Diverticulitis is a condition that causes inflammation in the small pouches, known as diverticula, that form in the lining of the digestive system. This article will explore the risk factors associated with developing diverticulitis and provide essential precautions to minimize its occurrence. By understanding the factors that contribute to the development of this condition and incorporating preventive measures into your lifestyle, you can significantly reduce the chances of experiencing the discomfort and complications associated with diverticulitis. So, let’s dive into the world of risk factors and precautions for diverticulitis, ensuring a healthier future for you.
Risk Factors for Diverticulitis
Age
Diverticulitis primarily affects individuals who are over the age of 40. As you age, the risk of developing diverticulitis increases. Therefore, it is important to be aware of this risk factor and take precautions to prevent its occurrence or manage its symptoms if already diagnosed.
Diet
Your diet plays a crucial role in the development and management of diverticulitis. A low-fiber diet, which lacks the necessary roughage, can increase the risk of diverticulitis. It is recommended to consume a high-fiber diet, consisting of fruits, vegetables, whole grains, and legumes, to maintain a healthy digestive system and reduce the risk of diverticulitis.
Obesity
Being overweight or obese significantly increases the risk of diverticulitis. Excess weight puts pressure on the colon, making it more susceptible to developing diverticula and potentially leading to inflammation. By maintaining a healthy weight through a balanced diet and regular exercise, you can reduce the risk of diverticulitis.
Smoking
Smoking has been linked to various health conditions, and diverticulitis is no exception. Studies have shown that smoking increases the risk of developing diverticulitis and can worsen the symptoms for those already diagnosed. Quitting smoking not only reduces the risk of diverticulitis but also improves overall health and well-being.
Physical Inactivity
Engaging in regular physical activity offers numerous health benefits, including a reduced risk of diverticulitis. Physical inactivity can lead to constipation and a sluggish digestive system, increasing the likelihood of diverticula formation. Incorporating exercise into your daily routine, such as brisk walking, cycling, or swimming, can improve digestion and lower the risk of diverticulitis.
Genetic Factors
Family History
If you have a family history of diverticulitis, your risk of developing the condition is higher than the general population. Genetics plays a role in the development of diverticulitis, and having a close relative with the condition increases your susceptibility. It is essential to keep your healthcare provider informed about your family history and take necessary precautions to reduce the risk.
Ethnicity
Certain ethnicities, such as individuals of African American or Hispanic descent, are more prone to developing diverticulitis. The reasons for this increased risk among specific ethnic groups are still being studied. However, it is important to keep in mind that anyone, regardless of ethnicity, can develop diverticulitis. Precautions and lifestyle modifications can be implemented to minimize the risk.
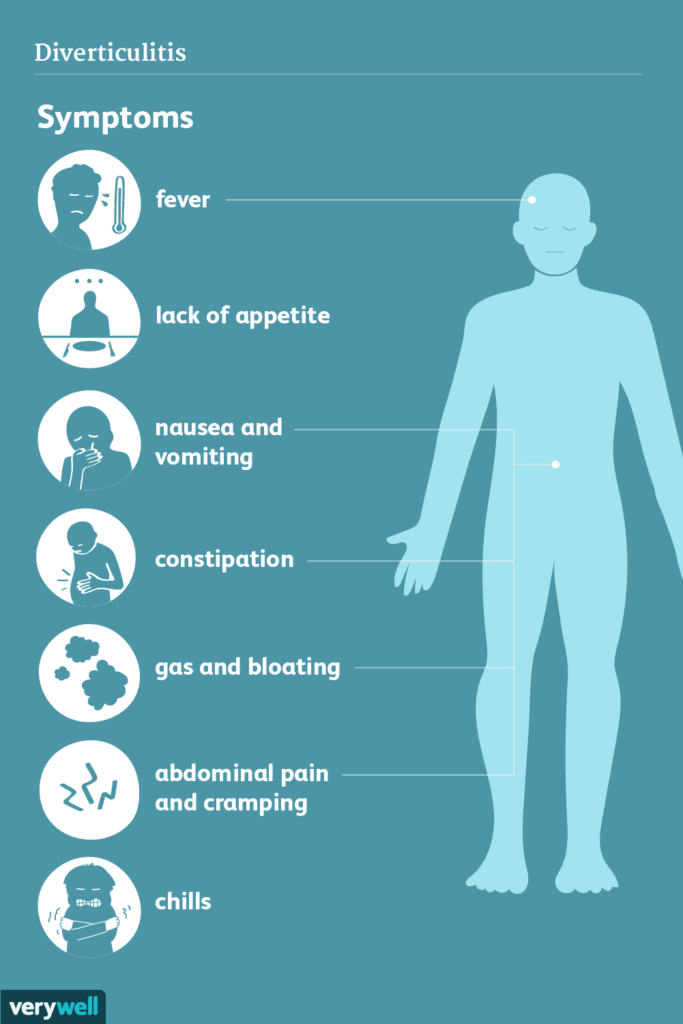
Medical Conditions
Connective Tissue Disorders
Connective tissue disorders, such as Ehlers-Danlos syndrome or Marfan syndrome, can increase the risk of developing diverticulitis. These conditions weaken the connective tissues in the body, including the walls of the colon, making them more susceptible to diverticula formation. It is essential to work closely with your healthcare provider to manage these conditions and reduce the risk of diverticulitis.
Immunosuppression
Individuals with weakened immune systems, such as those undergoing chemotherapy or organ transplant recipients, have a higher risk of developing diverticulitis. Immunosuppression compromises the body’s ability to fight off infections and can lead to more severe symptoms of diverticulitis. It is crucial to discuss your medical conditions and medications with your healthcare provider to determine the best course of action in preventing diverticulitis.
Chronic Diseases
Certain chronic conditions, such as diabetes or kidney disease, can increase the risk of diverticulitis. These conditions often require specific dietary modifications, including restrictions on fiber intake, which can contribute to diverticula formation. Managing these chronic diseases through proper medication and lifestyle changes is crucial in lowering the risk of diverticulitis.
Medications
Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
Long-term or excessive use of nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen can increase the risk of diverticulitis. These medications can irritate the lining of the digestive tract, potentially leading to inflammation and complications. It is advisable to use NSAIDs only as directed by your healthcare provider and explore alternative pain management options whenever possible.
Steroids
Steroids, particularly when used for extended periods, can weaken the immune system and increase the risk of diverticulitis. These medications can contribute to diverticula formation and worsen symptoms if diverticulitis is already present. It is important to follow your healthcare provider’s instructions when taking steroids and discuss any concerns or potential risks associated with their use.

Precautions for Diverticulitis
Dietary Modifications
One of the most effective ways to prevent or manage diverticulitis is through dietary modifications. Increasing your fiber intake is key, as it helps maintain regular bowel movements and prevents constipation. Aim to incorporate whole grains, fresh fruits and vegetables, legumes, nuts, and seeds into your diet. Additionally, limit your consumption of processed foods, fast foods, and products made from refined white flour.
Adequate Fluid Intake
Alongside a high-fiber diet, adequate fluid intake is crucial for the prevention and management of diverticulitis. Water is the best option to stay hydrated, but herbal teas and clear broths can also contribute to fluid intake. Avoid excessive consumption of caffeinated and sugary beverages, as they can dehydrate the body and potentially worsen symptoms.
Regular Exercise
Regular exercise offers numerous benefits for overall health, including a reduced risk of diverticulitis. Engaging in moderate-intensity aerobic activities like brisk walking, cycling, or swimming improves digestion and helps maintain bowel regularity. Aim for at least 150 minutes of moderate-intensity exercise per week, or as recommended by your healthcare provider.
Weight Management
Maintaining a healthy weight is important for reducing the risk of diverticulitis. Excess weight puts pressure on the colon, making it more susceptible to the development and complications of diverticula. Incorporate a balanced diet and regular exercise into your lifestyle to achieve and maintain a healthy weight.
Smoking Cessation
Smoking not only increases the risk of various health conditions but also exacerbates the symptoms of diverticulitis. Quitting smoking is highly beneficial for reducing the risk of diverticulitis and improving overall health. Seek support from healthcare professionals, friends, and family to successfully quit smoking and reduce the likelihood of complications associated with diverticulitis.
High-Fiber Diet
Importance of Fiber
Fiber plays a crucial role in the prevention and management of diverticulitis. It adds bulk to the stools, promoting regular bowel movements and preventing constipation. Additionally, fiber helps maintain the health of the colon walls and reduces the risk of diverticula formation. Make sure to include an adequate amount of fiber in your daily diet to support a healthy digestive system.
Sources of Fiber
Including a variety of fiber-rich foods in your diet is key to meeting your daily fiber intake. Whole grains like oats, quinoa, and brown rice, fresh fruits and vegetables, legumes such as beans and lentils, and nuts and seeds are excellent sources of fiber. Be creative in incorporating these foods into your meals and snacks to ensure a well-rounded and fiber-rich diet.
Types of Fiber
There are two types of dietary fiber: soluble and insoluble fiber. Soluble fiber dissolves in water and forms a gel-like substance in the digestive system, helping regulate blood sugar levels and lower cholesterol. Insoluble fiber, on the other hand, adds bulk to the stools, aiding in regular bowel movements and preventing constipation. Both types of fiber are important for maintaining a healthy digestive system and preventing diverticulitis.
Recommended Daily Fiber Intake
The recommended daily fiber intake varies depending on age and gender. For adults, it is generally recommended to consume between 25-38 grams of fiber per day. However, it is advisable to consult with your healthcare provider or a registered dietitian to determine the appropriate fiber intake for your specific needs and health conditions.

Low-Fiber Foods to Avoid
Processed Foods
Processed foods, such as packaged snacks, sugary cereals, and ready-to-eat meals, are typically low in fiber and high in unhealthy fats and sugars. These foods can contribute to constipation and increase the risk of diverticulitis. It is best to limit your consumption of processed foods and opt for whole, unprocessed foods whenever possible.
Fast Foods
Fast foods, including burgers, fries, and fried chicken, are often high in unhealthy fats, low in fiber, and lacking essential nutrients. Regular consumption of fast food can lead to weight gain, inflammation, and gastrointestinal issues such as constipation. It is advisable to avoid or minimize fast food intake to reduce the risk of diverticulitis and maintain overall health.
White Flour Products
White flour products like white bread, pastries, and white pasta are refined carbohydrates that have undergone a process that removes most of the fiber and nutrients. These low-fiber foods can contribute to constipation and should be limited in a diverticulitis diet. Opt for whole grain alternatives, such as whole wheat bread, whole wheat pasta, and whole grain crackers, to increase your fiber intake.
Foods to Include in a Diverticulitis Diet
Whole Grains
Whole grains like oats, quinoa, brown rice, whole wheat bread, and whole grain cereals are excellent sources of fiber. Including these foods in your diet provides essential nutrients and promotes healthy digestion, reducing the risk of diverticulitis. Experiment with different whole grain options to add variety to your meals and snacks.
Fresh Fruits and Vegetables
Fresh fruits and vegetables should be a staple in a diverticulitis diet. They are rich in fiber, vitamins, minerals, and antioxidants, providing numerous health benefits. Incorporate a variety of fruits and vegetables into your meals, aiming for at least five servings per day. Choose fresh, seasonal produce whenever possible and experiment with different cooking methods to enhance the flavors.
Legumes
Legumes, including beans, lentils, chickpeas, and peas, are a fantastic source of fiber and plant-based protein. Adding legumes to your meals not only increases your fiber intake but also provides essential nutrients and promotes gut health. Explore various legume recipes, such as soups, salads, and stews, to incorporate them into your diet.
Nuts and Seeds
Nuts and seeds like almonds, chia seeds, flaxseeds, and sunflower seeds are excellent sources of healthy fats, fiber, and essential minerals. They can be added to a variety of dishes, including salads, smoothies, or used as a topping for yogurt or oatmeal. However, it is important to consume them in moderation as they are high in calories.

Importance of Adequate Fluid Intake
Water
Adequate fluid intake is crucial for maintaining a healthy digestive system and preventing constipation. Water is the most essential fluid you should consume throughout the day. It helps soften the stools and promotes regular bowel movements. Aim to drink at least 8 cups (64 ounces) of water per day, or more if you are physically active or in hot weather conditions.
Herbal Teas
Herbal teas, such as chamomile, peppermint, or ginger tea, can contribute to your fluid intake while offering additional health benefits. These teas have soothing properties and can help ease digestive discomfort. Avoid adding sugar or sweeteners to herbal teas, as they may irritate the digestive system.
Clear Broths
Clear broths, such as vegetable broth or bone broth, can also contribute to your fluid intake while providing nourishment. These broths are rich in minerals and can help hydrate the body. Opt for low-sodium options or make your own clear broth to control the sodium content.
Regular Exercise and Weight Management
Benefits of Exercise
Regular exercise offers numerous benefits, including a reduced risk of diverticulitis. Exercise helps maintain a healthy weight, improves digestion, reduces constipation, and enhances overall well-being. It also promotes the proper functioning of the digestive system and supports the body’s immune system. Engaging in regular physical activity can significantly contribute to the prevention and management of diverticulitis.
Recommended Exercise Types
To reap the benefits for your digestive health, aim for a combination of aerobic exercise and strength training. Moderate-intensity aerobic activities like brisk walking, cycling, or swimming help stimulate digestion and maintain bowel regularity. Strength training exercises, such as weightlifting or Pilates, can strengthen the abdominal muscles and support the digestive system. Consistency is key, so aim for at least 150 minutes of moderate-intensity exercise per week, or as recommended by your healthcare provider.
Maintaining a Healthy Weight
Maintaining a healthy weight is crucial for reducing the risk of diverticulitis. Excess weight puts pressure on the colon, making it more susceptible to diverticula formation and complications. By incorporating regular exercise and a balanced diet into your lifestyle, you can achieve and maintain a healthy weight. Consult with your healthcare provider or a registered dietitian for guidance on developing a personalized plan that suits your individual needs and goals.
In conclusion, understanding the risk factors for diverticulitis empowers you to take necessary precautions and make lifestyle modifications to prevent or manage the condition effectively. By considering factors such as age, diet, obesity, smoking, and physical inactivity, you can reduce the likelihood of developing diverticulitis and alleviate its symptoms. Emphasizing dietary modifications, adequate fluid intake, regular exercise, weight management, and smoking cessation can significantly contribute to a healthier digestive system and overall well-being. Remember to consult with your healthcare provider for personalized advice and guidance tailored to your specific needs.
