Did you know that the consumption of gluten can have a deep impact on the lives of those with celiac disease? This article explores the intricate link between gluten and celiac disease, shedding light on how this protein affects the health and well-being of individuals diagnosed with this condition. Whether you have celiac disease or simply want to better understand the connection between gluten and this autoimmune disorder, this article provides valuable insights into this often-misunderstood relationship. So, grab a cup of tea and get ready to uncover the truth behind the link between gluten and celiac disease.
Overview of Celiac Disease
Definition of Celiac Disease
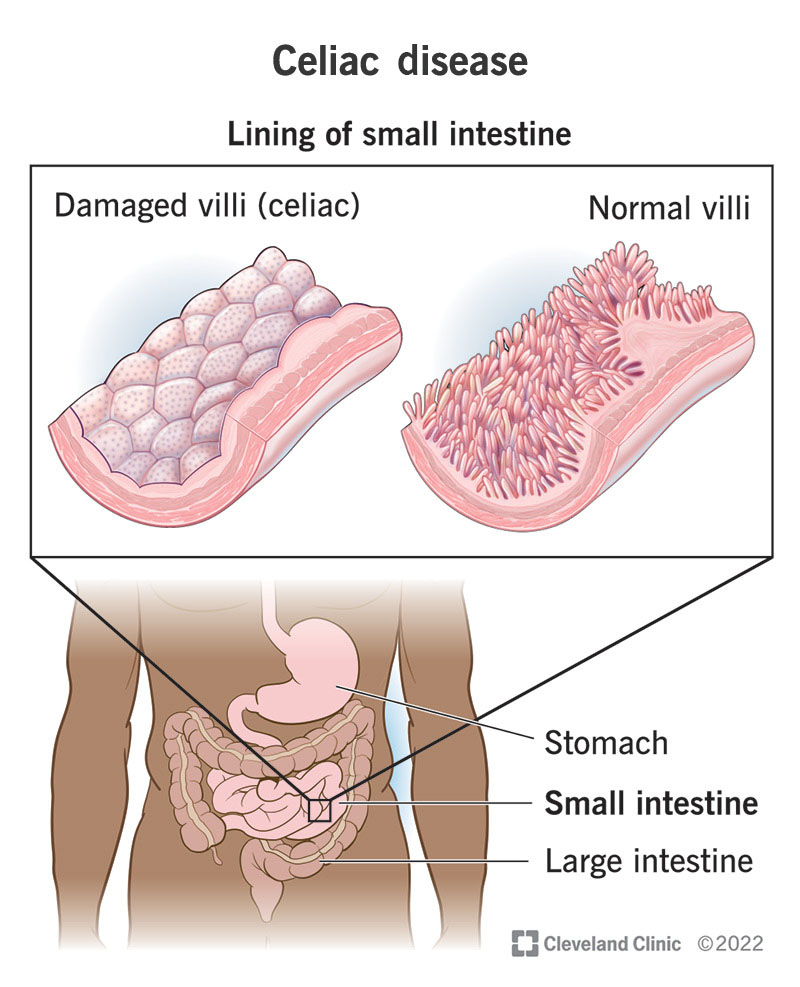
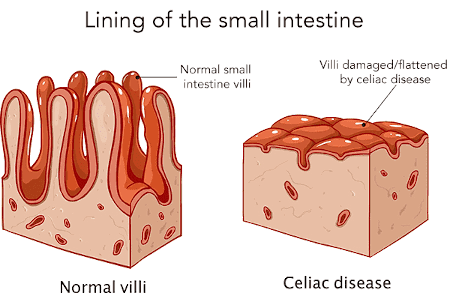
Celiac disease is an autoimmune disorder that affects the small intestine in response to gluten consumption. When individuals with celiac disease consume gluten, a protein found in wheat, barley, and rye, their immune system reacts by damaging the lining of the small intestine. This damage prevents the absorption of essential nutrients, leading to a range of symptoms and potential complications.
Prevalence and Symptoms of Celiac Disease
Celiac disease is more common than once believed and affects individuals of all ages and ethnicities. It is estimated that approximately 1 in 133 people in the United States have celiac disease, although many cases remain undiagnosed. Symptoms of celiac disease can vary greatly among individuals but commonly include abdominal pain, diarrhea, bloating, and fatigue. Other possible symptoms include weight loss, anemia, joint pain, and a skin rash known as dermatitis herpetiformis.
Understanding Gluten
What is Gluten?
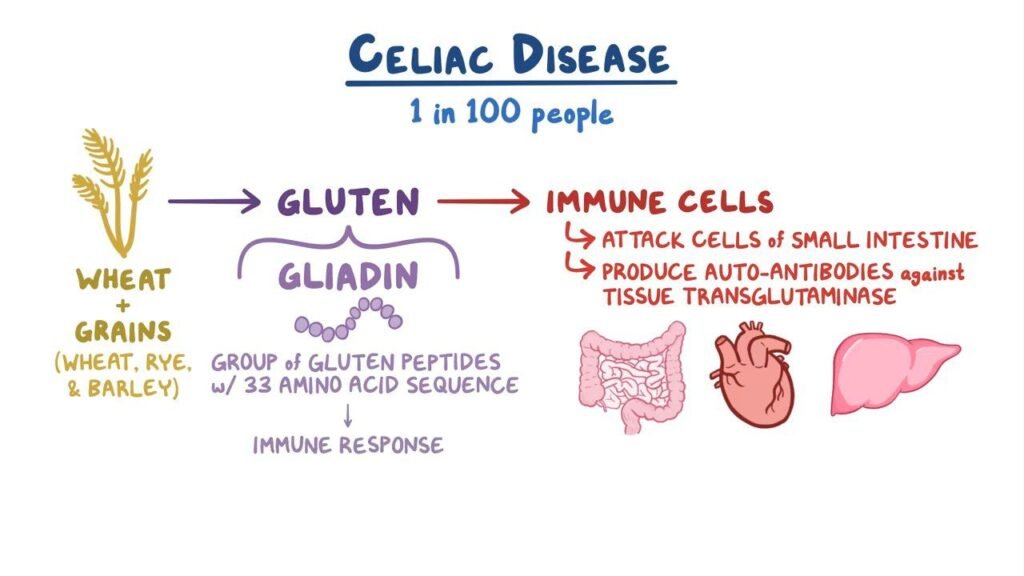
Gluten is a group of proteins found in grains such as wheat, barley, and rye. It provides elasticity to dough and gives bread its chewy texture. Gluten is composed of two main proteins, glutenin and gliadin, with gliadin being the component responsible for triggering the immune response in individuals with celiac disease.
Types of Gluten
There are different types of gluten found in various grains. Wheat gluten, composed of gliadin and glutenin, is the most common and problematic form of gluten for individuals with celiac disease. Barley and rye also contain gluten, with similar effects on those with the condition. Understanding the different types of gluten is important when navigating a gluten-free diet.
Sources of Gluten
Gluten can be found in a variety of foods and food products. It is commonly found in bread, pasta, cereals, and baked goods that contain wheat, barley, or rye. Additionally, gluten can be present in less obvious sources such as soups, sauces, processed meats, and even certain medications. It is crucial for individuals with celiac disease to carefully read food labels and be aware of potential hidden sources of gluten.

Mechanism of Gluten Intolerance in Celiac Disease
Immune Response to Gluten
In individuals with celiac disease, the immune system mistakenly identifies gluten as a threat and mounts an immune response. This immune response results in inflammation within the small intestine, leading to damage and subsequent malabsorption. The immune system reacts specifically to the gliadin component of gluten, causing the release of antibodies that attack the lining of the small intestine.
Role of Genetic Factors
Genetic factors play a significant role in the development of celiac disease. Individuals who have certain genetic markers, especially the human leukocyte antigen (HLA) genes, are more susceptible to developing celiac disease. However, not all individuals with these genetic markers will develop the condition, indicating that additional environmental factors may also be involved in the onset of celiac disease.
Diagnosis of Celiac Disease
Clinical Assessment and History
The diagnosis of celiac disease typically begins with a thorough clinical assessment and medical history. Healthcare professionals will inquire about symptoms, family history, and potential risk factors. It is crucial to provide accurate and detailed information to assist in the diagnostic process.
Serology Testing
Serology testing involves blood tests that look for specific antibodies associated with celiac disease. These antibodies, such as anti-tissue transglutaminase (tTG) and anti-endomysial (EMA) antibodies, are often elevated in individuals with the condition. Serology testing is a non-invasive and relatively reliable tool to aid in the diagnosis of celiac disease.
Endoscopic Biopsy
The gold standard for diagnosing celiac disease is an endoscopic biopsy of the small intestine. During this procedure, a small sample of tissue is taken from the lining of the small intestine and examined for characteristic changes associated with celiac disease, such as villous atrophy. This biopsy provides conclusive evidence of the condition and allows for accurate diagnosis and appropriate management.
Symptoms of Celiac Disease
Gastrointestinal Symptoms
Gastrointestinal symptoms are among the most common manifestations of celiac disease. These symptoms can vary from mild to severe and may include abdominal pain, bloating, gas, diarrhea, and constipation. In some cases, these symptoms can be mistaken for other gastrointestinal disorders, underscoring the importance of proper diagnosis.
Extraintestinal and Atypical Symptoms
Celiac disease can also exhibit extraintestinal symptoms, meaning symptoms that extend beyond the gastrointestinal tract. These symptoms can affect various organs and systems, including the skin, bones, nervous system, and reproductive organs. Atypical symptoms such as fatigue, anemia, dental enamel defects, and short stature may also be present. It is crucial to be aware of these potential symptoms to ensure early detection and appropriate management.
Potential Complications of Celiac Disease
Malabsorption and Nutritional Deficiencies
One of the most significant complications of celiac disease is malabsorption, which occurs due to the damage to the small intestine. Malabsorption can lead to deficiencies in essential nutrients such as iron, calcium, vitamin D, and B vitamins. These deficiencies can have far-reaching consequences on overall health, including the potential for anemia, osteoporosis, and developmental issues in children.
Osteoporosis and Bone Health
Individuals with untreated celiac disease are at an increased risk of developing osteoporosis and experiencing bone fractures. This increased risk is primarily due to malabsorption of calcium and vitamin D, essential nutrients for bone health. It is crucial for individuals with celiac disease to manage their condition effectively to minimize the risk of these long-term complications.
Increased Risk of Autoimmune Disorders
Celiac disease is associated with an increased risk of developing other autoimmune disorders. The exact mechanisms behind this association are not fully understood, but it is believed to be related to shared genetic factors and immune system dysregulation. Conditions such as type 1 diabetes, rheumatoid arthritis, thyroid disorders, and autoimmune liver diseases are more prevalent in individuals with celiac disease and should be monitored closely.

Gluten-Free Diet and Management of Celiac Disease
Strict Elimination of Gluten
The primary and most effective treatment for celiac disease is a strict gluten-free diet. This means completely eliminating all sources of gluten from the diet, including wheat, barley, and rye. Adopting and maintaining a gluten-free diet is essential to allow the small intestine time to heal and prevent further damage and symptoms.
Reading Food Labels for Hidden Gluten
Reading food labels is key to successfully managing a gluten-free diet. Many foods and food products may contain hidden sources of gluten, making label-reading essential. Look for terms such as “wheat,” “barley,” and “rye” in ingredient lists, and be aware of potential cross-contamination in manufacturing processes. Seeking out certified gluten-free products can provide added assurance.
Nutritional Considerations
When following a gluten-free diet, it is crucial to ensure adequate nutritional intake. Removing gluten-containing grains may result in decreased fiber, B vitamin, and iron intake. Incorporating alternative whole grains such as quinoa, amaranth, and millet, as well as a variety of fruits, vegetables, lean proteins, and healthy fats, can help address any potential nutritional gaps. Consulting with a registered dietitian experienced in celiac disease management is highly recommended.
Non-Celiac Gluten Sensitivity
Definition and Differentiation from Celiac Disease
Non-celiac gluten sensitivity, sometimes referred to as gluten intolerance, is a condition that shares some similarities with celiac disease but lacks the autoimmune response and damage to the small intestine. Individuals with non-celiac gluten sensitivity experience symptoms similar to those with celiac disease when consuming gluten, but do not test positive for celiac disease-specific antibodies or show intestinal damage.
Symptoms and Diagnosis
Symptoms of non-celiac gluten sensitivity can be similar to those of celiac disease, including gastrointestinal issues, fatigue, and joint pain. However, diagnosing non-celiac gluten sensitivity can be challenging, as there are no specific blood tests or intestinal biopsies that confirm the condition. The diagnosis is typically made through a process of exclusion, by ruling out celiac disease and wheat allergies.
Management Strategies
The primary management strategy for non-celiac gluten sensitivity is the avoidance of gluten-containing foods. While the symptoms can be debilitating in some cases, the long-term consequences and complications associated with celiac disease are not present. Individuals with non-celiac gluten sensitivity should work closely with a healthcare professional or registered dietitian to ensure a nutritionally balanced and sustainable gluten-free diet.
Research and Controversies
Advancements in Understanding Celiac Disease
Advancements in research have contributed to a better understanding of celiac disease and its various aspects. Studies have shed light on the genetic factors involved in the development of the condition, as well as the potential role of the gut microbiome and environmental triggers. Ongoing research continues to explore potential treatments and interventions to improve the quality of life for individuals with celiac disease.
Gluten Consumption and Non-Celiac Individuals
There is ongoing debate and controversy surrounding the effects of gluten consumption on individuals without celiac disease or non-celiac gluten sensitivity. Some individuals may report feeling better when following a gluten-free diet, even without a formal medical diagnosis. However, it is essential to differentiate between true gluten-related disorders and personal preferences or placebo effects. The impact of gluten consumption on non-celiac individuals is an area of active research.
Conclusion
Celiac disease is a complex autoimmune disorder characterized by an immune response to gluten consumption. With proper diagnosis and management, individuals with celiac disease can effectively control their symptoms and prevent potential complications. Understanding the mechanisms of gluten intolerance, adhering to a strict gluten-free diet, and seeking support from healthcare professionals are essential for maintaining optimal health and well-being. Ongoing research and advancements in understanding celiac disease will continue to expand our knowledge and improve the lives of those affected by this condition.