Imagine a mysterious illness that keeps striking with a vengeance, disappearing, and then striking again. This perplexing condition is called relapsing fever, and at its core lies the culprit: Borrelia recurrentis. With its ability to cause recurring bouts of sickness, understanding the role of this cunning bacterium is crucial in combating the disease. In this article, we will delve into the world of relapsing fever and explore the intricate role that Borrelia recurrentis plays in its relentless cycle. Get ready to uncover the secrets behind this puzzling ailment!

Overview of Relapsing Fever
Definition
Relapsing fever is an infectious disease caused by the bacterium Borrelia recurrentis. It is characterized by recurring episodes of high fever, hence the name “relapsing” fever. Unlike other types of fever, which tend to follow a consistent pattern, relapsing fever is marked by periods of fever that alternate with intervals of no fever. This cyclical nature of the disease makes it particularly challenging to diagnose and treat.
Causes
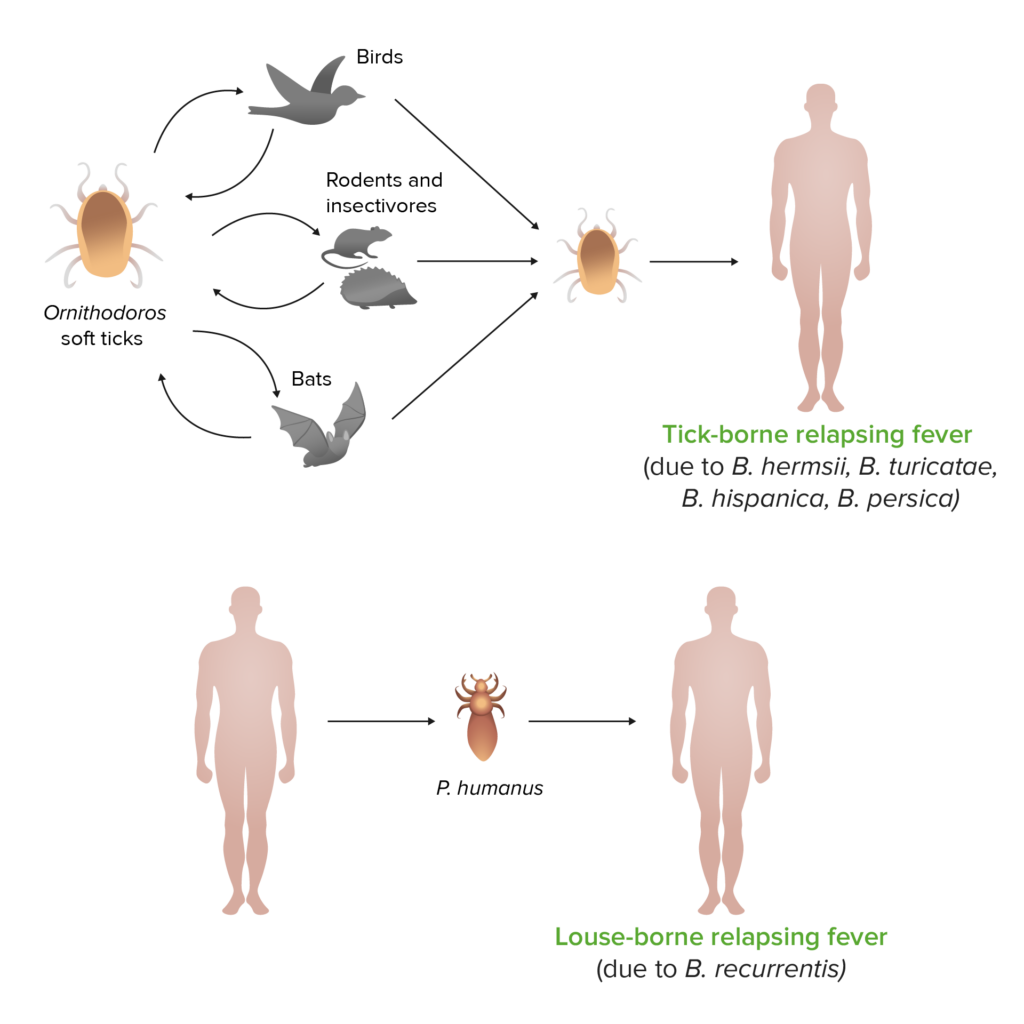
The primary cause of relapsing fever is infection with the bacterium Borrelia recurrentis. This spirochete bacterium is transmitted to humans through the bites of certain infected arthropods, such as ticks and lice. While the majority of cases are caused by the human body louse, known as Pediculus humanus humanus, there are also cases associated with tick-borne transmission. The bacterium can persist in the bloodstream for long periods of time, leading to recurrent bouts of fever.
Transmission
Relapsing fever is mainly transmitted through the bites of infected lice and ticks. When an infected arthropod feeds on a human host, the bacterium is introduced into the bloodstream. The bacteria then multiply within the host, leading to the characteristic symptoms of fever. When the infected arthropod feeds on another host, it can transmit the bacterium, continuing the cycle of infection.
Global Distribution
Relapsing fever is a global disease that has been documented in various parts of the world. Historically, it has been most prevalent in areas with poor sanitation and overcrowding, where lice infestations are more common. However, it can also occur in regions where ticks are abundant. Relapsing fever has been reported in Africa, Asia, Europe, and the Americas, with the highest burden of disease found in countries with limited resources and inadequate healthcare infrastructure.
Understanding Borrelia recurrentis
Introduction to Borrelia recurrentis
Borrelia recurrentis is the bacterium responsible for causing relapsing fever in humans. It belongs to the spirochete family, characterized by their long, thin, spiral-shaped appearance. Under a microscope, Borrelia recurrentis appears as a slender, coiled, and flexible organism. It has a unique ability to change the expression of its surface proteins, enabling it to evade the host’s immune system and persist in the bloodstream.
Morphology and Characteristics
Borrelia recurrentis is a highly motile bacterium, possessing a unique structure called an axial filament that allows it to move in a corkscrew-like manner. This enables the bacterium to navigate through various tissues and evade the host’s immune response. It is notably smaller in size compared to other Borrelia species, measuring about 18-30 micrometers in length and approximately 0.2 micrometers in width.
Genetic Makeup
The genetic makeup of Borrelia recurrentis is complex, with a relatively large genome compared to other spirochetes. Its genome contains numerous genes that contribute to its ability to evade the immune system and persist in the host. Additionally, it possesses a high degree of genetic variability, which plays a significant role in the disease dynamics and the development of antibiotic resistance.
Pathogenesis
The pathogenesis of Borrelia recurrentis involves a multifaceted interaction between the bacterium and the host’s immune system. Upon entering the human body through the bite of an infected arthropod, the bacterium rapidly disseminates to different organs, including the liver, spleen, and central nervous system. This widespread dissemination triggers an immune response by the host, leading to the characteristic symptoms of fever and inflammation. The bacterium’s ability to modify the expression of its surface proteins allows it to avoid detection by the immune system, leading to chronic infection and the potential for relapses.

Clinical Presentation and Symptoms
Early Symptoms
The onset of relapsing fever is usually abrupt, with symptoms appearing within a week of infection. The initial signs often include high fever, severe headache, muscle aches, and chills. Patients may also experience fatigue, weakness, and nausea. These early symptoms can be mistaken for other common febrile illnesses, making it important for healthcare providers to consider relapsing fever in regions where the disease is prevalent.
High Fever and Relapse
The hallmark of relapsing fever is the recurrence of high fever after a period of remission. This cyclical pattern is due to the bacterium’s ability to periodically change its surface proteins, allowing it to evade the immune response mounted by the host. Each relapse is characterized by a sudden onset of high fever, often reaching 39-40 degrees Celsius or higher, accompanied by other symptoms such as headache, muscle pain, and malaise.
Additional Manifestations
In addition to fever, relapsing fever can present with other manifestations depending on the severity and duration of the infection. Patients may develop a skin rash, enlarged lymph nodes, and splenomegaly (enlarged spleen). Some individuals may also experience chest pain, cough, and respiratory symptoms. In severe cases, complications such as jaundice, liver dysfunction, and neurological abnormalities can occur.
Complications
Although rare, relapsing fever can lead to serious complications if left untreated or if the infection is severe. Neurological complications, including meningitis and encephalitis, can occur due to the invasion of the central nervous system by the bacterium. Severe liver damage, known as Weil’s disease, can also develop, resulting in jaundice, hepatic failure, and kidney dysfunction. If untreated, relapsing fever can be fatal, particularly in individuals who are immunocompromised or have other underlying health conditions.
Diagnosis of Relapsing Fever
Clinical Evaluation
Diagnosing relapsing fever can be challenging due to its non-specific symptoms and the lack of specific diagnostic tests in resource-limited settings. Healthcare providers rely primarily on clinical evaluation, taking into account the patient’s history, symptoms, and potential exposure to infected vectors. In regions where relapsing fever is endemic, a high index of suspicion is crucial for prompt diagnosis and treatment.
Microscopic Examination
Microscopic examination of a blood smear is one of the key diagnostic tools for relapsing fever. During the febrile episodes, Borrelia recurrentis can be observed in the peripheral blood, where it appears as long, thin organisms known as spirochetes. Darkfield microscopy or Wright-Giemsa staining can enhance the visibility of the spirochetes, aiding in their identification.
PCR Testing
Polymerase chain reaction (PCR) testing is a sensitive and specific method for detecting the presence of Borrelia recurrentis DNA in clinical samples. This molecular technique amplifies specific regions of the bacterial genome, allowing for rapid and accurate diagnosis. PCR testing can be particularly useful when the organism cannot be visualized in blood smears or when a definitive diagnosis is required.
Serological Testing
Serological testing, such as enzyme-linked immunosorbent assay (ELISA) or indirect immunofluorescence assay (IFA), can be used to detect antibodies produced by the host in response to Borrelia recurrentis infection. Serological tests are especially useful during the convalescent phase of the infection, when the bacterium may no longer be present in the bloodstream. A rise in antibody titers between acute and convalescent samples can confirm the diagnosis.
Management and Treatment
Antibiotic Therapy
Effective antibiotic treatment is crucial for the management of relapsing fever. The choice of antibiotic depends on the severity of the infection and the susceptibility of the bacterium to specific drugs. Tetracyclines, such as doxycycline, and macrolides, such as azithromycin, are commonly used as first-line treatment options. In severe cases or when there is a suspicion of meningitis, intravenous antibiotics, such as penicillin G or ceftriaxone, may be necessary.
Special Considerations
Pregnant women, children, and individuals with underlying health conditions may require special considerations in the management of relapsing fever. The safety and efficacy of certain antibiotics during pregnancy and in pediatric populations should be carefully evaluated. Close monitoring of vital signs, hydration status, and organ function is essential in severe cases to ensure appropriate supportive care.
Prevention and Control
Prevention and control strategies for relapsing fever primarily focus on reducing exposure to infected lice or ticks. This involves maintaining good personal hygiene, regularly washing clothes and bedding, and ensuring proper sanitation practices. In regions where louse-borne transmission is predominant, efforts to control lice infestations through insecticidal treatments and improved living conditions can help reduce the risk of transmission.
Role of Public Health Agencies
Public health agencies play a crucial role in the surveillance, prevention, and control of relapsing fever. These agencies work closely with healthcare providers to monitor the incidence and prevalence of the disease, investigate outbreaks, and implement control measures. They also play a vital role in educating the public, healthcare professionals, and policymakers about the importance of early detection and appropriate management of relapsing fever.
Epidemiology and Burden of Disease
Historical Significance
Relapsing fever has a long history of causing significant morbidity and mortality, particularly in regions with poor living conditions and limited access to healthcare. Outbreaks of relapsing fever have been documented throughout history, including the devastating epidemics during times of war and displacement. The disease has left a lasting impact on the health and wellbeing of affected populations, underscoring the need for continued efforts to eliminate and control the disease.
Current Incidence and Prevalence
Relapsing fever continues to be a public health concern in certain regions of the world. The exact incidence and prevalence of the disease are challenging to determine due to underreporting and limited surveillance systems in resource-limited settings. However, it is estimated that tens of thousands of cases occur annually, with the majority of cases reported in Africa.
Outbreaks and Global Health Impact
Outbreaks of relapsing fever can have significant health and socioeconomic impacts on affected communities. The sudden increase in cases overwhelms healthcare systems, leading to a higher burden of disease and increased mortality. Outbreaks of relapsing fever in vulnerable populations, such as refugees and internally displaced persons, further exacerbate the already challenging circumstances faced by these individuals.
Risk Factors for Transmission
Several risk factors contribute to the transmission of relapsing fever. Poor sanitation, overcrowding, and lack of access to healthcare facilities are significant factors that increase the risk of lice infestations and subsequent transmission. Vector control measures, such as the use of insecticides and insecticide-treated bed nets, are crucial for reducing the risk of tick-borne transmission and minimizing the overall burden of disease.

Relationship with Lice and Human Body Lice
Introduction to Lice
Lice are small, wingless insects that infest the human body, particularly the hair and clothing. They are obligate parasites, relying on human blood for survival and reproduction. Lice infestations are a significant public health concern, as they can transmit several diseases, including relapsing fever.
Role of Lice in Transmission
The human body louse, Pediculus humanus humanus, plays a critical role in the transmission of Borrelia recurrentis. When an infected louse feeds on a human host, the bacterium is ingested into the louse’s gut. The bacterium then multiplies within the louse and can be transmitted to another human host through louse bites or contact with louse feces.
Impact on Disease Dynamics
The relationship between lice and Borrelia recurrentis is crucial for the dynamics of relapsing fever. Lice infestations provide a conducive environment for the bacterium to persist and replicate, allowing for efficient transmission to new hosts. Understanding the ecology and behavior of lice is essential for developing effective control strategies to interrupt the transmission cycle and reduce the burden of relapsing fever.
Efforts for Louse Control
Efforts to control lice infestations involve a multifaceted approach that focuses on both personal and environmental measures. Personal hygiene practices, such as regular bathing and laundering of clothes, can help reduce the risk of lice infestations. Insecticidal treatments, such as shampoos or creams containing pediculicides, are commonly used to kill lice and their eggs. Environmental measures, such as improving living conditions and implementing insecticide spraying in high-risk areas, also contribute to louse control efforts.
Host-Pathogen Interactions
Mechanisms of Transmission
The transmission of Borrelia recurrentis relies on the interaction between the bacterium, its arthropod vector, and the human host. After entering the human body through the bite of an infected arthropod, the bacterium evades the host’s immune system and disseminates to various organs. The arthropod vector plays a crucial role in the transmission of the bacterium, as it allows for the maintenance and amplification of the infection within the population.
Immune Response to Borrelia recurrentis
Upon infection with Borrelia recurrentis, the host’s immune system mounts a complex response to eliminate the bacterium. This includes the activation of both innate and adaptive immune responses. Innate immune cells, such as neutrophils and macrophages, are the first line of defense against the bacterium, while adaptive immune cells, such as T and B cells, produce specific antibodies and eliminate the infection. However, Borrelia recurrentis employs various strategies to evade and manipulate the host’s immune response, allowing for its persistence and relapses.
Immune Evasion Strategies
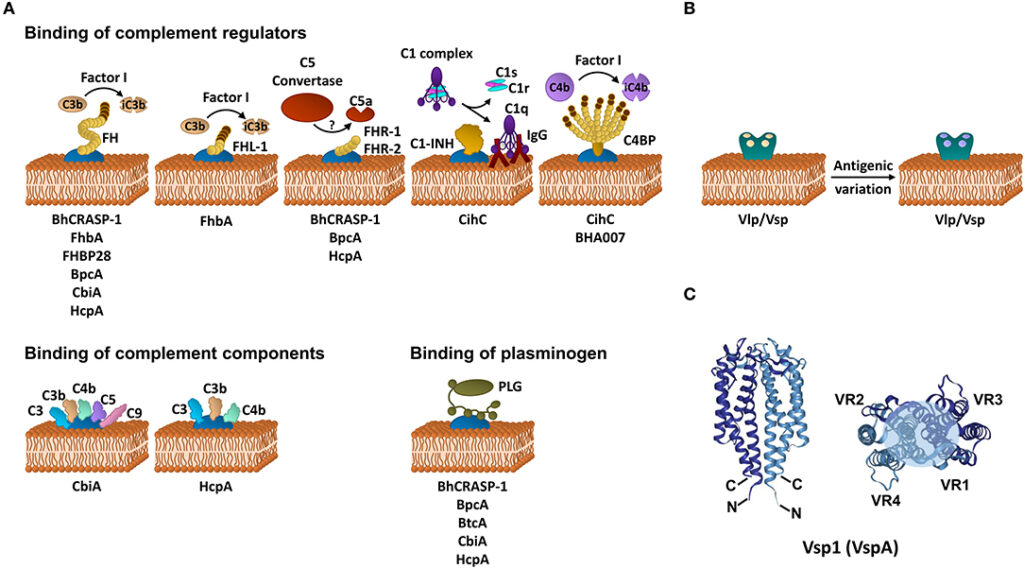
Borrelia recurrentis utilizes several immune evasion strategies to avoid detection by the host’s immune system. One of the key mechanisms is antigenic variation, through which the bacterium changes the expression of its surface proteins. This phenomenon allows the bacterium to stay one step ahead of the host’s immune response, as it continually presents new antigens that the immune system has not encountered before. By constantly changing its surface proteins, Borrelia recurrentis can avoid recognition and elimination by the host’s immune cells.
Role of Innate and Adaptive Immunity
Both innate and adaptive immune responses play important roles in controlling and resolving Borrelia recurrentis infection. Innate immune cells, such as neutrophils and macrophages, are involved in the initial recognition and phagocytosis of the bacterium. They also produce pro-inflammatory molecules to recruit other immune cells to the site of infection. Adaptive immune cells, including T and B cells, recognize and respond to specific antigens present on the surface of the bacterium. B cells produce antibodies that neutralize the bacterium, while T cells coordinate the immune response and help eliminate infected cells. Deficiencies in either innate or adaptive immunity can lead to persistent infection and an increased risk of relapses.
Genetic Variability and Resistance
Genetic Diversity in B. recurrentis
Borrelia recurrentis exhibits a high degree of genetic diversity, which contributes to its ability to persist and cause relapsing fever. The bacterium possesses a large number of genes responsible for antigenic variation, allowing it to change its surface proteins and evade the host’s immune response. This genetic variability plays a significant role in disease dynamics, as it enables the bacterium to adapt to changing environments and host immune pressures.
Impact on Disease Dynamics
The genetic diversity of Borrelia recurrentis has important implications for the epidemiology and clinical presentation of relapsing fever. The ability of the bacterium to generate new antigenic variants enables it to cause multiple episodes of fever and relapse, making the disease challenging to diagnose and treat. Additionally, genetic variability can influence the severity of the infection, the immune response mounted by the host, and the development of antibiotic resistance.
Antibiotic Resistance
Antibiotic resistance can emerge in populations of Borrelia recurrentis, which poses a significant challenge for the treatment of relapsing fever. The genetic variability of the bacterium allows it to acquire and transfer resistance genes, rendering certain antibiotics ineffective. This highlights the importance of appropriate antibiotic stewardship and surveillance systems to monitor the development and spread of antibiotic resistance among Borrelia recurrentis strains.
Implications for Treatment Strategies
The genetic variability of Borrelia recurrentis has implications for the development of treatment strategies. The use of combination antibiotic therapy, targeting different mechanisms of action, can help overcome the potential for resistance and improve treatment outcomes. Long-term surveillance of circulating strains and their susceptibility to antibiotics is crucial for guiding treatment decisions and ensuring the effectiveness of therapeutic interventions.
Research and Future Directions
Advances in Diagnostic Techniques
Advances in diagnostic techniques are essential for improving the timely and accurate diagnosis of relapsing fever. Ongoing research focuses on the development of rapid point-of-care tests that can detect specific antigens or antibodies associated with Borrelia recurrentis. These tests would enable healthcare providers in resource-limited settings to diagnose the disease quickly and initiate appropriate treatment.
Development of Vaccines
The development of vaccines against Borrelia recurrentis is an area of active research. Vaccines could provide long-term immunity and prevent relapses and complications associated with the disease. Several vaccine candidates targeting the surface proteins of the bacterium are currently under investigation, although significant challenges remain in terms of safety, efficacy, and implementation.
Understanding the Pathogenesis
Further research into the pathogenesis of relapsing fever is necessary to elucidate the mechanisms by which Borrelia recurrentis interacts with the human host. This includes studying the genetic and molecular factors involved in immune evasion, dissemination, and relapse. A better understanding of these mechanisms will aid in the development of targeted therapeutic interventions and preventive strategies.
Surveillance and Control Efforts
Surveillance and control efforts are crucial for reducing the burden of relapsing fever and preventing outbreaks. Ongoing research focuses on improving surveillance systems and implementing integrated control programs targeting both human hosts and arthropod vectors. These efforts aim to interrupt the transmission cycle, reduce the prevalence of lice and ticks, and ultimately eliminate relapsing fever as a public health threat.
In conclusion, relapsing fever caused by Borrelia recurrentis is a challenging infectious disease with a complex host-pathogen interaction. Understanding the epidemiology, clinical presentation, and genetic variability of the bacterium is crucial for accurate diagnosis, effective treatment, and the development of preventive measures. Ongoing research and collaborative efforts among healthcare providers, researchers, and public health agencies are necessary to combat relapsing fever and reduce its global burden.