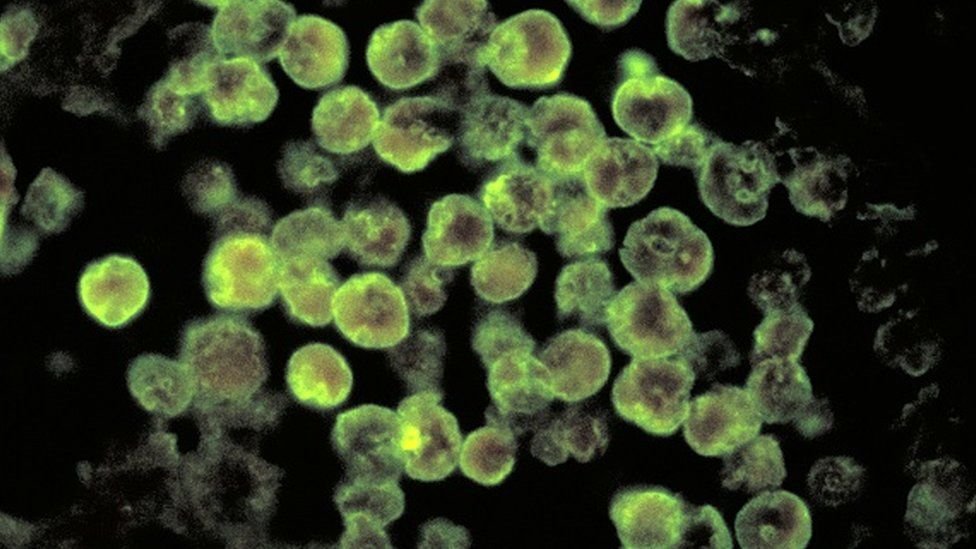
Imagine a tiny organism, invisible to the naked eye, lurking in the depths of warm freshwater lakes and rivers. Its sheer existence sends a shiver down your spine. This mysterious creature is none other than the brain-eating amoeba. This article aims to unravel the enigma surrounding these microscopic predators and shed light on their potential dangers to humans. So, fasten your seatbelts and let’s embark on a captivating journey through the realm of these minuscule yet formidable creatures.
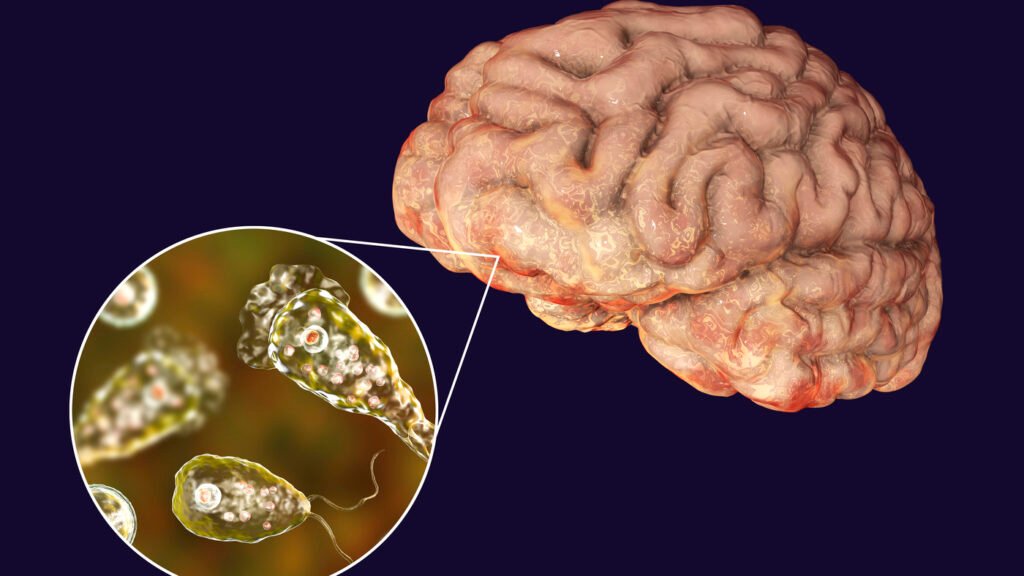
Factors of Brain-Eating Amoeba Infections
Introduction to brain-eating amoeba
Brain-eating amoeba, scientifically known as Naegleria fowleri, is a microscopic amoebic species that can cause a rare and devastating infection of the brain. This free-living amoeba is naturally found in warm freshwater environments, such as lakes, hot springs, and poorly maintained swimming pools. While brain-eating amoeba infections are extremely rare, they attract significant attention due to their often severe and fatal outcomes.
Prevalence and distribution
Brain-eating amoeba infections are primarily found in regions with warm climates, particularly in the southern United States, but cases have been reported worldwide. These infections tend to occur more frequently during the summer months when water temperatures are higher, providing an optimal environment for the amoeba to thrive. While the overall prevalence of brain-eating amoeba infections remains low, it is important to understand the conditions that promote their occurrence.
Conditions favoring infection
Several factors contribute to the increased risk of brain-eating amoeba infections. Firstly, warm freshwater environments, such as lakes or untreated hot springs, provide an ideal habitat for the growth and proliferation of Naegleria fowleri. Additionally, activities that involve water entering the nasal passages, such as swimming, diving, or using contaminated water for nasal irrigation, can increase the likelihood of infection. Finally, individuals with weakened immune systems or those who have experienced recent nasal trauma may be more susceptible to infection.
Sources of infection
The primary source of brain-eating amoeba infection is exposure to water containing Naegleria fowleri. As mentioned earlier, warm freshwater environments are the natural habitat of these amoebae. It is essential to note that brain-eating amoebas cannot infect individuals through ingestion or skin contact with contaminated water. Infections only occur when water enters the nasal passages and allows the amoebas to travel to the brain through the olfactory nerve.
Understanding Naegleria Fowleri
Characteristics of Naegleria fowleri
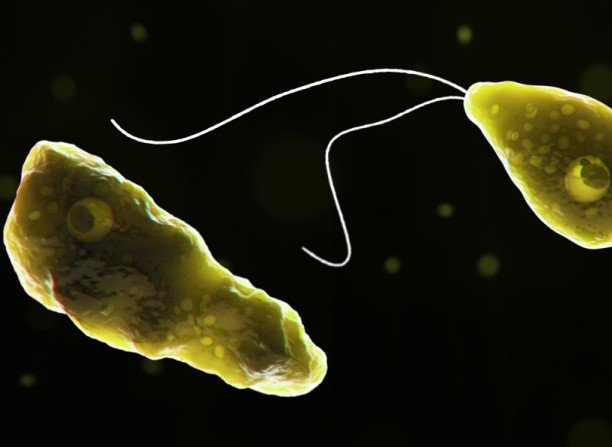
Naegleria fowleri is a single-celled organism belonging to the phylum Percolozoa. Under the microscope, it appears as a rounded amoeba with a size of approximately 8 to 15 micrometers. This amoebic species has two distinct forms – a feeding form, known as the trophozoite, and a resting form, known as the cyst. The trophozoite actively feeds on bacteria and other organic matter, while the cyst serves as a survival mechanism during unfavorable conditions.
Life cycle and behavior
The life cycle of Naegleria fowleri involves three main stages – the trophozoite, cyst, and flagellate stage. In the trophozoite stage, the amoebas actively feed and reproduce by binary fission. As environmental conditions become unfavorable, Naegleria fowleri transforms into a dormant cyst, which allows it to survive in a dormant state until favorable conditions return. When in contact with warm freshwater and human nasal passages, the amoeba can transform into its active feeding form and migrate to the brain, leading to infection.
Transmission pathways
Transmission of Naegleria fowleri occurs exclusively through the nasal passages. When water containing the amoebas enters the nasal cavity, the amoebas can traverse the olfactory nerve and enter the brain, leading to the development of a brain-eating amoeba infection. It is important to note that the infection is not contagious and cannot be transmitted from person to person through casual contact.
Symptoms and Diagnosis
Early symptoms of brain-eating amoeba infection
The early symptoms of brain-eating amoeba infection are often nonspecific and can resemble those of other common illnesses. Initial symptoms may include fever, headache, nausea, vomiting, and a stiff neck. As the infection progresses, individuals may experience seizures, altered mental state, hallucinations, and coma. It is crucial to seek immediate medical attention if these symptoms arise, especially in individuals with a recent history of water-related activities.
Progression of infection
Once Naegleria fowleri enters the brain, the infection rapidly progresses and can cause severe damage. The amoebas feed on brain tissue, leading to the destruction of neurons and the development of inflammation. This inflammation triggers an immune response, resulting in the release of cytokines and further damage to brain tissue. As the infection progresses, brain swelling and edema may occur, leading to increased intracranial pressure and potentially fatal outcomes if left untreated.
Diagnostic methods
Diagnosing brain-eating amoeba infections can be challenging due to the rarity of cases and the nonspecific nature of early symptoms. However, several diagnostic methods can aid in the identification of the infection. These methods include examining cerebrospinal fluid for the presence of amoebas, performing polymerase chain reaction (PCR) tests to detect Naegleria fowleri DNA, and conducting brain imaging studies, such as computed tomography (CT) scans or magnetic resonance imaging (MRI), to assess brain abnormalities.
Treatment and Prevention
Challenges in treating brain-eating amoeba infections
Treating brain-eating amoeba infections poses significant challenges due to the advanced stage of the infection by the time symptoms manifest and the aggressive nature of the amoeba. The limited availability of effective treatments further exacerbates the challenges. Additionally, the blood-brain barrier poses a barrier for many medications, making it difficult to effectively target the infection site within the brain.
Available treatment options
The primary treatment approach for brain-eating amoeba infections is the administration of antifungal and antimicrobial medications. However, the efficacy of these treatments remains limited, and the survival rate of infected individuals remains low. Other supportive measures, such as keeping the patient’s body temperature stable, reducing intracranial pressure, and managing seizures, may also be employed to alleviate symptoms and improve outcomes.
Preventive measures against infection
Preventing brain-eating amoeba infections primarily involves taking precautionary measures to minimize exposure to contaminated water sources. Avoiding water-related activities in warm freshwater environments with low water levels, keeping nasal passages closed or using nose plugs while engaged in water activities, and ensuring proper maintenance and chlorination of swimming pools can significantly reduce the risk of infection. Public education campaigns and raising awareness among healthcare professionals also play a crucial role in prevention efforts.

Case Studies
Notable cases of brain-eating amoeba infections
Several notable cases of brain-eating amoeba infections have drawn attention to the seriousness of these infections. For example, the case of a young boy in the United States who contracted the infection after playing in a water park brought national attention to the issue. Similarly, cases reported in other countries have highlighted the global impact of brain-eating amoeba infections and the need for preventive measures and research.
Effects on survivors and their families
Surviving a brain-eating amoeba infection is a rare occurrence, and those who do survive often face significant challenges and long-term effects. Survivors may experience neurological deficits, cognitive impairments, and profound emotional and psychological impacts. The families of infected individuals also endure immense emotional distress and may require ongoing support and specialized care for the affected individual’s needs.
Research and Experimental Treatments
Current research on brain-eating amoeba
Research on brain-eating amoeba is ongoing, with scientists aiming to better understand the behavior, life cycle, and pathogenesis of Naegleria fowleri. Efforts are being made to develop accurate diagnostic tools, innovative treatment approaches, and preventative measures. By studying the genetic makeup and virulence factors of the amoeba, researchers hope to identify potential targets for drug development and to improve patient outcomes.
Experimental treatments and therapeutics
Experimental treatments and therapeutics for brain-eating amoeba infections are being explored. These include the use of novel antifungal agents, immunotherapeutic approaches, and targeted drug delivery strategies to improve the efficacy of treatments. However, further research and clinical trials are necessary to validate these experimental approaches before they can be implemented in the clinical setting.

Public Awareness and Education
Educational campaigns and public outreach efforts
Public awareness and education initiatives play a crucial role in preventing brain-eating amoeba infections. Educational campaigns aim to inform the public about the risks associated with warm freshwater environments and emphasize the importance of taking preventive measures. These campaigns often involve disseminating information through various channels, such as social media, public service announcements, and educational materials distributed to schools, recreational facilities, and healthcare providers.
Raising awareness among healthcare professionals
Raising awareness among healthcare professionals is essential for early detection and prompt treatment of brain-eating amoeba infections. Medical organizations and professional societies conduct conferences, symposiums, and educational sessions to update healthcare providers on the latest research findings, diagnostic techniques, and treatment recommendations. By incorporating information about brain-eating amoeba infections into medical curricula and continuing education programs, healthcare professionals can play a vital role in prevention and early intervention.
Global Impact and Response
Response of health organizations and governments
Health organizations and governments worldwide recognize the importance of addressing brain-eating amoeba infections. National and international health agencies collaborate to establish guidelines and protocols for the detection, prevention, and management of these infections. By monitoring cases, implementing surveillance systems, and sharing information, these organizations strive to enhance public health efforts and minimize the occurrence and impact of brain-eating amoeba infections.
Outbreaks and regional differences in prevalence
While brain-eating amoeba infections are rare, occasional outbreaks occur. These outbreaks are often associated with specific water sources or environmental conditions. The prevalence of brain-eating amoeba infections can vary across regions due to differences in climate, water sources, and public health practices. Understanding these regional differences can help tailor prevention strategies and allocate appropriate resources to areas at higher risk.
Future Directions
Advancements in diagnostics and treatment
Advancements in diagnostics and treatment hold promise for improving outcomes for individuals affected by brain-eating amoeba infections. Scientists are exploring the use of advanced molecular techniques for rapid and accurate diagnosis. Additionally, ongoing research on potential therapeutic targets and experimental treatments may lead to the development of more effective treatment options in the future.
Prospects for prevention and eradication
Prevention and eradication of brain-eating amoeba infections remain a long-term goal for public health efforts. Continued research, public awareness campaigns, and implementation of preventive measures are key to decreasing the incidence of these infections. By addressing the factors favoring infection, enhancing water management practices, and promoting widespread education, it is possible to reduce the burden of brain-eating amoeba infections and improve overall public health.
Conclusion
Brain-eating amoeba infections are rare but devastating conditions that capture significant attention due to their severe outcomes. Understanding the factors contributing to these infections, the behavior of Naegleria fowleri, the progression of the disease, and the available treatment options is crucial for prevention and early intervention. Ongoing research, public awareness campaigns, and global collaboration are essential in advancing diagnostics, treatment, and preventive measures. By prioritizing public health initiatives and raising awareness, we can strive towards a future where brain-eating amoeba infections are minimized and lives are saved.