Imagine having a chronic condition that affects every aspect of your daily life. That’s what living with Diabetes Mellitus is like. In this article, we will explore the ins and outs of this common disease, shedding light on its causes, symptoms, and management strategies. Whether you are personally affected by this condition or want to gain a deeper understanding, this informative piece will empower you to navigate the intricate world of Diabetes Mellitus. So let’s embark on this journey together and unravel the mysteries of this prevalent ailment.
Overview of Diabetes Mellitus
Introduction to Diabetes Mellitus
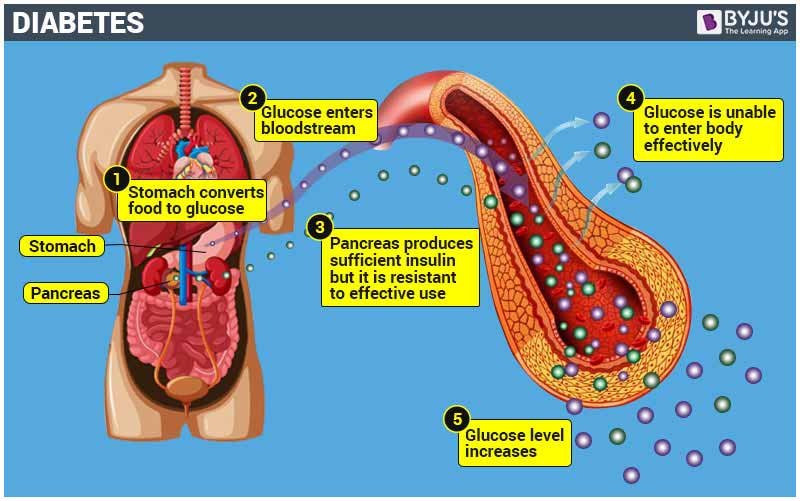
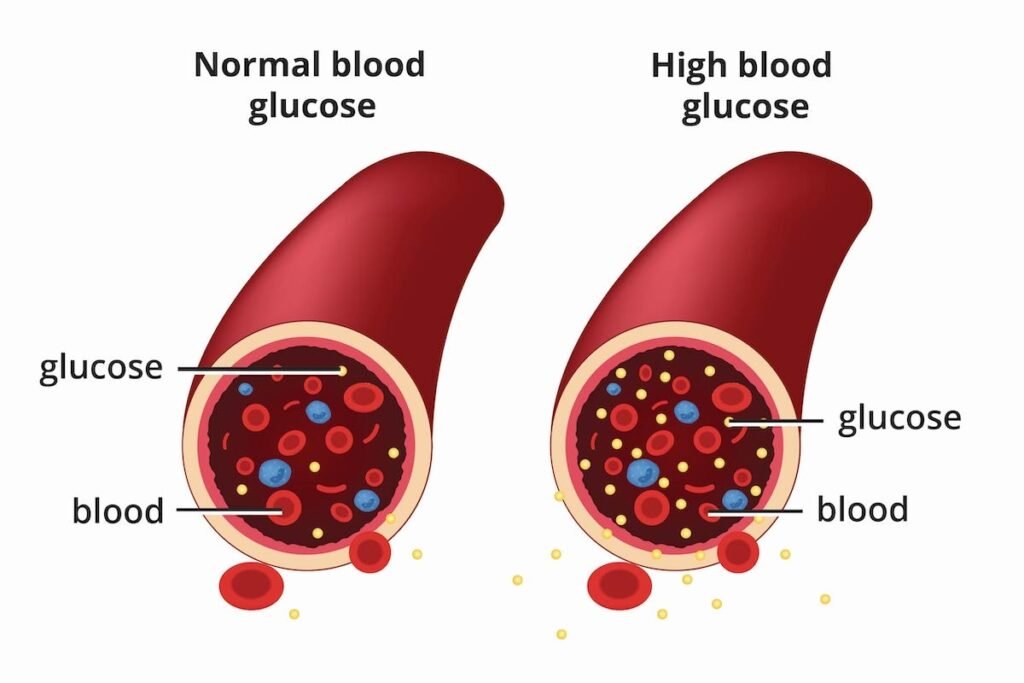
Diabetes Mellitus, commonly referred to as diabetes, is a chronic medical condition that affects the body’s ability to regulate blood sugar levels. It is a metabolic disorder that occurs when the body either doesn’t produce enough insulin or cannot effectively use the insulin it produces. Insulin is a hormone that allows glucose from food to enter the body’s cells, where it is used for energy. Without proper insulin functioning, glucose builds up in the bloodstream, leading to high blood sugar levels.
Types of Diabetes Mellitus
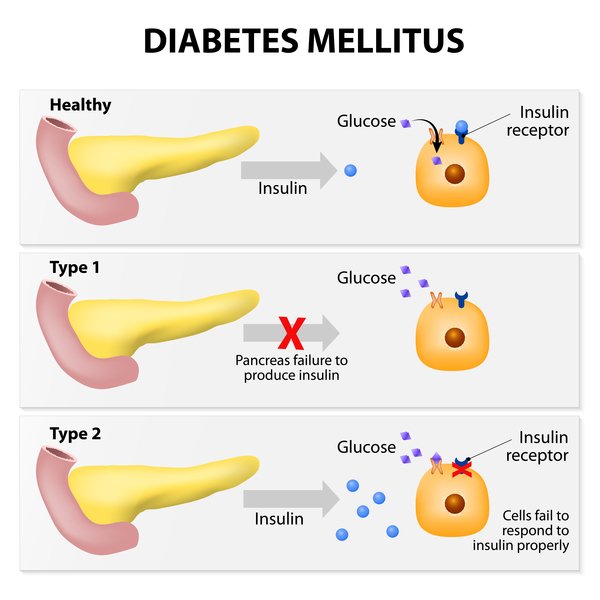
There are several types of diabetes mellitus, including Type 1 Diabetes, Type 2 Diabetes, and Gestational Diabetes. Each type has its own causes, risk factors, and treatment approaches.
Prevalence of Diabetes Mellitus
Diabetes mellitus is a widespread health issue that affects millions of people worldwide. According to the International Diabetes Federation, as of 2019, approximately 463 million adults have diabetes, with the numbers expected to rise to 700 million by 2045. This prevalence underscores the importance of understanding and managing diabetes effectively.
Understanding Type 1 Diabetes
Causes and Risk Factors
Type 1 Diabetes, also known as insulin-dependent diabetes, is an autoimmune disease that usually develops during childhood or adolescence. It occurs when the immune system mistakenly attacks and destroys the insulin-producing cells in the pancreas. The exact cause of Type 1 Diabetes is still unknown, but genetic and environmental factors are believed to play a role.
Pathophysiology of Type 1 Diabetes
In Type 1 Diabetes, the destruction of insulin-producing cells leads to an absolute deficiency of insulin. Without sufficient insulin, glucose cannot enter the cells, causing high blood sugar levels. To manage this condition, individuals with Type 1 Diabetes must rely on exogenous insulin (administered through injections or an insulin pump) to regulate their blood sugar levels.
Symptoms of Type 1 Diabetes
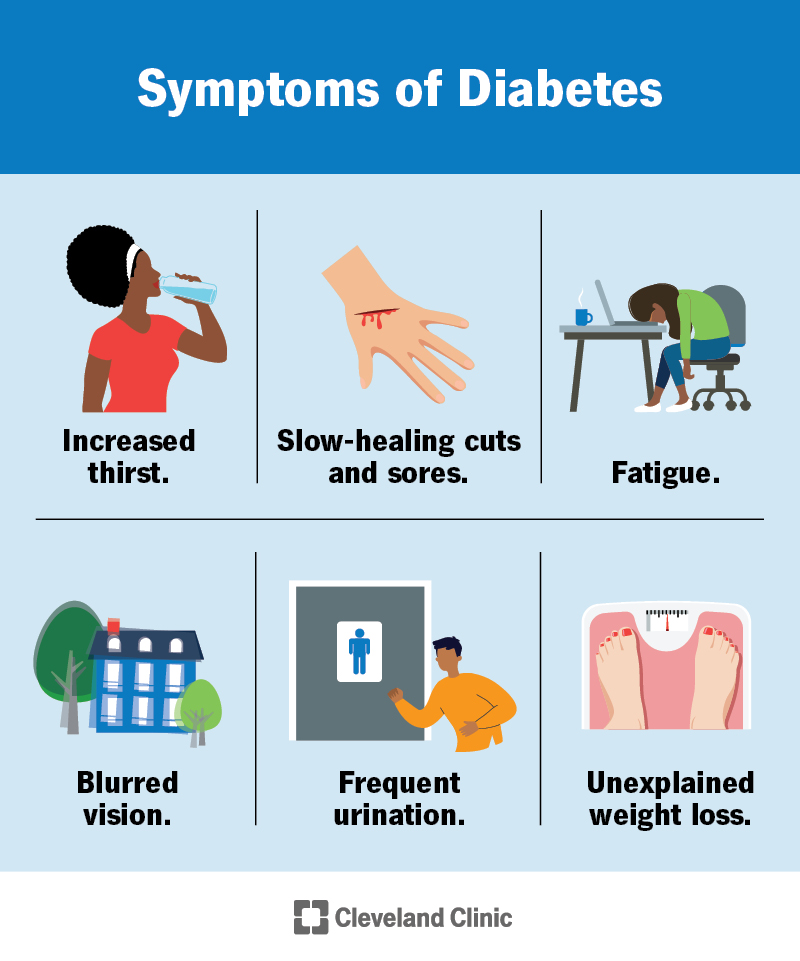
The symptoms of Type 1 Diabetes may include frequent urination, excessive thirst, unexplained weight loss, fatigue, and increased hunger. Since Type 1 Diabetes often develops rapidly, these symptoms may appear suddenly and can quickly become severe if left untreated.
Diagnosis and Treatment
Diagnosing Type 1 Diabetes involves blood tests that measure the blood sugar levels and the presence of specific antibodies associated with the destruction of insulin-producing cells. Once diagnosed, treatment primarily focuses on insulin replacement therapy to maintain blood sugar control. Continuous blood sugar monitoring, carbohydrate counting, and regular medical check-ups are crucial for managing Type 1 Diabetes effectively.
Understanding Type 2 Diabetes
Causes and Risk Factors
Type 2 Diabetes, the most common form of diabetes, occurs when the body becomes resistant to the effects of insulin and doesn’t produce enough insulin to maintain normal blood sugar levels. While the exact cause of Type 2 Diabetes is not fully understood, risk factors include obesity, sedentary lifestyle, genetics, and age.
Pathophysiology of Type 2 Diabetes
In Type 2 Diabetes, the body’s cells become resistant to insulin, and the pancreas may not produce enough insulin to meet the body’s needs. This leads to elevated blood sugar levels. Over time, the pancreas may lose its ability to produce insulin altogether, further exacerbating the condition.
Symptoms of Type 2 Diabetes
Symptoms of Type 2 Diabetes may include increased thirst, frequent urination, unexplained weight loss, fatigue, blurred vision, and slow-healing wounds. However, some individuals with Type 2 Diabetes may not display noticeable symptoms, making regular screenings and check-ups essential for early detection.
Diagnosis and Treatment
Type 2 Diabetes is typically diagnosed through blood tests that measure fasting blood sugar levels and the body’s ability to respond to insulin. Treatment typically includes lifestyle modifications, such as a balanced diet, regular exercise, and weight management. Some individuals may require oral medications or insulin therapy to help control their blood sugar levels effectively.
Lifestyle Management
Lifestyle management plays a crucial role in managing Type 2 Diabetes. Adopting healthy lifestyle habits can help improve insulin resistance and overall blood sugar control. These habits include maintaining a balanced diet, portion control, regular physical activity, stress management, and adequate sleep. Working closely with healthcare professionals and diabetes educators is essential to develop a personalized lifestyle management plan.
Gestational Diabetes
Causes and Risk Factors
Gestational Diabetes is a type of diabetes that occurs during pregnancy. It is caused by hormonal changes that affect the way the body uses insulin. Risk factors for developing gestational diabetes include advanced maternal age, a family history of diabetes, being overweight or obese, and certain ethnic backgrounds.
Symptoms of Gestational Diabetes
Gestational Diabetes often does not present noticeable symptoms. However, some women may experience increased thirst, frequent urination, fatigue, and blurred vision. Regular prenatal check-ups include screenings to detect gestational diabetes, especially around the 24th to 28th week of pregnancy.
Diagnosis and Treatment
Gestational Diabetes is typically diagnosed through a glucose tolerance test, which measures blood glucose levels after consuming a sugary drink. If diagnosed, the goal is to manage blood sugar levels to ensure a healthy pregnancy and minimize the risk of complications. Treatment often involves diet modifications, regular exercise, blood sugar monitoring, and, in some cases, insulin therapy.
Impact on Mother and Baby
If left unmanaged, gestational diabetes can pose risks for both the mother and baby. It increases the risk of high blood pressure, preeclampsia, cesarean delivery, and type 2 diabetes development later in life for the mother. For the baby, risks include excessive birth weight, low blood sugar levels after birth, and an increased likelihood of developing obesity and type 2 diabetes later in life.
Management during Pregnancy
Proper management of gestational diabetes during pregnancy is crucial for the health and well-being of both the mother and baby. This includes regular check-ups with healthcare professionals, following a balanced diet, maintaining physical activity as recommended by the doctor, monitoring blood sugar levels, and close monitoring of fetal growth and development.
Complications of Diabetes Mellitus
Short-term Complications
Short-term complications of diabetes mellitus can occur when blood sugar levels become too high (hyperglycemia) or too low (hypoglycemia). Hyperglycemia, if left uncontrolled, can lead to diabetic ketoacidosis (DKA) in Type 1 Diabetes and hyperosmolar hyperglycemic state (HHS) in Type 2 Diabetes. Both conditions are medical emergencies that require immediate treatment. Hypoglycemia can result from insulin or medication overdose, skipped meals, or excessive exercise. It is important to address both high and low blood sugar levels promptly to prevent complications.
Long-term Complications
Long-term complications of diabetes mellitus can affect various organs and systems in the body. These complications include cardiovascular disease, kidney disease, eye damage, nerve damage (neuropathy), foot problems, and increased susceptibility to infections. Managing blood sugar levels, blood pressure, and cholesterol levels effectively, as well as adopting a healthy lifestyle, can help reduce the risk of these complications.
Prevention and Management
Preventing and effectively managing complications of diabetes mellitus involves a comprehensive approach. This includes regularly monitoring blood sugar levels, adhering to prescribed medications, maintaining a healthy lifestyle, seeking regular medical check-ups, and managing other risk factors such as high blood pressure and high cholesterol levels. Early detection and intervention are key to preventing or minimizing the impact of complications.
Managing Diabetes Mellitus
Blood Sugar Monitoring
Regular blood sugar monitoring is essential in managing diabetes mellitus. It helps individuals make informed decisions about medication doses, dietary choices, and physical activity levels. Blood sugar monitoring methods include self-monitoring using finger pricks, continuous glucose monitoring (CGM) systems, and occasional laboratory tests.
Insulin Administration
For individuals with Type 1 Diabetes or Type 2 Diabetes who require insulin therapy, proper insulin administration is crucial. Insulin can be administered through injections using insulin pens, syringes, or insulin pumps. It is important to follow healthcare professional guidelines and receive proper training to ensure accurate and safe insulin administration.
Oral Medications
For individuals with Type 2 Diabetes, oral medications may be prescribed to help manage blood sugar levels. These medications work in various ways to lower blood sugar levels, improve insulin sensitivity, or reduce glucose production in the liver. Adherence to medication schedules and regular follow-ups with healthcare professionals are important for successful oral medication management.
Dietary Considerations
Diet plays a crucial role in managing diabetes mellitus. A balanced diet that focuses on portion control, carbohydrate counting, and choosing nutrient-dense foods can help stabilize blood sugar levels. Consulting with a registered dietitian or certified diabetes educator can provide personalized recommendations for meal planning.
Exercise and Physical Activity
Regular physical activity is essential for managing diabetes effectively. It helps improve insulin sensitivity, control blood sugar levels, maintain a healthy weight, and reduce the risk of cardiovascular complications. Engaging in activities such as walking, cycling, swimming, or strength training, as recommended by healthcare professionals, can make a significant positive impact on overall diabetes management.
Stress Management
Stress can affect blood sugar levels and overall well-being. Managing stress through techniques such as deep breathing, meditation, yoga, or engaging in hobbies can help individuals with diabetes improve their quality of life. Seeking support from healthcare professionals or support groups can also be beneficial when dealing with the emotional impact of diabetes.
Diabetes Education and Support
Importance of Diabetes Education
Diabetes education is crucial for individuals to effectively manage their condition and prevent complications. It provides valuable knowledge and skills related to blood sugar monitoring, medication management, healthy eating, physical activity, stress management, and problem-solving. Diabetes education also empowers individuals to take an active role in their own care and make informed decisions.
Professional Healthcare Providers
Healthcare providers, such as doctors, nurses, and certified diabetes educators, play a vital role in providing education, treatment, and ongoing support for individuals with diabetes. Regular medical check-ups, diabetes-specific screenings, medication adjustments, and personalized care plans are important aspects of managing diabetes effectively.
Support Groups and Peer Support
Engaging with support groups and seeking peer support can provide valuable emotional support and practical tips for living with diabetes. Connecting with others who understand the challenges and experiences associated with diabetes can provide a sense of camaraderie and reduce feelings of isolation. Online platforms, local community centers, and healthcare organizations often offer support group programs.
Self-Care and Empowerment
Self-care is a crucial aspect of managing diabetes. It involves taking care of physical, mental, and emotional well-being through activities such as regular exercise, stress management, mindfulness, and adequate rest. Empowering oneself through education, support, and self-advocacy can lead to better diabetes management and overall quality of life.
Prevention of Diabetes Mellitus
Healthy Lifestyle Habits
Adopting healthy lifestyle habits can significantly reduce the risk of developing Type 2 Diabetes. This includes regular exercise, maintaining a healthy weight, eating a balanced diet, avoiding tobacco use, limiting alcohol consumption, and getting adequate sleep. Small, sustainable lifestyle changes can have a significant impact on preventing the onset of diabetes mellitus.
Maintaining a Balanced Diet
Eating a balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats is key to preventing diabetes mellitus. Portion control, minimizing the intake of processed foods, sugary beverages, and foods high in saturated fats are important dietary considerations. Consultation with a registered dietitian can provide personalized guidance for maintaining a nutritious diet.
Regular Exercise and Physical Activity
Engaging in regular exercise and physical activity is vital for preventing diabetes mellitus. It helps maintain a healthy weight, improves insulin sensitivity, and lowers the risk of developing obesity and related metabolic disorders. Aim for a combination of cardiovascular exercises, strength training, and flexibility exercises, as recommended by healthcare professionals.

Diabetes Research and Advancements
Current Research Studies
Ongoing research in the field of diabetes aims to expand knowledge about its causes, prevention, and treatment options. Studies explore areas such as the genetics of diabetes, immunotherapy, stem cell research, and the development of new medications. Participating in research studies can provide individuals with diabetes the opportunity to contribute to advancements in diabetes management and treatment.
New Treatment Approaches
Advancements in diabetes treatment are continually being developed. New insulin formulations, medications, and delivery methods are being explored to improve blood sugar control and reduce the burden of diabetes management. Additionally, technologies such as closed-loop insulin delivery systems (artificial pancreas) and mobile health applications (apps) are revolutionizing diabetes care.
Technological Advancements
Technology plays a significant role in diabetes management and monitoring. Continuous glucose monitoring (CGM) systems, insulin pumps, and glucose meters with advanced features and connectivity options enable individuals to monitor their blood sugar levels more easily and make informed decisions about their diabetes management. These advancements have greatly improved the quality of life for people with diabetes.
Living a Healthy Life with Diabetes
Creating a Diabetes Management Plan
Developing a comprehensive diabetes management plan involves considering various aspects of self-care and lifestyle management. This plan may include following healthcare professional recommendations, taking prescribed medications, monitoring blood sugar levels, practicing healthy eating habits, engaging in regular physical activity, managing stress, and seeking support when needed.
Prioritizing Self-Care
Self-care is an essential aspect of living a healthy life with diabetes. It involves prioritizing one’s physical, mental, and emotional well-being. This includes managing blood sugar levels, maintaining a healthy lifestyle, getting regular check-ups, practicing stress management techniques, and seeking support from healthcare professionals, support groups, and loved ones.
Building a Support Network
Building a supportive network of healthcare professionals, family, friends, and other individuals with diabetes can be invaluable when living with the condition. Support networks provide emotional support, encouragement, and practical advice. By surrounding oneself with a strong support system, individuals with diabetes can navigate the challenges of managing their condition more effectively.
Maintaining Emotional Well-being
Living with diabetes can have a significant impact on one’s emotional well-being. It is important to address feelings of stress, anxiety, and depression that may arise. Seeking professional help, joining support groups, practicing stress management techniques, engaging in enjoyable activities, and maintaining open communication with loved ones can all contribute to improving emotional well-being.
In conclusion, diabetes mellitus is a complex condition that requires a comprehensive understanding and management approach. Whether it is Type 1 Diabetes, Type 2 Diabetes, or Gestational Diabetes, a combination of medication, lifestyle modifications, and proper support is key to effectively managing the condition and preventing complications. By staying educated, seeking professional guidance, and prioritizing self-care, individuals with diabetes can lead healthy, fulfilling lives.