In this article, you will discover the impact of insulin resistance on heart health. Insulin resistance refers to a condition where the body’s cells become less responsive to the hormone insulin, leading to elevated blood sugar levels. While commonly associated with diabetes, insulin resistance can also have significant repercussions on heart health. By understanding how insulin resistance affects your heart, you can take proactive steps to protect your cardiovascular well-being.
The Basics of Insulin Resistance
What is Insulin Resistance?
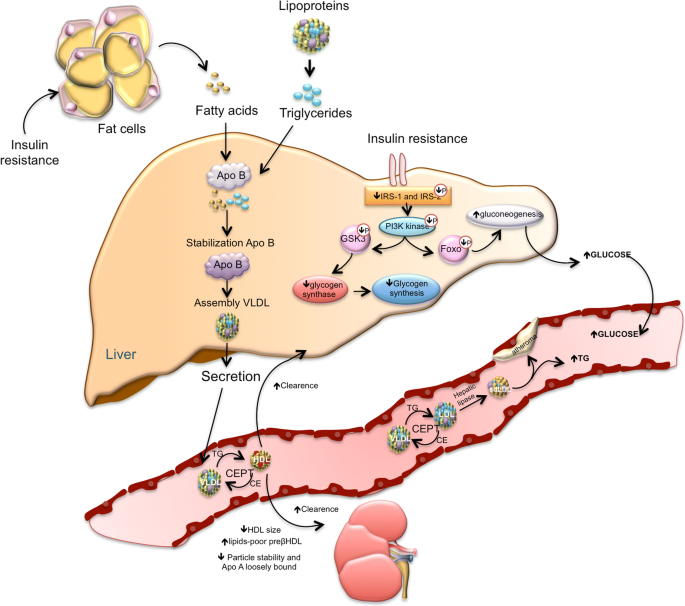
Insulin resistance is a condition in which your body’s cells become less responsive to the effects of insulin, a hormone produced by the pancreas. Normally, insulin helps regulate the level of glucose (sugar) in your blood by allowing it to enter your cells and be used for energy. However, when you have insulin resistance, your cells are unable to effectively respond to insulin, resulting in elevated levels of glucose in your bloodstream. This condition can have various impacts on your health, including your heart health.
Causes of Insulin Resistance
Insulin resistance can be caused by a combination of genetic and lifestyle factors. Certain genetic variations can predispose individuals to develop insulin resistance. However, lifestyle choices, such as a sedentary lifestyle, poor diet, and excess body weight, have a significant influence on the development of insulin resistance. Consuming a high-calorie diet, especially one that is rich in refined carbohydrates and added sugars, can contribute to insulin resistance over time.
How Insulin Resistance Develops
Insulin resistance often develops gradually, and several key mechanisms are involved. Overconsumption of refined carbohydrates and added sugars can lead to elevated blood sugar levels. As a result, the pancreas produces more insulin to help regulate blood sugar. Over time, the cells may become less responsive to higher insulin levels, leading to insulin resistance. Additionally, increased levels of free fatty acids in the bloodstream, often seen in obesity, can interfere with insulin signaling and contribute to the development of insulin resistance.
Impact of Insulin Resistance on Heart Health
Increased Risk of Cardiovascular Disease
Insulin resistance is closely linked to an increased risk of cardiovascular disease. When insulin resistance occurs, the body compensates by producing more insulin to keep blood sugar levels in check. The excess insulin can lead to the buildup of plaque in the arteries, a condition known as atherosclerosis. This plaque buildup can narrow the arteries and restrict blood flow to the heart, increasing the risk of heart attacks and other cardiovascular events.
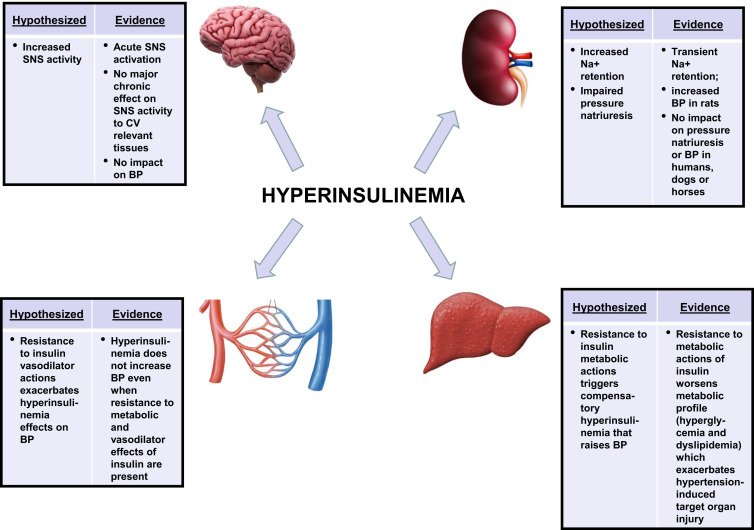
Effects on Blood Pressure
Insulin resistance also has an impact on blood pressure regulation. The excessive levels of insulin present in individuals with insulin resistance can affect the lining of blood vessels and cause them to constrict. This constriction raises blood pressure and puts additional strain on the heart. Over time, this can contribute to the development of hypertension, a major risk factor for heart disease and stroke.
Impact on Cholesterol Levels
Insulin resistance can negatively affect cholesterol levels in the body. It can lead to higher levels of low-density lipoprotein (LDL) cholesterol, commonly known as “bad” cholesterol. Elevated levels of LDL cholesterol increase the risk of plaque formation in the arteries. Additionally, insulin resistance can reduce levels of high-density lipoprotein (HDL) cholesterol, which is known as “good” cholesterol. HDL cholesterol helps remove excess cholesterol from the arteries, so lower levels can further contribute to cardiovascular risks.
Insulin Resistance and Inflammation
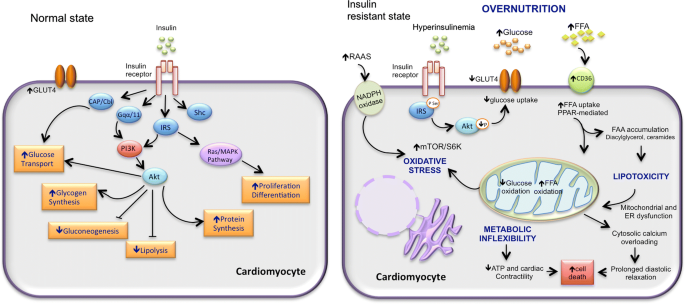
Role of Inflammation in Insulin Resistance
Inflammation plays a significant role in the development of insulin resistance. When there is chronic inflammation in the body, it can impair insulin signaling and contribute to insulin resistance. Inflammation can occur due to various factors, including excess body fat, poor dietary choices, and sedentary behavior. The inflammation disrupts the normal functioning of insulin, making it more challenging for insulin to adequately regulate blood sugar levels.
Inflammatory Processes and Heart Health
The inflammation associated with insulin resistance not only affects insulin signaling but also directly impacts heart health. Chronic inflammation can lead to damage to the inner lining of blood vessels, promoting the formation of plaque. Additionally, inflammation can trigger the release of substances that contribute to the clotting of blood, increasing the risk of heart attacks and strokes. Addressing inflammation through lifestyle modifications and potentially anti-inflammatory medications can play a crucial role in managing insulin resistance and reducing cardiovascular risks.
Insulin Resistance and Blood Sugar Control
Link between Insulin Resistance and Diabetes
Insulin resistance is closely linked to the development of type 2 diabetes. When insulin resistance occurs, the pancreas tries to compensate by producing even more insulin, leading to high levels of both insulin and glucose in the blood. Over time, the pancreas may become unable to keep up with the demand, resulting in high blood sugar levels and the development of diabetes. Proper management of insulin resistance is crucial in preventing the progression to diabetes and minimizing the associated cardiovascular risks.
Glycemic Control and Heart Health
Achieving and maintaining optimal blood sugar control is essential for preserving heart health in individuals with insulin resistance. High levels of glucose in the bloodstream can contribute to inflammation and the formation of plaque in the arteries. By effectively managing blood sugar levels through appropriate lifestyle interventions, medication, and monitoring, individuals with insulin resistance can help reduce the risk of developing cardiovascular complications.

Insulin Resistance and Obesity
Connection between Insulin Resistance and Obesity
Insulin resistance and obesity often go hand in hand. Excess body weight, particularly abdominal obesity, is strongly associated with insulin resistance. The presence of excess fat, especially in the abdominal area, can promote inflammation and release substances that interfere with insulin signaling. Additionally, obesity can lead to metabolic dysfunction, further exacerbating insulin resistance. Addressing obesity through lifestyle changes, including diet modifications and regular physical activity, is crucial for managing insulin resistance and improving heart health.
Obesity and Cardiovascular Risks
Obesity significantly increases the risk of various cardiovascular conditions, and insulin resistance plays a key role in that association. The combination of excess body weight and insulin resistance can lead to an unfavorable lipid profile, elevated blood pressure, and increased inflammation, all of which increase the risk of heart disease and stroke. Losing weight through a combination of healthy eating and regular exercise can help improve insulin sensitivity, reduce cardiovascular risks, and improve overall heart health.
Insulin Resistance and Insulin Sensitizers
Role of Insulin Sensitizers in Managing Insulin Resistance
Insulin sensitizers are medications that help improve the body’s response to insulin, making it easier for cells to uptake glucose from the bloodstream. These medications work by various mechanisms, such as enhancing insulin signaling or reducing insulin resistance at the cellular level. Insulin sensitizers can be an effective treatment option for individuals with insulin resistance, especially those who have not achieved adequate blood sugar control through lifestyle interventions alone.
Effects of Insulin Sensitizers on Heart Health
In addition to improving blood sugar control, insulin sensitizers can have positive effects on heart health. Some insulin sensitizers, such as metformin, have been shown to have cardiovascular benefits, including reducing the risk of heart attack and improving lipid profiles. The use of insulin sensitizers in combination with lifestyle modifications can help manage insulin resistance, improve glycemic control, and reduce cardiovascular risks.
Diet and Lifestyle Interventions for Insulin Resistance
Importance of Healthful Diet
Adopting a healthful diet is a cornerstone of managing insulin resistance and promoting heart health. A diet rich in whole, unprocessed foods, including fruits, vegetables, whole grains, lean proteins, and healthy fats, can help improve insulin sensitivity and maintain stable blood sugar levels. Avoiding sugary beverages, refined carbohydrates, and excessive calorie intake is crucial for managing insulin resistance and reducing the risk of cardiovascular complications.
Physical Activity and Regular Exercise
Regular physical activity is essential for improving insulin sensitivity and overall cardiovascular health. Engaging in aerobic exercise, such as brisk walking, cycling, or swimming, can help lower blood sugar levels and reduce insulin resistance. Strength training exercises can also be beneficial in improving body composition and increasing muscle mass, further enhancing insulin sensitivity. Aim for at least 150 minutes of moderate-intensity exercise or 75 minutes of vigorous-intensity exercise per week, along with regular resistance training.
Other Lifestyle Modifications
In addition to diet and exercise, other lifestyle modifications can contribute to managing insulin resistance and improving heart health. Getting an adequate amount of sleep is crucial, as sleep deprivation has been associated with insulin resistance and increased cardiovascular risks. Stress management techniques, such as mindfulness meditation or deep breathing exercises, can help reduce stress levels, which can also impact insulin sensitivity. Avoiding smoking and limiting alcohol consumption are further steps to protect heart health and manage insulin resistance.
Insulin Resistance and Medications
Insulin Therapy
In some cases, individuals with insulin resistance may require insulin therapy to manage their blood sugar levels effectively. Insulin therapy involves the use of insulin injections or an insulin pump to help regulate blood sugar and prevent complications associated with elevated glucose levels. Insulin therapy is usually reserved for individuals with severe insulin resistance or those with type 2 diabetes who are unable to achieve adequate blood sugar control through lifestyle modifications and oral medications alone.
Oral Medications
Several oral medications are available for the management of insulin resistance and blood sugar control. These medications work by various mechanisms, such as reducing glucose production by the liver, enhancing insulin secretion, or improving insulin sensitivity. Some commonly prescribed medications include metformin, sulfonylureas, thiazolidinediones, and GLP-1 receptor agonists. The choice of medication depends on individual factors, such as overall health, medical history, and potential side effects.
Potential Side Effects
Like any medication, oral medications and insulin therapy may have potential side effects. Common side effects of oral medications include gastrointestinal disturbances, weight gain, and low blood sugar (hypoglycemia). Insulin therapy can also lead to hypoglycemia if dosages are not appropriately adjusted. It is important to discuss potential side effects with your healthcare provider and to carefully monitor blood sugar levels when initiating new medications or insulin therapy.

Prevention and Management of Insulin Resistance
Lifestyle Changes for Prevention
Prevention of insulin resistance involves adopting a healthy lifestyle from an early age. Maintaining a balanced diet, engaging in regular physical activity, and maintaining a healthy body weight are the key components of preventing insulin resistance. Avoiding excessive intake of sugary foods and beverages and opting for whole, nutrient-dense foods can help reduce the risk of developing insulin resistance and its associated cardiovascular complications.
Screening and Early Detection
Early detection of insulin resistance is essential for effective management and prevention of further complications. Routine blood tests, such as fasting glucose and hemoglobin A1c levels, can help identify early signs of insulin resistance. Additionally, healthcare providers may assess additional risk factors, such as family history, waist circumference, and blood pressure, to determine an individual’s risk and develop an appropriate management plan.
Integrated Approach to Treatment
An integrated approach to the treatment of insulin resistance involves addressing multiple aspects of lifestyle and medication management. Lifestyle modifications, including dietary changes, regular exercise, adequate sleep, and stress management, should be the foundation of treatment. Depending on individual needs, healthcare providers may also recommend medications, such as insulin sensitizers or oral antidiabetic medications, to improve insulin sensitivity and blood sugar control. Regular monitoring of blood sugar levels and cardiovascular risk factors is essential to ensure effective management and prevent complications.
In conclusion, insulin resistance has significant implications for heart health. It increases the risk of cardiovascular disease, affects blood pressure and cholesterol levels, and promotes inflammation. However, with the right interventions, such as lifestyle modifications, medications, and early detection, insulin resistance can be effectively managed, reducing the risk of cardiovascular complications. By adopting a holistic approach that prioritizes healthy habits and regular medical monitoring, individuals can take control of their insulin resistance and protect their heart health.