You may have heard of Hashimoto’s Thyroiditis and Hypothyroidism, but did you know that there is a strong link between the two? Hashimoto’s Thyroiditis, an autoimmune condition that affects the thyroid gland, is actually the most common cause of hypothyroidism. In this article, we will explore this connection and shed light on how understanding this link can help in the diagnosis and treatment of these conditions. So, grab a cup of tea and get ready to dive into the fascinating world of the thyroid gland and its intricate relationship with our overall health.
Understanding Hashimoto’s Thyroiditis
Definition and Overview
Hashimoto’s Thyroiditis is an autoimmune disorder that affects the thyroid gland. It is named after the Japanese physician, Dr. Hakaru Hashimoto, who first described the condition in 1912. In this condition, the immune system mistakenly attacks the thyroid gland, leading to inflammation and damage. Over time, this can result in an underactive thyroid or hypothyroidism.
Causes and Risk Factors
The exact cause of Hashimoto’s Thyroiditis is unknown, but it is believed to be a combination of genetic and environmental factors. Family history of autoimmune diseases, such as Hashimoto’s Thyroiditis, increases the risk of developing the condition. Other risk factors include having other autoimmune disorders, such as type 1 diabetes or rheumatoid arthritis, being female, and certain genetic variations.
Symptoms
The symptoms of Hashimoto’s Thyroiditis can vary from person to person. Some individuals may experience no symptoms or only mild symptoms, while others may have more severe symptoms. Common symptoms include fatigue, weight gain, sensitivity to cold, dry skin, constipation, muscle weakness, hair loss, and depression. These symptoms are often non-specific and can be mistaken for other conditions, making accurate diagnosis important.
Diagnosis
Diagnosing Hashimoto’s Thyroiditis usually involves a combination of medical history, physical examination, and laboratory tests. Your doctor will ask about your symptoms, review your medical history, and perform a physical examination to check for signs of hypothyroidism. Blood tests are then conducted to measure levels of thyroid-stimulating hormone (TSH), thyroxine (T4), and thyroid antibodies. Elevated levels of thyroid antibodies, such as thyroid peroxidase antibody (TPOAb) and thyroglobulin antibody (TgAb), indicate an autoimmune thyroid condition.
Treatment
Treatment for Hashimoto’s Thyroiditis aims to restore normal thyroid function and alleviate symptoms. The mainstay of treatment is hormone replacement therapy, which involves taking synthetic thyroid hormones, such as levothyroxine. This medication helps to replenish the inadequate levels of thyroid hormones and regulate metabolism. Regular monitoring of thyroid hormone levels and adjustments to medication dosage may be necessary to achieve optimal control. In addition to medication, lifestyle changes, such as getting regular exercise, managing stress, and maintaining a healthy diet, can also help support thyroid health.
Understanding Hypothyroidism
Definition and Overview
Hypothyroidism, also known as an underactive thyroid, is a condition where the thyroid gland does not produce enough thyroid hormones. It can be caused by various factors, including Hashimoto’s Thyroiditis. When the thyroid gland is not functioning properly, it affects the body’s metabolism and can lead to a wide range of symptoms.
Causes and Risk Factors
Hypothyroidism can be caused by several factors, including autoimmune diseases like Hashimoto’s Thyroiditis, thyroid surgery, radiation therapy, certain medications, and congenital factors. Risk factors for hypothyroidism include being female, being over the age of 60, having a family history of thyroid problems, and having an autoimmune disorder.
Symptoms
The symptoms of hypothyroidism can vary from person to person and may develop slowly over time. Common symptoms include fatigue, weight gain, sensitivity to cold, constipation, dry skin, hair loss, muscle weakness, and depression. These symptoms are similar to those of Hashimoto’s Thyroiditis, which can make it difficult to differentiate between the two conditions without proper testing.
Diagnosis
Diagnosing hypothyroidism involves a combination of medical history, physical examination, and blood tests. Your doctor will ask about your symptoms and review your medical history to determine if there are any risk factors or underlying conditions. A physical examination may reveal signs of hypothyroidism, such as dry skin, hair loss, and a slowed heart rate. Blood tests will be conducted to measure levels of TSH and thyroid hormones. Elevated TSH levels and decreased levels of thyroid hormones indicate an underactive thyroid.
Treatment
The primary treatment for hypothyroidism is hormone replacement therapy, which involves taking synthetic thyroid hormones to replace the inadequate levels produced by the thyroid gland. The most commonly prescribed medication is levothyroxine, which is similar to the hormone produced by the thyroid gland. Regular monitoring of thyroid hormone levels is important to ensure the dosage is adjusted as needed. In addition to medication, lifestyle changes such as eating a balanced diet, engaging in regular exercise, managing stress, and getting enough sleep can help support overall thyroid health.

The Connection Between Hashimoto’s Thyroiditis and Hypothyroidism
Autoimmune Mechanism
Hashimoto’s Thyroiditis is an autoimmune disease, meaning that the immune system mistakenly attacks the body’s own tissues. In the case of Hashimoto’s Thyroiditis, the immune system targets the thyroid gland. This autoimmune mechanism leads to inflammation and damage to the thyroid gland, resulting in impaired thyroid function. Over time, this can lead to an underactive thyroid or hypothyroidism.
Effect on Thyroid Function
Hashimoto’s Thyroiditis can have a significant impact on thyroid function. As the immune system attacks the thyroid gland, it causes inflammation and damage to the thyroid tissue. This leads to decreased production of thyroid hormones, such as thyroxine (T4) and triiodothyronine (T3). The reduced levels of thyroid hormones result in a slowdown of metabolic processes in the body, leading to the symptoms of hypothyroidism.
Prevalence
Hashimoto’s Thyroiditis is the most common cause of hypothyroidism in the United States. It affects approximately 5% of the population, with women being more commonly affected than men. The prevalence of Hashimoto’s Thyroiditis increases with age, and it is most commonly diagnosed between the ages of 30 and 50. Having a family history of autoimmune diseases, including Hashimoto’s Thyroiditis, increases the risk of developing the condition.
Impact on Treatment Approaches
The presence of Hashimoto’s Thyroiditis can impact the treatment approach for hypothyroidism. In cases where Hashimoto’s Thyroiditis is the underlying cause of hypothyroidism, hormone replacement therapy with levothyroxine is still the primary treatment. However, monitoring of thyroid antibodies and thyroid function may be necessary to ensure optimal control. The autoimmune nature of Hashimoto’s Thyroiditis requires ongoing management and monitoring to prevent further damage to the thyroid gland and ensure proper thyroid hormone levels.
Autoimmune Mechanism
Explanation of Autoimmunity
Autoimmunity refers to a condition where the immune system mistakenly attacks the body’s own tissues, leading to inflammation and damage. Normally, the immune system defends the body against foreign invaders, such as bacteria and viruses. In autoimmunity, the immune system fails to recognize the body’s own tissues as “self” and instead targets them as if they were foreign. This can result in chronic inflammation and damage to various organs or tissues, depending on the specific autoimmune condition.
The Role of Thyroid Antibodies
Thyroid antibodies play a crucial role in the development and progression of Hashimoto’s Thyroiditis. These antibodies, such as thyroid peroxidase antibody (TPOAb) and thyroglobulin antibody (TgAb), are produced by the immune system and target specific proteins found in the thyroid gland. The presence of these antibodies in the blood indicates an autoimmune attack on the thyroid gland. Measuring thyroid antibodies is an important diagnostic tool for identifying Hashimoto’s Thyroiditis.
Inflammatory Response
In Hashimoto’s Thyroiditis, the immune system launches an inflammatory response against the thyroid gland. This leads to chronic inflammation within the thyroid tissue, causing damage to the cells that produce thyroid hormones. The inflammation also stimulates the production of reactive oxygen species and cytokines, further contributing to tissue damage. Over time, the chronic inflammation and tissue damage can result in decreased thyroid hormone production and an underactive thyroid.
Effect on Thyroid Function
Hashimoto’s Thyroiditis has a direct impact on thyroid function. The autoimmune attack on the thyroid gland leads to inflammation, destruction of thyroid cells, and impaired production of thyroid hormones. As the thyroid tissue becomes damaged, it is less able to produce an adequate amount of thyroid hormones, such as thyroxine (T4) and triiodothyronine (T3). The decrease in thyroid hormone production leads to a slowdown in metabolic processes in the body.
Effect on Thyroid Function
Thyroid Hormone Production
The thyroid gland plays a vital role in the production and regulation of thyroid hormones. T4 and T3 are the two main hormones produced by the thyroid gland, and they are involved in regulating metabolism and essential body functions. In Hashimoto’s Thyroiditis, the autoimmune attack on the thyroid gland leads to inflammation and damage, impairing its ability to produce sufficient amounts of thyroid hormones. This results in a decrease in thyroid hormone levels, leading to an underactive thyroid or hypothyroidism.
Regulation and Feedback Loop
The production and release of thyroid hormones are regulated by a feedback loop involving the hypothalamus, pituitary gland, and thyroid gland. The hypothalamus releases thyrotropin-releasing hormone (TRH), which stimulates the pituitary gland to release thyroid-stimulating hormone (TSH). TSH then acts on the thyroid gland, stimulating it to produce and release thyroid hormones. In hypothyroidism, the impaired thyroid function leads to low thyroid hormone levels, causing the pituitary gland to increase TSH production in an attempt to stimulate the thyroid gland.
Impact on Metabolism and Body Functions
Thyroid hormones play a crucial role in regulating metabolism and influencing various body functions. In hypothyroidism, the decreased levels of thyroid hormones lead to a slowdown of metabolic processes in the body. This can result in symptoms such as fatigue, weight gain, sensitivity to cold, constipation, dry skin, and muscle weakness. Additionally, thyroid hormones affect the functioning of organs and tissues, including the heart, brain, and digestive system. A deficiency in thyroid hormones can have wide-ranging effects on overall health and well-being.
Prevalence
Demographics and Epidemiology
Hashimoto’s Thyroiditis affects people of all ages and ethnic backgrounds, but certain demographics have a higher prevalence of the condition. It is more common in women than men, with women being five to eight times more likely to develop Hashimoto’s Thyroiditis. The condition tends to occur most frequently in middle-aged individuals, with the peak incidence occurring between the ages of 30 and 50. Hashimoto’s Thyroiditis is also more prevalent in populations of iodine-deficient regions.
Gender and Age Differences
The higher prevalence of Hashimoto’s Thyroiditis in women suggests a possible hormonal influence on the development of the condition. Hormonal factors, such as estrogen and prolactin, have been implicated in the increased susceptibility of women to autoimmune diseases. Additionally, the age distribution of Hashimoto’s Thyroiditis indicates that hormonal changes during puberty, pregnancy, and menopause may play a role in triggering the autoimmune response.
Genetic Predisposition
There is a significant genetic component to the development of autoimmune diseases like Hashimoto’s Thyroiditis. Having a family history of autoimmune diseases, including Hashimoto’s Thyroiditis, increases the risk of developing the condition. Certain genes, such as the HLA-DR3 and HLA-DR5 genes, have been associated with an increased risk of developing Hashimoto’s Thyroiditis. However, the precise genetic factors involved in the development of the condition are still not fully understood and further research is needed.

Diagnostic Methods
Evaluation of Symptoms
Diagnosing Hashimoto’s Thyroiditis involves evaluating a combination of symptoms, medical history, and physical examination findings. Common symptoms of Hashimoto’s Thyroiditis, such as fatigue, weight gain, and depression, can be non-specific and overlap with other conditions. Your doctor will ask detailed questions about your symptoms and how they have been affecting your daily life. Information about family history, previous medical conditions, and exposure to potential risk factors will also be considered.
Thyroid Function Tests
Thyroid function tests are crucial for diagnosing Hashimoto’s Thyroiditis. These blood tests measure levels of thyroid hormones, such as TSH, T4, and T3. In Hashimoto’s Thyroiditis, TSH levels are typically elevated due to decreased thyroid hormone production. Additionally, levels of free T4 and free T3 may also be measured to assess the actual amounts of active thyroid hormones in the bloodstream.
Antibody Testing
Testing for thyroid antibodies, such as TPOAb and TgAb, is an important diagnostic tool for Hashimoto’s Thyroiditis. The presence of elevated levels of these antibodies indicates an autoimmune attack on the thyroid gland. These tests are usually performed alongside thyroid function tests to provide a comprehensive picture of thyroid health.
Imaging Techniques
In some cases, imaging techniques may be used to further evaluate the condition of the thyroid gland. Ultrasound imaging can provide detailed images of the thyroid gland, allowing for the identification of any abnormalities, such as nodules or inflammation. Imaging techniques may be useful for monitoring the progression of the disease and assessing the response to treatment.
Management and Treatment Options
Medication and Hormone Replacement Therapy
The primary treatment for Hashimoto’s Thyroiditis and its associated hypothyroidism is hormone replacement therapy. This involves taking synthetic thyroid hormones, such as levothyroxine, to replace the inadequate levels of thyroid hormones produced by the thyroid gland. Levothyroxine medication is similar to the hormone produced by the thyroid gland and helps to regulate metabolism and alleviate symptoms. Regular monitoring of thyroid hormone levels is essential to ensure that the dosage is adjusted to maintain optimal control.
Lifestyle Changes
In addition to medication, certain lifestyle changes can help support thyroid health and improve overall well-being. Engaging in regular exercise, such as brisk walking or yoga, can help boost metabolism and promote a healthy weight. Managing stress through relaxation techniques, such as deep breathing or meditation, can also have a positive impact on thyroid function. Adequate sleep and maintaining a healthy diet that includes nutrient-rich foods, such as fruits, vegetables, and lean proteins, can further support thyroid health.
Diet and Nutrition
While there is no specific diet that can cure or prevent Hashimoto’s Thyroiditis, certain dietary considerations may be beneficial. Some individuals with Hashimoto’s Thyroiditis may have food sensitivities or intolerances that can exacerbate symptoms. It may be helpful to work with a healthcare provider or registered dietitian to identify and eliminate potential trigger foods. Additionally, ensuring adequate intake of iodine, selenium, and other essential nutrients necessary for thyroid function can be important.
Stress Management
Stress can have a negative impact on overall health and may exacerbate symptoms of Hashimoto’s Thyroiditis. Finding effective stress management techniques is important for managing the condition. This may include engaging in relaxation exercises, practicing mindfulness or meditation, seeking support through therapy or support groups, and making time for hobbies and activities that bring joy and relaxation. Prioritizing self-care and finding healthy ways to manage stress can help support overall well-being and thyroid health.

Complications and Prevention
Potential Long-term Effects
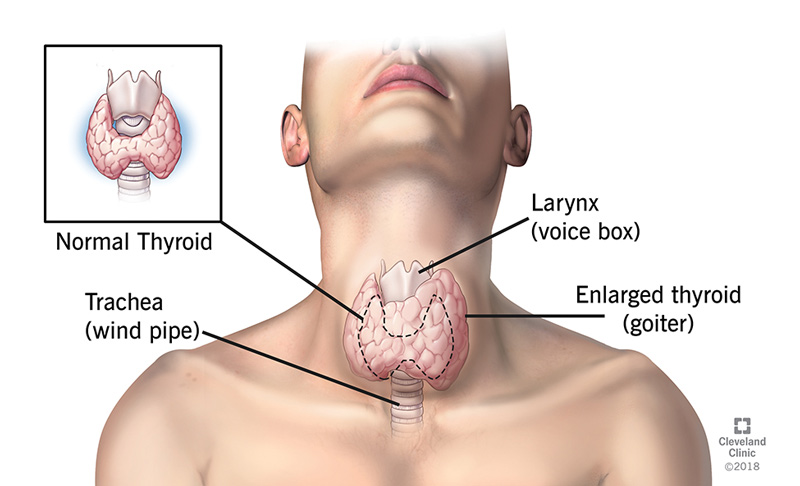
If left untreated or improperly managed, Hashimoto’s Thyroiditis can lead to various long-term complications. These include persistent symptoms of hypothyroidism, goiter (enlargement) of the thyroid gland, heart problems, infertility or pregnancy complications, and mental health issues. It is important to follow the prescribed treatment plan and regularly monitor thyroid hormone levels to prevent or minimize the risk of these long-term effects.
Monitoring and Follow-up Care
Regular monitoring and follow-up care are essential for managing Hashimoto’s Thyroiditis effectively. This includes regular visits to your healthcare provider to assess thyroid hormone levels, adjust medication dosage if necessary, and evaluate symptoms. Monitoring for potential complications, screening for other autoimmune diseases or thyroid abnormalities, and checking for signs of disease progression are also important components of ongoing care.
Preventive Measures
While there is no way to prevent the development of Hashimoto’s Thyroiditis, certain measures may help reduce the risk of complications. Following a healthy lifestyle, including regular exercise, stress management, and a balanced diet, can support overall thyroid health. It is also important to maintain regular check-ups with your healthcare provider, especially if you have a family history of autoimmune diseases or other risk factors. Identifying and addressing any potential risk factors or underlying conditions early can help prevent or minimize the impact of Hashimoto’s Thyroiditis.
Research and Future Directions
Advancements in Diagnosis
Research in the field of autoimmune thyroid disorders, including Hashimoto’s Thyroiditis, continues to advance our understanding of disease mechanisms and improve diagnostic techniques. Novel biomarkers and genetic tests are being developed to aid in the early detection and monitoring of Hashimoto’s Thyroiditis. Advancements in imaging technology also hold promise for improved visualization and evaluation of the thyroid gland, allowing for more accurate diagnoses and targeted treatment approaches.
Emerging Treatment Approaches
Current treatment options for Hashimoto’s Thyroiditis primarily focus on hormone replacement therapy. However, ongoing research is exploring novel therapeutic approaches to modulate the immune response and halt the progression of the disease. This includes the use of immunomodulatory drugs, targeted therapies, and even stem cell transplantation. While these approaches are still in the experimental stage, they offer potential new avenues for more precise and personalized treatment options for individuals with Hashimoto’s Thyroiditis.
Precision Medicine and Personalized Care
Advances in genomics and precision medicine hold promise for the future of Hashimoto’s Thyroiditis management. Genetic testing can help identify individuals who may be at a higher risk of developing the condition or predict their response to specific treatments. Personalized care plans that take into account an individual’s genetic predisposition, environmental factors, and unique symptom profile can improve treatment outcomes and enhance overall well-being. As research progresses, the integration of these personalized approaches into clinical practice may become more widespread, leading to more effective management of Hashimoto’s Thyroiditis.