Hey there! Have you ever heard of insulin resistance? It might not be something that’s talked about often, but it’s actually a silent threat to your health. Insulin resistance is a condition where your body becomes less responsive to the hormone insulin, which is responsible for regulating your blood sugar levels. This can lead to a whole host of health problems, including type 2 diabetes and cardiovascular diseases. So, in this article, we’re going to dive into the world of insulin resistance and explore why it’s something you should definitely be aware of. Trust me, it’s worth knowing about!

What is Insulin Resistance?
Definition
Insulin resistance is a condition in which the body’s cells become less responsive to the hormone insulin. Insulin is produced by the pancreas and allows glucose (sugar) from the bloodstream to enter the cells, where it is used for energy. When there is insulin resistance, the cells do not respond properly to insulin, resulting in elevated blood sugar levels. This can eventually lead to the development of type 2 diabetes if left untreated.
How does it occur?
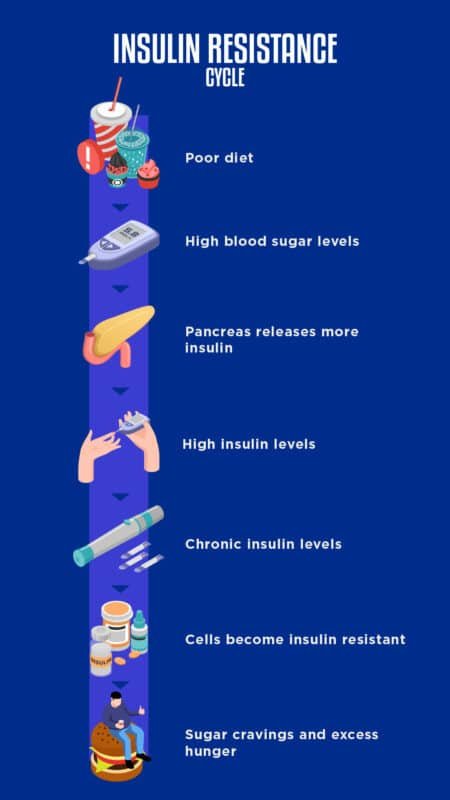
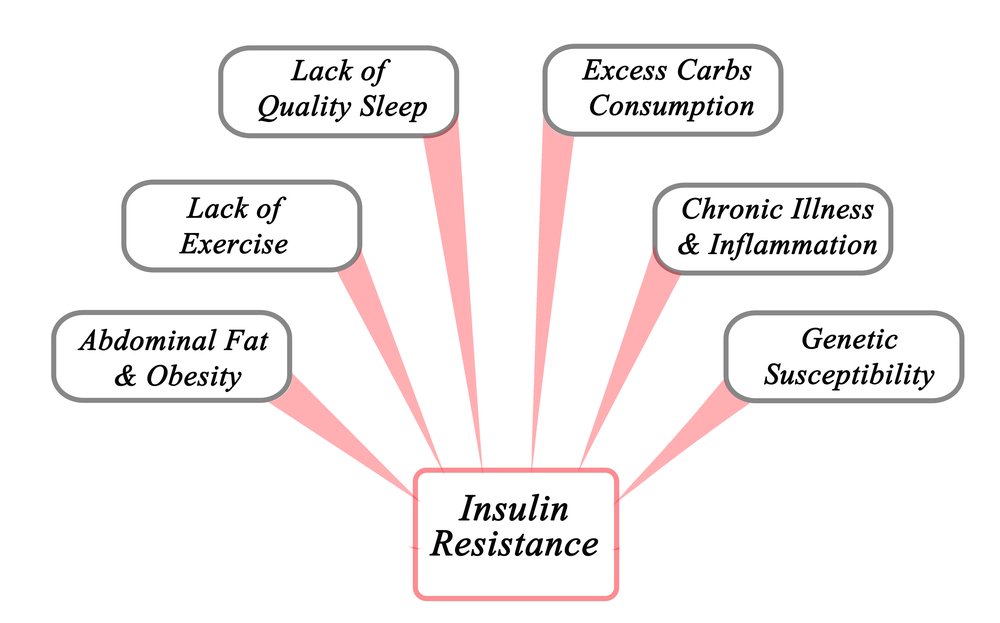
Insulin resistance occurs when the body is consistently exposed to high levels of insulin. This is often caused by a combination of genetic factors, poor diet, physical inactivity, and excess body weight. When the body is constantly exposed to high levels of insulin, the cells gradually become desensitized to its effects, leading to insulin resistance.
Risk factors
Certain factors increase the risk of developing insulin resistance. These include obesity, particularly excess fat around the abdomen, a sedentary lifestyle, a diet high in processed foods and sugar, high blood pressure, a family history of diabetes, and certain medical conditions such as polycystic ovary syndrome (PCOS). Age, ethnicity, and hormonal changes in women, such as during pregnancy or menopause, can also contribute to the risk of developing insulin resistance.
Effects of Insulin Resistance
Weight gain
Insulin resistance can contribute to weight gain and make it difficult to lose weight. When cells become resistant to insulin, glucose is not efficiently transported into the cells for energy. Instead, the body releases more insulin to compensate, which can promote the storage of excess glucose as fat. This can lead to weight gain, particularly around the abdomen, and make it challenging to shed those extra pounds.
Type 2 Diabetes
Insulin resistance is a major precursor to the development of type 2 diabetes. When the body cannot properly utilize insulin, blood sugar levels remain elevated. Over time, the pancreas may struggle to produce enough insulin to compensate, leading to further increases in blood sugar levels. If left untreated, this can result in the onset of type 2 diabetes, a chronic condition characterized by high blood sugar levels.
Cardiovascular disease
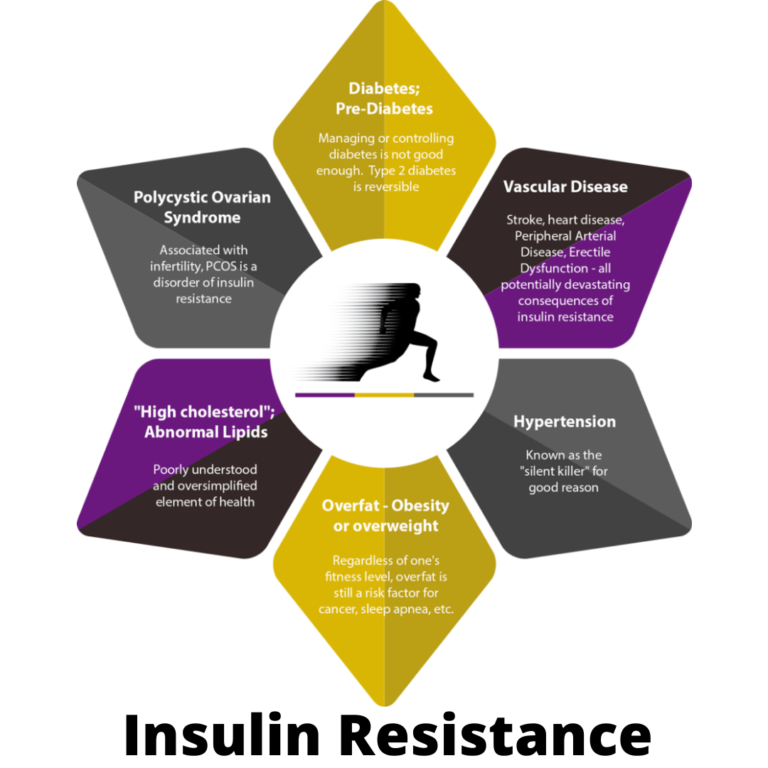
Insulin resistance is closely linked to an increased risk of cardiovascular disease. Elevated blood sugar levels, along with other metabolic abnormalities associated with insulin resistance, can contribute to the development of conditions such as hypertension (high blood pressure), dyslipidemia (abnormal cholesterol levels), and atherosclerosis (hardening of the arteries). These factors collectively increase the risk of heart disease, heart attacks, and strokes.
Polycystic ovary syndrome (PCOS)
Insulin resistance is commonly seen in women with polycystic ovary syndrome (PCOS). PCOS is a hormonal disorder characterized by enlarged ovaries with cysts and imbalances in levels of reproductive hormones. Insulin resistance plays a key role in the development and progression of PCOS, and the condition is often associated with obesity and difficulties in managing weight. PCOS can lead to irregular periods, fertility problems, and an increased risk of other health issues such as diabetes and cardiovascular disease.
Non-alcoholic fatty liver disease (NAFLD)
Insulin resistance is a significant factor in the development of non-alcoholic fatty liver disease (NAFLD). NAFLD is characterized by an accumulation of fat in the liver, which can progress to inflammation and liver damage. Insulin resistance disrupts the normal metabolism of fats in the liver, leading to the build-up of fat deposits. NAFLD is commonly associated with obesity, type 2 diabetes, and metabolic syndrome.
Cognitive decline
Insulin resistance has also been linked to cognitive decline and an increased risk of developing dementia, including Alzheimer’s disease. Research suggests that impaired insulin signaling in the brain can contribute to the accumulation of harmful proteins and the formation of plaques associated with Alzheimer’s disease. Maintaining insulin sensitivity through a healthy lifestyle may help reduce the risk of cognitive decline.
Cancer risk
Insulin resistance has been associated with an increased risk of certain types of cancer. Elevated insulin levels can stimulate cell growth and division, which can increase the risk of abnormal cell growth and tumor formation. Some studies have found links between insulin resistance and cancers such as breast, colorectal, and pancreatic cancer. However, more research is needed to fully understand the mechanisms underlying this relationship.
Diagnosing Insulin Resistance
Blood tests
Blood tests are commonly used to diagnose insulin resistance. A fasting blood glucose test measures the amount of glucose in the bloodstream after a period of fasting. If the blood glucose level is consistently above normal, it may indicate insulin resistance. Additionally, a fasting insulin test measures the level of insulin in the blood. High levels of insulin, along with high blood glucose, can suggest insulin resistance.
Glucose tolerance test
A glucose tolerance test (GTT) is another diagnostic tool for insulin resistance. It involves drinking a glucose solution, and blood samples are taken at regular intervals to measure how the body metabolizes the glucose. This test helps determine how effectively the body responds to glucose and can identify insulin resistance.
HbA1c test
The HbA1c test measures the average blood sugar levels over the past two to three months. Higher levels of HbA1c indicate poor blood sugar control, which may be a sign of insulin resistance. While the HbA1c test is primarily used to diagnose and monitor diabetes, it can also provide clues about insulin resistance.
Preventing Insulin Resistance
Maintaining a healthy weight
Maintaining a healthy weight is crucial in preventing insulin resistance. Excess body fat, particularly around the abdomen, increases the risk of insulin resistance. Adopting a balanced, portion-controlled diet and engaging in regular physical activity can help achieve and maintain a healthy weight, reducing the risk of insulin resistance.
Regular exercise
Regular exercise plays a significant role in preventing insulin resistance. Physical activity helps improve insulin sensitivity, allowing the body’s cells to respond more effectively to insulin. Aim for at least 150 minutes of moderate-intensity aerobic exercise per week, along with strength training exercises two or more days a week, to reduce the risk of insulin resistance.
Balanced diet
A balanced diet rich in whole foods, including fruits, vegetables, whole grains, lean proteins, and healthy fats, can help prevent insulin resistance. Limiting the intake of processed foods, sugary beverages, and foods high in saturated and trans fats can reduce the risk of insulin resistance. Focus on creating balanced meals that provide a variety of nutrients and promote stable blood sugar levels.
Managing stress levels
Chronic stress can contribute to insulin resistance. Finding healthy ways to manage stress, such as practicing relaxation techniques, engaging in hobbies, or seeking support from friends and family, can help prevent or mitigate the effects of stress on insulin resistance. Prioritizing self-care and taking time for activities that promote relaxation is essential for overall health and well-being.
Avoiding excessive alcohol consumption
Excessive alcohol consumption can disrupt normal insulin function and promote insulin resistance. It is important to moderate alcohol intake and avoid excessive or binge drinking. For women, moderate drinking is generally defined as up to one drink per day, while for men, it is up to two drinks per day.
Managing Insulin Resistance
Lifestyle changes
Making lifestyle changes is crucial in managing insulin resistance. Adopting a healthy eating plan, engaging in regular physical activity, managing stress, and maintaining a healthy weight are all key components of managing insulin resistance. These changes can improve insulin sensitivity, lower blood sugar levels, and reduce the risk of complications associated with insulin resistance.
Medications
In some cases, medication may be prescribed to help manage insulin resistance. Metformin is a common medication used to improve insulin sensitivity and lower blood sugar levels. Other medications, such as thiazolidinediones and GLP-1 receptor agonists, may also be prescribed to help manage insulin resistance and diabetes. It is important to work closely with a healthcare provider to determine the most appropriate medication and dosage for individual needs.
Monitoring blood sugar levels
Regular monitoring of blood sugar levels is essential for managing insulin resistance. This can be done through at-home blood glucose monitoring using a glucose meter. Monitoring helps track blood sugar patterns, identify potential issues, and adjust lifestyle or medication as needed. It is important to follow the individualized monitoring plan provided by a healthcare provider.
Working with a healthcare team
Managing insulin resistance requires a comprehensive approach that involves working with a healthcare team. This team may include a primary care physician, endocrinologist, registered dietitian, and exercise specialist. Collaborating with healthcare professionals can help individuals develop a personalized treatment plan, receive ongoing support and education, and address any concerns or complications associated with insulin resistance.
Effects of Insulin Resistance on Weight
How insulin resistance leads to weight gain
Insulin resistance can contribute to weight gain through several mechanisms. When cells are resistant to insulin, glucose cannot effectively enter the cells, resulting in higher blood sugar levels. The pancreas responds by producing more insulin, which can promote the storage of excess glucose as fat. Additionally, insulin resistance is often associated with imbalances in other hormones, such as leptin and ghrelin, which can affect appetite regulation and metabolism, contributing to weight gain.
Role of insulin in fat storage
Insulin plays a crucial role in fat storage. When insulin levels are elevated, it signals the body to store excess glucose as fat. Moreover, insulin inhibits the breakdown of fat in fat cells. In the presence of insulin resistance, higher insulin levels can promote increased fat storage and make it harder for the body to access stored fat for energy.
Difficulties in losing weight with insulin resistance
Individuals with insulin resistance may find it more challenging to lose weight. The imbalances in hormones and impaired insulin signaling can affect the body’s metabolism, making it harder to burn stored fat. Additionally, insulin resistance is often associated with increased appetite and cravings for sugary and high-calorie foods, which can further hinder weight loss efforts. However, adopting a healthy lifestyle, including regular exercise and a balanced diet, along with appropriate medical management, can still lead to successful weight loss even with insulin resistance.
Insulin Resistance and Type 2 Diabetes
Relationship between insulin resistance and diabetes
Insulin resistance is a key factor in the development of type 2 diabetes. When the body becomes resistant to insulin, the pancreas tries to compensate by producing more insulin. However, over time, the pancreas may no longer be able to keep up with the demand, resulting in high blood sugar levels. This leads to the development of type 2 diabetes. Insulin resistance and type 2 diabetes often coexist, and the majority of individuals with type 2 diabetes have some degree of insulin resistance.
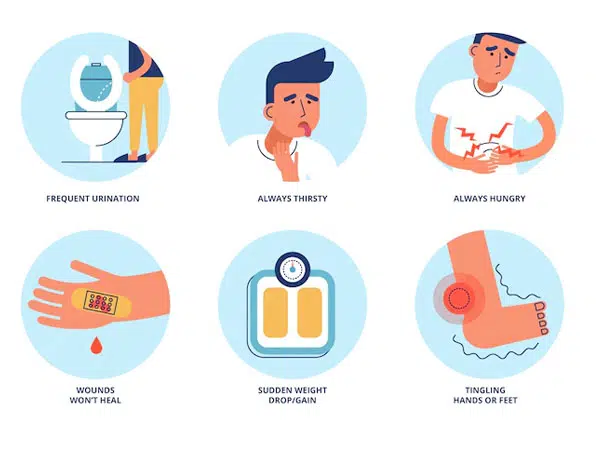
Symptoms and complications of type 2 diabetes
Type 2 diabetes can cause a range of symptoms, including increased thirst, frequent urination, unexplained weight loss, fatigue, blurred vision, and slow wound healing. If left untreated or poorly managed, type 2 diabetes can lead to various complications, including cardiovascular disease, kidney disease, nerve damage, eye problems, and foot problems. It is essential to promptly diagnose and effectively manage type 2 diabetes to prevent or minimize these complications.
Managing diabetes with insulin resistance
Managing both insulin resistance and type 2 diabetes often involves similar approaches. Lifestyle modifications, such as adopting a healthy eating plan, engaging in regular physical activity, and achieving a healthy weight, are crucial. Additionally, medications such as metformin or other glucose-lowering medications may be prescribed to help improve insulin sensitivity and effectively manage blood sugar levels. Regular monitoring of blood sugar levels and working closely with a healthcare team are also important for successful management.
Cardiovascular Risks Associated with Insulin Resistance
Increased risk of heart disease and stroke
Insulin resistance is associated with an increased risk of heart disease and stroke. The metabolic abnormalities associated with insulin resistance, including elevated blood sugar levels, high blood pressure, abnormal cholesterol levels, and inflammation, contribute to the development of atherosclerosis (hardening of the arteries). Over time, this can lead to the narrowing and blockage of blood vessels, increasing the risk of heart attacks and strokes.
Effects on blood pressure and cholesterol levels
Insulin resistance can lead to elevated blood pressure and abnormal cholesterol levels. Insulin is involved in regulating blood vessel constriction and relaxation, and its resistance can disrupt these processes, leading to higher blood pressure. Insulin resistance is also associated with imbalances in cholesterol levels, including higher levels of LDL cholesterol (the “bad” cholesterol) and lower levels of HDL cholesterol (the “good” cholesterol), which further contribute to cardiovascular risks.
Preventive measures for cardiovascular health
Preventing cardiovascular complications associated with insulin resistance involves managing the risk factors through lifestyle modifications and medical management. Adopting a heart-healthy diet, regular physical activity, maintaining a healthy weight, and quitting smoking are essential. Additionally, medications to control blood pressure, cholesterol levels, and blood sugar, as prescribed by a healthcare provider, may be necessary. Regular monitoring of blood pressure and cholesterol levels, along with ongoing collaboration with a healthcare team, are essential for managing cardiovascular risks.
Insulin Resistance and Polycystic Ovary Syndrome (PCOS)
Link between insulin resistance and PCOS
Insulin resistance is strongly associated with polycystic ovary syndrome (PCOS). In fact, insulin resistance is thought to play a significant role in the development and progression of PCOS. Insulin resistance disrupts the normal hormonal balance in the ovaries, leading to the production of excess androgens (male hormones). This hormonal imbalance can cause irregular menstrual cycles, ovarian cysts, infertility, and other symptoms associated with PCOS.
Symptoms and complications of PCOS
PCOS can cause a range of symptoms, including irregular or absent periods, excessive hair growth (hirsutism), acne, weight gain, and fertility problems. Over time, if not effectively managed, PCOS can lead to complications such as type 2 diabetes, high blood pressure, high cholesterol, sleep apnea, and an increased risk of endometrial cancer. Early detection and appropriate management of PCOS are crucial.
Treatment options for PCOS with insulin resistance
Managing PCOS with insulin resistance often involves a combination of lifestyle changes and medications. Lifestyle modifications, such as weight loss if necessary, a balanced diet, regular exercise, and stress management, can help improve insulin sensitivity and regulate hormone levels. Medications such as metformin or insulin-sensitizing agents may be prescribed to lower insulin levels and manage the symptoms of PCOS. Working closely with a healthcare team, including an endocrinologist and gynecologist, is important for individualized treatment and ongoing support.
Insulin Resistance and Non-alcoholic Fatty Liver Disease (NAFLD)
Connection between insulin resistance and NAFLD
Insulin resistance is closely linked to the development of non-alcoholic fatty liver disease (NAFLD). When the body is resistant to insulin, it struggles to efficiently metabolize fats, leading to the build-up of fat in the liver. This excess fat can cause inflammation and eventually progress to non-alcoholic steatohepatitis (NASH), a more severe form of NAFLD that can lead to liver fibrosis and cirrhosis. Insulin resistance is a significant contributor to the development and progression of NAFLD.
Effects on liver health and function
Insulin resistance and the associated NAFLD can have profound effects on liver health and function. The accumulation of fat in the liver can cause inflammation and damage, leading to the scarring and fibrosis of liver tissue. This can impair liver function and increase the risk of complications such as liver cirrhosis and liver cancer. Managing insulin resistance and NAFLD is crucial for maintaining liver health.
Management of NAFLD in the presence of insulin resistance
Managing NAFLD in the presence of insulin resistance requires a comprehensive approach that targets both conditions. Lifestyle modifications, including a balanced diet, regular physical activity, and weight loss if necessary, are key components of managing both conditions. Medications such as vitamin E, pioglitazone, and GLP-1 receptor agonists may be prescribed to help improve insulin sensitivity and liver health. Close monitoring by a healthcare team, including a hepatologist or gastroenterologist, is essential for effective management of NAFLD and insulin resistance.
In conclusion, insulin resistance is a significant health concern with various consequences on weight, diabetes, cardiovascular health, PCOS, liver health, cognitive function, and cancer risk. Recognizing the signs, taking preventive measures, and working closely with healthcare professionals can help manage insulin resistance and minimize the associated risks. Embracing a healthy lifestyle, including a balanced diet, regular exercise, stress management, and maintaining a healthy weight, is crucial in preventing or managing insulin resistance. Remember, your health is in your hands, and taking steps to address insulin resistance can lead to a healthier and happier future.