies that target abnormal protein deposits, or gene therapies aimed at modifying the underlying genetic factors associated with DLB. It is important to note that emerging treatments are still in the experimental stage and further research is needed before they can be widely implemented.
Genetic and Biomarker Research
Genetic and biomarker research aims to identify potential genetic risk factors and abnormal biological markers associated with DLB. Genetic studies can help identify specific genes that may increase the risk of developing DLB, allowing for early identification of at-risk individuals and potentially guiding future treatment strategies. Biomarkers, such as protein levels in blood or cerebrospinal fluid, can provide objective measures of disease progression and treatment response. These research efforts have the potential to enhance our understanding of DLB and contribute to the development of personalized treatment approaches.
Conclusion
Dementia with Lewy Bodies is a complex neurodegenerative disorder that affects cognition, behavior, and movement. Its symptoms can have a significant impact on the daily lives of individuals with DLB and their caregivers. However, with a comprehensive diagnosis and a multidisciplinary approach to management, it is possible to address the various aspects of the disease and improve the quality of life for those affected. Ongoing research and emerging treatment approaches offer hope for improved understanding, diagnosis, and treatment in the future. By continuing to advance our knowledge and support individuals with DLB and their caregivers, we can strive for better outcomes and a brighter future for those living with this challenging condition.