Living with diabetes can be challenging, but what many people don’t realize is that it can have a significant impact on mental health as well. The intricate relationship between diabetes mellitus and mental health is a topic that deserves attention and understanding. In this article, we explore the various ways in which diabetes can affect your mental well-being, leading to increased stress, anxiety, and even depression. By shedding light on this often overlooked aspect of diabetes management, we aim to provide valuable insights and support for those affected, helping them navigate the complexities of their health journey with both physical and mental wellbeing in mind.

Understanding Diabetes Mellitus
Diabetes Mellitus, commonly referred to as diabetes, is a chronic condition that affects the body’s ability to regulate blood sugar levels. It is characterized by high levels of glucose (sugar) in the blood, which can lead to a range of health complications if left uncontrolled.
Definition of Diabetes Mellitus
Diabetes Mellitus is a metabolic disorder characterized by elevated blood sugar levels due to either insufficient production of insulin by the pancreas or the body’s inability to effectively use insulin. Insulin is a hormone that helps regulate blood sugar levels and allows glucose to enter the cells to provide energy. Without proper insulin functioning, glucose builds up in the blood, resulting in hyperglycemia.
Types of Diabetes Mellitus
There are several types of diabetes mellitus, the most common being Type 1 and Type 2 diabetes.
Type 1 diabetes occurs when the body’s immune system mistakenly attacks and destroys the insulin-producing cells in the pancreas. This leads to a complete lack of insulin production and requires lifelong insulin therapy.
Type 2 diabetes is the most prevalent form of diabetes and occurs when the body becomes resistant to the effects of insulin or doesn’t produce enough insulin. It is often associated with lifestyle factors such as obesity, sedentary behavior, and poor diet.
Other forms of diabetes include gestational diabetes, which occurs during pregnancy, and rarer types such as monogenic diabetes and secondary diabetes caused by certain medications or medical conditions.
Causes and Risk Factors
The causes of diabetes mellitus are complex and can vary depending on the type of diabetes. Type 1 diabetes is believed to have a genetic predisposition, but environmental triggers, such as viral infections, may also play a role. Type 2 diabetes is primarily influenced by lifestyle factors, including poor diet, lack of physical activity, obesity, and family history.
Risk factors for developing diabetes include age, ethnicity, family history, obesity, sedentary lifestyle, and certain medical conditions such as polycystic ovary syndrome (PCOS) and prediabetes.
Prevalence and Incidence
Diabetes mellitus is a global health issue, with its prevalence steadily increasing over the years. According to the International Diabetes Federation (IDF), approximately 463 million adults were living with diabetes in 2019, and this number is projected to rise to 700 million by 2045. The majority of people with diabetes have Type 2 diabetes, accounting for about 90% of cases.
The incidence of diabetes varies across different regions and populations, with certain ethnic groups, such as South Asians and Hispanics, being at a higher risk. Additionally, the aging population and the rising prevalence of obesity contribute to the growing burden of diabetes worldwide.
Link between Diabetes Mellitus and Mental Health
Impact of Diabetes on Mental Health
Living with diabetes can significantly impact a person’s mental well-being. The daily management challenges, potential complications, and lifestyle adjustments associated with diabetes can lead to emotional distress, anxiety, and depression. The constant vigilance required to monitor blood sugar levels, take medication or insulin, and adhere to dietary restrictions can contribute to feelings of overwhelm and frustration.
Common Mental Health Conditions in Diabetes Patients
People with diabetes are at an increased risk of developing mental health conditions. Depression and anxiety are frequently associated with diabetes, with studies suggesting that individuals with diabetes are twice as likely to experience depression compared to the general population. Anxiety disorders, including generalized anxiety disorder and panic disorder, are also prevalent among individuals with diabetes.
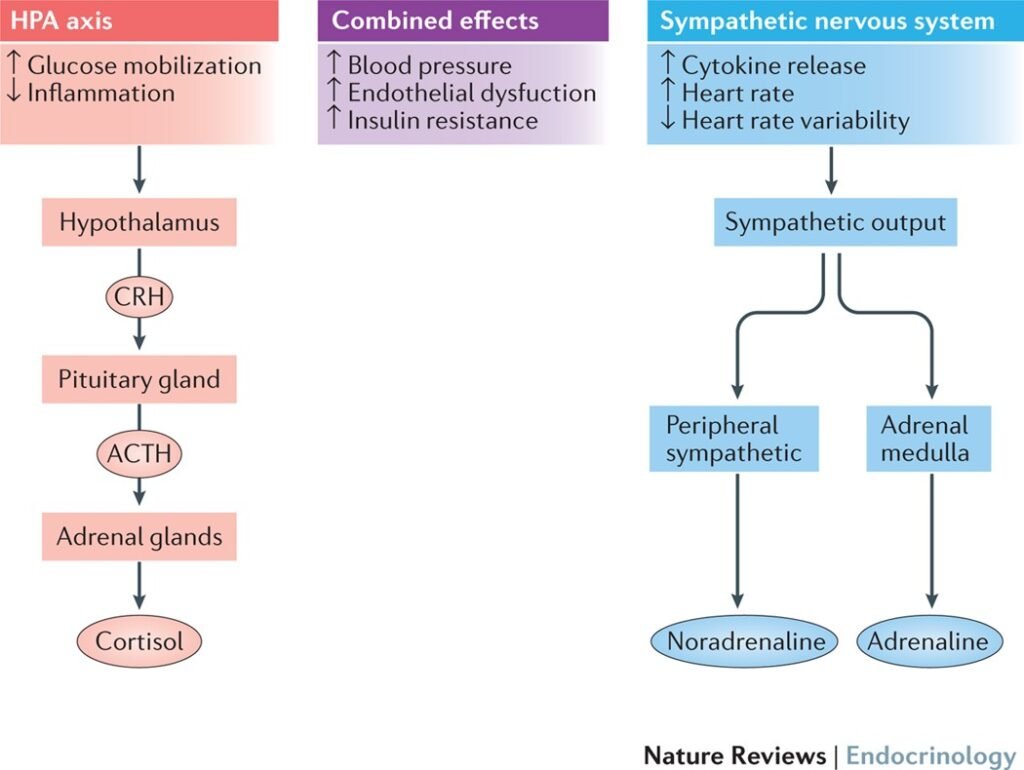
Biological Mechanisms
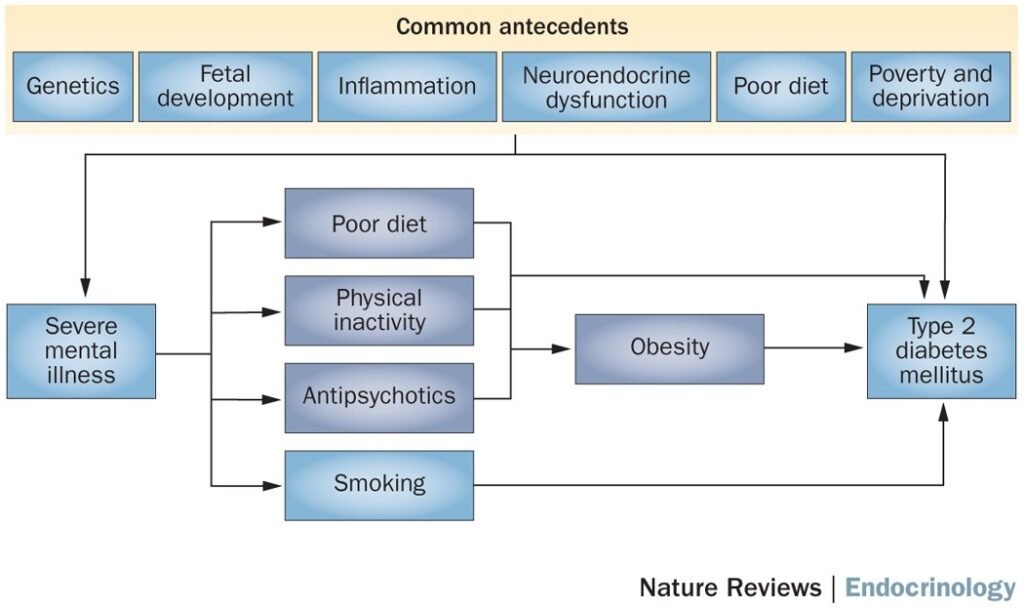
The connection between diabetes and mental health is not only psychological but also rooted in biological mechanisms. Diabetes can have a direct impact on brain function and neurotransmitter balance. The dysregulation of insulin and glucose metabolism may influence neurotransmitter levels, potentially contributing to mood disorders.
Psychosocial Factors
Psychosocial factors play a key role in the relationship between diabetes and mental health. The stress of living with a chronic condition, coping with the demands of diabetes management, and concerns about potential complications can all contribute to psychological distress. The social and emotional impact of receiving a diabetes diagnosis and facing stigma or discrimination related to the condition can further exacerbate mental health challenges.
Psychological Challenges in Diabetes Management
Managing diabetes can present various psychological challenges for individuals, impacting their emotional well-being and overall quality of life.
Emotional Adjustment to Diagnosis
Receiving a diabetes diagnosis can be emotionally overwhelming. It may involve a significant adjustment to a new way of life, including dietary changes, self-monitoring of blood sugar levels, and the need for medications or insulin injections. The initial shock, fear, and uncertainty following a diagnosis can affect a person’s emotional well-being and require support and guidance.
Depression and Anxiety in Diabetes
Depression and anxiety are common psychological challenges faced by individuals with diabetes. The constant management tasks, fear of complications, and the impact of diabetes on daily life can contribute to the development or exacerbation of these mental health conditions. Symptoms such as low mood, loss of interest, irritability, excessive worry, and difficulty concentrating may be signs of depression or anxiety in diabetes patients.
Diabetes Distress
Diabetes distress refers to the emotional burden and frustration associated with managing diabetes. It encompasses feelings of sadness, frustration, stress, and burnout related to the daily demands of diabetes self-care. Diabetes distress can influence a person’s motivation, adherence to treatment, and overall well-being.
Fear of Hypoglycemia
Hypoglycemia, or low blood sugar, is a common concern for individuals with diabetes, especially those using insulin or certain medications. Fear of hypoglycemia can cause anxiety and lead to behaviors such as avoiding physical activity or skipping meals. This fear can significantly impact diabetes management and compromise overall health.
Psychological Insulin Resistance
Psychological insulin resistance refers to the resistance or reluctance to initiate or intensify insulin treatment despite medical recommendations. It can stem from various factors, including fear of injections, concerns about side effects, misconceptions about insulin, or the stigma associated with insulin use. Psychological insulin resistance can impair diabetes control and increase the risk of complications.
Mental Health Screening and Assessment in Diabetes
Importance of Screening
Screening for mental health issues in individuals with diabetes is crucial for early detection and intervention. Mental health problems often go unrecognized and untreated in diabetes care, leading to additional health risks and decreased quality of life. Routine screening can help identify individuals who may benefit from psychological support or intervention.
Screening Tools
Several screening tools are available to assess mental health in diabetes patients. The Patient Health Questionnaire (PHQ-9) is commonly used to screen for depression, while the Generalized Anxiety Disorder scale (GAD-7) can evaluate anxiety symptoms. Other specific tools, such as the Problem Areas in Diabetes (PAID) scale, assess diabetes-related emotional distress.
Clinical Assessment
Clinical assessments involve a comprehensive evaluation of a person’s mental health, considering the impact of diabetes on psychological well-being. Assessments may include interviews, questionnaires, and observations to gather information about symptoms, emotional functioning, perception of quality of life, and adherence to diabetes treatment.
Collaborative Care Approach
The collaborative care approach involves a team-based approach to managing both diabetes and mental health. It involves collaboration between healthcare providers, such as primary care physicians, endocrinologists, psychiatrists, psychologists, and diabetes educators. This approach ensures that both physical and mental health needs are addressed, leading to improved outcomes for individuals with diabetes.

Treatment Approaches and Interventions
Medication and Behavioral Interventions
Treatment for mental health conditions in diabetes patients often involves a combination of medication and behavioral interventions. Antidepressants and anxiolytics may be prescribed to manage symptoms of depression and anxiety. Behavior-focused interventions, such as cognitive-behavioral therapy (CBT) and psychoeducation, can help individuals develop coping skills and improve their self-management of diabetes and mental health.
Psychoeducation and Self-Management
Psychoeducation plays a crucial role in empowering individuals with diabetes to better understand the connection between diabetes and mental health. Educating individuals about the impact of stress, high and low blood sugar levels, and the importance of self-care can enhance self-management skills and promote overall well-being.
Cognitive Behavioral Therapy
Cognitive-behavioral therapy (CBT) is a widely used therapeutic approach for individuals with diabetes and comorbid mental health conditions. CBT helps individuals identify and modify negative thought patterns, develop problem-solving skills, and improve coping strategies. This can lead to a reduction in psychological distress and improved diabetes management outcomes.
Mindfulness-Based Interventions
Mindfulness-based interventions, such as mindfulness-based stress reduction (MBSR) and mindfulness-based cognitive therapy (MBCT), have shown promise in improving mental health outcomes in diabetes patients. These interventions focus on cultivating present-moment awareness, non-judgmental acceptance, and coping with stress through mindfulness practices. They can enhance emotional well-being and promote self-care behaviors.
Support Groups and Peer Counseling
Support groups and peer counseling provide individuals with diabetes an opportunity to connect with others who share similar experiences. These group settings offer emotional support, validation, and practical advice for managing diabetes and mental health challenges. Peer counseling, where individuals with lived experience of diabetes offer support to others, can be a valuable resource in promoting self-care and reducing isolation.
Role of Healthcare Providers
Patient Education and Empowerment
Healthcare providers play a vital role in educating and empowering individuals with diabetes to manage their condition effectively. By providing clear and accurate information about diabetes, its complications, and the link to mental health, healthcare providers can help individuals make informed decisions about their treatment and self-care.
Collaborative Care Model
The collaborative care model involves coordinated and integrated care among various healthcare providers. It emphasizes a team-based approach to address the physical, mental, and emotional aspects of diabetes. Collaborative care models can lead to improved outcomes and better quality of life for individuals with diabetes.
Interdisciplinary Approach
An interdisciplinary approach involves healthcare professionals from various disciplines working together to address the complex needs of individuals with diabetes. This may include endocrinologists, primary care physicians, psychologists, diabetes educators, and other specialists. By combining their expertise, these professionals can provide comprehensive care that considers both physical and mental health.
Integrated Care Settings
Integrated care settings aim to merge primary care and mental health services, ensuring that individuals with diabetes can access mental health support alongside their routine diabetes care. By providing both services conveniently in one location, integrated care settings reduce barriers and improve access to mental health care for individuals with diabetes.
Prevention and Early Intervention Strategies
Diabetes Prevention Programs
Diabetes prevention programs focus on promoting healthy lifestyle habits, such as regular physical activity, healthy eating, and weight management, to reduce the risk of developing Type 2 diabetes. These programs often incorporate behavioral counseling, education, and support to help individuals make sustainable lifestyle changes.
Mental Health Promotion
Promoting mental health in individuals with diabetes involves strategies to enhance emotional well-being, strengthen coping skills, and reduce stress. This can include promoting self-care, stress management techniques, and encouraging social support networks. Mental health promotion aims to reduce the risk of mental health problems and improve overall quality of life.
Early Identification of Mental Health Issues
Early identification of mental health issues in individuals with diabetes is crucial for timely intervention. Routine screening for symptoms of depression, anxiety, and diabetes distress can help identify individuals who may benefit from mental health support. Training healthcare providers to recognize the signs of mental health problems and establishing pathways for referral to mental health services are essential components of early identification.
Integrated Preventive Care
Integrated preventive care involves addressing both physical and mental health needs simultaneously to prevent the onset or progression of diabetes and mental health conditions. This comprehensive approach emphasizes the importance of early intervention, regular monitoring, and coordinated care to optimize long-term health outcomes.
Barriers and Challenges in Diabetes-Mental Health Care
Stigma and Social Attitudes
Stigma surrounding mental health and diabetes can create significant barriers to accessing appropriate care. The fear of being judged or misunderstood may prevent individuals from seeking help for their mental health concerns or disclosing their struggles to healthcare providers. Addressing stigma and promoting a supportive, non-judgmental environment is crucial for improving the integration of diabetes and mental health care.
Limited Access to Mental Health Services
Access to mental health services, particularly in underserved areas or communities, can be limited. Many individuals with diabetes lack access to mental health professionals who are knowledgeable about the unique challenges of living with diabetes. Improving access to mental health services and incorporating mental health professionals within diabetes care settings is essential for comprehensive care.
Lack of Resources
A lack of resources, including financial resources, support programs, and educational materials, can hinder individuals’ ability to effectively manage their diabetes and mental health. Limited resources may prevent individuals from accessing appropriate treatment, medications, or self-management tools. Adequate funding and resource allocation are necessary to address these barriers and provide comprehensive care.
Healthcare System Challenges
The fragmentation of healthcare systems and the lack of integration between physical health and mental health services pose challenges in providing optimal care for individuals with diabetes and mental health conditions. Limited communication and coordination between healthcare providers can result in incomplete care and missed opportunities for early intervention. Addressing systemic challenges and promoting collaborative care models can improve the integration of diabetes and mental health care.
Future Directions and Research
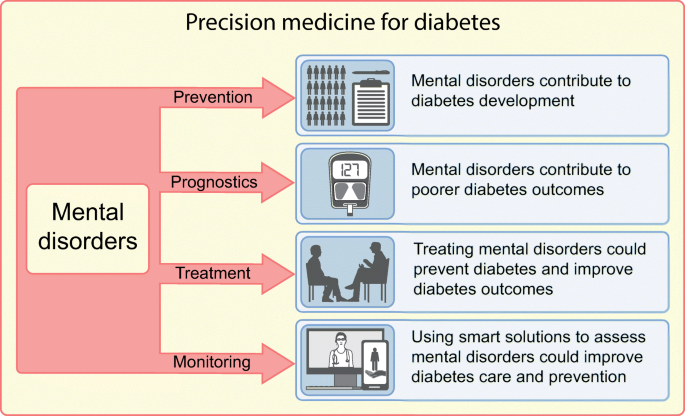
Identification of Risk Factors
Future research should focus on identifying additional risk factors for the development of mental health conditions in individuals with diabetes. Understanding the interplay between genetic, environmental, and lifestyle factors can inform targeted preventive strategies and early interventions.
Interventions and Treatment Innovation
Continued research on effective interventions and treatment approaches for individuals with diabetes and mental health conditions is imperative. Exploring new interventions, such as digital health platforms, telemedicine, and mobile applications, can enhance access to mental health support and improve self-management outcomes in individuals with diabetes.
Longitudinal Studies
Longitudinal studies tracking the mental health outcomes and diabetes management outcomes over extended periods can help uncover the long-term implications of living with diabetes and mental health conditions. These studies can identify protective factors, highlight areas for intervention, and inform strategies for improving patient care.
Improved Care Integration
Efforts should focus on improving the integration of diabetes and mental health care within healthcare systems. This includes creating collaborative care teams, implementing care pathways, and improving communication and coordination between healthcare providers. Integrating mental health services within diabetes care settings and promoting interdisciplinary collaboration can optimize patient outcomes.
Conclusion
The link between diabetes mellitus and mental health is complex and multifaceted. Individuals with diabetes face various psychological challenges, including emotional adjustment to diagnosis, depression, anxiety, and diabetes-specific distress. Mental health screening, assessment, and appropriate interventions are crucial for holistic diabetes management. Collaborative care models, interdisciplinary approaches, and integrated care settings can facilitate comprehensive care delivery. To overcome barriers and challenges in diabetes-mental health care, addressing stigma, improving access to mental health services, and allocating adequate resources are essential. Future research should improve risk factor identification, explore innovative interventions, conduct longitudinal studies, and promote care integration. By recognizing and addressing the connection between diabetes and mental health, healthcare providers can help individuals with diabetes achieve optimal physical and emotional well-being.