In this article, get ready to learn about the symptoms of a truly terrifying infection: the brain-eating amoeba. Yes, you read that right – it’s as horrifying as it sounds. Although these cases are rare, understanding the symptoms is crucial for early detection and treatment. So, grab your reading glasses and prepare to delve into the world of brain-eating amoebas, where we’ll explore the signs that might indicate this serious infection.
What is Brain-Eating Amoeba?
Definition
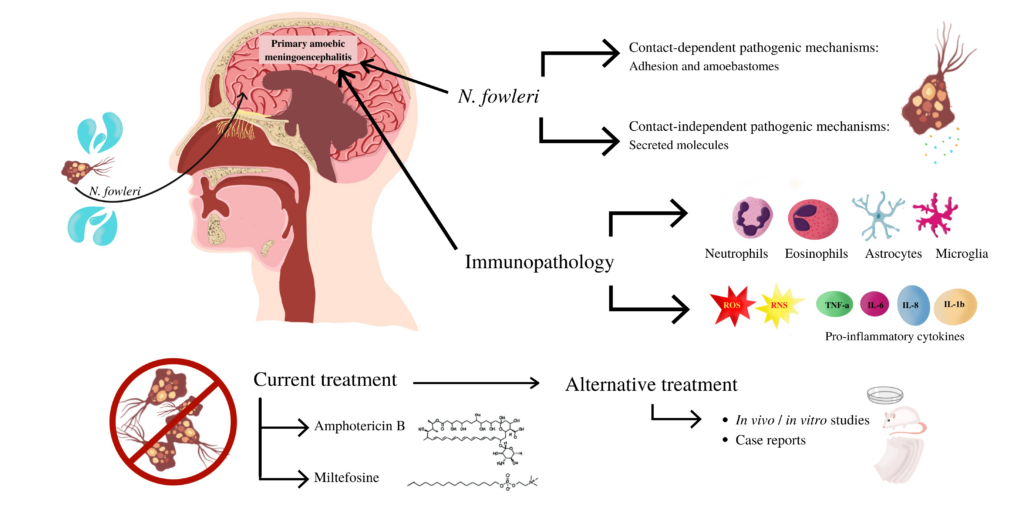
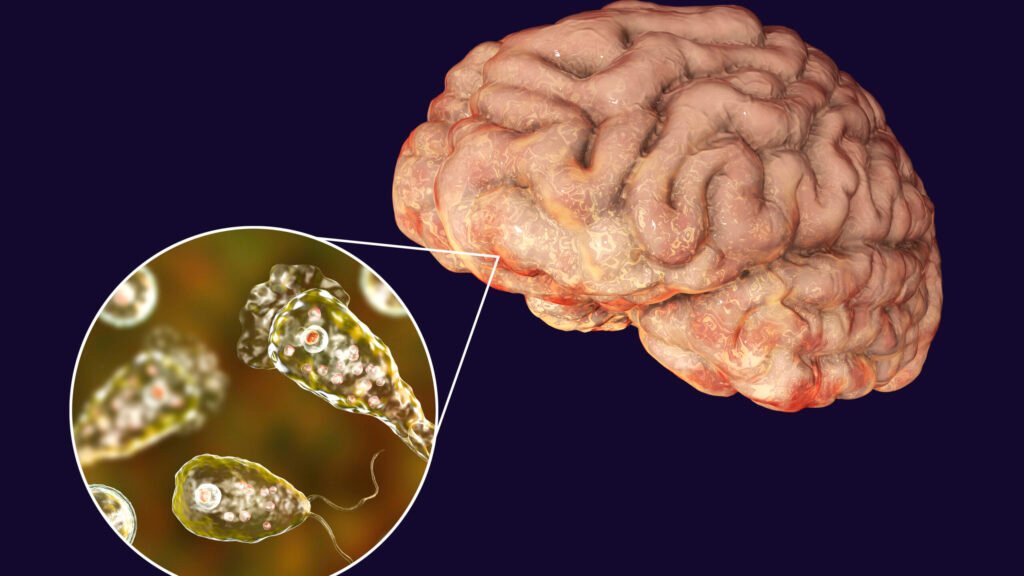
Brain-Eating Amoeba, scientifically known as Naegleria fowleri, is a rare and highly dangerous amoeba that can cause a severe brain infection called primary amebic meningoencephalitis (PAM). This amoeba is found in warm freshwater environments, such as lakes, hot springs, and poorly maintained swimming pools or hot tubs.
How does it enter the body?
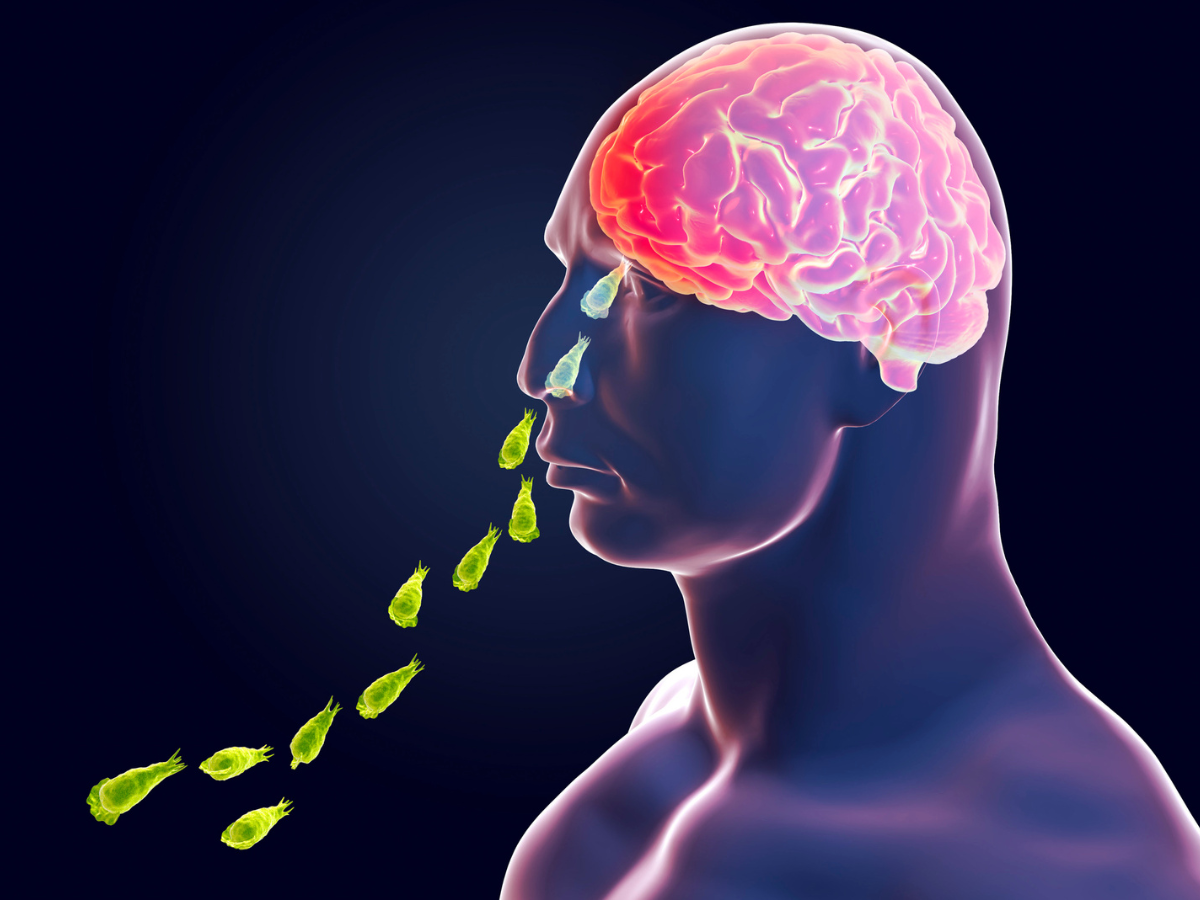
The entry point for Brain-Eating Amoeba is through the nose. When you swim or dive in contaminated water, the amoeba can enter your nasal passages and travel up into your brain. It can also enter the body through the eyes, although this is less common.
Common sources of infection
Some common sources of Brain-Eating Amoeba infection include warm freshwater bodies like lakes, rivers, hot springs, and even improperly chlorinated or heated swimming pools. It is important to note that Brain-Eating Amoeba infection cannot be spread by drinking contaminated water and is not contagious.
Prevalence and Risk Factors
Geographical distribution
Cases of Brain-Eating Amoeba infection are relatively rare but more commonly reported in certain parts of the world. In the United States, for example, most cases occur in the southern states, where the climate is warmer and the amoeba thrives. However, cases have been reported in other countries as well, including Australia, India, and parts of Europe.
Typical age groups affected
Brain-Eating Amoeba infection tends to affect individuals of all age groups, but certain age groups are more susceptible. The majority of cases occur in young children and teenagers, possibly due to their increased likelihood of engaging in water-related activities in contaminated environments.
Underlying health conditions that increase risk
Individuals with weakened immune systems, such as those who have undergone organ transplants or are living with HIV/AIDS, are at a higher risk of developing severe infection if exposed to Brain-Eating Amoeba. Additionally, people with underlying health conditions like diabetes, cancer, and liver disease may also have a higher risk.
Pathophysiology
Site of infection
Once the Brain-Eating Amoeba enters the body through the nose, it travels through the nasal passages and migrates to the brain. It primarily infects the olfactory bulbs, which are responsible for the sense of smell, and the frontal lobe of the brain.
Mechanism of infection
The amoeba uses its pseudopods (finger-like projections) to attach itself to the nasal tissues and penetrate the cribriform plate, a thin bone that separates the nasal cavity from the brain. From there, it enters the olfactory nerves and migrates to the brain parenchyma.
Damage to the brain
Infection with Brain-Eating Amoeba leads to a severe inflammatory response in the brain, causing damage to the brain tissue. This can result in brain swelling (cerebral edema), destruction of nerve cells, and disruption of normal brain function, leading to the symptoms and complications associated with the infection.
Early Symptoms
General manifestations
In the early stages of Brain-Eating Amoeba infection, the symptoms may initially resemble those of other common illnesses, making it challenging to diagnose. Some general manifestations include fever, headache, nausea, vomiting, and a stiff neck. These symptoms usually appear within a few days of exposure to the amoeba.
Specific signs to watch out for
As the infection progresses, specific signs may start emerging. These can include altered mental status, confusion, seizures, hallucinations, and sensitivity to light. It is crucial to pay attention to any sudden and severe changes in behavior, memory, or cognitive function, as they may be indicative of Brain-Eating Amoeba infection.
Progression of Symptoms
Neurological symptoms
As Brain-Eating Amoeba infection progresses, the symptoms become increasingly severe. Neurological symptoms may include a sudden onset of severe headaches, changes in behavior or personality, loss of motor coordination, seizures, and eventually, a state of confusion or coma.
Gastrointestinal symptoms
In some cases, individuals infected with Brain-Eating Amoeba may experience gastrointestinal symptoms. These can include nausea, vomiting, abdominal pain, and diarrhea. Although less common, these symptoms may be present alongside the neurological symptoms.
Respiratory symptoms
Respiratory symptoms are not typically associated with Brain-Eating Amoeba infection, as the amoeba primarily affects the brain. However, some individuals may experience respiratory distress or difficulty breathing, particularly as the infection progresses and causes increased swelling and pressure in the brain.
Complications
Meningitis
Meningitis, characterized by inflammation of the membranes surrounding the brain and spinal cord, is a severe complication that can occur as a result of a Brain-Eating Amoeba infection. This can further contribute to headaches, fever, stiff neck, and sensitivity to light.
Cerebral edema
Cerebral edema, or brain swelling, is common in severe cases of Brain-Eating Amoeba infection. The inflammation caused by the amoeba leads to an increase in fluid accumulation within the brain, causing pressure and potentially life-threatening complications.
Seizures
As the Brain-Eating Amoeba infection progresses and affects brain function, it can trigger seizures. Seizures are abnormal electrical discharges in the brain that can vary from mild to severe, and they can cause further damage to the brain tissue.
Diagnosis
Physical examination
In the early stages, it can be challenging to diagnose Brain-Eating Amoeba infection based solely on physical examination. However, a thorough evaluation including a neurological examination can provide valuable insights into the presence of symptoms and clues to support the diagnosis.
Laboratory tests
Laboratory tests play a crucial role in confirming Brain-Eating Amoeba infection. Cerebrospinal fluid (CSF) analysis, obtained through a lumbar puncture, can reveal elevated white blood cell count, increased protein levels, and evidence of the amoeba itself. Polymerase chain reaction (PCR) testing may also be performed to detect the presence of Naegleria fowleri DNA.
Imaging studies
Imaging studies, such as a computed tomography (CT) scan or magnetic resonance imaging (MRI), are essential to assess the extent of brain damage and identify any abnormalities. These imaging modalities can help distinguish Brain-Eating Amoeba infection from other brain infections and assist in guiding appropriate treatment strategies.
Treatment
Antifungal medications
Antifungal medications, such as amphotericin B, are the primary treatment option for Brain-Eating Amoeba infection. This medication is administered intravenously to target and destroy the amoeba in the brain. Other supportive medications, such as anticonvulsants to manage seizures, may also be prescribed.
Emergency procedures
In severe cases, emergency procedures such as therapeutic hypothermia, where the body temperature is lowered to reduce brain swelling, may be employed. In some instances, surgery may be necessary to relieve pressure on the brain caused by cerebral edema.
Supportive care
Supportive care plays a crucial role in the management of Brain-Eating Amoeba infection. This includes providing measures to reduce fever, relieve pain, control seizures, and sustain proper fluid and electrolyte balance. Close monitoring for complications and ongoing rehabilitation are also essential for the overall care of the patient.
Prevention
Avoiding contaminated water
To reduce the risk of Brain-Eating Amoeba infection, it is important to avoid swimming or diving in warm freshwater bodies that may be contaminated. Staying aware of any advisories or warnings regarding water quality, and only swimming in well-maintained swimming pools and hot tubs, can help minimize exposure.
Using nose plugs or clips
Using nose plugs or clips can act as a barrier and minimize the chance of Brain-Eating Amoeba entering the body through the nasal passages while swimming or engaging in water-related activities. This precaution is particularly important in areas where the amoeba is known to be present.
Educating about the risk factors
Raising awareness about the risk factors associated with Brain-Eating Amoeba infection can help individuals make informed decisions and take necessary precautions. This includes educating the public about the specific regions where the amoeba is more prevalent, the symptoms to watch out for, and the importance of seeking prompt medical attention if symptoms arise.
Prognosis
Survival rate
Unfortunately, the prognosis for Brain-Eating Amoeba infection is typically poor. The infection progresses rapidly, and even with treatment, the survival rate is low. According to reported cases, the mortality rate is estimated to be around 97%.
Long-term effects on survivors
Survivors of Brain-Eating Amoeba infection may experience long-term effects on their cognitive function, memory, and overall neurological health. Rehabilitation plays a critical role in helping survivors regain their independence and manage any residual impairments.
Potential for recurrence
Despite successful treatment, the potential for recurrence of Brain-Eating Amoeba infection is extremely rare. However, individuals who have survived the infection should continue following preventive measures to reduce the risk of future exposure and reinfection.
In conclusion, Brain-Eating Amoeba, while rare, is a highly dangerous infection that can lead to severe brain damage and a high mortality rate. Understanding the symptoms, risk factors, and prevention strategies is crucial in minimizing the risk of infection and ensuring prompt medical intervention if necessary. If you suspect any symptoms or have concerns about potential exposure, it is important to seek immediate medical attention for a thorough evaluation and appropriate management. Stay informed, be cautious, and prioritize your health and well-being when engaging in water-related activities.