Living with Diabetes Mellitus can be a challenging yet manageable journey. From monitoring your blood sugar levels to making conscious decisions about your diet and exercise routine, there are various aspects to consider when living with this chronic condition. However, with the right knowledge and support, you can lead a fulfilling life while effectively managing your diabetes. In this article, we will explore the key strategies and lifestyle changes that can empower you to take control of your health and thrive despite the challenges that come with Diabetes Mellitus.

Understanding Diabetes Mellitus
Diabetes Mellitus is a chronic condition characterized by high levels of glucose in the blood. It occurs when the body either doesn’t produce enough insulin or cannot effectively use the insulin it does produce. Insulin is a hormone that regulates the amount of glucose in the bloodstream.
Definition of Diabetes Mellitus
Diabetes Mellitus is a metabolic disorder that impairs the body’s ability to properly regulate blood sugar levels. There are two main types of diabetes: Type 1 diabetes and Type 2 diabetes. In Type 1 diabetes, the body does not produce enough insulin, while in Type 2 diabetes, the body does not efficiently use the insulin it produces.
Types of Diabetes
Type 1 diabetes is an autoimmune disease where the immune system mistakenly attacks and destroys the insulin-producing cells in the pancreas. This form of diabetes typically develops during childhood or adolescence. Type 2 diabetes, on the other hand, is more common and is often associated with lifestyle factors such as obesity and physical inactivity.
Causes of Diabetes Mellitus
The exact causes of diabetes vary depending on the type. Type 1 diabetes is believed to be caused by a combination of genetic and environmental factors, including certain viral infections. Type 2 diabetes is primarily influenced by lifestyle factors such as poor diet, lack of exercise, and being overweight or obese. Other risk factors include age, family history, and certain medical conditions.
Symptoms of Diabetes Mellitus
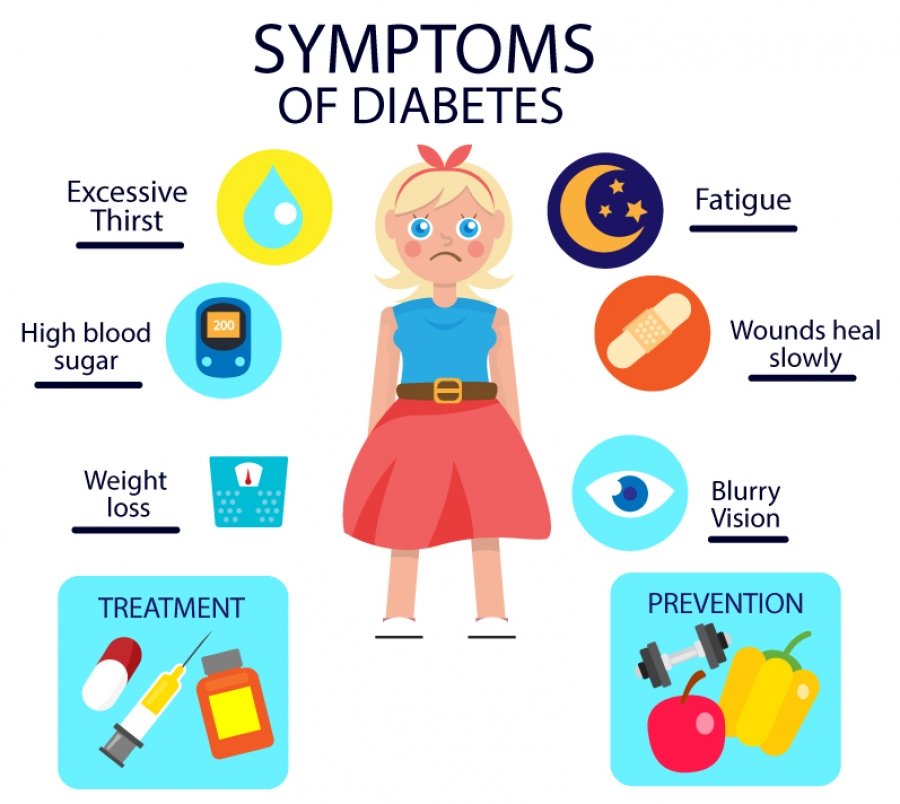
Some common symptoms of diabetes mellitus include frequent urination, increased thirst, unexplained weight loss, fatigue, blurred vision, slow-healing wounds, and recurring infections. These symptoms may vary in intensity and may not always be present in individuals with diabetes. If you experience any of these symptoms, it is important to consult a healthcare professional for further evaluation.
Diagnosing Diabetes Mellitus
Early diagnosis is crucial in managing diabetes effectively. Several tests are available to diagnose diabetes mellitus and determine the type of diabetes a person has.
Routine Blood Tests
Routine blood tests, including a fasting blood glucose test, are often used as a screening tool for diabetes. If the results indicate high blood sugar levels, further testing is typically done to confirm the diagnosis.
Glycated Hemoglobin (A1C) Test
The A1C test measures the average blood glucose levels over the past two to three months. It provides a snapshot of how well blood sugar levels have been controlled over time. An A1C level of 6.5% or higher is generally indicative of diabetes.
Fasting Plasma Glucose (FPG) Test
The FPG test measures blood glucose levels after an overnight fast. A normal fasting glucose level is below 100 mg/dL, while levels between 100-125 mg/dL may be indicative of prediabetes, and levels of 126 mg/dL or higher may indicate diabetes.
Oral Glucose Tolerance Test (OGTT)
During an OGTT, blood glucose levels are measured before and two hours after consuming a sugary drink. This test is primarily used to diagnose gestational diabetes in pregnant women but is also occasionally used to diagnose Type 2 diabetes.

Diabetes Treatment Options
While there is currently no cure for diabetes, there are various treatment options available to help manage the condition and control blood sugar levels.
Lifestyle Changes
Implementing lifestyle changes is a fundamental aspect of diabetes management. This includes adopting a healthy diet, engaging in regular physical activity, managing stress, getting enough sleep, and avoiding unhealthy habits such as smoking and excessive alcohol consumption.
Dietary Modifications
Following a balanced and nutritious diet is essential for individuals with diabetes. This involves monitoring carbohydrate intake, choosing foods with a low glycemic index, and incorporating plenty of fruits, vegetables, whole grains, lean proteins, and healthy fats into your diet.
Exercise and Physical Activity
Regular physical activity can help improve insulin sensitivity and lower blood sugar levels. Aim for at least 150 minutes of moderate-intensity aerobic exercise per week, along with strength training exercises two to three times a week.
Oral Medications
For individuals with Type 2 diabetes, oral medications may be prescribed to help manage blood sugar levels. These medications work by reducing insulin resistance, increasing insulin production, or slowing down the absorption of glucose from the digestive tract.
Insulin Therapy
In some cases, insulin therapy may be necessary for individuals with Type 1 diabetes and for those with Type 2 diabetes who cannot achieve adequate blood sugar control with oral medications alone. Insulin can be administered through injections or the use of an insulin pump.
Alternative Therapies
Some individuals with diabetes may seek alternative therapies to complement their conventional treatment plan. These may include herbal supplements, acupuncture, yoga, and other holistic approaches. It is important to discuss these options with a healthcare professional before incorporating them into your diabetes management strategy.
Monitoring Blood Sugar Levels
Regular and accurate monitoring of blood sugar levels is crucial for effectively managing diabetes. There are various tools and techniques available for monitoring blood sugar levels at home.
The Importance of Blood Sugar Monitoring
Monitoring blood sugar levels helps individuals with diabetes understand how their lifestyle choices, medication, and other factors impact their blood glucose levels. By keeping track of these levels, individuals can make informed decisions about their diet, medication, and physical activity to achieve optimal blood sugar control.
Blood Glucose Meters
Blood glucose meters are portable devices that measure blood sugar levels from a tiny sample of blood obtained by pricking the fingertip. These meters provide immediate results and are a common tool for self-monitoring blood sugar levels.
Continuous Glucose Monitoring (CGM) Systems
CGM systems use a small sensor inserted under the skin to continuously measure glucose levels in the interstitial fluid. These systems provide real-time glucose readings and can alert individuals to high or low blood sugar levels. CGM systems are especially helpful for individuals who experience significant fluctuations in their blood sugar levels.
Interpreting Blood Sugar Readings
Understanding blood sugar readings is important for making appropriate adjustments to diet, medication, and physical activity. Target blood sugar ranges may vary depending on factors such as age, overall health, and individual treatment goals.
Managing High and Low Blood Sugar Levels
If blood sugar levels are consistently high, adjustments may need to be made to the treatment plan. This can involve medication changes, dietary modifications, or consultation with a healthcare provider. Conversely, if blood sugar levels are frequently low, raising blood sugar with fast-acting carbohydrates such as fruit juice or glucose tablets may be necessary.

Managing a Diabetic Diet
A healthy and well-balanced diet is a cornerstone of diabetes management. The following strategies can help individuals with diabetes manage their diet effectively.
Carbohydrate Counting
Carbohydrate counting involves monitoring the amount of carbohydrates consumed in a meal and matching it with the appropriate insulin dose. This strategy allows for better blood sugar control and flexibility in food choices.
Glycemic Index and Load
The glycemic index measures how quickly carbohydrates in food raise blood sugar levels. Foods with a low glycemic index cause a slower and steadier increase in blood sugar, while foods with a high glycemic index cause a rapid spike in blood sugar. The glycemic load takes into account both the glycemic index and the quantity of carbohydrates in a food serving.
Balancing Macronutrients
Aim to include a balance of carbohydrates, proteins, and fats in each meal. This balance helps regulate blood sugar levels, provides essential nutrients, and promotes overall health.
Meal Planning Strategies
Meal planning is beneficial for individuals with diabetes as it enables them to make healthier food choices, control portion sizes, and maintain more consistent blood sugar levels. Strategies such as batch cooking, pre-portioning meals, and incorporating a variety of nutritious foods can simplify the meal planning process.
Snacking Tips
Snacking can be part of a healthy diet for individuals with diabetes if done mindfully. Opt for snacks that combine carbohydrates with protein or healthy fats to help stabilize blood sugar levels. Examples include apple slices with nut butter, yogurt with berries, or raw vegetables with hummus.
Eating Out with Diabetes
Eating out can pose challenges for individuals with diabetes, but with proper planning and awareness, it is still possible to enjoy restaurant meals while maintaining blood sugar control. It is helpful to review the menu in advance, choose balanced meal options, request modifications, and be mindful of portion sizes.
Engaging in Regular Physical Activity
Regular physical activity plays a crucial role in diabetes management. It helps improve insulin sensitivity, aids in weight management, reduces the risk of cardiovascular complications, and promotes overall well-being.
Benefits of Exercise for Diabetes Management
Exercise offers numerous benefits for individuals with diabetes, including improved insulin sensitivity, better blood sugar control, weight management, reduced risk of heart disease, increased energy levels, improved sleep quality, and enhanced mood.
Recommended Types of Exercise
Both aerobic exercises (such as walking, jogging, swimming, or cycling) and strength training exercises are important for individuals with diabetes. Aim for a combination of aerobic and strength training activities to reap the full range of benefits.
Setting Realistic Exercise Goals
Setting realistic exercise goals is essential to ensure long-term adherence and prevent burnout or injury. Start with small achievable goals and gradually increase the intensity, duration, and frequency of exercise as fitness improves.
Creating an Exercise Routine
Establishing a consistent exercise routine is key to making physical activity a habit. Schedule exercise at a convenient time, choose activities that are enjoyable, and find an exercise buddy or join a group exercise class for added motivation and accountability.
Preventing and Treating Exercise-Related Hypoglycemia
Exercise can sometimes cause blood sugar levels to drop too low, resulting in hypoglycemia. To prevent hypoglycemia, it is important to monitor blood sugar levels before, during, and after exercise. Consuming a carbohydrate-containing snack or adjusting medication doses may be necessary to maintain blood sugar stability.

Managing Stress and Mental Health
Stress and diabetes can influence each other, as stress hormones can raise blood sugar levels and make diabetes management more challenging. Taking steps to manage stress and prioritize mental health is essential in effectively managing diabetes.
Understanding the Connection between Stress and Diabetes
Chronic stress can have a negative impact on blood sugar control as it triggers the release of hormones that can raise blood sugar levels. Additionally, managing diabetes itself can be a significant source of stress, creating a cyclical relationship between stress and diabetes management.
Stress Management Techniques
Incorporating stress management techniques into your daily routine can help reduce stress levels. These may include deep breathing exercises, meditation, yoga, regular physical activity, engaging in hobbies and activities you enjoy, and seeking support from friends, family, or professionals.
Improving Sleep Quality
Adequate sleep is important for overall health and diabetes management. Poor sleep can contribute to insulin resistance and higher blood sugar levels. Prioritizing good sleep habits, creating a relaxing bedtime routine, and addressing any sleep disorders can help improve sleep quality.
Coping with Diabetes-Related Emotional Challenges
Dealing with a chronic condition like diabetes can sometimes be mentally challenging. It is normal to experience a range of emotions, including frustration, anxiety, and stress. Finding healthy outlets for these emotions, such as talking to loved ones, joining support groups, or seeking professional counseling, can be beneficial.
Seeking Professional Support
If you are struggling with diabetes management or experiencing emotional difficulties related to your condition, it is important to seek support from healthcare professionals specializing in diabetes care or mental health. They can provide guidance, support, and resources to help you effectively manage your condition and maintain emotional well-being.
Dealing with Diabetes-Related Complications
Living with diabetes increases the risk of developing certain complications over time. Proactive management and regular monitoring can help reduce the risk and severity of these complications.
Long-Term Complications
Uncontrolled diabetes can lead to long-term complications affecting various organ systems, including the heart, kidneys, eyes, nerves, and skin. These complications can include cardiovascular disease, diabetic nephropathy, diabetic retinopathy, neuropathy, and skin infections or conditions.
Foot Problems and Care
Diabetes can cause nerve damage (neuropathy) and poor blood circulation, increasing the risk of foot problems. Regular foot care, such as daily foot inspections, wearing proper footwear, and seeking prompt medical attention for any foot issues, is essential to prevent complications.
Cardiovascular Health
Diabetes is a major risk factor for cardiovascular disease. Managing blood pressure and cholesterol levels, adopting a heart-healthy diet, engaging in regular physical activity, avoiding tobacco use, and taking prescribed medications as directed can help reduce the risk of cardiovascular complications.
Kidney Health
Diabetic nephropathy, also known as diabetic kidney disease, is a common complication of diabetes. Managing blood pressure and blood sugar levels, maintaining a healthy diet, and avoiding excessive protein intake can help promote kidney health and delay the progression of kidney disease.
Eye Health
Diabetic retinopathy is a condition that affects the blood vessels in the retina, potentially leading to vision loss. Regular eye examinations, strict blood sugar control, blood pressure management, and early intervention can help prevent or minimize the impact of diabetic retinopathy.
Dental Health
Diabetes can increase the risk of gum disease, tooth decay, and other oral health issues. Maintaining good oral hygiene habits, visiting the dentist regularly, and controlling blood sugar levels can help prevent dental complications.
Neuropathy
Diabetic neuropathy is a type of nerve damage that can cause pain, numbness, and tingling in the extremities. Achieving and maintaining stable blood sugar levels, managing any existing pain or discomfort, practicing good foot care, and seeking medical treatment as needed are key to managing diabetic neuropathy.
Skin Conditions
Diabetes can make individuals more susceptible to various skin conditions, including fungal infections, bacterial infections, and dry skin. Proper hygiene, regular moisturizing, prompt treatment of any skin issues, and maintaining good blood sugar control can help prevent and manage these conditions.
Educating Oneself and Seeking Support
Education and support play crucial roles in effective diabetes management. By empowering yourself with knowledge and seeking support, you can make informed decisions, adhere to treatment plans, and live a fulfilling life with diabetes.
Importance of Diabetes Education
Diabetes education equips individuals with the knowledge and skills necessary to effectively manage their condition. It covers topics such as self-care, medication management, blood sugar monitoring, healthy lifestyle habits, and prevention of complications.
Finding Reliable Information
With the abundance of information available online, it is important to seek reliable sources when learning about diabetes. Trusted sources such as reputable healthcare websites, diabetes associations, and healthcare professionals can provide accurate and up-to-date information.
Support Groups and Online Communities
Joining support groups, either in-person or online, can provide a sense of community and understanding. These groups offer a space to share experiences, gain support, exchange practical tips, and learn from others who are living with diabetes.
Working with Healthcare Professionals
Your healthcare team, which may include doctors, nurses, dietitians, and diabetes educators, plays a vital role in your diabetes management. Regular check-ups, open communication, and collaboration are essential for developing and adjusting your treatment plan.
Involving Family and Friends
Family and friends can offer valuable support in managing diabetes. By involving them in your journey, educating them about the condition, and communicating your needs, you can build a strong support system and ensure a better understanding of your unique challenges and goals.
Promoting Diabetes Prevention
While Type 1 diabetes cannot be prevented, the development of Type 2 diabetes, which is the most common form, can often be prevented or delayed by adopting a healthy lifestyle and reducing specific risk factors.
Understanding Type 2 Diabetes Prevention
Type 2 diabetes prevention involves making healthy choices regarding diet, physical activity, weight management, and overall lifestyle. By addressing modifiable risk factors, individuals can significantly reduce their risk of developing Type 2 diabetes.
Risk Factors for Type 2 Diabetes
Several factors increase the risk of developing Type 2 diabetes, including being overweight or obese, living a sedentary lifestyle, having a family history of diabetes, being over 45 years of age, having high blood pressure or high cholesterol, and certain ethnic backgrounds such as African, Hispanic, or Asian descent.
Adopting a Healthy Lifestyle
Adopting a healthy lifestyle is a key component in preventing Type 2 diabetes. This includes maintaining a balanced diet, engaging in regular physical activity, achieving and maintaining a healthy weight, avoiding tobacco use, limiting alcohol intake, and managing stress.
Regular Medical Check-ups
Regular medical check-ups are important for early detection and prevention of diabetes. These check-ups may include routine blood tests, blood pressure measurements, cholesterol checks, and monitoring of other risk factors.
Community Initiatives for Diabetes Prevention
Many community initiatives focus on raising awareness about diabetes prevention and providing resources to individuals at risk. These initiatives may include educational workshops, free health screenings, access to fitness programs, and community-based support groups.
By understanding diabetes, implementing lifestyle changes, effectively monitoring blood sugar levels, managing diet and physical activity, prioritizing mental health, addressing complications, seeking education and support, and promoting prevention efforts, individuals can lead fulfilling lives while effectively managing diabetes mellitus. Remember, with proper management and support, diabetes does not have to define you or limit your potential for a healthy and vibrant life.
