Picture this: it’s a warm summer day, and you’re enjoying a picnic in the park with friends. Suddenly, out of nowhere, your lips start swelling up to twice their size, making it hard to speak or even breathe. What you’re experiencing is angioedema, a condition that causes sudden swelling in the deeper layers of your skin. But did you know that angioedema can be linked to allergies? In this article, we’ll take a closer look at this mysterious connection and shed light on what can trigger these uncomfortable episodes. So sit back, relax, and let’s explore the fascinating world of angioedema and allergies together.
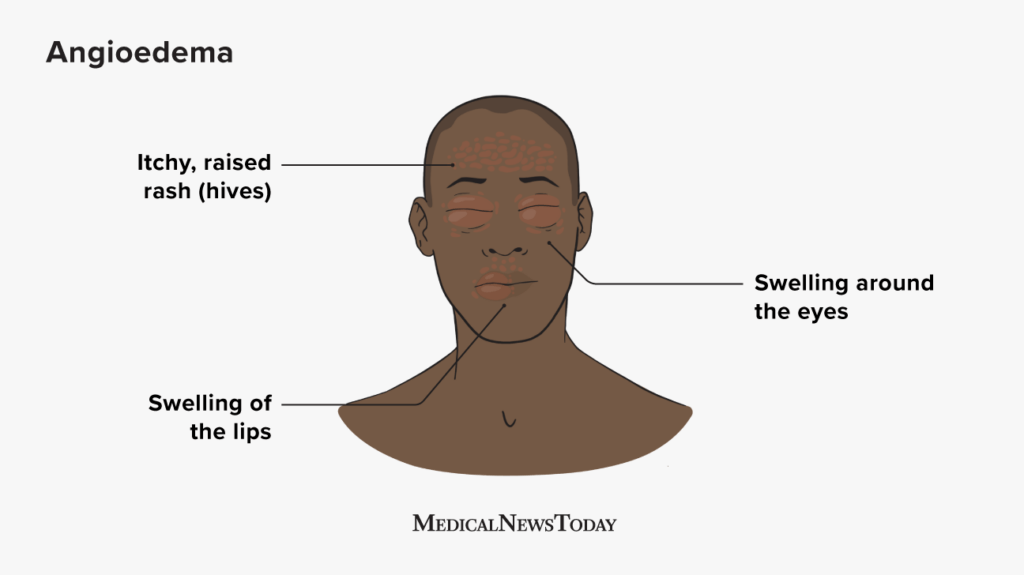
Overview of Angioedema and Allergies
Definition of Angioedema
Angioedema is a condition characterized by localized swelling and inflammation of the deeper layers of the skin and submucosal tissues. This swelling occurs most commonly in the face, lips, tongue, throat, and genital area. It is often accompanied by itching and a burning sensation. The swelling in angioedema can be sudden and severe, causing discomfort and potential breathing difficulties.
Definition of Allergies
Allergies, on the other hand, are immune system reactions to substances that are usually harmless. When an individual with allergies comes into contact with an allergen, the immune system releases a chemical called histamine, which triggers an inflammatory response. This response can manifest in various ways, such as sneezing, itching, watery eyes, and in some cases, angioedema.
Types of Angioedema
There are different types of angioedema, including hereditary angioedema (HAE), acquired angioedema (AAE), and idiopathic angioedema. HAE is a rare genetic disorder caused by a deficiency or dysfunction of a protein called C1 inhibitor. AAE is typically associated with autoimmune disorders or certain medications. Idiopathic angioedema, on the other hand, has no clearly identifiable cause.
Causes of Angioedema
Angioedema can have various underlying causes, including allergic reactions, medications, infection, autoimmune disorders, and genetic factors. Allergic angioedema is triggered by exposure to allergens, such as certain foods, insect bites, medications, or environmental factors. Identifying the specific cause of angioedema is crucial in determining the most appropriate treatment plan.
Common Allergens
Several common allergens can trigger angioedema in susceptible individuals. Food allergies, such as those to nuts, shellfish, milk, and eggs, are known to cause angioedema in some cases. Insect stings or bites from bees, wasps, or ants can also lead to angioedema. Moreover, certain medications, such as penicillin or non-steroidal anti-inflammatory drugs (NSAIDs), have been associated with allergic angioedema. It’s important for individuals prone to angioedema to be aware of these common allergens and take necessary precautions.
Symptoms and Diagnosis
Symptoms of Angioedema
The symptoms of angioedema are characterized by sudden swelling of the affected areas, such as the face, lips, or throat. The swelling can be accompanied by redness, warmth, and itching. In some cases, angioedema may cause difficulty in breathing, speaking, or swallowing, which can be life-threatening. It is important to recognize these symptoms early on and seek medical attention to prevent any complications.
Diagnosing Angioedema
Diagnosing angioedema often involves a comprehensive evaluation of the patient’s medical history, physical examination, and diagnostic tests. The doctor will inquire about any family history of angioedema, exposures to potential triggers, and the characteristics of the swelling and associated symptoms. Blood tests may also be conducted to check for any underlying autoimmune disorders or deficiencies in specific proteins.
Distinguishing Angioedema from Allergies
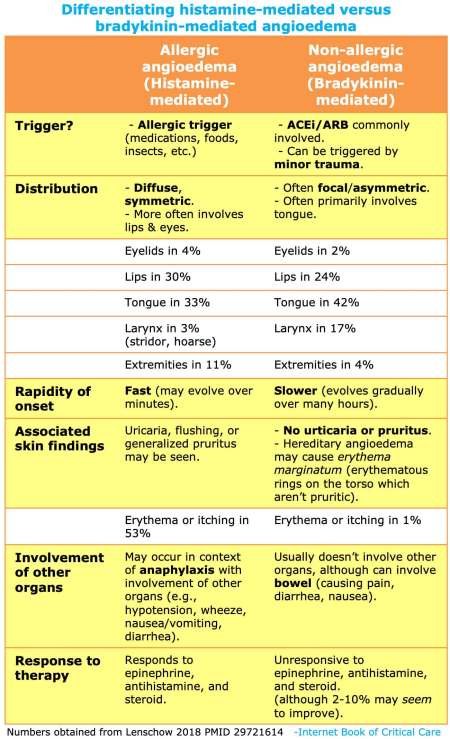
Distinguishing between angioedema and allergies can sometimes be challenging, as they share similar symptoms such as swelling, redness, and itching. However, there are certain distinguishing factors to consider. Angioedema typically involves swelling beneath the skin’s surface, while allergic reactions often cause more superficial swelling. Additionally, angioedema is often associated with a rapid onset and can affect specific areas, such as the lips or throat, whereas allergies may result in more generalized symptoms throughout the body.
Understanding the Link
Mechanism of Allergic Angioedema
Allergic angioedema occurs when an individual with a hypersensitive immune system comes into contact with an allergen. The immune system recognizes the allergen as a threat and releases immunoglobulin E (IgE) antibodies. These antibodies then bind to mast cells, triggering the release of various chemical mediators, including histamine. Histamine causes blood vessels to dilate and become leaky, leading to localized swelling and inflammation, characteristic of angioedema.
Role of IgE in Angioedema
Immunoglobulin E (IgE) plays a crucial role in allergic angioedema. IgE is an antibody produced by the immune system in response to an allergen exposure. When the specific allergen is encountered again, the immune system recognizes it, causing the release of IgE antibodies. These antibodies then bind to mast cells and basophils, triggering the release of histamine and other inflammatory substances, leading to angioedema.
Other Related Allergic Reactions
Allergic angioedema is often associated with other allergic reactions, such as hives (urticaria) or allergic rhinitis (hay fever). Hives are characterized by raised, itchy, and red welts on the skin, while allergic rhinitis commonly presents as a runny or stuffy nose, sneezing, and itchy eyes. These reactions may occur simultaneously with angioedema or independently, depending on the individual’s immune system response to the allergen.
Risk Factors and Prevention
Risk Factors for Angioedema
Certain factors can increase an individual’s risk of developing angioedema. These include a family history of angioedema, a personal history of allergies or allergic reactions, and certain underlying medical conditions, such as autoimmune disorders or chronic urticaria. It is important for individuals with these risk factors to be aware of the potential for angioedema and take appropriate precautions.
Preventing Angioedema in Allergic Individuals
Preventing angioedema in allergic individuals primarily involves avoiding triggering allergens. This may include strict avoidance of certain foods or medications, using insect repellent to prevent insect bites, and taking necessary precautions in known environments that may contain allergens, such as pollen-rich areas during allergy seasons. Consulting with an allergist can help develop a personalized management plan to minimize the risk of angioedema.
Avoiding Common Allergens
Being knowledgeable about common allergens is crucial for individuals prone to angioedema. It is important to read ingredient labels carefully and avoid foods that contain allergens known to trigger angioedema, such as nuts, shellfish, or eggs. Furthermore, individuals should inform healthcare providers of any known allergies or previous episodes of angioedema to prevent the prescribing of medications that could potentially trigger a reaction.
Treatment Options
Medications for Acute Angioedema
The treatment of acute angioedema often involves the use of antihistamines and corticosteroids to reduce the allergic response and alleviate symptoms. Antihistamines work by blocking the effects of histamine, while corticosteroids help reduce inflammation. In more severe cases, epinephrine may be administered to counteract the allergic response and quickly relieve swelling and breathing difficulties.
Long-Term Management of Angioedema
For individuals with recurrent or chronic angioedema, long-term management is necessary to prevent future episodes. This may include identifying and avoiding triggering factors, such as certain medications or allergens, and taking preventative medications, such as antihistamines or leukotriene inhibitors. Maintaining a healthy lifestyle, managing stress, and avoiding extreme temperatures or physical exertion can also be beneficial in managing angioedema.
Emergency Measures for Severe Angioedema
In cases of severe angioedema that affects the airways and potentially leads to difficulty breathing, immediate medical attention is crucial. Emergency measures may include the administration of epinephrine, along with other supportive measures such as airway management, oxygen supplementation, and intravenous fluids. Prompt action is necessary to prevent life-threatening complications, such as anaphylaxis.
Case Studies and Research
Recent Studies on Angioedema and Allergies
Recent studies have focused on further understanding the link between angioedema and allergies, as well as exploring effective treatment options. Some studies have identified genetic factors contributing to the development of angioedema, while others have investigated new medications that target specific pathways involved in the allergic response. These studies provide valuable insights into the mechanisms behind angioedema and may lead to improved management strategies.
Case Studies on Allergic Angioedema
Numerous case studies have been conducted to explore the specific triggers and management approaches for allergic angioedema. These case studies often involve detailed patient histories, diagnostic evaluations, and response to various treatment modalities. By analyzing these individual cases, healthcare professionals can gain valuable insights into the complexities of allergic angioedema and tailor treatment plans to meet the specific needs of patients.

Potential Complications
Anaphylaxis and Angioedema
One potential complication of angioedema is anaphylaxis, a severe and life-threatening allergic reaction. Anaphylaxis involves a rapid and widespread release of inflammatory mediators, leading to a systemic response that can affect multiple organs, including the respiratory system, cardiovascular system, and skin. Prompt recognition and treatment are essential in these cases, as anaphylaxis can rapidly progress and be fatal if left untreated.
Chronic Angioedema and Quality of Life
Chronic angioedema can significantly impact an individual’s quality of life. Recurrent episodes of swelling, discomfort, and potential limitations in daily activities may lead to feelings of frustration, anxiety, and reduced self-esteem. Seeking support from healthcare professionals, joining support groups, and educating oneself about the condition can help patients cope with the challenges of living with chronic angioedema.
Living with Angioedema
Coping Strategies for Angioedema Patients
Living with angioedema can be challenging, but there are coping strategies that can help manage the condition. It is important to stay informed about triggers and avoid exposure to allergens whenever possible. Developing a personalized management plan with the guidance of healthcare professionals can provide a sense of control and empower individuals to proactively manage their angioedema. Additionally, stress management techniques, such as deep breathing exercises and mindfulness, may help reduce the frequency and severity of episodes.
Support Groups and Resources
Joining support groups or connecting with others who have similar experiences can provide invaluable emotional support for individuals living with angioedema. These groups can provide an opportunity to share experiences, exchange strategies for coping, and find comfort in knowing that one is not alone. Online resources, such as educational websites and forums, can also provide helpful information and support for individuals and their families.
When to Seek Medical Help
Situations Requiring Immediate Medical Attention
It is important to seek immediate medical attention if an individual experiences severe angioedema that affects the airways or if they exhibit signs of anaphylaxis. Symptoms such as difficulty breathing, swelling in the throat or tongue, chest pain, dizziness, or fainting should never be ignored. Timely intervention in these situations can be life-saving and prevent potential complications.
Conclusion
Summary of Angioedema-Allergy Connection
In summary, angioedema can be triggered by allergic reactions and is often associated with other allergic conditions, such as hives or allergic rhinitis. Understanding the link between angioedema and allergies is essential for effective prevention, diagnosis, and management of this condition. By identifying triggering factors, taking preventative measures, and seeking prompt medical attention when necessary, individuals can better navigate living with angioedema, ensuring a higher quality of life. With ongoing research and advancements in treatment options, the outlook for individuals with angioedema continues to improve.