In the world of health and wellness, understanding the complexities of our bodies is paramount. One key factor that has been gaining attention is the role of insulin resistance in metabolic syndrome. Insulin resistance is a condition where the body’s cells become less responsive to insulin, a hormone responsible for regulating blood sugar levels. This article aims to shed light on the connection between insulin resistance and metabolic syndrome, exploring the impact it has on our overall health and well-being. By uncovering this vital information, we can take proactive steps towards preventing and managing this syndrome for a healthier future.

The Role of Insulin Resistance in Metabolic Syndrome
Insulin Resistance is a condition that plays a significant role in the development of Metabolic Syndrome, a cluster of conditions that increase the risk of heart disease, stroke, and diabetes. By understanding the causes and effects of insulin resistance, we can better comprehend its link to metabolic syndrome and explore potential treatments and interventions.
1. Understanding Insulin Resistance
Definition of Insulin Resistance
Insulin Resistance is a condition in which the body’s cells become less responsive to the effects of insulin, a hormone produced by the pancreas that helps regulate blood sugar levels. When cells are resistant to insulin, they fail to effectively take up glucose from the bloodstream, causing blood sugar levels to rise.
How Insulin Resistance Develops
Insulin Resistance usually develops gradually over time due to a combination of genetic and lifestyle factors. Factors such as obesity, physical inactivity, and poor dietary choices contribute to the development of insulin resistance. Over time, the body’s cells become less sensitive to insulin, leading to an impaired ability to regulate blood sugar levels.
Effects of Insulin Resistance on Glucose Metabolism
In individuals with insulin resistance, the body’s cells do not respond adequately to insulin, impairing the uptake of glucose from the bloodstream. As a result, blood sugar levels remain high, leading to hyperglycemia. This persistent elevation in blood sugar can eventually contribute to the development of prediabetes and type 2 diabetes.
Impact of Insulin Resistance on Lipid Metabolism
Insulin resistance also has a significant impact on lipid metabolism. When cells become resistant to insulin, the body compensates by producing more insulin. This excess insulin promotes the production of triglycerides and inhibits the breakdown of fats, leading to elevated levels of triglycerides and low-density lipoprotein (LDL) cholesterol. These lipid abnormalities increase the risk of cardiovascular disease.
Role of Insulin Resistance in Inflammation
Insulin resistance is closely linked to chronic low-grade inflammation within the body. It is believed that insulin resistance itself promotes the release of inflammatory molecules, contributing to the development of chronic inflammation. This chronic inflammation is an underlying factor in the pathogenesis of various metabolic disorders, including metabolic syndrome.

2. Risk Factors for Insulin Resistance
Obesity
Obesity is a significant risk factor for insulin resistance. Excess body fat, especially visceral fat (fat around the abdomen), promotes the release of inflammatory molecules that disrupt insulin signaling. Furthermore, adipose tissue releases adipokines, hormones that can interfere with insulin action, further exacerbating insulin resistance.
Physical Inactivity
Leading a sedentary lifestyle and lack of regular physical activity are associated with an increased risk of insulin resistance. Physical activity helps improve insulin sensitivity and promotes glucose uptake by the muscles, thereby reducing the risk of insulin resistance.
Genetic Predisposition
Genetic factors also play a role in the development of insulin resistance. Certain genes may influence insulin signaling pathways, making individuals more susceptible to developing insulin resistance. However, having a genetic predisposition does not guarantee the development of insulin resistance, as lifestyle factors also significantly contribute to its development.
Ethnicity and Insulin Resistance
Certain ethnicities, such as individuals of South Asian, Hispanic, African, and Native American descent, have a higher prevalence of insulin resistance compared to other population groups. These ethnic groups are also more prone to developing metabolic syndrome and related complications.
Age and Insulin Resistance
With age, the risk of developing insulin resistance increases. This may be attributed to age-related changes in body composition, reduced physical activity, and hormonal alterations. Aging individuals should be particularly mindful of their lifestyle choices to minimize the risk of developing insulin resistance.
Gestational Diabetes
Women who have had gestational diabetes during pregnancy are at higher risk of developing insulin resistance later in life. Gestational diabetes is a condition that occurs during pregnancy, where insulin resistance impairs the body’s ability to regulate blood sugar levels. These women should be closely monitored for the development of insulin resistance and metabolic syndrome post-pregnancy.
3. The Link Between Insulin Resistance and Metabolic Syndrome
Definition and Components of Metabolic Syndrome
Metabolic Syndrome is a cluster of conditions that occur together and increase the risk of cardiovascular disease, stroke, and type 2 diabetes. The diagnostic criteria for metabolic syndrome include abdominal obesity, elevated blood pressure, elevated blood sugar levels, elevated triglycerides, and reduced high-density lipoprotein (HDL) cholesterol levels.
Prevalence of Insulin Resistance in Metabolic Syndrome
Insulin resistance is a key underlying factor in the development of metabolic syndrome. Studies have shown that the majority of individuals with metabolic syndrome have underlying insulin resistance. The presence of insulin resistance contributes to the systemic dysregulation of glucose and lipid metabolism, leading to the development of the various components of metabolic syndrome.
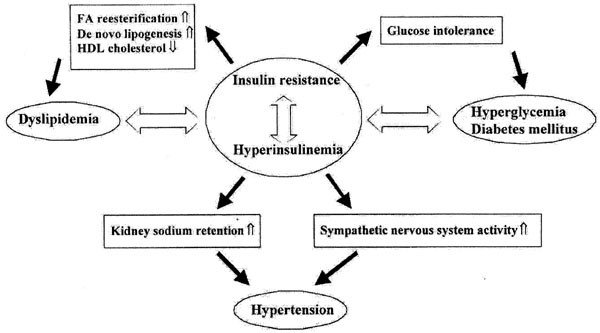
Impact of Insulin Resistance on the Development of Metabolic Syndrome
Insulin resistance plays a pivotal role in the development and progression of metabolic syndrome. Insulin resistance disrupts the balance between insulin production and insulin action, leading to hyperinsulinemia, elevated blood glucose levels, and dyslipidemia. These metabolic abnormalities contribute to the development of the various components of metabolic syndrome.
Role of Insulin Resistance in Abdominal Obesity
Abdominal obesity, characterized by excess fat accumulation around the waistline, is a hallmark component of metabolic syndrome. Insulin resistance promotes the storage of fat in the abdominal region, leading to visceral fat accumulation. Visceral fat is particularly detrimental as it releases inflammatory molecules and hormones that exacerbate insulin resistance and contribute to the development of metabolic syndrome.
Insulin Resistance and Dyslipidemia
Insulin resistance disrupts lipid metabolism, leading to dyslipidemia, a condition characterized by abnormal lipid levels in the blood. Insulin resistance promotes the production of triglycerides while inhibiting the breakdown of fats. This leads to elevated levels of triglycerides and LDL cholesterol and reduced levels of HDL cholesterol, contributing to the development of metabolic syndrome.
Insulin Resistance and Hypertension
Insulin resistance has been associated with elevated blood pressure levels, another component of metabolic syndrome. The exact mechanisms linking insulin resistance to hypertension are not fully understood, but it is believed that insulin resistance contributes to the impairment of blood vessel function and increases sodium reabsorption, leading to increased blood pressure.
Insulin Resistance and Pro-Inflammatory State
Insulin resistance is closely associated with chronic low-grade inflammation, which is a contributing factor in the development of metabolic syndrome. Inflammatory molecules released by adipose tissue and other cells promote the disruption of insulin signaling, exacerbating insulin resistance. This chronic inflammatory state further contributes to the development and progression of metabolic syndrome.
Insulin Resistance and Cardiovascular Disease
Insulin resistance significantly increases the risk of cardiovascular disease. The combination of dyslipidemia, hypertension, hyperglycemia, and chronic inflammation associated with insulin resistance accelerates atherosclerosis, the buildup of plaque in the arteries. This increases the risk of heart attacks, strokes, and other cardiovascular complications.
Insulin Resistance and Type 2 Diabetes
Insulin resistance is a major risk factor for the development of type 2 diabetes. When insulin resistance is present, the pancreas compensates by producing more insulin. Over time, the pancreas may become overwhelmed and fail to produce enough insulin to overcome insulin resistance, resulting in high blood sugar levels and the development of type 2 diabetes.
Treatments and Interventions Targeting Insulin Resistance in Metabolic Syndrome
The management of insulin resistance in metabolic syndrome involves a multi-faceted approach. Lifestyle modifications such as regular physical activity, a healthy diet, weight loss, and smoking cessation are essential components of treatment. In some cases, pharmacological interventions may also be necessary to improve insulin sensitivity and manage metabolic abnormalities.

4. Clinical Diagnosis and Management of Insulin Resistance
Diagnostic Criteria for Insulin Resistance
Insulin resistance is not typically diagnosed directly but rather inferred from certain metabolic assessments. Tests such as fasting insulin levels, fasting glucose levels, and the Homeostatic Model Assessment of Insulin Resistance (HOMA-IR) can provide insights into insulin resistance status. However, it is important to note that these tests are not definitive and should be interpreted in the context of the individual’s overall health and risk factors.
Assessment of Insulin Resistance
The assessment of insulin resistance involves a comprehensive evaluation of an individual’s medical history, physical examination, and laboratory tests. Alongside fasting insulin and glucose levels, other parameters such as hemoglobin A1c, lipid profile, and markers of inflammation may be assessed to evaluate the severity and impact of insulin resistance.
Lifestyle Modifications for Insulin Resistance
Lifestyle modifications are fundamental in the management of insulin resistance. Regular physical activity, including aerobic exercises and resistance training, helps improve insulin sensitivity and promotes glucose uptake by the muscles. A healthy, balanced diet with a focus on whole grains, lean proteins, fruits, vegetables, and healthy fats can also aid in managing insulin resistance.
Pharmacological Interventions for Insulin Resistance
In some cases, lifestyle modifications alone may not be sufficient to manage insulin resistance effectively. Pharmacological interventions may be prescribed to improve insulin sensitivity or manage associated conditions such as dyslipidemia and hypertension. Medications such as metformin, thiazolidinediones, statins, and antihypertensive drugs may be utilized based on individual needs and medical history.
5. Future Directions and Research
Emerging Therapies for Insulin Resistance
Research is continuously advancing in the field of insulin resistance, aiming to identify novel therapeutic approaches. Emerging therapies include the use of incretin-based therapies, such as glucagon-like peptide-1 (GLP-1) receptor agonists and dipeptidyl peptidase-4 (DPP-4) inhibitors, that enhance insulin secretion and improve insulin sensitivity. Additionally, investigations into insulin sensitizers and medications that target specific pathways involved in insulin resistance are ongoing.
Advancements in Genetic Studies of Insulin Resistance
Understanding the genetic factors contributing to insulin resistance is crucial in developing personalized treatments. Advances in genetic studies have identified various genes and genetic variants associated with insulin resistance. Further research in this area may lead to the development of genetic screening tools and personalized treatments targeted at individuals with specific genetic predispositions.
Potential Personalized Treatments for Insulin Resistance
With the advancements in genetic and molecular research, there is a growing interest in personalized treatments for insulin resistance. Tailoring therapies based on an individual’s genetic profile, metabolic characteristics, and response to treatment may help optimize outcomes and improve the management of insulin resistance.
Investigation of Insulin Resistance and Metabolic Syndrome in Children
As the prevalence of childhood obesity and metabolic disorders continues to rise, understanding the development and impact of insulin resistance in children is crucial. Research is investigating the relationships between insulin resistance, metabolic syndrome, and long-term health outcomes in pediatric populations. This knowledge can aid in developing early intervention strategies and preventive measures to mitigate the long-term consequences of insulin resistance.
In conclusion, insulin resistance plays a crucial role in the development and progression of metabolic syndrome. Understanding the causes, effects, and interventions associated with insulin resistance is vital in combating the detrimental health outcomes linked to this condition. Through further research and advancements in personalized treatments, we can strive towards better management and prevention of insulin resistance and metabolic syndrome.