Have you ever heard of Legionnaires’ Disease? It is a respiratory illness caused by the bacteria Legionella. If you haven’t come across it before, don’t worry! In this article, we will explore the symptoms and treatment options for Legionnaires’ Disease, ensuring you have the knowledge to recognize and address it if ever encountered. So, let’s get started!
Symptoms of Legionnaires’ Disease
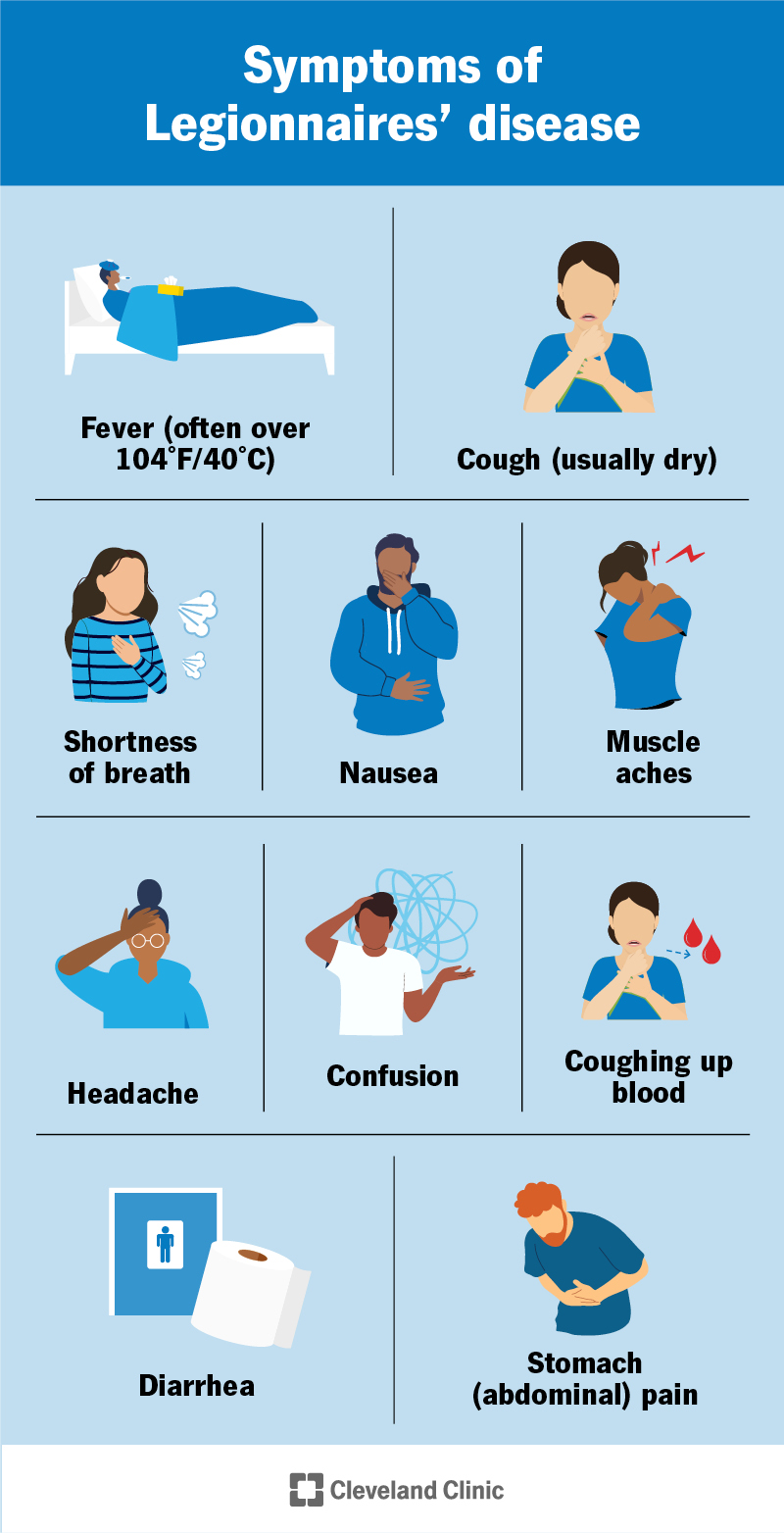
Legionnaires’ Disease is a severe form of pneumonia caused by the Legionella bacteria. Recognizing the symptoms is crucial for early diagnosis and prompt treatment. Here are the key symptoms to watch out for:
Fever
One of the primary symptoms of Legionnaires’ Disease is a high fever. This fever can often be accompanied by chills and shivering, which can make you feel extremely uncomfortable. It is important to monitor your body temperature and seek medical attention if you experience a persistent fever.
Cough
A persistent cough is also a common symptom of Legionnaires’ Disease. It may start as a dry cough but can progress to producing phlegm or mucus. If you find yourself coughing excessively and the symptoms do not subside, it is advisable to consult a healthcare professional.
Shortness of Breath
Shortness of breath, or difficulty in breathing, is another symptom that could indicate Legionnaires’ Disease. This occurs due to the inflammation in the lungs caused by the infection. If you experience breathlessness or a rapid increase in your breathing rate, it is crucial to seek medical attention immediately.
Muscle aches
Legionnaires’ Disease can cause intense muscle pain and discomfort. You may feel soreness or stiffness in various parts of your body, which can make even simple movements challenging. Pay attention to these muscle aches, especially when combined with other symptoms, as it may indicate a more serious underlying condition.
Headaches
Headaches are a common symptom of many illnesses, but they can also occur in individuals with Legionnaires’ Disease. These headaches can range from mild to severe and can be accompanied by additional symptoms such as fever and muscle aches. It is important to communicate any persistent or severe headaches to your healthcare provider.
Gastrointestinal symptoms
In some cases, Legionnaires’ Disease can manifest with gastrointestinal symptoms such as diarrhea, nausea, vomiting, and abdominal pain. These symptoms can be easily mistaken for a stomach bug, but if you have been exposed to contaminated water sources or have other symptoms of Legionnaires’ Disease, it is crucial to discuss these gastrointestinal symptoms with your healthcare provider.
Confusion or cognitive changes
Legionnaires’ Disease can affect the central nervous system, leading to confusion, disorientation, and cognitive changes. These symptoms can be particularly concerning, as they may interfere with daily functioning and require immediate medical attention. Do not hesitate to seek help if you or someone you know experiences confusion or cognitive changes along with other symptoms of Legionnaires’ Disease.
Loss of appetite
A loss of appetite is another potential symptom of Legionnaires’ Disease. You may experience a decreased desire to eat and a general lack of interest in food. While this symptom on its own may not be indicative of the disease, it becomes more significant when combined with other symptoms such as fever, cough, and muscle aches.
Sore throat
Although a sore throat is a common symptom of many respiratory infections, it can also be present in cases of Legionnaires’ Disease. The throat may feel dry, scratchy, or painful, making it uncomfortable to swallow or talk. If your sore throat persists or worsens, consult your healthcare provider for further evaluation.
Chest pain
Chest pain is a symptom that should not be ignored, as it can be a sign of a serious condition such as Legionnaires’ Disease. The inflammation in the lungs caused by the infection can lead to chest discomfort or pain, especially when taking deep breaths or coughing. If you experience chest pain along with other symptoms, seek immediate medical attention.
Diagnosis of Legionnaires’ Disease
Prompt and accurate diagnosis of Legionnaires’ Disease is crucial for initiating appropriate treatment. The following diagnostic methods are commonly used:
Physical examination
During a physical examination, your healthcare provider will assess your symptoms, perform a thorough examination of your lungs and respiratory system, check your vital signs, and inquire about your medical history and recent activities. This initial assessment helps in determining the likelihood of Legionnaires’ Disease and guides further diagnostic tests.
Chest X-rays
Chest X-rays are often the first imaging test done to evaluate lung involvement in Legionnaires’ Disease. These images help identify any abnormalities or infiltrates in the lungs, such as areas of consolidation or fluid accumulation. Chest X-rays can help confirm the diagnosis and monitor the progression of the disease during treatment.
Laboratory tests
Laboratory tests play a crucial role in diagnosing Legionnaires’ Disease. Blood tests, such as a complete blood count (CBC) and blood cultures, are performed to analyze the presence of infection and evaluate the overall immune response. Elevated levels of inflammatory markers in the blood can provide important clues for diagnosis.
Urinary antigen test
The urinary antigen test is a rapid and reliable diagnostic tool for Legionnaires’ Disease. This test detects a specific antigen, called Legionella pneumophila serogroup 1, in a urine sample. A positive result confirms the presence of Legionella bacteria and aids in making an accurate diagnosis.
Sputum culture
A sputum culture may be performed to isolate and identify the Legionella bacteria. This involves collecting a deep coughed sputum sample and sending it to the laboratory for analysis. While this culture may take longer for results, it can help identify the specific strain of Legionella bacteria causing the infection.
Blood tests
Blood tests, such as serology tests, may be conducted to detect specific antibodies produced in response to Legionella infection. These tests measure the levels of antibodies, such as Immunoglobulin M (IgM) and Immunoglobulin G (IgG), which can aid in confirming the diagnosis of Legionnaires’ Disease.
Legionella culture
A Legionella culture involves collecting samples from potentially contaminated water sources, such as cooling towers or hot water systems, and testing them in a laboratory to isolate and identify the Legionella bacteria. This helps in identifying the source of the infection and preventing further spread.

Risk Factors for Legionnaires’ Disease
Certain factors can increase the risk of contracting Legionnaires’ Disease. While everyone is vulnerable, some individuals are more susceptible to severe infections due to the following risk factors:
Age
Advanced age is a significant risk factor for Legionnaires’ Disease. Older adults, especially those over the age of 50, are more likely to experience severe symptoms and complications. Age-related changes in the immune system can make individuals less able to fight off infections effectively, making them more susceptible to severe forms of the disease.
Smoking
Smoking weakens the immune system and damages the respiratory system, making smokers more susceptible to respiratory infections, including Legionnaires’ Disease. The harmful chemicals in tobacco smoke impair the cilia in the respiratory tract, reducing their ability to clear pathogens and increasing the risk of infection.
Weak immune system
Individuals with weakened immune systems, such as those with HIV/AIDS, organ transplant recipients, or individuals undergoing chemotherapy, are at an increased risk of developing severe Legionnaires’ Disease. When the immune system is compromised, it becomes less effective in fighting off infections, making these individuals more susceptible to severe complications.
Chronic lung diseases
Chronic lung diseases, such as chronic obstructive pulmonary disease (COPD) and asthma, can weaken the respiratory system and compromise lung function. This impaired lung function makes individuals with these conditions more susceptible to respiratory infections, including Legionnaires’ Disease. Proper management of these underlying lung conditions is essential in reducing the risk.
Underlying medical conditions
Certain medical conditions, such as diabetes, kidney disease, and liver disease, can weaken the immune system and impair overall health. Individuals with these underlying medical conditions may be more prone to infections, including Legionnaires’ Disease. It is important for individuals with these conditions to take appropriate precautions and seek medical attention promptly if they experience symptoms.
Recent hospital stay
Patients who have recently been hospitalized or have received intensive care are at an increased risk of developing healthcare-associated Legionnaires’ Disease. Healthcare facilities can be a breeding ground for Legionella bacteria if water systems are not properly maintained. If you have recently been hospitalized, be vigilant about any signs or symptoms of infection and report them to your healthcare provider immediately.
Exposure to contaminated water sources
Exposure to contaminated water sources, such as hot tubs, cooling towers, or large plumbing systems, increases the risk of Legionnaires’ Disease. Legionella bacteria thrive in warm water environments and can be inhaled in aerosolized droplets. Activities involving exposure to water sources, especially in buildings with inadequate water system maintenance, can pose a higher risk of infection.
Prevention of Legionnaires’ Disease
Taking preventive measures is crucial in reducing the risk of Legionnaires’ Disease. By following these precautionary steps, you can protect yourself and others from this potentially severe infection:
Regular maintenance of water systems
Proper maintenance of water systems is essential in preventing the growth and spread of Legionella bacteria. Regular cleaning, disinfection, and monitoring of cooling towers, hot tubs, showers, faucets, and other plumbing systems can help minimize the risk of contamination.
Proper disinfection
Using appropriate disinfection methods, such as chlorine or other approved disinfectants, is important in killing and preventing the growth of Legionella bacteria in water systems. Following recommended disinfection protocols and ensuring that disinfectants are used correctly can significantly reduce the risk of Legionnaires’ Disease.
Monitoring water quality
Regularly monitoring the quality of water in buildings, especially those with larger water systems, can help identify potential sources of Legionella contamination. Routine testing of water samples and maintaining appropriate water quality standards are crucial in preventing the proliferation of bacteria and reducing the risk of infection.
Water temperature management
Maintaining optimal water temperatures can help prevent the growth of Legionella bacteria. Following specific guidelines for hot water systems, such as maintaining water temperatures above 140°F (60°C) and ensuring safe and consistent flow rates, can significantly reduce the risk of Legionnaires’ Disease.
Use of water filters
Installing point-of-use filters, such as showerhead filters or faucet filters, can serve as an additional layer of protection against the inhalation of Legionella bacteria in aerosolized water droplets. These filters can help remove or reduce the presence of bacteria and other potential pathogens, minimizing the risk of infection.

Treatment for Legionnaires’ Disease
Timely and appropriate treatment is vital for individuals diagnosed with Legionnaires’ Disease. The following treatment strategies are commonly employed:
Hospitalization
Hospitalization is often required for individuals with Legionnaires’ Disease, especially those with severe symptoms or complications. In a hospital setting, close monitoring and specialized care can be provided to ensure the best possible outcomes. The severity of the infection, underlying health conditions, and individual patient factors will determine the duration of hospitalization.
Antibiotic therapy
Antibiotics, such as fluoroquinolones or macrolides, are the mainstay of treatment for Legionnaires’ Disease. These medications are effective in targeting the Legionella bacteria and helping to eradicate the infection. The choice of antibiotics and the duration of treatment will depend on the severity of the disease, the specific strain of Legionella bacteria, and individual patient factors.
Supportive care
Supportive care measures are essential in managing the symptoms and promoting recovery in individuals with Legionnaires’ Disease. These measures may include adequate hydration, pain management, and fever-reducing medications. Supportive care aims to alleviate discomfort and improve overall well-being during the recovery process.
Management of complications
In severe cases of Legionnaires’ Disease, complications can arise that require additional management. For example, if respiratory failure occurs due to severe lung involvement, respiratory support measures such as oxygen therapy or mechanical ventilation may be necessary. Other complications, such as kidney failure or septic shock, require specific interventions tailored to the individual’s condition.
Respiratory support
Severe cases of Legionnaires’ Disease may require respiratory support to ensure adequate oxygenation and ventilation. Oxygen therapy, delivered via nasal prongs or a face mask, can help improve breathing and alleviate respiratory distress. In more critical cases, mechanical ventilation may be necessary to assist with breathing until the infection is under control.
Prognosis and Complications of Legionnaires’ Disease
Prognosis
With appropriate and timely treatment, the prognosis for most individuals with Legionnaires’ Disease is generally favorable. However, the prognosis can vary depending on various factors, such as the severity of the infection, the presence of underlying medical conditions, and the promptness of treatment initiation. Early diagnosis and prompt administration of antibiotics significantly improve the chances of a full recovery.
Complications
Legionnaires’ Disease can lead to serious complications, especially in individuals with weakened immune systems or pre-existing health conditions. Potential complications may include respiratory failure, kidney failure, septic shock, or other multiorgan dysfunction. Prompt diagnosis, early initiation of treatment, and appropriate management of complications are crucial in minimizing the risk of severe outcomes.

Outbreaks of Legionnaires’ Disease
Common locations for outbreaks
Legionnaires’ Disease outbreaks can occur in various settings where Legionella bacteria can thrive and be disseminated in aerosolized water droplets. Common locations for outbreaks include hotels, large office buildings, hospitals, nursing homes, cruise ships, and recreational facilities with hot tubs or water cooling systems. These settings often have larger water systems that require regular monitoring and maintenance.
Investigation and control measures
In the event of a Legionnaires’ Disease outbreak, prompt investigation and control measures are essential for containing the spread of infection. Public health authorities work closely with healthcare providers, facility managers, and water management experts to identify the source of the contamination, implement appropriate control measures, and ensure the safety of the affected population.
History of Legionnaires’ Disease
First identified outbreak
Legionnaires’ Disease gained public attention following a significant outbreak in July 1976 during an American Legion convention in Philadelphia. Over 200 people fell ill, with 34 deaths attributed to the disease. This outbreak led to an extensive investigation by epidemiologists, ultimately leading to the discovery of the Legionella bacteria as the causative agent of the disease.
Discovery of Legionella bacteria
Shortly after the outbreak, researchers successfully isolated and identified the Legionella bacteria responsible for causing the severe respiratory illness. The bacterium was subsequently named Legionella pneumophila. Since then, numerous species and serogroups of Legionella have been identified, highlighting the diverse nature of this group of bacteria and their potential to cause severe illnesses.

Comparison with Other Similar Diseases
Legionnaires’ disease vs. Pontiac fever
Legionnaires’ Disease and Pontiac fever are both caused by the Legionella bacteria but differ in terms of severity and symptoms. Pontiac fever is a milder illness that manifests with flu-like symptoms such as fever, muscle aches, and headaches. Unlike Legionnaires’ Disease, Pontiac fever does not involve pneumonia or respiratory complications and typically resolves without specific treatment.
Legionnaires’ disease vs. Pneumonia
Pneumonia is a broader term referring to inflammation and infection in the lungs caused by various pathogens, including bacteria, viruses, and fungi. Legionnaires’ Disease is a specific form of pneumonia caused by the Legionella bacteria. While both can present with similar symptoms, Legionnaires’ Disease often has more severe symptoms and can lead to complications if left untreated.
Legionnaires’ disease vs. Tuberculosis
Legionnaires’ Disease and tuberculosis (TB) are both respiratory infections but are caused by different pathogens. Legionnaires’ Disease is caused by the Legionella bacteria, while TB is caused by Mycobacterium tuberculosis. TB can affect various organs, including the lungs, kidneys, and bones. Legionnaires’ Disease primarily affects the lungs and can cause severe pneumonia.
Conclusion
Legionnaires’ Disease is a severe respiratory infection that can lead to pneumonia and potentially life-threatening complications. Recognizing the symptoms, such as fever, cough, shortness of breath, and muscle aches, is crucial for timely diagnosis and treatment. Various diagnostic methods, including physical examinations, chest X-rays, and laboratory tests, aid in confirming the diagnosis. Individuals with certain risk factors, such as advanced age, smoking, weak immune systems, and exposure to contaminated water sources, are more susceptible to the disease. Preventive measures, including regular maintenance of water systems, proper disinfection, and monitoring water quality, can help reduce the risk of infection. Treatment of Legionnaires’ Disease often involves hospitalization, antibiotic therapy, supportive care, and management of complications. With prompt treatment, the prognosis for most individuals is favorable. However, it is essential to be aware of potential complications and seek medical attention if symptoms worsen or new symptoms appear. By understanding the symptoms, risk factors, and preventive measures, individuals can protect themselves and others from this potentially severe respiratory infection.