In this article, we will explore the intriguing connection between insulin resistance and Polycystic Ovary Syndrome (PCOS) in women. PCOS, a common hormonal disorder, affects many women worldwide and can lead to various health complications. Our focus will be on understanding how insulin resistance plays a significant role in the development and management of PCOS, and the potential implications this has for treatment options. By delving into the intricacies of this relationship, we hope to provide valuable insights into the underlying mechanisms of PCOS and offer potential avenues for improved care and support for women diagnosed with this condition. So, let’s embark on this journey and unlock the mysteries of insulin resistance in women with PCOS together!
Insulin Resistance in Polycystic Ovary Syndrome (PCOS)

Definition and Overview
Polycystic Ovary Syndrome (PCOS) is a common hormonal disorder that affects many women of reproductive age. It is characterized by a combination of symptoms, including irregular menstrual cycles, high levels of androgens (male hormones), and the presence of cysts on the ovaries. One important and often overlooked aspect of PCOS is the association with insulin resistance.
Insulin resistance occurs when the body’s cells do not respond properly to insulin, a hormone that regulates blood sugar levels. As a result, the body produces more insulin to compensate, leading to higher levels of insulin in the bloodstream. This can have various negative health implications, including an increased risk of developing type 2 diabetes and cardiovascular disease.
Prevalence of PCOS in Women
PCOS is one of the most common endocrine disorders in women of reproductive age, affecting approximately 5-10% of women worldwide. It is often underdiagnosed and misdiagnosed, making it difficult to estimate the true prevalence. However, it is clear that PCOS is a significant health concern that affects a large number of women.

Correlation between PCOS and Insulin Resistance
Research has shown a strong correlation between PCOS and insulin resistance. In fact, it is estimated that up to 70-80% of women with PCOS have some degree of insulin resistance. The exact relationship between PCOS and insulin resistance is complex and multifactorial, involving various genetic, hormonal, and environmental factors.
Implications and Health Risks
Insulin resistance in PCOS can have significant implications for a woman’s health. It can contribute to the development of metabolic disorders, such as prediabetes and type 2 diabetes mellitus. Women with PCOS and insulin resistance are also at a higher risk of developing gestational diabetes during pregnancy. Additionally, insulin resistance can increase the risk of cardiovascular disease, as well as other long-term health issues, including endometrial cancer.
Causes of Insulin Resistance in PCOS
Genetic Factors
Genetic factors play a significant role in the development of insulin resistance in PCOS. Several gene variants have been identified that are associated with an increased risk of developing insulin resistance. These genes are involved in various aspects of insulin action and metabolism, including insulin receptor signaling pathways.
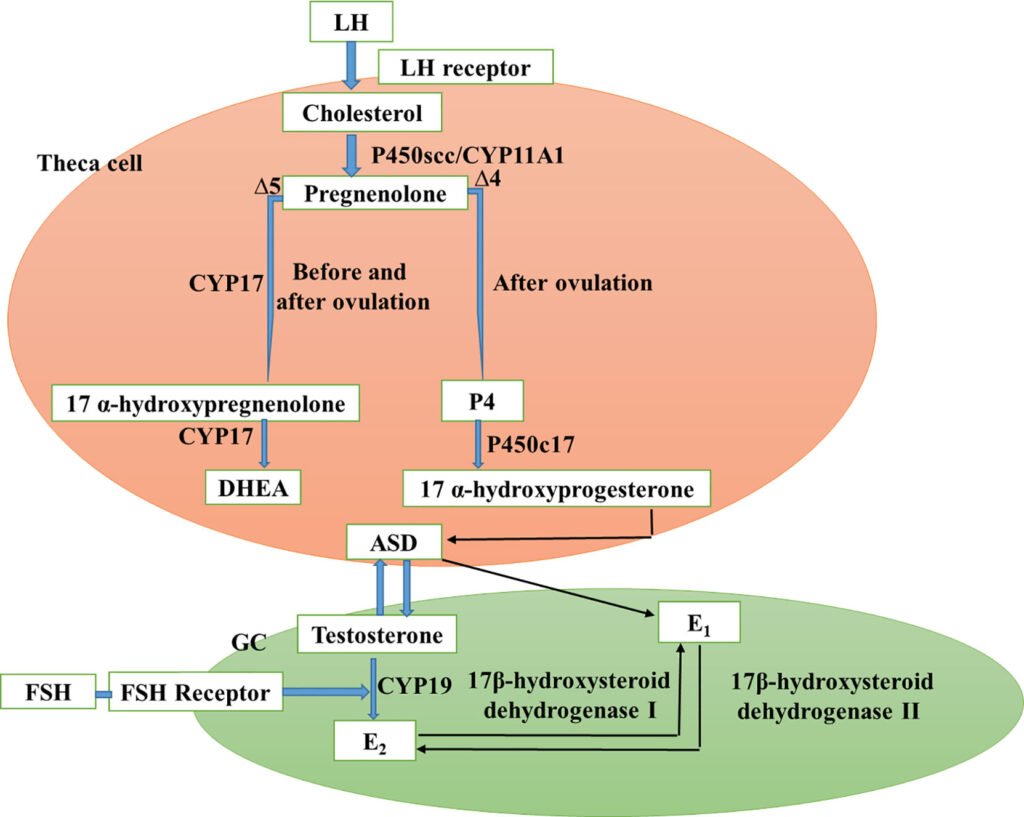
Hormonal Imbalance
Hormonal imbalances, such as elevated levels of androgens and insulin, can contribute to insulin resistance in PCOS. Androgens, which are typically elevated in women with PCOS, can interfere with insulin signaling pathways and lead to insulin resistance. Similarly, elevated insulin levels can disrupt hormonal balance and contribute to the development of insulin resistance.
Obesity and Weight Gain
Obesity and weight gain are known risk factors for the development of insulin resistance in PCOS. Excess adipose tissue, especially visceral fat, produces hormones and inflammatory factors that can interfere with insulin signaling pathways. Women with PCOS who are overweight or obese are more likely to have insulin resistance.
Role of Adipose Tissue
Adipose tissue, or body fat, plays a critical role in the development of insulin resistance in PCOS. Adipose tissue is not just a passive storage site for energy; it is an active endocrine organ that produces hormones, inflammatory factors, and other molecules that can impact insulin action. Increased levels of adipose tissue, especially in the abdominal region, are associated with insulin resistance in PCOS.
Inflammation and Oxidative Stress
Inflammation and oxidative stress are two interconnected processes that can contribute to insulin resistance in PCOS. Chronic low-grade inflammation and increased oxidative stress can impair insulin signaling pathways and promote insulin resistance. These processes are influenced by various factors, including hormonal imbalances, obesity, and lifestyle factors.
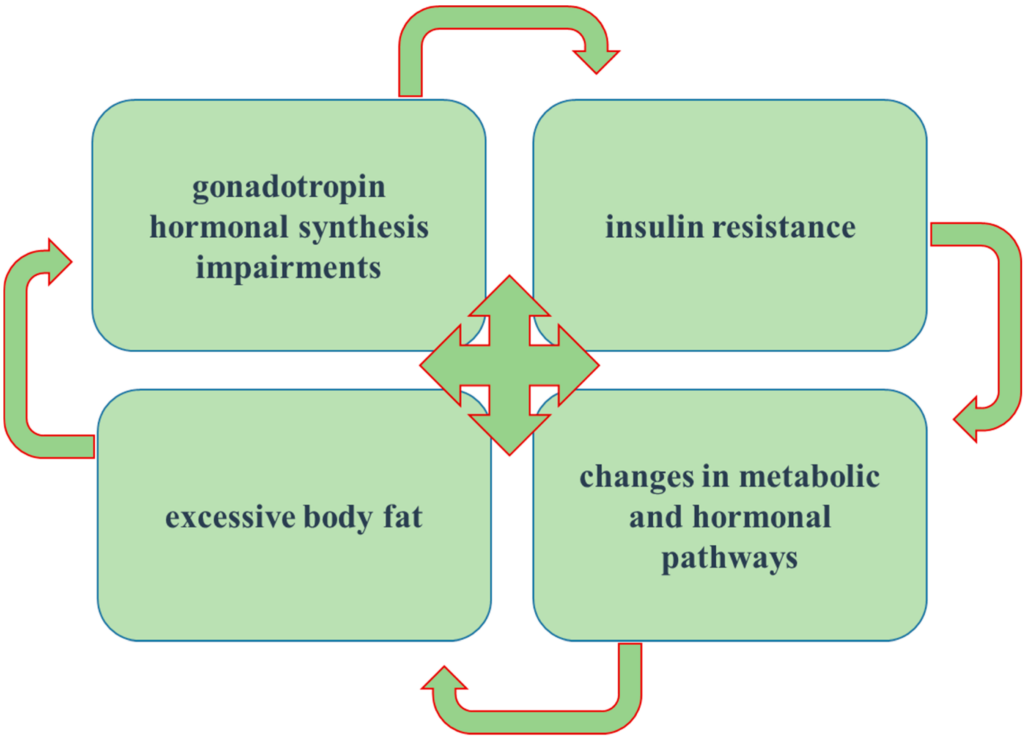
Mechanisms of Insulin Resistance in PCOS
Insulin Signaling Pathway
Insulin resistance in PCOS is characterized by defects in the insulin signaling pathway. In normal conditions, insulin binds to its receptor on the surface of cells, initiating a cascade of events that allow glucose to enter the cell. In women with PCOS and insulin resistance, this signaling pathway is impaired, leading to reduced glucose uptake and increased blood sugar levels.
Intra-ovarian Abnormalities
Abnormalities within the ovaries themselves can also contribute to insulin resistance in PCOS. The ovaries of women with PCOS are often enlarged and contain numerous follicles, which can interfere with insulin signaling and glucose metabolism. These intra-ovarian abnormalities can further contribute to hormonal imbalances and insulin resistance.
Hyperandrogenism
Hyperandrogenism, or elevated levels of androgens, is a hallmark feature of PCOS and can contribute to insulin resistance. Androgens, such as testosterone, can disrupt insulin signaling pathways and impair glucose metabolism. In turn, insulin resistance can further exacerbate hyperandrogenism, creating a vicious cycle that perpetuates the underlying hormonal imbalances.
Adipokines and Cytokines
Adipokines and cytokines are proteins secreted by adipose tissue and immune cells, respectively. In women with PCOS, there is dysregulation in the production and release of these molecules, which can contribute to insulin resistance. Adipokines, such as adiponectin and leptin, can impact insulin sensitivity, while cytokines, such as tumor necrosis factor-alpha (TNF-alpha), can induce inflammation and interfere with insulin signaling.
Impact of Insulin Resistance on PCOS Symptoms
Menstrual Irregularities
Insulin resistance can disrupt the delicate hormonal balance in women with PCOS, leading to menstrual irregularities. Women with insulin resistance may experience missed periods, infrequent periods, or prolonged periods. These disruptions in the menstrual cycle can make it difficult for women with PCOS to conceive and can contribute to fertility issues.
Hyperandrogenism and Hirsutism
Insulin resistance can exacerbate hyperandrogenism in women with PCOS, leading to increased levels of male hormones. This can result in symptoms such as hirsutism (excessive hair growth), acne, and male pattern baldness. These physical manifestations of hyperandrogenism can have a significant impact on a woman’s self-esteem and quality of life.
Polycystic Ovaries
Insulin resistance is closely associated with the formation of multiple cysts on the ovaries, a hallmark feature of PCOS. The impaired insulin signaling pathways in the ovaries can disrupt follicle development and lead to the formation of cysts. The presence of polycystic ovaries can further contribute to hormonal imbalances and insulin resistance in PCOS.
Metabolic Disorders
Insulin resistance in PCOS is strongly associated with the development of metabolic disorders, such as prediabetes and type 2 diabetes mellitus. Women with PCOS and insulin resistance have an increased risk of developing these conditions compared to women without PCOS. Controlling insulin resistance and maintaining healthy blood sugar levels is crucial in preventing the progression to these metabolic disorders.
Cardiovascular Risk
Insulin resistance in PCOS is also a risk factor for cardiovascular disease. Women with PCOS and insulin resistance are more likely to develop high blood pressure, dyslipidemia (abnormal cholesterol levels), and other risk factors for cardiovascular disease. Managing insulin resistance and adopting a heart-healthy lifestyle are essential for reducing these risks.
Diagnostic Methods for Insulin Resistance in PCOS
Oral Glucose Tolerance Test (OGTT)
The oral glucose tolerance test (OGTT) is a commonly used diagnostic tool for assessing insulin resistance. During this test, a fasting blood sample is taken, followed by the administration of a glucose-rich drink. Blood samples are then taken at regular intervals to measure how the body handles the glucose. Elevated blood glucose levels and insulin levels during the test indicate insulin resistance.
Fasting Insulin Levels
Fasting insulin levels can provide valuable information about insulin resistance in PCOS. Elevated fasting insulin levels are indicative of decreased insulin sensitivity and may suggest the presence of insulin resistance. However, fasting insulin levels alone may not provide a complete picture, and additional tests may be necessary to confirm the diagnosis.
Homeostatic Model Assessment of Insulin Resistance (HOMA-IR)
The homeostatic model assessment of insulin resistance (HOMA-IR) is a mathematical formula that estimates insulin resistance based on fasting glucose and insulin levels. It provides a convenient and cost-effective method for assessing insulin resistance in clinical settings. HOMA-IR values above a certain threshold indicate insulin resistance.
Hyperinsulinemic Euglycemic Clamp
The hyperinsulinemic euglycemic clamp is considered the gold standard for measuring insulin resistance. It involves the continuous infusion of insulin to maintain a stable blood glucose level. The amount of glucose needed to maintain euglycemia (normal blood sugar level) during the clamp procedure reflects insulin sensitivity. Lower glucose infusion rates indicate higher insulin resistance.
Other Emerging Biomarkers
Researchers are exploring other potential biomarkers for assessing insulin resistance in PCOS. These include adipokines, such as adiponectin and leptin, and inflammatory markers, such as C-reactive protein (CRP). These biomarkers may provide additional insights into the underlying mechanisms of insulin resistance and could potentially be used for diagnostic purposes in the future.
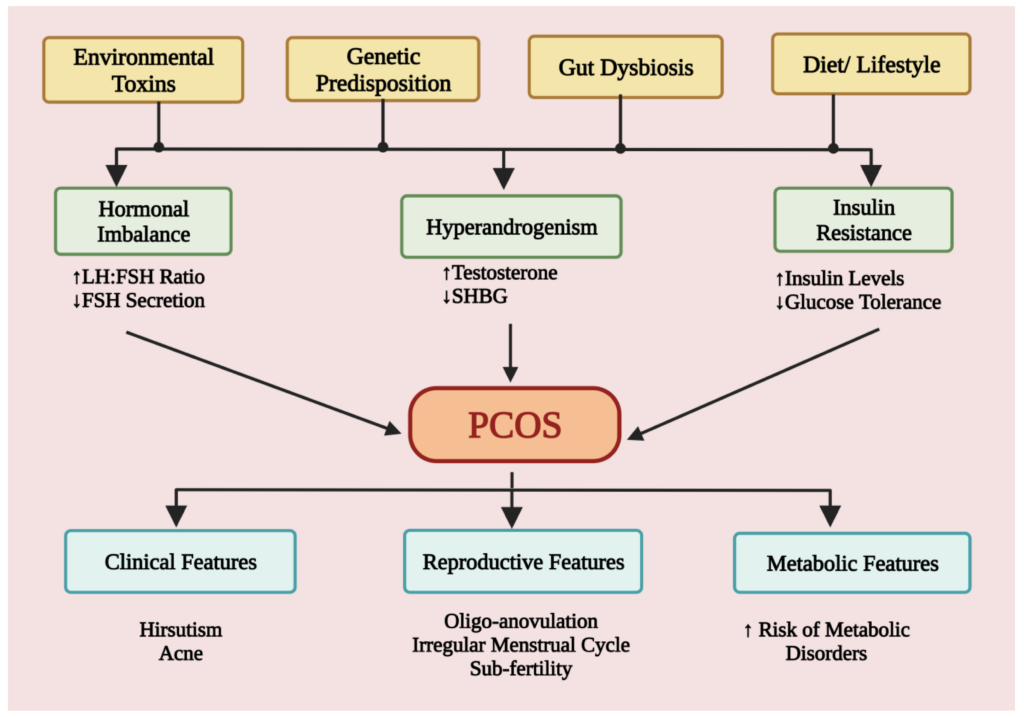
Management and Treatment of Insulin Resistance in PCOS
Lifestyle Modifications
Lifestyle modifications are the first line of treatment for insulin resistance in PCOS. These include adopting a healthy diet, engaging in regular physical activity, managing stress levels, and getting adequate sleep. These lifestyle changes can help improve insulin sensitivity, promote weight loss, and reduce the risk of developing metabolic and cardiovascular complications.
Dietary Interventions
Certain dietary interventions have been shown to be beneficial for women with PCOS and insulin resistance. These include following a low-glycemic index diet, which focuses on consuming foods that have a minimal impact on blood sugar levels. Increasing fiber intake, eating balanced meals, and avoiding highly processed foods can also help improve insulin sensitivity.
Weight Loss
Weight loss is an essential component of managing insulin resistance in PCOS, particularly in overweight or obese individuals. Even modest weight loss of 5-10% can improve insulin sensitivity and reduce the risk of metabolic complications. Combining dietary changes with regular physical activity is the most effective approach for achieving sustainable weight loss.
Exercise and Physical Activity
Regular exercise and physical activity are crucial for improving insulin sensitivity in women with PCOS. Engaging in aerobic exercise, such as walking, jogging, swimming, or cycling, can help lower insulin levels, increase glucose uptake by muscles, and improve overall metabolic health. Strength training exercises can also be beneficial for building lean muscle mass and improving insulin sensitivity.
Pharmacological Interventions
In some cases, lifestyle modifications alone may not be sufficient to manage insulin resistance in PCOS. Pharmacological interventions, such as metformin, may be prescribed to help improve insulin sensitivity. Metformin is an oral medication that reduces glucose production by the liver and enhances glucose uptake by muscles. It is commonly used in the treatment of type 2 diabetes and has been shown to be beneficial for women with PCOS and insulin resistance.
Long-term Health Implications of Insulin Resistance in PCOS
Type 2 Diabetes Mellitus (T2DM)
Insulin resistance in PCOS significantly increases the risk of developing type 2 diabetes mellitus (T2DM) later in life. Women with PCOS and insulin resistance should be closely monitored for the development of prediabetes and T2DM. Lifestyle modifications, including healthy eating, regular exercise, and weight management, are crucial for preventing or delaying the onset of T2DM.
Gestational Diabetes
Insulin resistance in PCOS is also a risk factor for developing gestational diabetes during pregnancy. Women with PCOS should be screened for gestational diabetes early in pregnancy and managed appropriately to ensure a healthy pregnancy outcome. Close monitoring of blood glucose levels, dietary modifications, and, in some cases, insulin therapy may be necessary.
Cardiovascular Disease
Insulin resistance in PCOS is associated with an increased risk of cardiovascular disease. Women with PCOS should be screened for cardiovascular risk factors, such as high blood pressure and abnormal cholesterol levels, and managed accordingly. Adopting a heart-healthy lifestyle, including regular exercise, a balanced diet, and smoking cessation, is essential for reducing the risk of cardiovascular complications.
Endometrial Cancer
Insulin resistance in PCOS is a risk factor for endometrial cancer, a type of cancer that affects the lining of the uterus. Chronic exposure to high levels of insulin and elevated estrogen levels associated with insulin resistance can increase the risk of abnormal cell growth in the endometrium. Regular gynecological screenings and appropriate management of insulin resistance are crucial for reducing the risk of endometrial cancer.
Psychological and Emotional Impact
The impact of insulin resistance in PCOS goes beyond physical health and can significantly affect a woman’s psychological and emotional well-being. The hormonal imbalances, menstrual irregularities, and physical changes associated with PCOS and insulin resistance can lead to feelings of anxiety, depression, and decreased quality of life. It is important for healthcare providers to address these psychological aspects and provide appropriate support and counseling.
Differentiating Insulin Resistance in PCOS from Other Conditions
Type 2 Diabetes Mellitus
Insulin resistance in PCOS and type 2 diabetes mellitus share some similarities but have distinct differences. While both conditions are characterized by insulin resistance, PCOS is primarily a hormonal disorder with additional features such as irregular menstrual cycles and polycystic ovaries. Type 2 diabetes, on the other hand, is a metabolic disorder characterized by elevated blood sugar levels and impaired insulin production.
Metabolic Syndrome
Metabolic syndrome is a collection of conditions that occur together and increase the risk of cardiovascular disease and type 2 diabetes. Insulin resistance is a key feature of metabolic syndrome, along with obesity, high blood pressure, abnormal cholesterol levels, and abdominal obesity. While some women with PCOS may also have metabolic syndrome, not all individuals with insulin resistance in PCOS will meet the criteria for metabolic syndrome.
Cushing’s Syndrome
Cushing’s syndrome is a rare hormonal disorder characterized by elevated levels of cortisol, a stress hormone. It can cause weight gain, high blood pressure, and insulin resistance, among other symptoms. While both PCOS and Cushing’s syndrome can lead to insulin resistance, their underlying causes and clinical presentations are distinct. Diagnostic testing, including cortisol level measurements, can help differentiate between the two conditions.
Non-Alcoholic Fatty Liver Disease (NAFLD)
Insulin resistance is closely associated with the development of non-alcoholic fatty liver disease (NAFLD), a condition characterized by excessive fat accumulation in the liver. Both PCOS and NAFLD are often associated with insulin resistance, but they can occur independently of each other. Women with PCOS and insulin resistance should be monitored for the development of NAFLD and managed accordingly.
Future Research and Advancements in Understanding Insulin Resistance in PCOS
Identification of Novel Biomarkers
Ongoing research aims to identify novel biomarkers that can accurately assess insulin resistance in PCOS. These biomarkers may provide valuable insights into the underlying mechanisms of insulin resistance and help improve diagnostic accuracy and personalized treatment approaches.
Targeted Therapies
Advancements in our understanding of the molecular mechanisms of insulin resistance in PCOS may lead to the development of targeted therapies. These therapies could specifically address the underlying defects in insulin signaling pathways and improve insulin sensitivity in women with PCOS.
Precision Medicine Approaches
Precision medicine approaches, which involve tailoring treatments to an individual’s specific characteristics, hold promise for managing insulin resistance in PCOS. By considering an individual’s genetic, hormonal, and metabolic profiles, healthcare providers can optimize treatment plans and improve outcomes for women with PCOS and insulin resistance.
Role of Gut Microbiota
Emerging evidence suggests that the gut microbiota, the trillions of bacteria residing in the intestines, may play a role in insulin resistance and PCOS. Future research will likely explore the relationship between gut microbiota composition, insulin resistance, and PCOS, with the aim of developing targeted interventions that modulate the gut microbiota and improve metabolic health.
Conclusion
Insulin resistance is a significant feature of polycystic ovary syndrome (PCOS) and has important implications for a woman’s health. Understanding the causes, mechanisms, and impact of insulin resistance in PCOS is crucial for improving diagnostic accuracy and developing targeted treatment strategies. Lifestyle modifications, including healthy eating, regular exercise, and weight management, are the cornerstone of management. Pharmacological interventions may also be necessary in some cases. By addressing insulin resistance and its associated health risks, women with PCOS can improve their overall well-being and reduce the long-term complications associated with the condition.