Unraveling the Complexities of Angioedema: A Comprehensive Guide is your go-to resource for understanding the intricate nature of this perplexing condition. Delving into the depths of angioedema, this comprehensive guide serves as a compass in navigating through the complexities and intricacies of its symptoms, causes, and treatments. Whether you’re seeking answers for yourself or a loved one, this guide offers a friendly and comprehensive overview that will leave you equipped with knowledge and understanding to tackle angioedema head-on.
Understanding Angioedema
Angioedema is a condition characterized by the swelling of the deep layers of the skin and underlying tissues. It typically affects areas such as the face, lips, tongue, throat, and genitalia. This condition is often sudden and can cause discomfort, pain, and changes in appearance. It is important to understand the different types of angioedema, its causes, prevalence, and risk factors in order to effectively recognize, diagnose, and manage this condition.
Definition and Overview
Angioedema is a form of localized edema that affects the deep layers of the skin and submucosal tissues. It involves the dilation and increased permeability of blood vessels, leading to fluid accumulation in the affected areas. This results in swelling and inflammation, which can occur in isolation or as a part of a more systemic allergic reaction. The areas commonly affected are the face, lips, tongue, throat, and genitalia.
Types of Angioedema
There are different types of angioedema, each with its own unique characteristics and underlying causes. The main types include:
-
Allergic Angioedema: This type is triggered by an allergic reaction to specific allergens such as food, medication, insect bites, or environmental factors. It is commonly associated with hives and often occurs within minutes to hours after exposure to the triggering allergen.
-
Hereditary Angioedema (HAE): HAE is a rare, genetic form of angioedema that is caused by a deficiency or dysfunction of certain proteins involved in regulating blood vessel permeability. It typically presents with recurrent episodes of angioedema, which can be triggered by stress, trauma, hormonal changes, or certain medications.
-
Acquired Angioedema: Unlike HAE, acquired angioedema is not hereditary and is usually associated with underlying medical conditions such as autoimmune disorders, lymphoproliferative disorders, or certain cancers. It can also be triggered by medications or infections.
-
Idiopathic Angioedema: This form of angioedema is characterized by recurrent episodes of swelling without an identifiable cause. It can be challenging to diagnose and manage, as the underlying trigger is unknown.
Causes of Angioedema
Angioedema can have various causes, depending on the type. Allergic angioedema is primarily caused by an allergic reaction to specific triggers, such as certain foods, medications, insect bites, or environmental factors like pollen. Hereditary angioedema results from genetic abnormalities that affect the production or function of proteins involved in regulating blood vessel permeability. Acquired angioedema can occur as a result of underlying medical conditions, certain medications, or infections. The exact cause of idiopathic angioedema remains unknown, making it a challenge to manage effectively.
Prevalence and Risk Factors
Angioedema is not uncommon, with estimates suggesting that it affects approximately 15-20% of the population at some point during their lifetime. It can affect individuals of all ages, genders, and ethnicities. However, certain risk factors may increase the likelihood of developing angioedema. These include a personal or family history of angioedema, a history of allergies or allergic conditions, exposure to known triggers, and certain medical conditions such as autoimmune disorders or lymphoproliferative disorders. It is crucial to be aware of these risk factors to effectively manage and prevent angioedema episodes.
Recognizing Symptoms
In order to effectively manage angioedema, it is essential to recognize and distinguish its symptoms from those of other conditions. Angioedema can present in localized or systemic forms, and its symptomatology may vary depending on the individual and underlying cause.
Localized vs. Systemic Angioedema
Localized angioedema primarily affects specific areas of the body, such as the face, lips, tongue, or throat. The swelling is typically asymmetrical and may be accompanied by redness, warmth, and itching. Systemic angioedema, on the other hand, involves the swelling of deeper tissues and organs, such as the digestive system, respiratory system, or genitalia. This can be life-threatening if it affects the airway or causes digestive complications.
Common Symptomatology
The common symptoms of angioedema include sudden swelling of the affected areas, such as the face, lips, or tongue, which can cause discomfort, pain, or changes in appearance. The swelling can be accompanied by redness, warmth, and itching. In some cases, individuals may also experience difficulty breathing, hoarseness, or a feeling of tightness in the throat or chest. It is important to note that the severity and duration of symptoms can vary, depending on the underlying cause and individual response.
Atypical Presentations
In some cases, angioedema can present with atypical symptoms that may be challenging to recognize. These can include gastrointestinal symptoms like abdominal pain, nausea, or vomiting, or neurological symptoms such as dizziness or confusion. Atypical presentations of angioedema may delay the diagnosis and appropriate management, highlighting the need for awareness and vigilance.
Distinguishing Angioedema from Other Conditions
Angioedema can sometimes be mistaken for other conditions, such as cellulitis, urticaria (hives), or erythema multiforme. However, there are some key differences that can help distinguish angioedema from these conditions. Unlike urticaria, angioedema primarily affects the deeper layers of the skin and submucosal tissues, resulting in swelling and not the characteristic raised, itchy wheals associated with urticaria. Cellulitis, on the other hand, usually involves warmth, redness, and pain, and is often associated with skin infection. Erythema multiforme typically presents with distinctive target-shaped or “bull’s-eye” lesions.
Diagnostic Approaches
Accurate diagnosis of angioedema relies on a comprehensive evaluation of the patient’s medical history, a thorough physical examination, and appropriate laboratory tests and imaging studies. Specialized procedures may also be necessary in certain cases to further investigate the underlying cause.
Medical History and Physical Examination
A detailed medical history and physical examination are crucial in diagnosing angioedema. The medical history should include questions about the frequency, duration, and severity of episodes, known triggers, presence of any underlying medical conditions, and any medications or recent infections. The physical examination will focus on assessing the extent and location of the swelling, as well as any associated symptoms such as difficulty breathing or gastrointestinal symptoms.
Laboratory Tests
Laboratory tests may be ordered to help identify the underlying cause of angioedema. These can include blood tests to assess for allergic reactions, autoimmune markers, or specific protein deficiencies associated with hereditary angioedema. Additional tests may be required to evaluate for underlying infections or abnormal immune system responses.
Imaging Studies
In some cases, imaging studies may be necessary to evaluate the extent of tissue involvement or to identify potential causes such as a localized infection or structural abnormalities. Imaging techniques like ultrasound, CT scans, or MRI scans can be used to visualize the affected areas and provide valuable information for diagnosis and treatment planning.
Specialized Procedures
Specialized procedures, such as skin biopsies or allergen testing, may be necessary in certain cases to help identify the underlying cause of angioedema. These procedures can provide valuable insights into the specific triggers or immune responses that are contributing to the condition.
Management and Treatment
Managing and treating angioedema involves a combination of acute management during attacks, chronic management to prevent recurrent episodes, and the use of appropriate medications and therapies. In recent years, there have also been advancements in treatment options, providing hope for improved outcomes and reduced burden for those living with angioedema.
Acute Management
During an acute angioedema attack, it is important to take immediate action to alleviate symptoms and prevent complications. This may involve administering medications such as antihistamines, corticosteroids, or epinephrine to reduce swelling and inflammation. In severe cases with airway involvement, emergency medical intervention may be required to ensure adequate oxygenation and prevent respiratory distress.
Chronic Management
For individuals who experience recurrent angioedema episodes, chronic management is essential to prevent future attacks and minimize the impact of the condition on daily life. This may involve identifying and avoiding triggers, taking preventive medications, and implementing lifestyle modifications to reduce the risk of flares. Regular follow-up with healthcare providers is crucial to monitor the effectiveness of management strategies and adjust treatment plans as needed.
Medications and Therapies
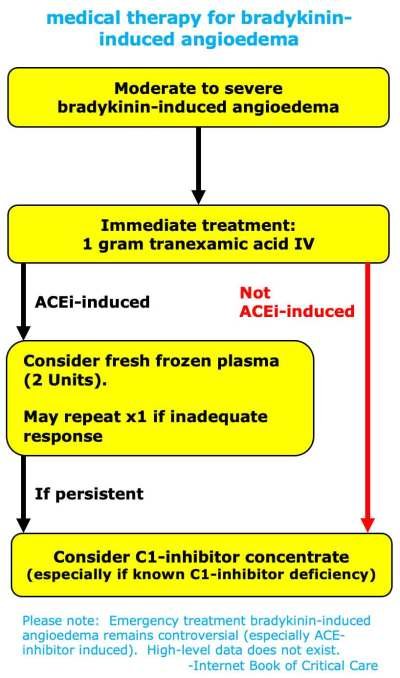
Medications play a key role in the management of angioedema. Antihistamines, corticosteroids, and leukotriene receptor antagonists are commonly prescribed to relieve symptoms and prevent recurrence. For hereditary angioedema, specific medications such as C1 esterase inhibitors or bradykinin receptor antagonists may be used. In certain cases, immunomodulatory therapies or biologic agents may also be considered. It is important to work closely with healthcare providers to determine the most appropriate medication regimen for each individual.
Preventive Measures
Prevention is a crucial aspect of managing angioedema and reducing the frequency and severity of attacks. This may involve identifying and avoiding triggers that have been associated with previous episodes, such as specific foods, medications, or environmental factors. It is also important to ensure proper management of underlying medical conditions or infections that may contribute to angioedema. Additionally, some individuals may benefit from using protective measures such as wearing medical alert bracelets or carrying emergency medications for rapid intervention during severe episodes.
Emerging Treatment Options
Advancements in angioedema research have led to the exploration of new treatment options that show promise in improving outcomes for individuals with this condition. These include targeted therapies like monoclonal antibodies that specifically block the pathways involved in angioedema attacks. Ongoing clinical trials are further evaluating the safety and efficacy of these emerging treatment options, offering hope for improved symptom control and quality of life for those affected by angioedema.
Identifying Underlying Causes
Understanding the underlying causes of angioedema is key to effective management and prevention of recurrent episodes. While some cases may be idiopathic, there are several known factors that can contribute to the development of angioedema.
Genetic Factors
In the case of hereditary angioedema, genetic factors play a significant role in the occurrence of recurrent angioedema episodes. Specific gene mutations or deficiencies in proteins involved in regulating blood vessel permeability can lead to uncontrolled swelling and inflammation.
Allergic Triggers
Allergic triggers, such as certain foods, medications, insect bites, or environmental factors, can cause allergic angioedema in individuals who have a hypersensitivity or allergy to these substances. Identifying and avoiding these triggers is an important part of managing this type of angioedema.
Autoimmune Disorders
Certain autoimmune disorders, such as lupus or vasculitis, can contribute to the development of angioedema. The underlying autoimmune response may cause increased blood vessel permeability and subsequent swelling in various parts of the body.
Drug-Induced Angioedema
Certain medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), ACE inhibitors, or antibiotics, can induce angioedema as a side effect. It is important to be aware of potential drug-induced triggers and to inform healthcare providers about any known allergies or adverse reactions to medications.
Idiopathic Angioedema
Idiopathic angioedema refers to episodes of swelling that occur without an identifiable cause. It can be challenging to manage, as the specific triggers are unknown. In these cases, a thorough evaluation by healthcare providers, including consideration of genetic factors, allergen testing, and other diagnostic approaches, is necessary to determine the most appropriate management strategy.
Associated Complications
Angioedema can lead to various complications, some of which can be severe and life-threatening if left untreated. It is important to be aware of these potential complications and take appropriate measures to prevent or manage them.
Airway Obstruction
One of the most critical complications of angioedema is airway obstruction. Swelling in the throat or tongue can compromise the airway, making it difficult to breathe. This can rapidly progress to respiratory distress, require emergency medical intervention, and become life-threatening if not addressed promptly.
Swelling of the Digestive Tract
Angioedema can sometimes affect the gastrointestinal tract, leading to severe abdominal pain, nausea, vomiting, or diarrhea. In some cases, it can cause bowel obstruction or impaired digestion and absorption of nutrients, requiring medical intervention and management.
Psychosocial Impacts
Living with angioedema can have a significant impact on an individual’s psychological well-being. The unpredictable nature of the condition, potential for disfigurement during episodes, and the need to constantly be vigilant can lead to increased anxiety, depression, and social isolation. It is crucial to address the psychosocial impacts of angioedema and provide appropriate support to individuals and their families.
Medical Emergencies
In severe cases, angioedema can result in medical emergencies that require immediate intervention. Airway obstruction, severe respiratory distress, or cardiovascular collapse can occur, necessitating prompt medical attention and treatment. It is important for individuals with angioedema, as well as their family members and caregivers, to be educated on recognizing emergency situations and seeking immediate medical help when necessary.
Effectively Managing Angioedema Attacks
To effectively manage angioedema attacks, it is essential to recognize the early symptoms, provide immediate first aid, seek appropriate medical intervention, and follow up with appropriate aftercare.
Recognition of Early Symptoms
Early recognition of the symptoms of angioedema is crucial to initiate prompt management and prevent complications. This includes being vigilant for signs of facial swelling, redness, itching, or any changes in the respiratory or gastrointestinal systems. Being aware of personal triggers and understanding individual patterns can also aid in early recognition.
Immediate First Aid
When an angioedema attack occurs, providing immediate first aid can help alleviate symptoms and prevent the situation from worsening. This may include staying calm, ensuring a clear airway, administering any prescribed emergency medication (such as epinephrine), and seeking medical assistance if needed.
Medical Intervention
In severe or life-threatening cases of angioedema, immediate medical intervention is necessary to stabilize the individual’s condition. This may involve emergency medical services, hospitalization, or specialized medical procedures to address airway obstruction, reduce swelling, and manage associated complications.
Aftercare and Follow-up
Following an angioedema attack, it is essential to seek appropriate aftercare and follow-up with healthcare providers. This may involve monitoring symptoms, adjusting medication regimens, addressing any complications, and receiving guidance on preventive measures and long-term management strategies. Regular communication with healthcare providers can help ensure optimal support and ongoing care.
Preventive Measures
Preventing angioedema attacks is a crucial aspect of managing the condition and improving quality of life for individuals affected by this condition. This involves identifying triggers, implementing avoidance strategies, educating oneself on the condition, and considering preventive medications when necessary.
Identifying Triggers
Identifying triggers that have been associated with previous episodes of angioedema is essential in preventing future attacks. This may involve keeping a diary to track symptoms, dietary intake, environmental exposures, and other potential triggers. By identifying and avoiding these triggers, the frequency and severity of angioedema episodes can be significantly reduced.
Avoidance Strategies
Once triggers have been identified, implementing avoidance strategies is key to prevent angioedema attacks. This may involve avoiding specific foods, medications, or factors such as insect bites or exposure to known allergens. In some cases, lifestyle modifications may be necessary, such as wearing protective clothing or using air filters to reduce potential exposure to triggers.
Education and Patient Empowerment
Education plays a vital role in effective management and prevention of angioedema attacks. Individuals and their families should be educated about the condition, its triggers, early recognition of symptoms, and appropriate management strategies. Empowering individuals to take an active role in their care can help reduce anxiety, improve adherence to treatment plans, and enhance overall well-being.
Preventive Medications
For individuals who experience recurrent episodes of angioedema, preventive medications may be prescribed to reduce the frequency and severity of attacks. These medications, such as antihistamines, corticosteroids, or specific medications for hereditary angioedema, work by stabilizing blood vessel permeability and modulating the immune response. It is important to work closely with healthcare providers to determine the most appropriate preventive medication regimen based on the individual’s specific circumstances.
Living with Angioedema
Living with angioedema can pose unique challenges, but with proper management and support, individuals can lead fulfilling lives. Coping strategies, support networks, and understanding the impact of angioedema on quality of life are important aspects of navigating this condition.
Coping Strategies
Developing effective coping strategies is essential for individuals living with angioedema. This can include mindfulness techniques, stress management strategies, and relaxation exercises to address anxiety or stress that may exacerbate or trigger episodes. Seeking support from mental health professionals or support groups can also provide valuable tools and strategies for managing the emotional impact of angioedema.
Support Networks
Having a strong support network is crucial for individuals with angioedema. This may include family members, friends, or support groups who can provide understanding, empathy, and practical assistance during episodes. Connecting with others who share similar experiences can be reassuring and empowering for individuals living with angioedema.
Impact on Quality of Life
Angioedema can significantly impact an individual’s quality of life. The unpredictability of attacks, the need to constantly be vigilant, and the potential for disfigurement during episodes can cause anxiety, social isolation, and limitations in daily activities. Understanding and addressing these challenges are important for individuals with angioedema to maintain a positive outlook and overall well-being.
Patient Stories and Experiences
Sharing patient stories and experiences can provide valuable insights and support for individuals living with angioedema. Hearing about others’ journeys and how they navigate the challenges associated with this condition can help individuals feel less alone and may offer practical tips or inspiration for effective management and living a fulfilling life despite the challenges.
Advancements in Angioedema Research
Medical research is continuously advancing our understanding of angioedema, leading to innovations in diagnosis, treatment, and overall care. Exploring the pathophysiology of angioedema, developing new diagnostic techniques, and investigating treatment innovations are some of the areas where progress is being made.
Exploring the Pathophysiology
Ongoing research is focused on unraveling the complex pathophysiology underlying angioedema. This involves understanding the molecular and immunological mechanisms that contribute to increased blood vessel permeability, identifying key mediators involved in the inflammatory response, and exploring potential targets for therapeutic interventions. By further elucidating the pathophysiology, researchers hope to develop more targeted and effective treatment approaches.
New Diagnostic Techniques
Advancements in diagnostic techniques are improving the accuracy and efficiency of diagnosing angioedema. This includes the development of more sensitive laboratory tests to detect specific autoimmune markers or genetic abnormalities associated with angioedema. Additionally, imaging techniques are becoming increasingly sophisticated, allowing for precise visualization of affected areas and identifying potential underlying causes.
Treatment Innovations
In recent years, there have been significant treatment innovations for angioedema. Targeted therapies, such as monoclonal antibodies, are being developed to specifically block the pathways involved in angioedema attacks. These medications show promise in reducing the frequency and severity of episodes and improving overall symptom control. Other treatment strategies under investigation include gene therapy to correct genetic abnormalities associated with hereditary angioedema and the development of new therapies that modulate the immune response.
Current Clinical Trials
Clinical trials are essential for advancing our understanding of angioedema and testing the safety and efficacy of emerging treatment options. Participating in clinical trials can provide individuals with access to cutting-edge therapies and contribute to the development of new treatment approaches. For those interested in participating in clinical trials, it is important to consult with healthcare providers and research centers to explore available opportunities and determine eligibility.
In conclusion, understanding angioedema is crucial for effective management and prevention of this condition. By recognizing the different types, identifying triggers, implementing preventive measures, and staying informed about advancements in research and treatment options, individuals with angioedema can lead fulfilling lives while minimizing the impact of this complex condition. With proper support, education, and a proactive approach to care, it is possible to navigate the complexities of angioedema and achieve optimal well-being.