In this article, we will take a closer look at the fascinating connection between the Epstein-Barr virus and Burkitt lymphoma. This relationship between a virus and a type of cancer highlights the intricate nature of the human body and the potential impacts of viral infections. By exploring the mechanisms behind this connection, we hope to gain a better understanding of the development and progression of Burkitt lymphoma, ultimately paving the way for improved diagnostic and treatment strategies. So grab a cup of tea, get comfortable, and let’s embark on this enlightening exploration together.
Overview of Epstein-Barr Virus (EBV)
Introduction to EBV
Epstein-Barr Virus (EBV) is a member of the herpesvirus family and is one of the most common human viruses worldwide. It was first discovered in 1964 by Sir Michael Anthony Epstein and Ms. Yvonne Barr. EBV is known for causing infectious mononucleosis, also known as “mono” or “the kissing disease” due to its mode of transmission. However, EBV can also lead to the development of various cancers, including Burkitt Lymphoma.
Prevalence of EBV
EBV infection is highly prevalent globally, with an estimated 95% of adults being infected with the virus at some point in their lives. The infection usually occurs during childhood or adolescence, often without causing any noticeable symptoms. In developed countries, primary EBV infection is more common in individuals from lower socioeconomic backgrounds.
Transmission of EBV
EBV spreads through direct contact with the saliva or mucus of an infected person. It can be transmitted through activities such as kissing, sharing utensils or drinks, or even through respiratory droplets. Additionally, EBV can be spread through blood transfusions or organ transplantations from infected individuals.
EBV Infection and Latency
After initial infection, EBV establishes lifelong latency within B lymphocytes, a type of white blood cell. During this latent phase, the virus can reactivate periodically, but usually remains dormant and does not cause any harm. However, in certain circumstances, such as immune suppression or genetic predisposition, EBV can lead to the development of tumors, including Burkitt Lymphoma.
Symptoms and Complications of EBV Infection
When primary EBV infection occurs, it often presents as infectious mononucleosis. Common symptoms include severe fatigue, sore throat, swollen lymph nodes, and fever. In some cases, the spleen or liver may become enlarged. Most individuals recover from mono within a few weeks or months, but fatigue may persist for several months. However, EBV infection can also lead to more serious complications, such as Burkitt Lymphoma.
Introduction to Burkitt Lymphoma
Definition and Classification of Burkitt Lymphoma
Burkitt Lymphoma is a highly aggressive form of non-Hodgkin lymphoma, a type of cancer that affects the lymphatic system. It was first described by Denis Burkitt, a British surgeon, in the 1950s while working in Uganda. Burkitt Lymphoma is characterized by rapidly growing tumors that primarily affect the jaw and facial bones, although it can occur in other parts of the body as well. There are three distinct subtypes of Burkitt Lymphoma: endemic, sporadic, and immunodeficiency-associated.
Historical Background of Burkitt Lymphoma
Burkitt Lymphoma gained recognition in the medical community in the 1960s when it was observed that the disease was much more prevalent in certain regions of Africa, particularly where malaria was also endemic. This led to the hypothesis that there might be an infectious agent involved in the development of Burkitt Lymphoma. Subsequent research identified EBV as the primary contributing factor, especially in endemic Burkitt Lymphoma cases in Africa.
Global Occurrence of Burkitt Lymphoma
Burkitt Lymphoma occurs worldwide but exhibits substantial geographical variation in its distribution. Endemic Burkitt Lymphoma is most commonly found in equatorial Africa, accounting for a significant proportion of childhood cancers in this region. Sporadic Burkitt Lymphoma, on the other hand, is more prevalent in Western countries, including Europe and North America. Immunodeficiency-associated Burkitt Lymphoma occurs predominantly in individuals with compromised immune systems, such as those with HIV/AIDS.
Epstein-Barr Virus and Burkitt Lymphoma: Epidemiological Evidence
Association of EBV Infection with Burkitt Lymphoma
Extensive epidemiological and laboratory studies have established a strong association between EBV infection and the development of Burkitt Lymphoma. In endemic areas of Africa, nearly all cases of Burkitt Lymphoma are EBV-positive. However, in non-endemic regions, only a subset of Burkitt Lymphoma cases are associated with EBV infection, with varying frequencies depending on the population studied.
Geographical Variability of EBV-Positive Burkitt Lymphoma Cases
The relationship between EBV and Burkitt Lymphoma exhibits geographical variation. In endemic areas, nearly all Burkitt Lymphoma cases are EBV-positive. In contrast, sporadic Burkitt Lymphoma cases in Western countries have a lower prevalence of EBV association, ranging from 20% to 40%. Immunodeficiency-associated Burkitt Lymphoma cases, particularly in individuals with HIV infection, are frequently associated with EBV.
EBV Seroprevalence in Burkitt Lymphoma Patients
Seroprevalence studies have shown that individuals with Burkitt Lymphoma have higher levels of antibodies against EBV compared to healthy individuals. This suggests a link between EBV infection and the development of Burkitt Lymphoma. However, it is important to note that EBV infection alone is not sufficient to trigger the development of Burkitt Lymphoma, as the interplay between various genetic and environmental factors is also critical.
Mechanisms of EBV Contribution to Burkitt Lymphoma Development
Oncogenic Role of EBV in Burkitt Lymphoma
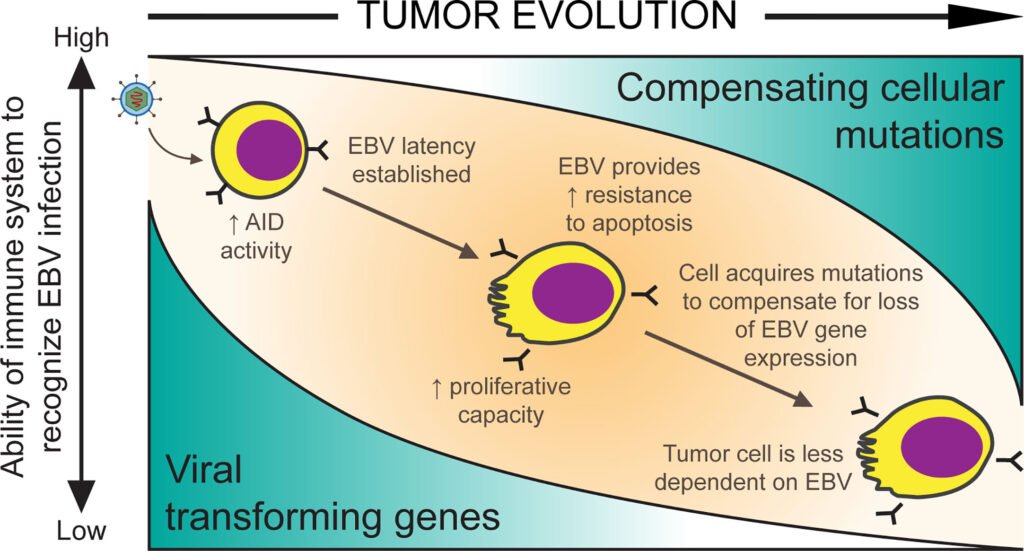
EBV plays an oncogenic role in the development of Burkitt Lymphoma by altering the growth and survival of B lymphocytes. The virus encodes several proteins that promote cell proliferation and prevent apoptosis, thereby contributing to the uncontrolled growth of cancerous lymphocytes. Additionally, EBV can dysregulate the immune system’s response to tumor cells, allowing the lymphoma cells to evade immune surveillance.
Activation of MYC Oncogene in EBV-Positive Burkitt Lymphoma
One of the key mechanisms through which EBV contributes to Burkitt Lymphoma development is by activating the MYC oncogene. MYC plays a critical role in cell growth and division and is usually tightly regulated. However, in Burkitt Lymphoma, EBV infection leads to the translocation of the MYC gene, resulting in its dysregulated expression. This uncontrolled MYC expression drives the aggressive growth of Burkitt Lymphoma cells.
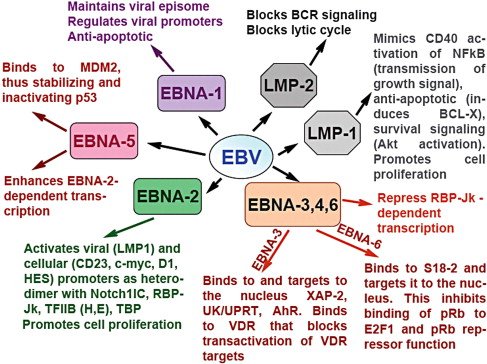
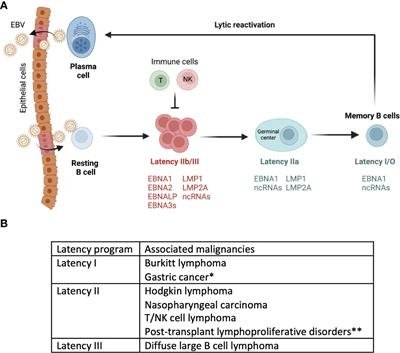
EBV Latency Patterns and Gene Expression in Burkitt Lymphoma
EBV demonstrates a latency pattern in Burkitt Lymphoma, with restricted viral gene expression. The virus mainly expresses a set of latent proteins, including Epstein-Barr Nuclear Antigen 1 (EBNA1) and Latent Membrane Proteins (LMP1, LMP2A, LMP2B). These proteins play a crucial role in lymphomagenesis by promoting cell survival, proliferation, and immune evasion.

EBV Infection and Immune Response in Burkitt Lymphoma
Immune Evasion Strategies Employed by EBV in Burkitt Lymphomagenesis
EBV has evolved various strategies to evade immune detection and destruction, thereby promoting the development and progression of Burkitt Lymphoma. The virus can manipulate both the innate and adaptive immune responses, impairing the recognition and elimination of infected cells by immune cells. This immune evasion allows EBV-infected B lymphocytes to persist and accumulate oncogenic alterations, leading to lymphoma development.
Role of Host Immune Response in Controlling EBV-driven Burkitt Lymphoma
Although EBV has developed immune evasion mechanisms, the host immune response still plays a crucial role in controlling EBV-driven Burkitt Lymphoma. The generation of EBV-specific immune cells, such as cytotoxic T lymphocytes (CTLs) and natural killer (NK) cells, is essential for the surveillance and elimination of EBV-infected cells. Enhancing the host immune response against EBV has been explored as a potential therapeutic strategy for Burkitt Lymphoma.
EBV-Specific Immune Therapies for Burkitt Lymphoma
Several approaches have been investigated for the development of EBV-specific immune therapies for Burkitt Lymphoma. These include adoptive immunotherapy, in which EBV-specific immune cells are expanded in the laboratory and infused back into the patient, and the use of therapeutic vaccines to enhance the immune response against EBV-infected cells. These strategies show promise in improving treatment outcomes for EBV-related Burkitt Lymphoma.
Diagnostic Tools for EBV-Associated Burkitt Lymphoma
Detection of EBV in Burkitt Lymphoma Tissue Samples
The presence of EBV in Burkitt Lymphoma tissue samples can be detected using various laboratory techniques. These include immunohistochemistry, in situ hybridization, and polymerase chain reaction (PCR) amplification of viral DNA. These methods enable the identification of EBV-infected cells, confirming the EBV association in Burkitt Lymphoma cases.
Serological Tests for EBV Antibodies in Burkitt Lymphoma Patients
Serological tests can be performed to detect the presence of EBV-specific antibodies in the blood of Burkitt Lymphoma patients. These tests measure the levels of specific antibodies, such as IgM and IgG, against viral proteins, indicating recent or past EBV infection. Serological testing can provide valuable information about the patient’s immune response to EBV and aid in the diagnosis of EBV-associated Burkitt Lymphoma.
Molecular Diagnostics for EBV-Positive Burkitt Lymphoma
Molecular diagnostic techniques, such as quantitative PCR or RNA sequencing, can be used to detect specific viral genes or gene expression patterns in Burkitt Lymphoma samples. These methods can provide valuable information about the viral load, identify viral gene rearrangements, and assess the expression levels of viral oncogenes. Molecular diagnostics play a crucial role in confirming the presence of EBV in Burkitt Lymphoma and guiding treatment decisions.
Treatment Strategies for EBV-Related Burkitt Lymphoma
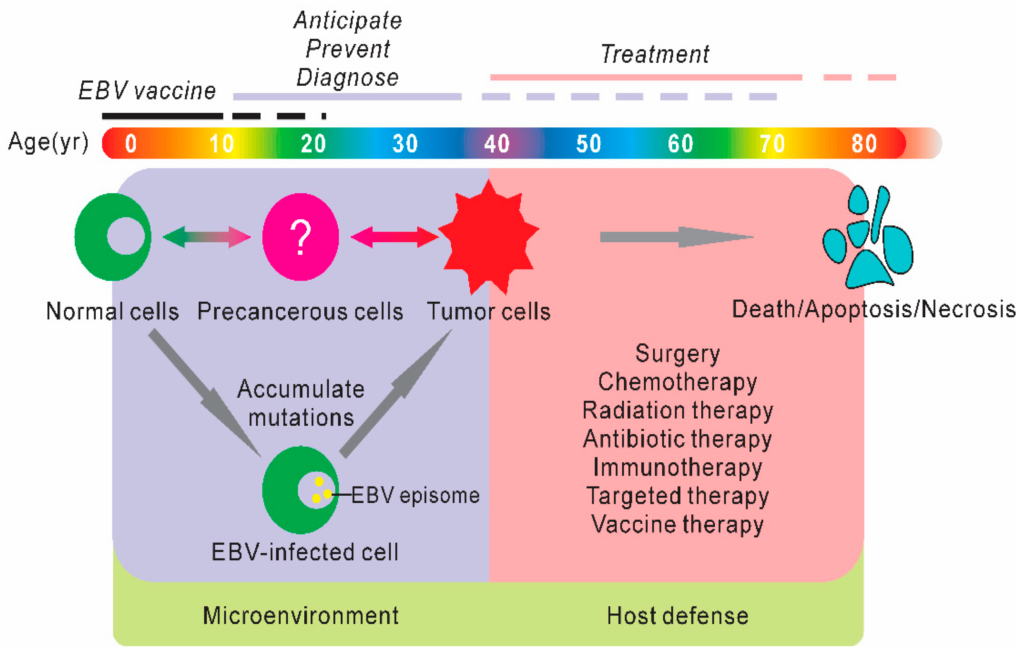
Standard Chemotherapy Protocols for Burkitt Lymphoma
Burkitt Lymphoma is an aggressive cancer that requires intensive treatment. Standard chemotherapy protocols, such as the modified LMB (Lymphomes Malins B) regimen or the CODOX-M/IVAC (Cyclophosphamide, Vincristine, Doxorubicin, and High-Dose Methotrexate/Ifosfamide, Etoposide, and Cytarabine) regimen, are commonly used. These regimens combine multiple chemotherapy drugs to achieve a high cure rate and reduce the risk of relapse.
Role of Anti-EBV Therapies in Burkitt Lymphoma Treatment
Given the association between EBV and Burkitt Lymphoma, anti-EBV therapies have been explored as potential treatment options. These include antiviral drugs, such as acyclovir, ganciclovir, or valganciclovir, which target viral replication. Additionally, novel agents that specifically inhibit viral gene expression or disrupt viral gene interactions with host cells are being investigated. Clinical trials are underway to evaluate the efficacy of these targeted anti-EBV therapies.
Immunotherapy Approaches in Tackling EBV-Associated Burkitt Lymphoma
Immunotherapy has emerged as an exciting area of research in cancer treatment, including Burkitt Lymphoma. Approaches such as chimeric antigen receptor (CAR) T-cell therapy, immune checkpoint inhibitors, and natural killer (NK) cell therapy have shown promise in targeting and eliminating EBV-infected lymphoma cells. These therapies aim to harness the power of the immune system to selectively target cancer cells while sparing normal cells.
Prognostic Factors and Outcomes in EBV-Positive Burkitt Lymphoma
Impact of EBV Infection on Burkitt Lymphoma Prognosis
The presence of EBV in Burkitt Lymphoma has been associated with both favorable and unfavorable prognostic factors. In endemic Burkitt Lymphoma, the presence of EBV is generally associated with a more favorable prognosis compared to non-endemic cases. However, in certain settings, such as immunodeficiency-associated Burkitt Lymphoma or cases with high viral load, the presence of EBV may confer a poorer prognosis.
Survival Rates and Relapse Rates in EBV-Positive Burkitt Lymphoma Cases
The survival rates for EBV-positive Burkitt Lymphoma vary depending on various factors such as tumor stage, age, and treatment response. Overall, the prognosis for Burkitt Lymphoma has improved significantly with modern treatment approaches, with survival rates ranging from 75% to 90%. However, relapse rates remain a challenge, highlighting the need for better risk stratification and targeted therapies.
Factors Influencing Treatment Response and Long-Term Outcomes
Several factors can influence the treatment response and long-term outcomes in EBV-positive Burkitt Lymphoma. These include tumor stage, patient age, genetic abnormalities, and host immune response. Early diagnosis, appropriate risk stratification, and timely initiation of intensive chemotherapy are crucial for maximizing treatment response and improving long-term outcomes.
Emerging Research and Future Directions
Current Advances in Understanding EBV-Burkitt Lymphoma Interplay
There is ongoing research to further understand the complex interplay between EBV and Burkitt Lymphoma. Scientists are unraveling the molecular mechanisms of EBV infection and latency, as well as the specific genetic alterations that occur in Burkitt Lymphoma. Furthermore, advancements in genomic profiling and single-cell analysis techniques are shedding light on the heterogeneity and clonal evolution of EBV-related Burkitt Lymphoma.
Exploration of Targeted Therapies for EBV-Driven Burkitt Lymphoma
Targeted therapies that specifically inhibit viral gene expression or disrupt viral-host interactions are being explored for the treatment of EBV-driven Burkitt Lymphoma. These therapies aim to selectively target viral oncogenes or exploit vulnerabilities in EBV-infected cells. The development of small-molecule inhibitors, RNA interference-based approaches, and proteasome inhibitors is underway to identify novel therapeutic targets.
Potential Strategies for EBV Prevention in Burkitt Lymphoma
Given the strong association between EBV infection and Burkitt Lymphoma, prevention strategies targeting EBV have the potential to reduce the incidence of this aggressive lymphoma. Vaccination against EBV is an area of active research, with efforts focused on developing vaccines that can elicit a robust and protective immune response. As our understanding of the virus improves, novel prevention strategies may emerge.
Conclusion
In summary, Epstein-Barr Virus (EBV) is a ubiquitous virus that can cause various diseases, including Burkitt Lymphoma. The association between EBV and Burkitt Lymphoma is well-established, particularly in endemic areas of Africa. EBV alters the growth and survival of B lymphocytes, playing an oncogenic role in the development of Burkitt Lymphoma. Advances in diagnostic tools, treatment strategies, and targeted therapies offer hope for improving the outcomes of EBV-related Burkitt Lymphoma. Further research is needed to unravel the complexities of the EBV-Burkitt Lymphoma interplay and explore innovative prevention and treatment approaches. The relationship between EBV and Burkitt Lymphoma remains an important area of investigation with significant clinical implications.