In the realm of oncology, Burkitt Lymphoma poses a unique set of challenges that demand careful consideration when it comes to treatment options. With its aggressive nature and rapid growth, finding the most effective approach can make a significant difference in mitigating its impact. This article will dive into the various management strategies available for Burkitt Lymphoma, shedding light on the latest advancements and providing insights on the potential paths to recovery. So, whether you’re a patient seeking information or a healthcare professional looking to enhance your knowledge, join us as we embark on a journey to explore the multifaceted world of Burkitt Lymphoma treatment.
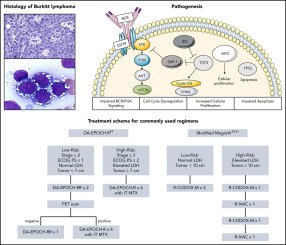
Diagnosis of Burkitt Lymphoma
Physical examination
During a physical examination, your healthcare provider will carefully check your body for any signs or symptoms of Burkitt Lymphoma. They will examine your lymph nodes, abdomen, and other areas of your body for any signs of swelling or abnormalities. Additionally, they may also perform a thorough medical history assessment to gather information about any symptoms you may have been experiencing, as well as any potential risk factors for the disease.
Laboratory tests
Laboratory tests play a crucial role in the diagnosis of Burkitt Lymphoma. Your healthcare provider will likely order blood tests to evaluate your overall health, including a complete blood count (CBC) to assess your red and white blood cell counts. They may also conduct various other tests to measure the levels of certain markers in your blood, such as lactate dehydrogenase (LDH) and beta-2 microglobulin.
Imaging tests
Imaging tests help your healthcare provider visualize the affected areas and determine the extent of the disease. Common imaging tests used in the diagnosis of Burkitt Lymphoma include computed tomography (CT) scans, magnetic resonance imaging (MRI), and positron emission tomography (PET) scans. These tests provide detailed images of your lymph nodes and other organs, aiding in the identification of any abnormalities or tumors.
Biopsy
A biopsy is usually the definitive test to confirm the diagnosis of Burkitt Lymphoma. During a biopsy, a small sample of tissue is surgically removed from a suspicious lymph node or affected area and examined under a microscope by a pathologist. This analysis helps determine the presence of cancer cells and their specific characteristics, allowing for an accurate diagnosis and classification of the lymphoma subtype.
Staging of Burkitt Lymphoma
Stage I
Stage I Burkitt Lymphoma refers to cancer that is confined to a single lymph node or a group of nearby lymph nodes on one side of the diaphragm. It has not spread to any other organs or tissues.
Stage II
In Stage II Burkitt Lymphoma, the cancer has spread to more than just one side of the diaphragm. It may involve either multiple lymph nodes or lymph nodes on one side of the diaphragm along with involvement of nearby organs or tissues.
Stage III
In Stage III Burkitt Lymphoma, the cancer has spread to lymph nodes both above and below the diaphragm. It may also involve the spleen and other nearby organs or tissues.
Stage IV
Stage IV Burkitt Lymphoma indicates that the cancer has spread to multiple organs or tissues outside of the lymphatic system. It may affect distant organs such as the bone marrow, liver, lungs, or central nervous system.

Treatment Approaches for Burkitt Lymphoma
Chemotherapy
Chemotherapy is a cornerstone of Burkitt Lymphoma treatment. It uses powerful drugs to destroy cancer cells and prevent their growth and spread. Depending on the stage and severity of the disease, different chemotherapy regimens may be employed. High-dose methotrexate and cyclophosphamide, ifosfamide, etoposide, and cytarabine, as well as the CODOX-M/IVAC regimen are commonly used for Burkitt Lymphoma.
Surgery
Although surgery is not typically the primary treatment for Burkitt Lymphoma, it may be performed in certain cases. For example, if a tumor mass causes a blockage or obstruction in a vital organ or if lymph nodes become significantly enlarged, surgical intervention may be necessary to alleviate these complications.
Radiation therapy
Radiation therapy may be utilized as part of the treatment plan for Burkitt Lymphoma. It involves the use of high-energy x-rays or other types of radiation to target and kill cancer cells. Radiation therapy is often employed in cases where the disease has spread to the central nervous system, bone marrow, or other specific sites.
Chemotherapy Regimens for Burkitt Lymphoma
High-dose methotrexate and cyclophosphamide
This chemotherapy regimen combines high doses of methotrexate and cyclophosphamide. Methotrexate inhibits the growth of cancer cells by interfering with their ability to use folate (an essential nutrient). Cyclophosphamide, on the other hand, works by damaging the DNA of cancer cells, preventing their replication. This combination is particularly effective in treating Burkitt Lymphoma.
Ifosfamide, etoposide, and cytarabine
The ifosfamide, etoposide, and cytarabine regimen (known as the “IEA” regimen) is commonly used in the treatment of Burkitt Lymphoma. Ifosfamide works by damaging the DNA of cancer cells, while etoposide and cytarabine disrupt the replication process of the cancer cells. This combination helps to target and destroy the rapidly dividing cancer cells characteristic of Burkitt Lymphoma.
CODOX-M/IVAC regimen
The CODOX-M/IVAC regimen is another highly effective chemotherapy treatment for Burkitt Lymphoma. It is a combination of two different chemotherapy regimens: CODOX-M and IVAC. The CODOX-M regimen includes cyclophosphamide, vincristine, doxorubicin, and high-dose methotrexate. The IVAC regimen consists of ifosfamide, etoposide, and high-dose cytarabine. The combination of these drugs helps to target and eliminate cancer cells in a comprehensive manner.

Stem Cell Transplantation
Autologous stem cell transplantation
Autologous stem cell transplantation involves the collection and storage of healthy stem cells from your own body. Before undergoing high-dose chemotherapy, your stored stem cells are reintroduced into your body to restore the blood cell production compromised by the treatment. This procedure can help to minimize the risks of infection, anemia, and bleeding associated with high-dose chemotherapy.
Allogeneic stem cell transplantation
Allogeneic stem cell transplantation involves the use of stem cells from a compatible donor, typically a family member or an unrelated individual with a closely matched tissue type. This procedure allows for the replacement of your damaged blood-forming cells with healthy cells from the donor, providing a new source of healthy blood cells. Allogeneic stem cell transplantation may be considered in cases where the disease has not responded well to other treatments or has relapsed.
Management of Complications
Tumor lysis syndrome
Tumor lysis syndrome is a potentially life-threatening complication that can occur during chemotherapy treatment for Burkitt Lymphoma. It is characterized by the rapid destruction of cancer cells, leading to the release of large amounts of waste products into the bloodstream. This can cause electrolyte imbalances and kidney dysfunction. To prevent or manage tumor lysis syndrome, your healthcare team will closely monitor your blood chemistry, administer intravenous fluids, and prescribe medications to stabilize your electrolyte levels.
Infections
Cancer treatments, including chemotherapy, can weaken your immune system, making you more susceptible to infections. Prompt identification and treatment of any infections is essential. Your healthcare provider may prescribe antibiotics or antifungal medications to fight off infections. It is also important to follow hygienic practices and avoid close contact with individuals who are sick or have infections.
Neuropathy
Neuropathy is a potential side effect of chemotherapy drugs and radiation therapy used in Burkitt Lymphoma treatment. It can cause numbness, tingling, or pain in the hands and feet. If you develop neuropathy, it is important to inform your healthcare provider so they can assess the severity and provide appropriate management strategies, which may include modifying the treatment regimen or prescribing medications to help alleviate the symptoms.
Renal toxicity
Certain chemotherapy drugs used in Burkitt Lymphoma treatment can pose a risk to kidney function. Monitoring your kidney function through regular blood tests is essential to detect any signs of renal toxicity. In some cases, fluid management and medication adjustments may be required to protect your kidneys during treatment.
Secondary malignancies
The risk of developing secondary malignancies, such as other types of lymphomas or solid tumors, can be increased in individuals who have received high-dose chemotherapy and radiation therapy. Regular follow-up visits and surveillance are crucial to detect any signs of secondary malignancies early on. Your healthcare team will monitor your health closely and conduct appropriate screening tests to detect any potential malignancies.

Prognosis and Survival
Factors affecting prognosis
Several factors can influence the prognosis of Burkitt Lymphoma. These include the stage of the disease at diagnosis, the presence of specific genetic abnormalities, your overall health and immune function, and how well you respond to treatment. The earlier the disease is diagnosed and treated, the better the overall prognosis.
Survival rates
With effective treatment, the overall survival rates for Burkitt Lymphoma have significantly improved over the years. However, individual survival outcomes can vary based on various factors. The five-year survival rate for localized (stage I and II) Burkitt Lymphoma exceeds 90%, while for more advanced forms (stage III and IV), it ranges between 60% and 90%.
Relapse and recurrence
Despite successful treatment, there is a risk of relapse or recurrence of Burkitt Lymphoma. Regular follow-up appointments and surveillance are vital to detect early signs of disease recurrence. Prompt intervention and appropriate treatment can improve the chances of successful management if recurrence occurs.
Follow-up Care
Regular medical check-ups
After completing the initial treatment for Burkitt Lymphoma, it is essential to continue with regular follow-up appointments with your healthcare team. These appointments will involve physical examinations, blood tests, and imaging studies to monitor your overall health and detect any signs of disease recurrence or late effects of treatment.
Monitoring for late effects
Long-term survivors of Burkitt Lymphoma may experience late effects related to their treatment. These can include cardiovascular problems, reproductive health issues, secondary cancers, hormonal imbalances, or problems with growth and development in children. Regular monitoring and appropriate interventions can help manage these late effects and improve long-term quality of life.
Psychosocial support
Coping with a cancer diagnosis and undergoing treatment can be emotionally challenging. Seek out support from friends, family, and support groups to help you navigate through any emotional or psychological difficulties. Psychosocial support can provide a valuable source of strength and encouragement throughout your journey.
Rehabilitation and survivorship programs
Rehabilitation programs can help you regain physical strength and manage any functional limitations resulting from treatment. Survivorship programs provide guidance and resources to help you transition into life after Burkitt Lymphoma treatment, addressing various aspects of survivorship, including physical, emotional, and social well-being.

Clinical Trials
Advancing research and treatment
Clinical trials are an important avenue for advancing research and treatment options for Burkitt Lymphoma. By participating in clinical trials, you have the opportunity to access experimental therapies and contribute to the development of new and potentially more effective treatments for the disease. Talk to your healthcare provider to explore whether you may be eligible for any ongoing clinical trials.
Accessing experimental therapies
In certain situations, accessing experimental therapies outside a clinical trial may be considered. This may occur when standard treatment options have been exhausted, or if you meet specific eligibility criteria. Discuss with your healthcare provider the possibility of accessing experimental therapies and explore any potential benefits and risks associated with such treatments.
Conclusion
Burkitt Lymphoma is an aggressive form of lymphoma that requires prompt and comprehensive management. With a combination of chemotherapy, radiation therapy, and in some cases, stem cell transplantation, the treatment outcomes for Burkitt Lymphoma have significantly improved. Regular medical check-ups, surveillance for late effects, and psychosocial support are essential components of long-term care for Burkitt Lymphoma survivors. By staying informed and actively participating in your treatment and follow-up care, you can maximize your chances of successful outcomes and achieve a healthier and fulfilling life beyond Burkitt Lymphoma.