If you’re a woman who has experienced the discomfort of bacterial vaginosis, you’re not alone. This comprehensive guide is here to help you manage and navigate this common infection. From understanding the symptoms to exploring treatment options, we’ve got you covered. Together, we’ll empower you with knowledge and practical tips to take control of your health and find relief from bacterial vaginosis. So, let’s embark on this informative journey and unlock the secrets to managing bacterial vaginosis.

Understanding Bacterial Vaginosis
What is Bacterial Vaginosis?
Bacterial vaginosis (BV) is a common vaginal infection that occurs when there is an imbalance in the bacteria naturally found in the vagina. In a healthy vagina, there is a delicate balance between “good” bacteria (also known as lactobacilli) and other bacteria. However, when the “bad” bacteria outnumber the good bacteria, it can lead to bacterial vaginosis.
Causes of Bacterial Vaginosis
The exact cause of bacterial vaginosis is still not fully understood. However, certain factors can increase the risk of developing BV. These factors include multiple sexual partners, douching, smoking, and a history of sexually transmitted infections (STIs). It is important to note that BV is not considered a sexually transmitted infection, although sexual activity can increase the risk.
Symptoms of Bacterial Vaginosis
One of the challenging aspects of bacterial vaginosis is that many women may not experience any symptoms. However, when symptoms do occur, they often include a thin, grayish-white vaginal discharge with a strong fishy odor. Some women may also experience itching or irritation around the vagina. It is crucial to consult a healthcare provider for an accurate diagnosis, as other conditions can cause similar symptoms.
Complications of Bacterial Vaginosis
While bacterial vaginosis itself does not typically cause serious complications, it can increase the risk of other health issues. Women with BV are more likely to contract sexually transmitted infections, including HIV, if exposed. Additionally, BV during pregnancy can lead to preterm birth and low birth weight. Therefore, timely diagnosis and treatment are essential to prevent these complications.
Diagnosing Bacterial Vaginosis
Visiting a Healthcare Provider
If you suspect you may have bacterial vaginosis, it is crucial to make an appointment with a healthcare provider. They have the expertise to accurately diagnose and provide appropriate treatment. Remember, self-diagnosis may not be accurate, and delaying medical attention can lead to complications.
Medical History and Physical Examination
During your visit, the healthcare provider will conduct a thorough medical history assessment, asking questions about your symptoms, sexual history, and previous pelvic infections. This information helps in determining the possible cause and appropriate treatment. A physical examination of the vagina and cervix may also be performed to assess any visible signs of BV.
Laboratory Tests for Bacterial Vaginosis
To confirm the diagnosis, the healthcare provider may collect a sample of vaginal discharge for laboratory testing. This test examines the vaginal fluid under a microscope and checks for the presence of bacterial overgrowth and the absence of lactobacilli. Laboratory tests are essential to ensure an accurate diagnosis, as symptoms alone may not be enough to determine whether it is BV or another vaginal infection.

Treating Bacterial Vaginosis
Antibiotics for Bacterial Vaginosis
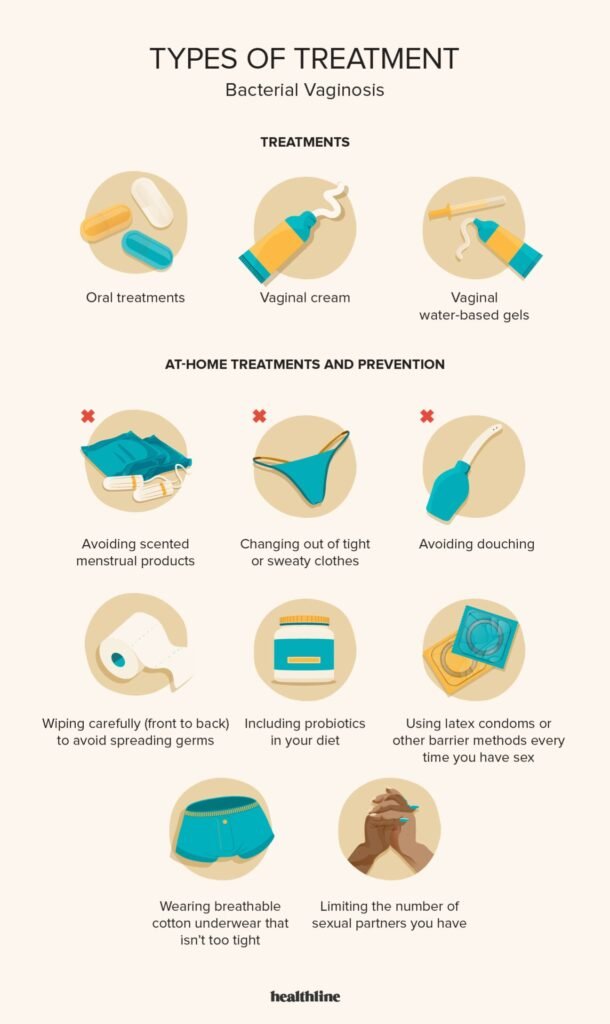
The primary treatment for bacterial vaginosis is the use of antibiotics, prescribed by a healthcare provider. These antibiotics can be administered orally or in the form of vaginal creams or gels. It is important to complete the full course of antibiotics, even if symptoms improve, to ensure eradication of the infection. Avoid self-medication or using leftover antibiotics, as it may lead to antibiotic resistance and recurring infections.
Home Remedies and Self-Care Measures
In addition to prescribed medications, there are a few self-care measures that can help manage bacterial vaginosis. These include:
- Avoiding douching: Douching disrupts the natural balance of bacteria in the vagina and can worsen BV.
- Gently washing the genital area: Use mild, fragrance-free soap and warm water to clean the external genital area. Avoid harsh soaps or scented products.
- Wearing breathable underwear: Opt for cotton underwear and avoid tight-fitting clothing to allow air circulation and minimize moisture buildup.
- Limiting the number of sexual partners: Having multiple sexual partners can increase the risk of recurring BV.
- Using condoms: Consistent and correct condom use can reduce the risk of developing BV, especially if you have a new sexual partner.
Alternative Treatment Options
Some women may explore alternative treatment options for bacterial vaginosis. However, it is important to note that there is limited scientific evidence supporting the effectiveness of these treatments. Some alternatives that have been studied include tea tree oil, probiotics, and hydrogen peroxide. It is crucial to consult with a healthcare provider before trying any alternative treatments to ensure they are safe and will not interfere with the prescribed treatment plan.
Preventing Bacterial Vaginosis
Maintaining Good Hygiene
Maintaining good hygiene is key to preventing bacterial vaginosis. You can follow these hygiene practices to reduce the risk of developing BV:
- Clean the genital area: Gently wash the external genital area with mild, fragrance-free soap and warm water. Avoid using harsh soaps or douching, as they can disrupt the natural balance of bacteria in the vagina.
- Wipe from front to back: After using the toilet, always wipe from front to back to prevent the spread of bacteria from the anus to the vagina.
- Avoid using scented products: Avoid using scented sanitary pads, tampons, powders, or sprays in the genital area, as they can irritate the vagina and disrupt the natural flora.
Avoiding Specific Practices
Certain practices can increase the risk of bacterial vaginosis. To prevent BV, it is advisable to:
- Limit douching: Douching can disrupt the natural balance of bacteria in the vagina and increase the risk of BV. It is best to avoid douching altogether.
- Use caution with new sexual partners: Having multiple sexual partners or engaging in unprotected sex can increase the risk of developing BV. Practicing safe sex and using condoms consistently can help reduce this risk.
Probiotics and Bacterial Vaginosis Prevention
Some studies suggest that the use of probiotics may help prevent bacterial vaginosis. Probiotics are live bacteria and yeasts that are beneficial for health. They can be found naturally in the vagina or taken orally in the form of supplements or consumed through certain foods, such as yogurt. However, more research is needed to definitively establish the effectiveness of probiotics in preventing BV. If considering probiotics, it is best to consult with a healthcare provider for guidance.
Managing Recurrent Bacterial Vaginosis
Understanding Recurrent Bacterial Vaginosis
Recurrent bacterial vaginosis refers to multiple episodes of BV within a year. It can be frustrating, but with proper management, recurrence can be minimized. It is essential to identify the underlying causes and triggers for recurring BV, as they may differ from the initial infection.
Identifying Triggers for Recurrence
Identifying triggers for recurrent bacterial vaginosis is crucial for effective management. Some common triggers may include:
- Sexual activity: Some women may notice BV episodes occurring after sexual intercourse. It is important to discuss this with a healthcare provider to explore potential preventive strategies.
- Hormonal changes: Fluctuations in hormone levels, such as during menstruation or menopause, may contribute to recurring BV. Managing hormonal changes alongside proper treatment can help reduce the recurrence rate.
Long-Term Management Strategies
To manage recurrent bacterial vaginosis, a healthcare provider may recommend a customized approach. This may include a combination of the following:
- Extended antibiotic treatment: A longer duration of antibiotic treatment, or intermittent dosing, may be prescribed to prevent recurrence.
- Probiotics: Regular use of probiotics, either orally or vaginally, may help maintain a healthy vaginal flora and reduce the risk of recurrent BV.
- Partner treatment: Treating sexual partners, especially for those who have multiple partners, may be recommended to prevent reinfection.
- Regular follow-ups: Regular check-ups with a healthcare provider can help monitor the effectiveness of the treatment and make any necessary adjustments.
Effects on Pregnancy
Bacterial Vaginosis and Pregnancy
Bacterial vaginosis can have implications for pregnant women and their unborn babies. It is important to seek proper diagnosis and treatment during pregnancy to reduce the risks associated with BV. Pregnant women with BV have an increased risk of premature birth, low birth weight, and infection of the amniotic sac and fluid.
Possible Complications
If left untreated during pregnancy, bacterial vaginosis can lead to complications such as:
- Preterm birth: BV increases the risk of delivering prematurely, which can pose health problems for the baby.
- Low birth weight: Babies born to mothers with untreated BV may have a lower birth weight, which can also increase the risk of certain health issues.
- Infection of the amniotic sac and fluid: BV can increase the risk of the amniotic sac and fluid becoming infected, which can be dangerous for both the mother and baby.
Prevention and Treatment during Pregnancy
Pregnant women should inform their healthcare provider about any symptoms or concerns related to bacterial vaginosis. Routine screening for BV is recommended during prenatal care, and if diagnosed, treatment with antibiotics may be necessary. Following the prescribed treatment plan is vital to reduce the risk of complications. It is important to note that not all pregnant women with BV require treatment, as healthcare providers carefully evaluate the risks and benefits of treatment on an individual basis.

Bacterial Vaginosis and Sexual Health
Transmission and Sexual Partners
Bacterial vaginosis is not considered a sexually transmitted infection (STI). However, the exact mechanisms of transmission are not fully understood. It is still possible for sexual partners to transmit or reinfect each other, even though BV is not solely caused by sexual activity. Treating sexual partners may be recommended in cases of recurrent BV.
Safe Sexual Practices and Prevention
Practicing safe sex can help reduce the risk of bacterial vaginosis. Consider the following tips:
- Consistent condom use: Using condoms consistently and correctly can help reduce the risk of recurrent BV and sexually transmitted infections.
- Limiting sexual partners: Having multiple sexual partners can increase the risk of developing BV. Reducing the number of sexual partners can lower the chances of acquiring or transmitting BV.
- Communication with sexual partners: Open communication with sexual partners about symptoms, testing, and treatment can help prevent reinfection or transmission of BV.
Bacterial Vaginosis and Menopause
Hormonal Changes and Bacterial Vaginosis
Hormonal changes that occur during menopause can influence the vaginal environment and increase the risk of developing bacterial vaginosis. The drop in estrogen levels can lead to a decrease in protective lactobacilli bacteria and a subsequent increase in harmful bacteria. Women going through menopause should be vigilant about their vaginal health and seek appropriate treatment if BV symptoms arise.
Treatment and Management during Menopause
The treatment options for bacterial vaginosis during menopause are generally the same as those for women in other stages of life. Antibiotics may be prescribed to eliminate the infection, and self-care measures, such as maintaining good hygiene and wearing breathable underwear, should be followed. It is important for menopausal women to consult with their healthcare provider for personalized advice and management strategies specific to their situation.

Addressing Mental and Emotional Impact
Emotional Impact of Bacterial Vaginosis
Bacterial vaginosis can have a significant emotional impact on women. It can lead to feelings of embarrassment, shame, or frustration due to the symptoms and potential recurrent episodes. It is important to remember that BV is a common condition that affects many women, and seeking support and understanding is crucial to managing the emotional impact.
Seeking Support and Coping Strategies
If you are experiencing emotional distress related to bacterial vaginosis, consider the following:
- Talk to your healthcare provider: Discuss your concerns and emotions openly with your healthcare provider. They can provide reassurance and advice on managing the emotional impact.
- Reach out to support groups: Online forums, support groups, or counseling services can offer a safe space to connect with others who may be experiencing similar challenges.
- Educate yourself: Understanding the condition, its causes, and treatment options can help reduce anxiety and provide a sense of control over the situation.
Talking Openly about Bacterial Vaginosis
Breaking the Silence and Reducing Stigma
The stigma surrounding any vaginal infection, including bacterial vaginosis, can prevent open discussions and limit access to accurate information. Breaking the silence around BV is crucial for raising awareness and ensuring that women feel comfortable seeking help and support. By speaking openly about BV, we can reduce the stigma associated with vaginal health issues.
Educating Others about Bacterial Vaginosis
Educating others about bacterial vaginosis is an essential step in dispelling myths and misconceptions. Share accurate information about the causes, symptoms, and treatment options for BV. Encourage open conversations about vaginal health and advocate for regular screenings and treatment when necessary. By increasing awareness, we can empower women to take control of their vaginal health and seek appropriate care.
