In this article, we will explore the various effective treatment options available for Lymphogranuloma Venereum (LGV). With the rising cases of this sexually transmitted infection, it is important to understand the different options that can help in managing and curing LGV. From antibiotics to lifestyle changes, we will discuss the methods that have proven to be successful in treating this condition. Whether you are seeking information for yourself or someone you know, this article aims to provide valuable insights on the treatment options for LGV in a friendly and informative manner.
Overview of Lymphogranuloma Venereum (LGV)
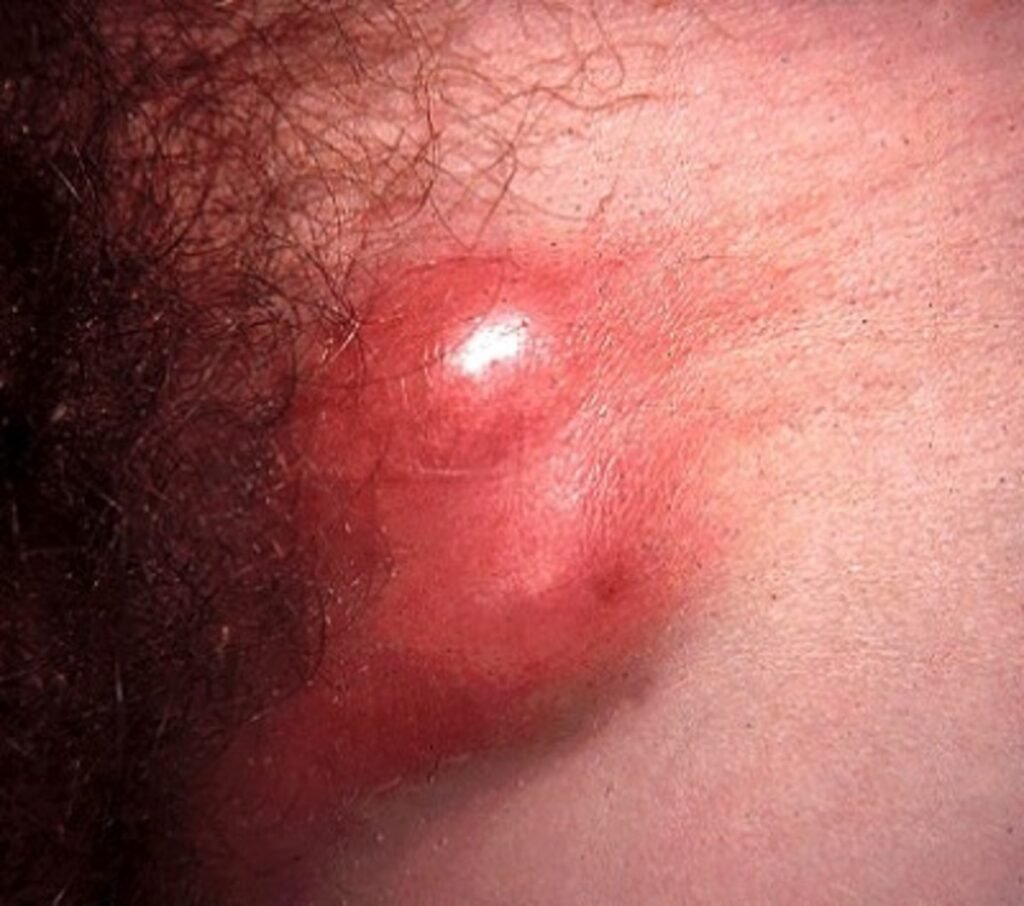
Lymphogranuloma Venereum (LGV) is a sexually transmitted infection caused by certain strains of the bacterium Chlamydia trachomatis. It primarily affects the lymph nodes and can lead to serious complications if not diagnosed and treated promptly. LGV is more prevalent in certain populations, such as men who have sex with men (MSM), and can occur concurrently with other sexually transmitted infections including HIV. This article will provide an overview of the diagnosis, treatment approaches, management of complications, prevention and control strategies, as well as specific considerations for LGV in special populations.
Diagnosis of LGV
Clinical Presentation
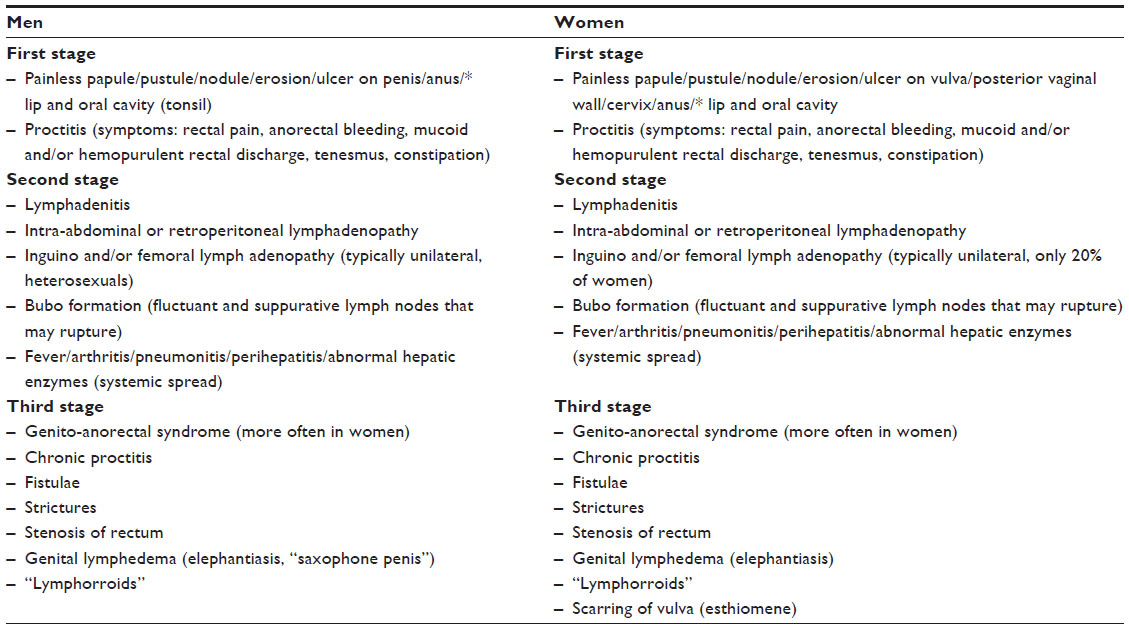
The clinical presentation of LGV can vary depending on the stage of the infection. In the early stages, individuals may experience painless genital ulcers, followed by swelling and inflammation of the inguinal lymph nodes. This can progress to the formation of abscesses and fistulas. In some cases, LGV can spread to other organs, causing systemic symptoms such as fever, fatigue, and weight loss. It is important to note that symptoms can be absent or mild in some individuals, leading to delayed diagnosis and potential complications.
Laboratory Tests
Laboratory tests are crucial for diagnosing LGV. Sampling of genital ulcers, rectal or cervical swabs, and lymph node biopsies can be used to detect the presence of Chlamydia trachomatis antigens or DNA using molecular testing methods like polymerase chain reaction (PCR). Serological tests can also be performed to detect LGV-specific antibodies, although they may not be available in all healthcare settings. A thorough history and physical examination, coupled with appropriate laboratory tests, are essential for accurate and timely diagnosis of LGV.

Treatment Approaches for LGV
Antibiotic Therapy
The primary treatment approach for LGV is antibiotic therapy. The most commonly prescribed antibiotics for LGV are doxycycline, erythromycin, or azithromycin. These antibiotics effectively target the Chlamydia trachomatis bacterium and help to resolve the infection. It is important to complete the full course of antibiotics as prescribed by your healthcare provider, even if your symptoms improve before completing the treatment.
Length of Treatment
The duration of antibiotic treatment for LGV depends on the severity of the infection and the presence of complications. Typically, a course of antibiotics lasting three weeks is recommended for the effective management of LGV. However, individual cases may require longer treatment durations based on medical assessment. It is crucial to adhere to the recommended treatment regimen and complete the full course of antibiotics to ensure the complete resolution of the infection.
Treatment for Asymptomatic LGV
In some cases, individuals may be asymptomatic carriers of LGV, meaning they do not exhibit any symptoms of the infection. However, it is important to note that asymptomatic carriers can still transmit the infection to others. If you have been diagnosed with LGV or have been in contact with an infected individual, your healthcare provider may recommend antibiotic treatment even in the absence of symptoms to prevent the spread of the infection.
Follow-Up Care
After completing the antibiotic treatment for LGV, it is important to attend follow-up appointments with your healthcare provider. These appointments allow for monitoring of treatment effectiveness, evaluation for any potential complications, and discussion of safe sexual practices to prevent future infections. Regular follow-up care is essential for the successful management of LGV and to ensure your overall health and well-being.
Specific Antibiotic Agents for LGV
Doxycycline
Doxycycline is one of the most commonly prescribed antibiotics for the treatment of LGV. It is typically taken orally, usually in a dosage of 100 mg twice daily for a duration of three weeks. Doxycycline is highly effective in treating LGV and its associated complications.
Erythromycin
Erythromycin is another antibiotic that can be used to treat LGV. It is usually taken orally, with a typical dosage of 500 mg four times daily for a similar duration of three weeks. Erythromycin is generally well-tolerated and effective in managing LGV.
Azithromycin
Azithromycin, a macrolide antibiotic, is also commonly used to treat LGV. It is typically taken orally as a single dose of 1 gram. However, in cases of severe or disseminated LGV, a longer course of treatment may be necessary. Azithromycin is generally well-tolerated and highly effective in resolving LGV infections.
Managing Complications of LGV
Abscess Formation
In some cases, LGV can lead to the formation of abscesses in the lymph nodes or surrounding tissues. These abscesses may require surgical drainage or aspiration to remove the pus and promote healing. Your healthcare provider will determine the appropriate management approach based on the severity and location of the abscess.
Obstructive Uropathy
LGV can also cause obstructive uropathy, a condition where the urinary flow is obstructed due to the inflammation and swelling of the lymph nodes near the urinary tract. Treatment aims to relieve the obstruction and ensure proper urinary flow. In some cases, surgical intervention may be necessary to address the underlying cause of the obstruction.
Fistula Formation
Chronic LGV infection can result in the formation of fistulas, abnormal connections between different organs or structures. Fistulas can occur in various areas of the body, including the rectum, genitals, or between the skin and lymph nodes. These complications may require surgical intervention or other specialized treatments to promote healing and prevent further complications.
Prevention and Control of LGV
Safe Sexual Practices
Practicing safe sexual practices is crucial in preventing the transmission of LGV and other sexually transmitted infections. This includes consistently and correctly using condoms, reducing the number of sexual partners, and getting tested regularly for sexually transmitted infections. Open and honest communication with sexual partners about potential risks and testing histories is also important.
Screening and Early Diagnosis
Regular screening for sexually transmitted infections, including LGV, is important for early diagnosis and treatment. Healthcare providers can perform genital, rectal, or cervical swabs to test for the presence of Chlamydia trachomatis and other sexually transmitted infections. Early diagnosis allows for prompt treatment and reduces the risk of complications and transmission to others.

LGV in Special Populations
LGV in Men who have Sex with Men (MSM)
LGV is more commonly diagnosed in men who have sex with men (MSM). The increased risk in this population may be due to specific sexual practices, including anal sex and oral-anal contact. It is crucial for MSM to be aware of the risks and symptoms of LGV, practice safe sexual behaviors, and undergo regular screening. In addition, healthcare providers should be well-informed about LGV in MSM and provide appropriate education, testing, and treatment options.
LGV in HIV-Positive Individuals
LGV can have unique considerations in individuals who are also living with HIV. The presence of HIV can affect the clinical course and management of LGV. It is important for healthcare providers to consider these factors and provide comprehensive care for individuals co-infected with LGV and HIV. Regular monitoring, early diagnosis, and appropriate treatment are fundamental in managing LGV in this population.
Public Health Considerations for LGV
Partner Notification and Contact Tracing
Partner notification and contact tracing are vital components in preventing the spread of LGV. Individuals diagnosed with LGV should inform their recent sexual partners about their diagnosis so that they can seek appropriate testing and treatment. Contact tracing involves identifying and notifying individuals who may have been exposed to LGV through sexual contact. This helps in early diagnosis, treatment, and prevention of further transmission.
Education and Awareness Campaigns
Public health organizations and healthcare providers play a key role in raising awareness about LGV and promoting prevention strategies. Education campaigns can include information about LGV, its symptoms, and the importance of early diagnosis and treatment. These campaigns can also emphasize the significance of safe sexual practices and regular testing for sexually transmitted infections.

Conclusion
Lymphogranuloma Venereum (LGV) is a sexually transmitted infection that can have significant consequences if not diagnosed and treated promptly. It is important to be aware of the clinical presentation, diagnostic methods, and treatment approaches for LGV. Adhering to recommended treatment regimens, practicing safe sexual behaviors, and seeking regular screening for sexually transmitted infections are crucial in preventing and managing LGV. By prioritizing prevention, early diagnosis, and comprehensive care, we can effectively address LGV and reduce its impact on individuals and communities.