Hey there! Have you ever wondered what exactly mumps is and why it’s considered a contagious viral infection? Well, wonder no more! In this article, we’ll be diving into the fascinating world of mumps, unraveling its mysterious nature, and exploring why it can be so easily passed from person to person. So grab a cup of tea, put on your learning cap, and get ready to uncover the secrets of mumps!
Causes and Transmission
Viral Pathogen: Mumps Virus
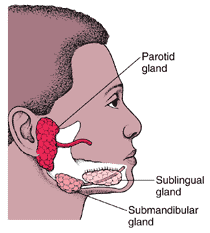
Mumps is a contagious viral infection caused by the mumps virus. The virus belongs to the paramyxovirus family and is spread from person to person through respiratory droplets. It primarily affects the salivary glands, leading to the characteristic swelling and tenderness of the cheeks and jaw. However, the virus can also cause inflammation in other parts of the body, such as the testes, ovaries, pancreas, and brain.
Modes of Transmission
The mumps virus is highly contagious and can be transmitted through close contact with an infected person. It can spread when an infected individual coughs or sneezes, releasing tiny droplets containing the virus into the air. These droplets can then be inhaled by others nearby, infecting them. The virus can also be spread through direct contact with an infected person’s saliva or by touching surfaces contaminated with the virus and then touching the mouth or nose.
Symptoms and Complications
Early Symptoms
After being exposed to the mumps virus, it takes about 12-25 days for symptoms to appear. The early symptoms of mumps are often nonspecific and can easily be mistaken for a common cold or flu. These initial signs may include fatigue, headache, muscle aches, fever, and loss of appetite. Some individuals may also experience a mild sore throat and difficulty swallowing.
Common Symptoms
Within a few days, the characteristic symptoms of mumps begin to manifest. Swelling and tenderness of the salivary glands, which are located at the sides of the face beneath the ears, are the most recognizable symptoms. This swelling can be bilateral or unilateral and usually lasts for about a week. Other common symptoms include pain while chewing or swallowing, dry mouth, fever, and a general feeling of malaise.
Serious Complications
Although most cases of mumps are mild and resolve on their own, serious complications can arise in some individuals. The virus can cause inflammation of the testicles in males, leading to orchitis, which can result in testicular atrophy and infertility in rare cases. In females, the virus can cause inflammation of the ovaries, known as oophoritis, which can lead to fertility problems. Mumps can also cause pancreatitis, meningitis, and encephalitis, which can potentially result in long-term neurological damage.

Diagnosis
Clinical Evaluation
To diagnose mumps, a healthcare professional will typically evaluate your symptoms and conduct a physical examination. The characteristic swelling of the salivary glands, particularly around the jaw and ears, is often enough for a preliminary diagnosis. However, further tests may be required to confirm the presence of the mumps virus and rule out other possible causes of the symptoms.
Laboratory Tests
Laboratory tests can be done to detect the presence of the mumps virus in the body. One common test is the polymerase chain reaction (PCR) test, which can amplify and identify the genetic material of the virus. Blood tests may also be performed to check for mumps-specific antibodies, which indicate a past or current infection. These tests help in confirming the diagnosis and can be particularly useful in cases where the symptoms are atypical or if there is a need to track the spread of the virus during an outbreak.
Prevention
Vaccination
Vaccination is the most effective method of preventing mumps. The MMR vaccine, which protects against measles, mumps, and rubella, is recommended for all children and adults who have not been previously vaccinated or have not had the diseases. The vaccine consists of two doses, typically given at 12-15 months of age and 4-6 years of age. The majority of individuals who receive two doses of the MMR vaccine develop immunity to mumps, significantly reducing the risk of infection and its complications.
Herd Immunity
Herd immunity plays an essential role in reducing the transmission of mumps. When a significant portion of the population is immune to the virus through vaccination, the spread of the disease is limited, protecting those who are unable to receive the vaccine or have a weakened immune system. Maintaining high vaccination rates is crucial for ensuring herd immunity and preventing outbreaks of mumps.
Isolation and Quarantine
During an outbreak, it is important to isolate and quarantine individuals with mumps to prevent the spread of the virus. Infected individuals should stay home from school, work, or other public places until they are no longer contagious. This typically involves staying isolated for at least five days after the onset of swelling in the salivary glands. It is also advisable to practice good respiratory hygiene, such as covering the mouth and nose when coughing or sneezing, to reduce the risk of transmitting the virus to others.

Treatment
Supportive Care
There is no specific antiviral treatment for mumps, and most cases resolve on their own with time. Treatment mainly focuses on relieving symptoms and providing supportive care. This includes getting plenty of rest, drinking fluids to stay hydrated, and using over-the-counter pain relievers, such as acetaminophen or ibuprofen, to alleviate fever and pain. Applying warm or cold compresses to the swollen areas may also help soothe discomfort.
Medication
In cases of severe complications or when the infection affects other areas of the body, such as the brain or testes, additional treatment may be required. Antiviral medications may be prescribed to help reduce the severity and duration of symptoms, especially if the infection progresses to encephalitis or meningitis. Pain medications or anti-inflammatory drugs may also be recommended to manage complications such as orchitis or oophoritis.
Epidemiology
Global Prevalence
Mumps is a global disease, although its prevalence varies from region to region. Prior to the introduction of widespread vaccination, mumps was common among children, with most individuals experiencing the infection during childhood or adolescence. However, due to the success of vaccination programs, the incidence of mumps has significantly declined in many countries.
Outbreaks and Trends
Despite the availability of vaccines, outbreaks of mumps still occur, often in communities where vaccination rates are low or among individuals who have not received the recommended doses of the MMR vaccine. These outbreaks can lead to a rapid spread of the virus and an increased number of cases. Monitoring and surveillance of mumps cases are crucial for identifying outbreaks, implementing control measures, and addressing any gaps in vaccination coverage.
History
First Recognized Cases
The first recognized cases of mumps were reported during the 5th century BC by Hippocrates, the ancient Greek physician often referred to as the “father of modern medicine.” However, it was not until the 1830s that the distinct features of mumps were described in detail by Dr. Robert Hamilton. The isolation of the mumps virus and the development of a vaccine came much later, with the virus being isolated in 1945 and the first mumps vaccine becoming available in 1967.
Vaccine Development
The development of the mumps vaccine was a significant milestone in the prevention and control of the disease. The first mumps vaccine, a live attenuated vaccine, was developed by Dr. Maurice Hilleman and colleagues at Merck & Co. The vaccine was initially combined with the vaccines for measles and rubella to create the MMR vaccine, which has since played a crucial role in reducing the incidence of these diseases worldwide.
Public Health Measures
Public Awareness Campaigns
Public awareness campaigns play a vital role in educating the public about mumps and the importance of vaccination. These campaigns provide information about the symptoms, transmission, and prevention of mumps, as well as dispelling any myths or misconceptions surrounding vaccination. By increasing knowledge and understanding, public awareness campaigns help promote vaccination and encourage individuals to take steps to protect themselves and their communities.
Surveillance and Reporting
Surveillance and reporting of mumps cases are essential for monitoring the prevalence and spread of the disease. Healthcare providers and laboratories are responsible for reporting suspected or confirmed cases of mumps to the relevant public health authorities. This information is used to track outbreaks, identify areas with low vaccination rates, and implement appropriate control measures to prevent further transmission of the virus.
Response to Outbreaks
During outbreaks, public health authorities work closely with healthcare providers, schools, and other community organizations to respond effectively. This may involve conducting contact tracing to identify and notify individuals who have been exposed to the virus, implementing isolation and quarantine measures, and providing guidance on vaccination and preventive measures. Prompt and coordinated responses are crucial for containing outbreaks and preventing further spread of the disease.

Controversies
Mumps Vaccine Safety
The safety of vaccines, including the MMR vaccine, has been a subject of controversy in recent years. However, extensive scientific research and numerous studies have consistently shown that the MMR vaccine is safe and effective. The most common side effects are mild and temporary, such as fever or rash. Severe allergic reactions or other serious adverse events are extremely rare. The benefits of vaccination, including the prevention of potentially severe complications of mumps, far outweigh the minimal risks associated with the vaccine.
Anti-Vaccination Movements
Despite the overwhelming evidence supporting the safety and efficacy of vaccines, there are still individuals and groups who choose not to vaccinate their children or advocate against vaccination. These anti-vaccination movements often spread misinformation and conspiracy theories, which can lead to vaccine hesitancy and a decline in vaccination rates. This poses a significant public health risk, as it increases the likelihood of outbreaks and puts individuals who are unable to receive vaccines at greater risk of infection.
Conclusion
Mumps is a contagious viral infection that can result in significant complications, including infertility and neurological damage. The best way to prevent mumps is through vaccination, which not only protects individuals but also contributes to herd immunity and reduces the overall transmission of the virus. Public health measures, such as surveillance, public awareness campaigns, and timely responses to outbreaks, are crucial for controlling the spread of mumps and ensuring the health and well-being of communities. It is important to address any controversies or hesitations surrounding vaccines and promote accurate information to counteract the impact of anti-vaccination movements. By staying informed, taking preventive measures, and supporting vaccination efforts, we can work together to prevent mumps and protect ourselves and our communities.
