In this comprehensive guide, you will learn everything you need to know about impetigo – a common skin infection that affects children. From understanding the causes and symptoms to discovering effective treatment options, this article aims to equip parents and caregivers with valuable insights on how to manage and prevent this contagious condition. With clear explanations and practical advice, you will gain the knowledge necessary to keep your child healthy and recognize the signs of impetigo early on, enabling prompt action and effective treatment.
What is Impetigo?
Impetigo is a common and highly contagious skin infection that primarily affects children, although it can also occur in adults. It is characterized by the development of red sores or blisters that eventually break open, ooze fluid, and form a yellowish-brown crust. The infection is typically caused by bacteria, most commonly Staphylococcus aureus or Streptococcus pyogenes.
Definition
Impetigo is a superficial bacterial skin infection that primarily affects the outer layers of the skin. It is characterized by the formation of sores or blisters that are often accompanied by itching and discomfort. The infection spreads easily through direct contact with infected skin or contaminated objects.
Causes
Impetigo is caused by certain strains of bacteria, particularly Staphylococcus aureus and Streptococcus pyogenes. These bacteria can enter the body through cuts, scratches, or insect bites, leading to the development of impetigo. Poor hygiene practices, crowded living conditions, and warm weather can also contribute to the spread of the infection.
Symptoms
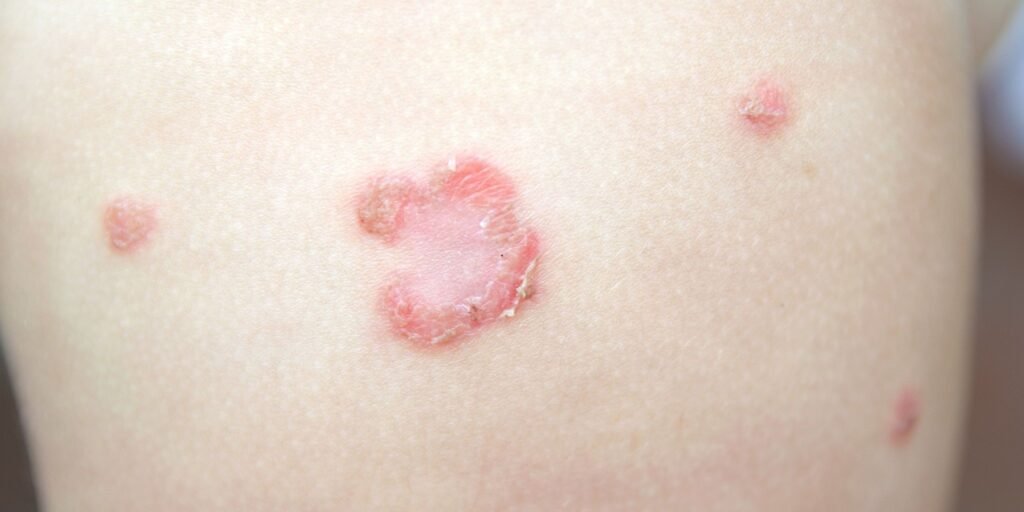
The symptoms of impetigo typically include red sores or blisters that quickly rupture, leaving behind a yellowish-brown crust. These crusts can be itchy and may cause discomfort or mild pain. In some cases, the lymph nodes near the affected area may become swollen.
Types of Impetigo
There are three main types of impetigo: non-bullous impetigo, bullous impetigo, and ecthyma. Each type has its own distinct characteristics and severity.
Non-bullous Impetigo
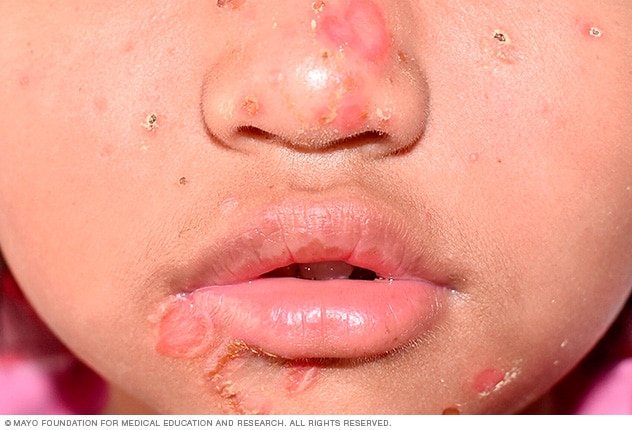
Non-bullous impetigo, also known as impetigo contagiosa, is the most common form of impetigo. It is characterized by small red sores or blisters that quickly burst and form a yellowish-brown crust. These crusts can be easily removed, revealing a red and moist base underneath. Non-bullous impetigo usually starts around the mouth and nose but can spread to other areas of the body through scratching or contact.
Bullous Impetigo
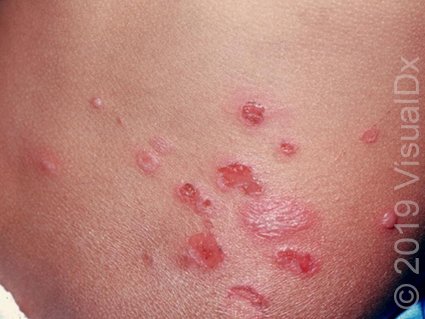
Bullous impetigo is a less common form of impetigo that primarily affects infants and young children. It is characterized by larger fluid-filled blisters that appear clear or yellowish and are surrounded by red skin. The blisters are fragile and easily rupture, leaving behind a thin, shiny crust. Bullous impetigo often develops on the buttocks, thighs, and diaper area.
Ecthyma
Ecthyma is a more severe form of impetigo that affects the deeper layers of the skin. It is characterized by painful ulcers or sores that are covered by a thick and hard crust. Ecthyma can leave behind scars and may take longer to heal compared to other forms of impetigo. It often occurs on the legs or feet and is more common in individuals with weakened immune systems.
Diagnosing Impetigo
To diagnose impetigo, a healthcare provider will typically perform a physical examination and may recommend laboratory tests to confirm the presence of bacteria.
Physical Examination
During a physical examination, the healthcare provider will carefully inspect the affected areas of the skin. They will look for characteristic signs of impetigo, such as red sores or blisters that have ruptured and formed a crust. The provider will also check for any swollen lymph nodes near the affected area.
Laboratory Tests
In some cases, a healthcare provider may collect a sample, such as a swab or scrape, from the affected area for laboratory testing. These tests can help identify the specific bacteria causing the infection and determine the most appropriate treatment.
Treatment Options
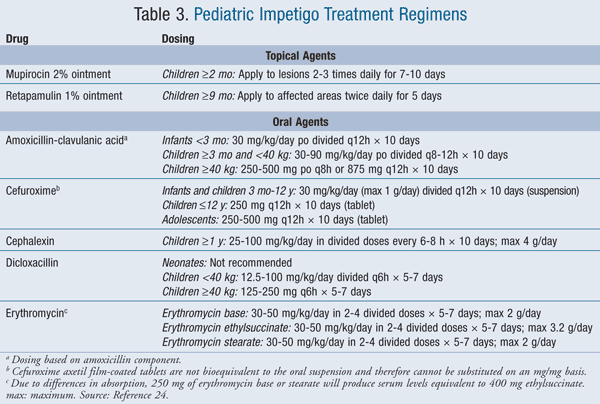
Impetigo can be effectively treated with various treatment options, depending on the severity of the infection. Common treatment options include topical antibiotics, oral antibiotics, and home remedies.
Topical Antibiotics
Topical antibiotics, such as mupirocin or retapamulin ointment, are often the first-line treatment for mild cases of impetigo. These antibiotics help kill the bacteria on the skin and reduce the risk of spreading the infection. It is important to apply the ointment as directed by a healthcare provider and continue treatment for the recommended duration.
Oral Antibiotics
In more severe cases or when the infection has spread to other parts of the body, oral antibiotics may be prescribed. Antibiotics such as penicillin, erythromycin, or cephalexin are commonly used to treat impetigo. It is essential to take the full course of antibiotics even if the symptoms improve to ensure complete eradication of the bacteria.
Home Remedies
While medical treatment is often necessary, certain home remedies can help alleviate symptoms and promote faster healing. These include gently washing the affected area with mild soap and water, applying warm compresses to help remove crusts, and keeping the area clean and dry to prevent further infection. It is important to consult a healthcare provider before trying any home remedies to ensure they are appropriate for the specific case of impetigo.
Preventing the Spread
To prevent the spread of impetigo, it is important to practice good hygiene and take appropriate disinfection measures.
Good Hygiene Practices
Frequent handwashing with soap and water is crucial in preventing the spread of impetigo. Encourage your child to wash their hands regularly, especially before and after touching the affected area. Avoid sharing personal items, such as towels, clothes, or toys, with the infected individual to minimize the risk of spreading the infection.
Disinfection Measures
Disinfecting contaminated objects and surfaces can help prevent the spread of impetigo. Cleanse surfaces that come into contact with the infected person’s skin or any items they have used. Use a disinfectant that is effective against bacteria to ensure proper sanitization.
Caring for a Child with Impetigo
When caring for a child with impetigo, there are several steps you can take to ensure their comfort and aid in the healing process.
Keeping the Affected Area Clean
Gently clean the affected area with mild soap and water to remove any crusts or discharge. Pat the area dry with a clean towel and avoid scrubbing as it can irritate the skin. Follow any specific cleaning instructions provided by the healthcare provider.
Minimizing Discomfort
Impetigo can be itchy and uncomfortable for your child. Apply cool compresses or over-the-counter hydrocortisone cream to soothe the affected area and reduce itching. Ensure your child wears loose-fitting, breathable clothing to prevent further irritation.
Ensuring Medication Adherence
If your child has been prescribed topical or oral antibiotics, make sure they take the medication exactly as directed by the healthcare provider. Prompt and consistent administration of medication is crucial to effectively treat the infection and prevent its spread.

Complications and When to Seek Medical Help
While impetigo is generally a mild infection, certain complications can arise, especially if left untreated.
Possible Complications
If impetigo is not properly treated, it can lead to complications such as cellulitis (a skin infection that spreads to the deeper layers), scarring, or the development of a more severe infection. In rare cases, impetigo can progress to a systemic infection, affecting other parts of the body and potentially causing more serious health issues.
When to Seek Medical Attention
If your child’s symptoms worsen, if they develop a fever, or if the infection spreads or persists despite treatment, it is essential to seek medical attention. Additionally, if your child has any underlying medical conditions that may weaken their immune system, it is advisable to consult a healthcare provider promptly.
Impetigo and School
Impetigo can pose certain challenges when it comes to a child’s attendance at school. Understanding school policies and implementing necessary precautions can help manage the situation effectively.
School Policies and Recommendations
Each school may have specific policies in place regarding attending school with impetigo. It is important to notify the school administration and follow their guidelines for preventing the spread of the infection. These policies may include exclusion from school until treatment is completed, maintaining good hygiene practices, and providing necessary documentation from a healthcare provider.
Returning to School
Once your child has completed the treatment and their symptoms have resolved, it is generally safe for them to return to school. Ensure that the affected areas are completely healed, crust-free, and no longer oozing fluid. It is a good idea to consult the school administration to confirm their specific requirements for the child’s return.
Frequently Asked Questions
Here are some commonly asked questions about impetigo:
Is impetigo contagious?
Yes, impetigo is highly contagious. It can easily spread through direct contact with infected skin or contaminated objects. It is important to practice good hygiene and take necessary precautions to prevent the spread of the infection.
Can impetigo be prevented?
While it may not be possible to completely prevent impetigo, certain measures can help reduce the risk. Practicing good hygiene, including regular handwashing and avoiding close contact with infected individuals or their personal belongings, can minimize the chances of contracting the infection.
Can impetigo recur?
Yes, impetigo can recur, especially in individuals with weakened immune systems or in settings where there may be ongoing exposure to the bacteria causing the infection. Taking appropriate preventive measures and maintaining good hygiene practices can help reduce the risk of recurrence.
Is impetigo dangerous?
In general, impetigo is not considered dangerous and can be effectively treated with appropriate medical care. However, complications can arise if the infection is left untreated or if it spreads to deeper layers of the skin. Prompt medical attention and adherence to treatment guidelines are essential to prevent complications.
Can impetigo affect adults?
While impetigo primarily affects children, it can also occur in adults. Adults with conditions that weaken the immune system, such as diabetes or HIV, may be more susceptible to developing impetigo. Similar preventive measures and treatment options apply to both children and adults.
Conclusion
Impetigo is a common and contagious skin infection that primarily affects children. It is important to recognize the signs and symptoms of impetigo and seek medical attention for proper diagnosis and treatment. By following good hygiene practices, adhering to treatment guidelines, and implementing preventive measures, the spread of impetigo can be minimized. With proper care and timely intervention, most cases of impetigo can be effectively managed, providing relief and promoting faster healing for the affected individuals.