Impetigo, a common and highly contagious skin infection, can be a cause for concern. This article aims to shed light on the causes, symptoms, and treatment options for this pesky condition. From understanding how impetigo is caused by bacteria to recognizing the telltale signs of blister-like sores and crusty patches, we will explore the various aspects of this condition. Additionally, we will discuss the different treatment options available, ranging from topical creams to antibiotics, and emphasize the importance of seeking medical advice for an accurate diagnosis. By gaining a better understanding of impetigo, you can take proactive steps to protect yourself and your loved ones from this bothersome infection.

Causes
Bacterial infection
Impetigo is a highly contagious skin infection that is primarily caused by bacteria. The most common bacteria responsible for impetigo are Staphylococcus aureus or Streptococcus pyogenes. These bacteria can enter the body through open wounds, cuts, insect bites, or even through healthy skin.
Transmission through direct contact
Impetigo is easily spread through direct contact with an infected individual or by touching contaminated objects. It commonly affects children, as they are more likely to come into close contact with each other during play or in school settings. Adults can also contract impetigo if they have open wounds or compromised immune systems.
Risk factors
Certain factors increase the risk of contracting impetigo. Poor hygiene and crowded living conditions can contribute to the spread of bacteria, making it more likely for someone to develop impetigo. Additionally, individuals with pre-existing skin conditions, such as eczema, are more susceptible to bacterial infections like impetigo.
Poor hygiene and crowded living conditions
Poor personal hygiene practices, including infrequent handwashing and not keeping clean, can promote the growth and spread of bacteria that cause impetigo. Living in overcrowded environments, such as schools or daycare centers, can also increase the likelihood of transmission due to close proximity between individuals.
Symptoms
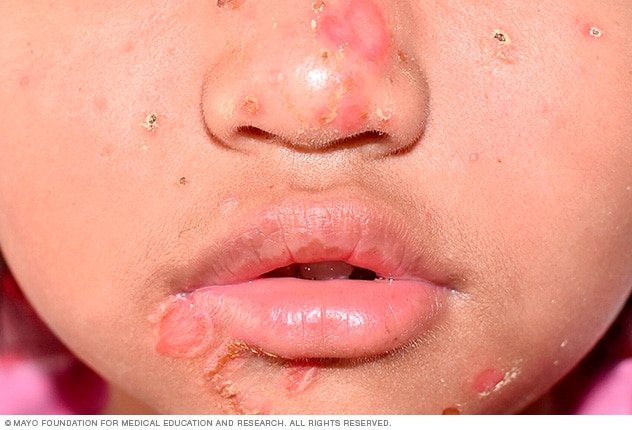
Appearance of sores
The first sign of impetigo is the appearance of small, red sores that can quickly spread and develop into larger patches. These sores are usually found on the face, particularly around the mouth and nose, but can also occur on other parts of the body. The sores may burst and ooze a yellowish fluid, forming a characteristic honey-colored crust.
Fluid-filled blisters
Impetigo can also present as fluid-filled blisters, which are often larger and appear more prominently on the skin. These blisters are fragile and may burst easily, causing the honey-colored crust to form. It’s important to be cautious while handling the blisters to prevent further spread of the infection.
Honey-colored crusts
One of the classic signs of impetigo is the formation of honey-colored crusts on the affected areas. These crusts are a result of the dried yellowish fluid that oozes from the sores or blisters. The crusts can be itchy and may cause discomfort or pain when touched.
Itching and pain
Impetigo can cause itching and discomfort in the affected areas. Itching is a common symptom, which can lead to scratching and potentially spreading the infection to other parts of the body. Though impetigo is not typically painful, some individuals may experience mild pain or tenderness around the sores or blisters.
Swollen lymph nodes
In some cases, impetigo can cause swelling of the lymph nodes near the affected area. Lymph nodes are part of the body’s immune system and can become enlarged as they work to fight off the infection. Swollen lymph nodes are usually temporary and will return to their normal size once the infection is treated.

Diagnosis
Physical examination
To diagnose impetigo, a healthcare provider will typically perform a physical examination of the affected area. They will examine the characteristic sores, blisters, or honey-colored crusts and evaluate the distribution and extent of the infection.
Bacterial culture
In certain cases, a bacterial culture may be performed to confirm the presence of bacteria causing impetigo. During this test, a sample of fluid or tissue from the affected area is collected and sent to a laboratory, where the bacteria can be identified and assessed for antibiotic susceptibility.
Differential diagnosis
In some instances, impetigo may be confused with other skin conditions, such as eczema or herpes simplex virus infection. Differential diagnosis involves ruling out other potential causes by considering the specific symptoms, distribution of lesions, and possibly conducting additional tests.
Complications
Cellulitis
If left untreated, impetigo can lead to cellulitis, a more serious infection that affects the deeper layers of the skin. Cellulitis typically causes redness, warmth, and tenderness in the affected area. It is important to seek prompt treatment for impetigo to prevent the development of cellulitis.
Ecthyma
Ecthyma is a deeper form of impetigo that can result in ulceration and formation of thick, scab-like crusts. It is often more painful and takes longer to heal compared to typical impetigo. Ecthyma can leave scars or pigment changes on the skin after the infection resolves.
Post-streptococcal glomerulonephritis
Rarely, impetigo caused by certain strains of Streptococcus bacteria can lead to a condition called post-streptococcal glomerulonephritis. This involves inflammation of the kidney’s filtering units and can result in symptoms such as blood in the urine, swelling, and high blood pressure. Prompt treatment of impetigo reduces the risk of developing this complication.
Treatment
Topical antibiotics
Most cases of impetigo can be treated with topical antibiotics. These medications are applied directly to the affected area, helping to kill the bacteria and promote healing. Topical antibiotics may be available in the form of creams or ointments and should be used as directed by a healthcare professional.
Oral antibiotics
For more severe or widespread cases of impetigo, oral antibiotics may be prescribed. These medications work systemically to eliminate the infection from within the body. It’s important to complete the full course of antibiotics as prescribed, even if symptoms improve before finishing the treatment.
Wound care
Proper wound care is crucial in managing impetigo. Keeping the affected area clean and dry can help prevent further infection and promote healing. Gently washing the sores or blisters with mild soap and water, followed by the application of antibiotic ointment and clean dressings, can aid in the healing process.
Symptom relief
To alleviate symptoms such as itching and discomfort, over-the-counter pain relievers and antihistamines may be recommended. It is important to consult a healthcare professional before taking any medications, especially for children or if you have any pre-existing medical conditions.
Preventive measures
Preventing the spread of impetigo can be achieved through various measures. Good hygiene practices, such as regular handwashing with soap and water, can help minimize the risk of infection. Prompt treatment of skin injuries, such as cuts or scrapes, can also prevent the entry of bacteria. Avoiding close contact with infected individuals or sharing personal items can further reduce the chances of transmission. Vaccination against certain bacterial strains associated with impetigo may also be available in some cases.
Prevention
Good hygiene practices
Practicing good hygiene is essential in preventing impetigo. This includes washing your hands thoroughly with soap and water, especially before and after touching infected areas or coming into contact with potentially contaminated objects.
Prompt treatment of skin injuries
Any skin injuries, such as cuts, scrapes, or insect bites, should be promptly cleaned and treated with an antiseptic to reduce the risk of bacterial infection. Keeping wounds covered with clean dressings can further prevent the entry of bacteria.
Avoiding close contact with infected individuals
To minimize the risk of impetigo transmission, it is important to avoid close contact with individuals who have active infections. This includes refraining from sharing personal items such as towels, clothing, or bedding, which can potentially harbor bacteria.
Vaccination
Vaccination may be an option for preventing specific strains of bacteria associated with impetigo. Consultation with a healthcare professional can help determine if vaccination is recommended based on individual circumstances, particularly for those at higher risk of developing impetigo or complications.
In conclusion, impetigo is a common bacterial skin infection that can be easily spread through direct contact. Maintaining good hygiene practices and promptly treating skin injuries are key preventive measures. If symptoms of impetigo occur, seeking medical attention for diagnosis and appropriate treatment is crucial to prevent complications and to ensure a full recovery.