You might not have heard of it before, but Lymphogranuloma Venereum, also known as LGV for short, is a sexually transmitted infection that is on the rise. This article will delve into the various ways in which LGV can be diagnosed, helping you understand what to look out for and ensuring that you can seek prompt medical attention if necessary. Whether you want to educate yourself on this lesser-known STI or simply want to be aware of the signs and symptoms, this article is here to help. So, let’s dive right in and learn more about diagnosing LGV.
Overview of Lymphogranuloma Venereum (LGV)
Definition
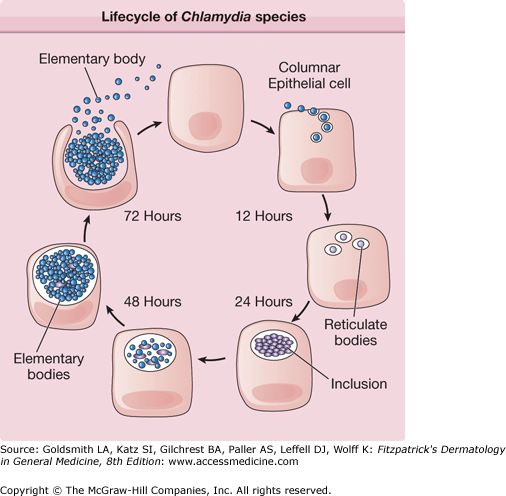
Lymphogranuloma Venereum (LGV) is a sexually transmitted infection caused by the bacteria Chlamydia trachomatis. It primarily affects the lymphatic system, leading to the formation of painful genital ulcers and lymph node swelling. LGV is categorized into three stages: the primary stage, secondary stage, and late stage.
Prevalence
LGV is more commonly found in tropical and subtropical regions, with higher rates of infection reported in certain populations such as men who have sex with men (MSM) and individuals involved in sex work. However, with increased global travel and migration, cases of LGV have been identified in other parts of the world as well.
Causative Agent
The causative agent of LGV is the bacteria Chlamydia trachomatis, specifically the L-serotypes L1, L2, and L3. These serotypes are more invasive compared to other chlamydial serotypes and have a unique capacity to infect and multiply within the lymphatic tissues.
Symptoms of LGV
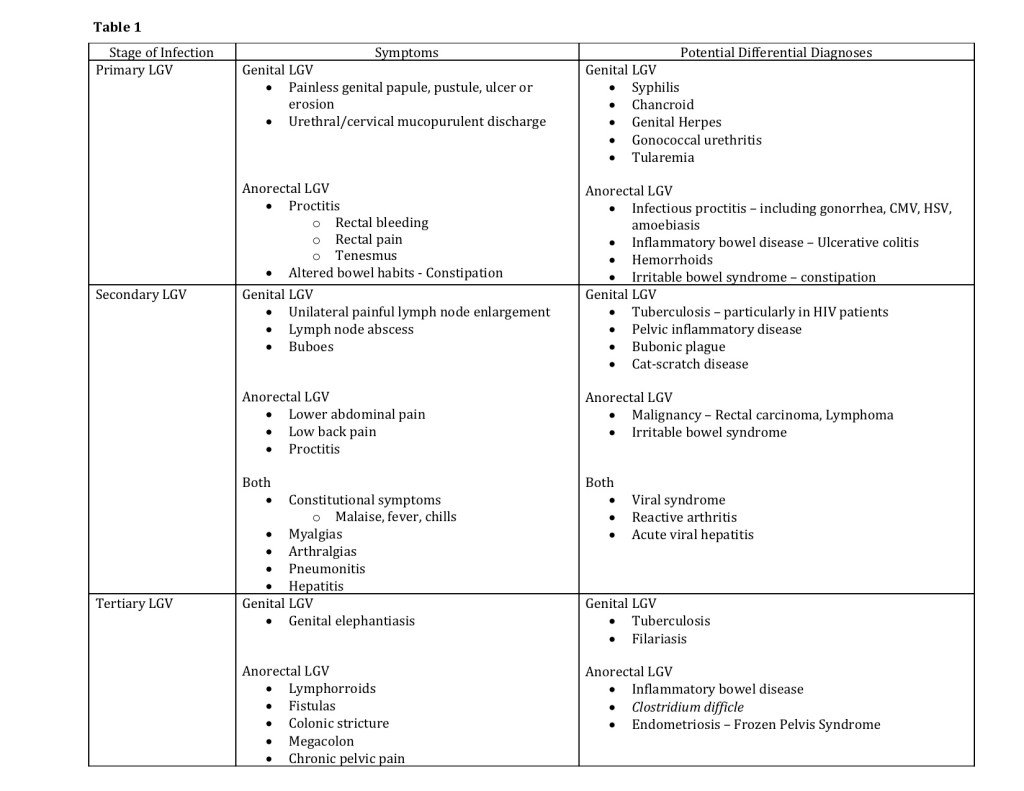
Primary Stage Symptoms
During the primary stage of LGV, small painless genital ulcers may develop at the site of infection, usually within one to three weeks after exposure. These ulcers may go unnoticed or heal spontaneously, often leading to delayed diagnosis and management.
Secondary Stage Symptoms
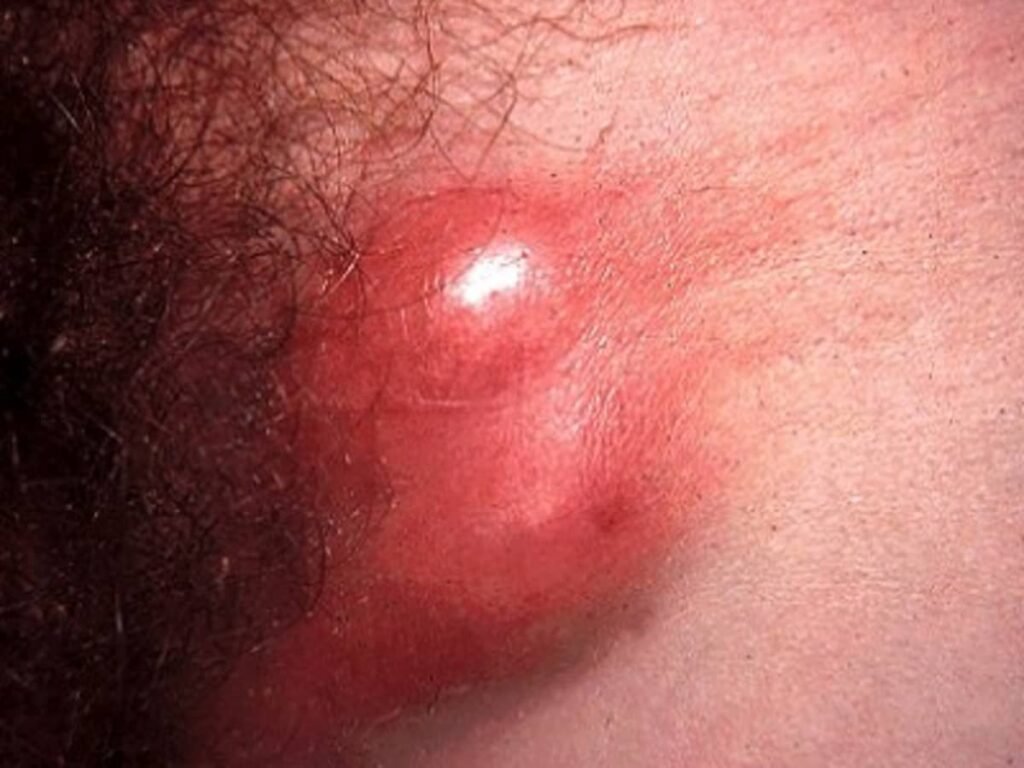
If left untreated, LGV progresses to the secondary stage characterized by swollen and painful lymph nodes in the groin area. The lymph nodes may become fluctuant and can eventually rupture, causing the formation of abscesses. Other symptoms that may be present during this stage include fever, malaise, and overall feeling of unwell.
Late Stage Symptoms
In the late stage of LGV, complications can arise due to the spread of the infection to other organs and tissues. These may include the development of rectal disease with symptoms such as rectal pain, bleeding, and discharge. In severe cases, the infection can cause urethral strictures, damage to the lymphatic system, and even genital elephantiasis.
Diagnosis of LGV
Physical Examination
A physical examination is an important component of diagnosing LGV. The healthcare provider will look for the presence of genital ulcers, swollen lymph nodes, and any signs of complications such as rectal disease or genital swelling. It is crucial for individuals to provide accurate information about their sexual history and any potential exposure to LGV.
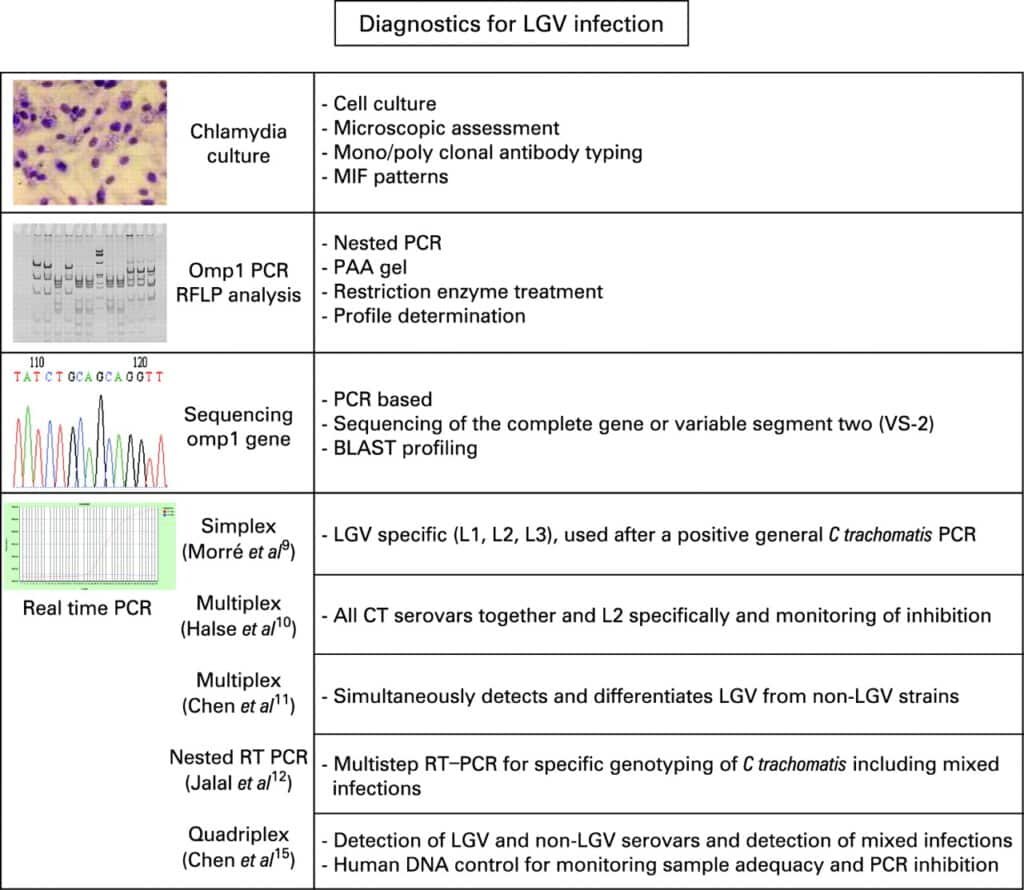
Laboratory Tests
Laboratory tests are essential in confirming the diagnosis of LGV. These may include the collection of specimens such as swabs or urine samples to test for the presence of Chlamydia trachomatis DNA. Additionally, serological tests can be performed to detect antibodies against the bacteria. It is important to note that LGV-specific tests are not widely available, and samples might need to be sent to specialized laboratories.
Diagnostic Criteria
The Centers for Disease Control and Prevention (CDC) have established diagnostic criteria for LGV. These criteria include clinical signs and symptoms, laboratory testing, and epidemiologic factors. Meeting these criteria helps ensure accurate diagnosis and appropriate management of LGV.
Differential Diagnosis
Chancroid
Chancroid is another sexually transmitted infection that can present with painful genital ulcers, similar to LGV. However, chancroid ulcers tend to be larger and more tender compared to LGV ulcers. The presence of buboes (swollen lymph nodes) distinguishes LGV from chancroid.
Syphilis
Syphilis is caused by the bacterium Treponema pallidum and can also present with genital ulcers. However, syphilis ulcers are typically painless and non-tender. A blood test is necessary for proper diagnosis and differentiation between LGV and syphilis.
Genital Herpes
Genital herpes is caused by the herpes simplex virus (HSV) and can cause painful blisters or ulcers on the genitals. Unlike LGV, genital herpes does not typically involve the lymph nodes. Laboratory testing, such as PCR or viral culture, can be used to differentiate between the two.
Granuloma Inguinale
Granuloma inguinale is caused by the bacteria Klebsiella granulomatis and can result in progressive genital ulcers. These ulcers tend to be painless, beefy red in appearance, and usually lack associated lymph node swelling. Laboratory tests are necessary to differentiate between LGV and granuloma inguinale.
Risk Factors
Unprotected Sex
Engaging in unprotected sexual intercourse, including vaginal, anal, or oral sex, increases the risk of acquiring LGV. Without the use of barrier methods, such as condoms, the chances of transmission are significantly higher.
Multiple Sexual Partners
Having multiple sexual partners also increases the risk of LGV. The more partners an individual has, the greater the chances of encountering someone who is infected with LGV or other sexually transmitted infections.
Men who have sex with men (MSM)
MSM are at higher risk of contracting LGV due to various factors, including increased prevalence within this population and the potential for rectal transmission during anal intercourse. It is essential for this group to practice safe sexual behaviors and undergo regular screening for sexually transmitted infections.
Sex Work
Engaging in sex work, either as a sex worker or a client, can increase the risk of LGV. This is due to the higher likelihood of having multiple sexual partners and engaging in unprotected sexual activities. Regular screenings and safe sex practices are crucial in reducing the transmission of LGV within this population.
Complications
Rectal Disease
LGV can cause inflammation and ulceration in the rectal area, leading to painful bowel movements, rectal bleeding, and discharge. Severe cases may result in fistulas (abnormal connections between organs) or strictures (narrowing of the rectal passage).
Urethral Strictures
Untreated or inadequately managed LGV can cause scarring and narrowing of the urethra, resulting in urethral strictures. This can lead to difficulties in urination, urinary tract infections, and potential kidney damage.
Lymphatic System Damage
LGV primarily affects the lymphatic system, leading to lymph node swelling and, in severe cases, damage to the lymphatic vessels. Lymphatic system damage can result in lymphedema, a condition characterized by chronic swelling of the affected body part.
Genital Elephantiasis
In rare cases, LGV can lead to the development of genital elephantiasis. This condition is characterized by massive genital swelling and can have significant physical and psychological impacts on the individual’s quality of life.

Treatment and Management of LGV
Drug Therapy
The primary treatment for LGV is antibiotic therapy with doxycycline or azithromycin. The duration of treatment may vary depending on the stage of infection and the individual’s response to therapy. If complications such as rectal disease or strictures are present, additional surgical interventions may be required.
Partner Notification and Treatment
Once diagnosed with LGV, it is important to notify sexual partners from the past 60 days so that they can seek appropriate testing and treatment. Partner notification helps prevent further transmission and ensures that all individuals involved receive appropriate care.
Follow-up and Monitoring
Regular follow-up visits with a healthcare provider are essential to monitor the efficacy of treatment and assess for any complications or recurrent infections. It also provides an opportunity for education on safe sexual practices and the prevention of future LGV infections.
Prevention of LGV
Safe Sexual Practices
Practicing safe sex is crucial in preventing LGV. This includes consistent and correct use of barrier methods, such as condoms, during sexual activities. Regular screening for sexually transmitted infections, including LGV, is recommended for individuals who engage in high-risk behaviors.
Use of Barrier Methods
Utilizing barrier methods, such as condoms, can significantly reduce the risk of LGV transmission. Condoms provide a physical barrier between partners, preventing direct contact and potential transmission of the bacteria.
Vaccination
Currently, there is no specific vaccine available for the prevention of LGV. However, routine immunization against other serotypes of Chlamydia trachomatis, such as those causing genital chlamydia, can help reduce the overall burden of chlamydial infections.
Public Health Implications
LGV Surveillance
Surveillance systems are crucial in collecting data on the prevalence, incidence, and trends of LGV. Accurate and timely reporting of cases allows public health authorities to monitor the spread of the infection, implement appropriate prevention strategies, and allocate resources effectively.
Education and Awareness Campaigns
Raising awareness about LGV and its risk factors is crucial in preventing new infections and reducing the burden of disease. Education campaigns targeting at-risk populations, healthcare providers, and the general public can provide information on safe sexual practices, the importance of regular screening, and the availability of treatment options.
Conclusion
Lymphogranuloma Venereum is a sexually transmitted infection caused by Chlamydia trachomatis. It can lead to various symptoms and complications if left untreated. Early diagnosis, prompt treatment, and following safe sexual practices are essential in preventing the spread of LGV. By implementing effective prevention strategies, raising awareness, and ensuring access to testing and treatment, the burden of LGV can be reduced, leading to better overall sexual health and well-being.