Vulval cancer, a lesser-known and often misunderstood form of cancer, is a condition that specifically affects the external female genitalia. It is crucial to shed light on this topic, as being informed about vulval cancer can help raise awareness and understanding of the risks, symptoms, and treatment options. In this article, you will gain valuable insights into the various aspects of vulval cancer, empowering you with the knowledge to support yourself or someone you care about who may be experiencing this condition.

Overview of Vulval Cancer
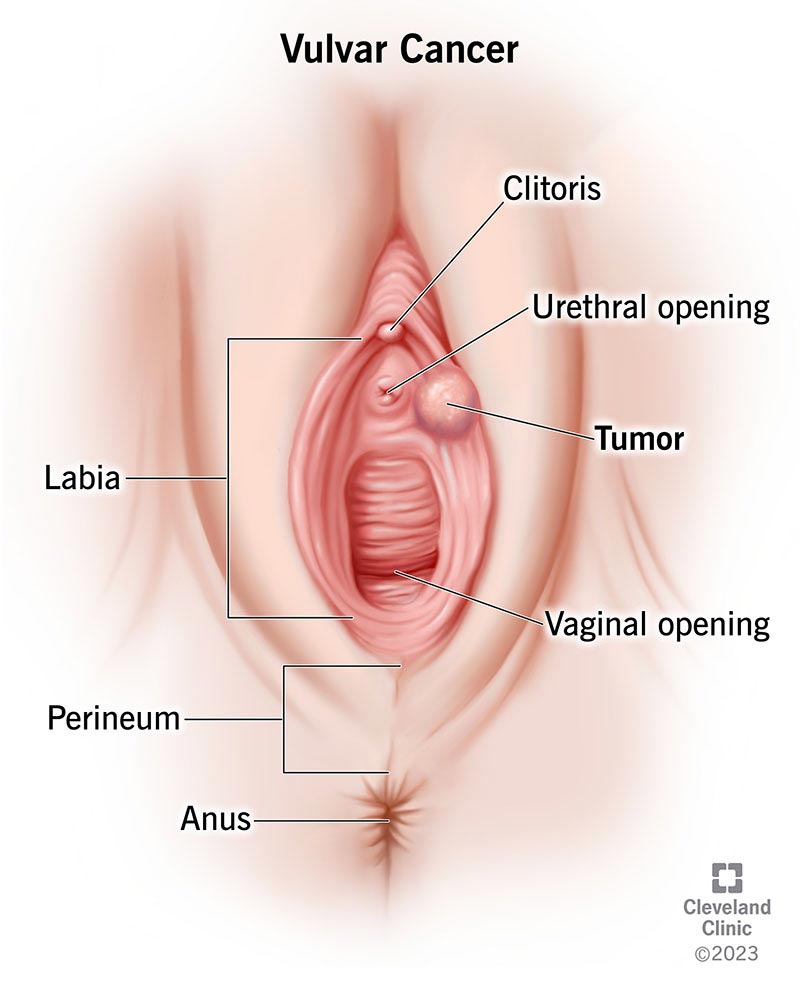
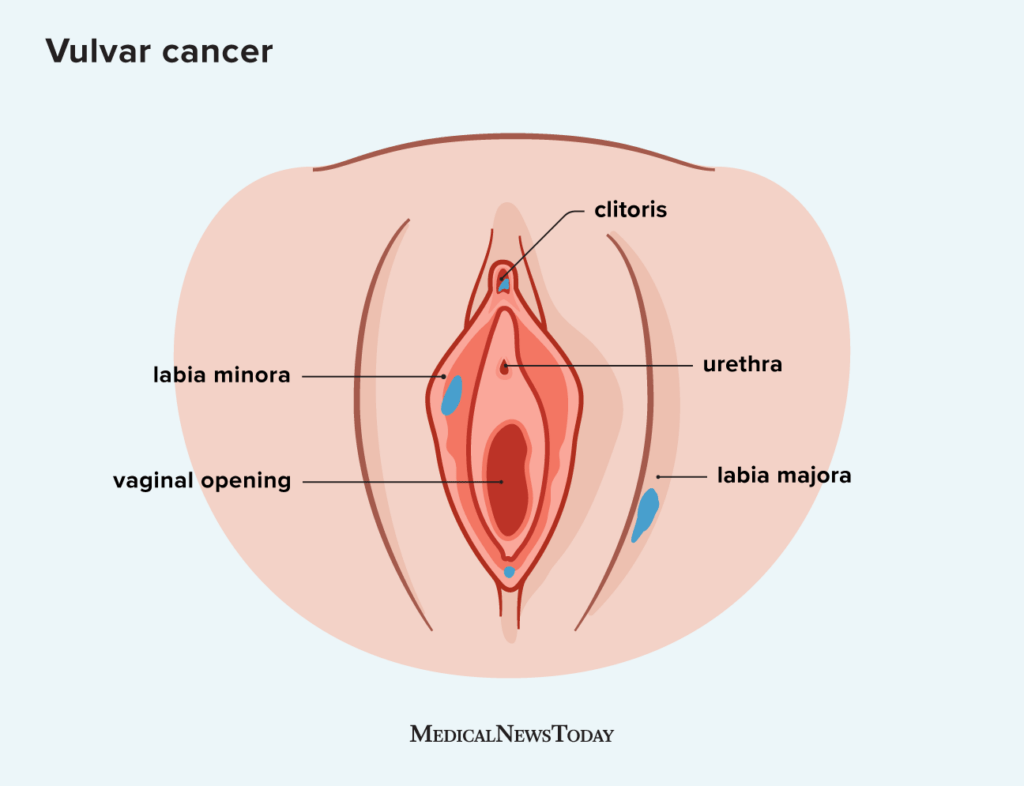
Vulval cancer is a type of cancer that occurs in the vulva, the external female genitalia. The vulva includes the labia majora, labia minora, clitoris, vaginal opening, and the opening of the urethra. Vulval cancer is a relatively rare cancer, accounting for about 4% of all gynecologic cancers. However, it is important to be aware of this condition as early detection and treatment can greatly improve outcomes.
Definition
Vulval cancer refers to the abnormal, uncontrolled growth of cells in the tissues of the vulva. These cancerous cells can invade nearby tissues and spread to other parts of the body if not treated. There are different types of vulval cancer, including squamous cell carcinoma, vulvar melanoma, basal cell carcinoma, and adenocarcinoma. Each type has its own characteristics and treatment approaches.
Prevalence
Vulval cancer is considered a rare cancer, with an estimated incidence rate of about 2 per 100,000 women per year. It typically occurs in older women, with the average age at diagnosis being around 65 years. However, it can also affect younger women, especially those with risk factors such as human papillomavirus (HPV) infection or a history of smoking.
Risk Factors
Several factors can increase the risk of developing vulval cancer. These include:
- HPV infection: Certain strains of HPV, such as HPV 16 and 18, can increase the risk of vulval cancer.
- Smoking: Women who smoke are at a higher risk of developing vulval cancer compared to non-smokers.
- Age: The risk of vulval cancer increases with age, particularly in women over the age of 60.
- Immunosuppression: Weakened immune system, due to conditions like HIV/AIDS or organ transplantation, can increase the risk of developing vulval cancer.
Signs and Symptoms of Vulval Cancer
Early detection of vulval cancer is crucial for effective treatment. Being aware of the signs and symptoms can help women seek medical attention promptly. The symptoms of vulval cancer can vary depending on the stage of the disease.
Early signs
In the early stages of vulval cancer, women may experience:
- Persistent itching or pain in the vulval area
- Changes in the color or texture of the skin, such as thickened or scaly areas
- A lump or bump that may be felt in the vulva
- Bleeding or discharge that is not related to menstruation
- Ulcers or sores that do not heal
Advanced signs
As vulval cancer progresses, additional symptoms may arise, including:
- Painful intercourse
- Swollen lymph nodes in the groin area
- Changes in bladder or bowel habits
- Weight loss without an apparent reason
Associated symptoms
Some women with vulval cancer may also experience associated symptoms, such as:
- Fatigue and lack of energy
- Loss of appetite
- Anemia (low red blood cell count)
- Generalized discomfort or malaise
It is important to note that these symptoms may be caused by other conditions as well, so it is essential to consult a healthcare professional for a proper diagnosis.
Types of Vulval Cancer
Vulval cancer can be classified into different types based on the specific cells involved. The most common types include:
Squamous cell carcinoma
Squamous cell carcinoma is the most prevalent type of vulval cancer, accounting for about 80-90% of cases. It usually originates in the surface layer of the vulva, known as the squamous epithelium. Squamous cell carcinoma often develops slowly over time and can be associated with HPV infection.
Vulvar melanoma
Vulvar melanoma is a rare form of vulval cancer that originates in the cells that produce pigment (melanocytes) in the skin. It accounts for around 4% of vulval cancers. Vulvar melanoma is often more aggressive and has a poorer prognosis compared to other types of vulval cancer.
Basal cell carcinoma
Basal cell carcinoma is a rare type of vulval cancer that starts in the basal cells of the epidermis, which is the outermost layer of the skin. It is typically slow-growing and has a relatively good prognosis. Basal cell carcinoma accounts for approximately 5% of vulval cancers.
Adenocarcinoma
Adenocarcinoma is a less common type of vulval cancer that develops in the glandular cells of the vulva. It tends to occur in older women and can be more difficult to detect and diagnose. Adenocarcinoma accounts for about 2-5% of vulval cancers.
Causes and Prevention of Vulval Cancer
The development of vulval cancer can be influenced by various factors, some of which can be prevented. Understanding these causes and taking preventive measures can contribute to a reduced risk of developing vulval cancer.
HPV infection
Human papillomavirus (HPV) infection is a significant risk factor for vulval cancer. Certain high-risk strains of HPV, such as types 16 and 18, have been linked to the development of vulval cancer. Practicing safe sex, including the consistent use of condoms and receiving the HPV vaccine, can help reduce the risk of HPV infection.
Smoking
Smoking is another well-established risk factor for vulval cancer. The chemicals in tobacco smoke can damage the DNA in the vulval cells, increasing the risk of cancer development. Quitting smoking or never starting can significantly reduce the risk of vulval cancer and improve overall health.
Age
The risk of vulval cancer increases with age, particularly in women over the age of 60. Regular gynecologic check-ups and screenings can help detect any abnormalities in the vulvar area and facilitate early diagnosis.
Immunosuppression
Having a weakened immune system, such as in cases of HIV/AIDS or organ transplantation, can increase the risk of developing vulval cancer. Maintaining a strong immune system through a healthy lifestyle, adequate rest, and managing underlying medical conditions can help reduce the risk.
Prevention methods
Although it may not be possible to prevent vulval cancer entirely, adopting certain preventive measures can reduce the risk:
- Practicing safe sex: Using condoms and getting vaccinated against HPV can lower the risk of HPV infection.
- Quitting smoking: Avoiding or quitting smoking can significantly reduce the risk of vulval cancer and other health complications.
- Maintaining good hygiene: Regularly washing the vulvar area with gentle soap and water can help maintain cleanliness and reduce the risk of infections.
It is important to consult with a healthcare professional for personalized advice on risk factors and appropriate preventive measures.
Diagnosis of Vulval Cancer
Diagnosing vulval cancer usually involves a combination of physical examination, biopsies, and imaging tests. Early detection and accurate diagnosis are crucial in determining the best treatment options and outcomes.
Physical examination
During a physical examination, the healthcare provider will visually inspect the vulva for any abnormalities, such as lumps, changes in color or texture, or ulcerations. They may also check for swollen lymph nodes in the groin area, as this can indicate the spread of cancer.
Biopsy
If any suspicious lesions or abnormalities are found during the physical examination, a biopsy will be performed. A biopsy involves removing a small sample of tissue from the affected area for laboratory analysis. This sample will be examined by a pathologist to determine if cancer or precancerous changes are present.
Imaging tests
Imaging tests, such as computed tomography (CT) scans, magnetic resonance imaging (MRI), or positron emission tomography (PET) scans, may be done to determine the extent of the cancer and if it has spread to other parts of the body. These tests can help determine the stage of the cancer and guide treatment decisions.
Staging and Prognosis of Vulval Cancer
Staging is an essential part of determining the extent and spread of vulval cancer. It helps healthcare professionals devise a treatment plan and predict the likely outcome or prognosis.
TNM staging system
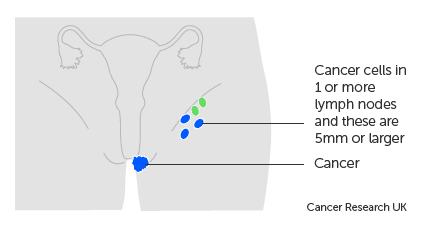
The TNM staging system is commonly used to stage vulval cancer. It categorizes cancer based on the size of the tumor (T), the involvement of nearby lymph nodes (N), and the presence of distant metastasis (M). The stages range from 0 (early-stage) to IV (advanced-stage), with subcategories within each stage.
Prognostic factors
Several factors can influence the prognosis of vulval cancer, including the stage of the cancer, tumor size, lymph node involvement, histological grade, and presence of distant metastasis. Additionally, factors such as the age and overall health of the individual can also impact the prognosis. Timely diagnosis and appropriate treatment can significantly improve the prognosis of vulval cancer.
Treatment Options for Vulval Cancer
The treatment approach for vulval cancer depends on various factors, including the type and stage of the cancer, as well as the individual’s overall health and personal preferences. Treatment options may include surgery, radiation therapy, chemotherapy, targeted therapy, or a combination of these approaches.
Surgery
Surgery is usually the primary treatment for vulval cancer. The extent of surgery will depend on the stage and location of the cancer. In early-stage cases, the tumor may be removed through local excision or wide local excision. In more advanced cases, a radical vulvectomy, which involves the removal of a larger portion of the vulva, may be necessary. In some cases, surgical reconstruction may be performed to restore the appearance and function of the vulva.
Radiation therapy
Radiation therapy uses high-energy beams to kill cancer cells and shrink tumors. It may be used before surgery (neoadjuvant therapy) to reduce the size of the tumor, after surgery (adjuvant therapy) to destroy any remaining cancer cells, or as the primary treatment for inoperable cases. Radiation therapy may be delivered externally or internally (brachytherapy) based on the specific needs of the individual.
Chemotherapy
Chemotherapy involves the use of drugs to kill cancer cells or stop their growth. It may be used in combination with surgery or radiation therapy, especially for advanced or recurrent cases. Chemotherapy can be administered orally, intravenously, or through other methods, depending on the specific drugs used and the individual’s condition.
Targeted therapy
Targeted therapy is a type of treatment that targets specific molecules or pathways involved in cancer growth. It is often used in cases where the cancer has specific genetic mutations or certain protein markers. Targeted therapy can be used in combination with other treatments or as a standalone option, depending on the individual’s specific circumstances.
The choice of treatment will be determined by a multidisciplinary team of healthcare professionals based on the individual’s specific situation and preferences.
Supportive Care for Vulval Cancer Patients
Managing the side effects and addressing the emotional and physical needs of individuals with vulval cancer is an important part of their overall care. Supportive care aims to improve the well-being and quality of life of patients throughout the treatment journey.
Pain management
Pain management is crucial for individuals with vulval cancer, especially during and after surgery or radiation therapy. Various approaches may be used, including medications, nerve blocks, topical treatments, or complementary therapies such as acupuncture or massage. It is important for individuals to communicate any pain or discomfort to their healthcare team so that appropriate measures can be taken.
Emotional support
A diagnosis of vulval cancer can be emotionally challenging for individuals and their loved ones. Emotional support can be provided through individual counseling, support groups, or online resources. It is important to address any feelings of anxiety, fear, or depression and to seek help when needed.
Rehabilitation
Rehabilitation may be necessary after surgery or other treatments for vulval cancer. Physical therapy and exercises can help regain strength, mobility, and function in the vulvar area. Rehabilitation specialists can provide guidance and support in this process.
Clinical Trials and Research
Clinical trials are important avenues for advancing the understanding and treatment of vulval cancer. These trials involve the evaluation of new treatments, medications, or therapeutic approaches in a controlled research setting.
Current research
Current research focuses on identifying better treatment strategies for vulval cancer, including novel targeted therapies, immunotherapy, and personalized medicine approaches. Researchers are also investigating the role of genetic mutations and molecular markers in predicting treatment response and outcomes.
Clinical trial participation
Participating in a clinical trial may be an option for individuals with vulval cancer. Clinical trials can offer access to innovative treatments or therapies that are not yet widely available. It is important to discuss the potential benefits and risks of participating in a clinical trial with a healthcare professional before making a decision.
Living with Vulval Cancer
Living with vulval cancer requires adjustments and coping strategies to manage the physical, emotional, and practical aspects of the condition. It is important to remember that each individual’s experience will be unique, and what works for one person may not work for another.
Coping strategies
Coping strategies can help individuals navigate the challenges of living with vulval cancer. These may include seeking support from loved ones, joining support groups, managing stress through relaxation techniques or hobbies, or seeking professional counseling. It is also helpful to maintain open and honest communication with healthcare providers and voice any concerns or questions.
Quality of life
Maintaining a good quality of life is important for individuals living with vulval cancer. This may involve making healthy lifestyle choices, engaging in activities that bring joy or relaxation, and taking care of overall physical and mental well-being. It is important to find a balance between self-care and receiving appropriate medical care.
Follow-up care
Regular follow-up appointments with healthcare providers are essential for monitoring the progress of vulval cancer and addressing any potential issues or concerns. Follow-up care may include physical exams, imaging tests, blood work, and discussions about treatment options or side effect management.
Support groups
Joining support groups or connecting with others who have experienced vulval cancer can provide immense emotional support. Support groups can offer a safe space to share experiences, obtain information, and find comfort in the knowledge that others have gone through similar challenges.
In conclusion, vulval cancer is a relatively rare but significant condition that requires understanding, early detection, and appropriate treatment. By being aware of the signs and symptoms, risk factors, and available treatment options, individuals and healthcare professionals can work together to improve outcomes and support those affected by vulval cancer. Regular check-ups, healthy lifestyle choices, and an open dialogue with healthcare providers are vital in reducing the risk and managing the impact of vulval cancer.
Overall, it is important to approach the topic of vulval cancer with empathy, compassion, and a commitment to raising awareness and supporting those affected by this condition.