You’re about to discover a comprehensive guide that sheds light on one of the most misunderstood autoimmune diseases: Lupus. In this article, we’ll explore the causes, symptoms, and treatments associated with Lupus, providing you with the knowledge you need to understand this condition better. Whether you’re seeking answers for yourself or someone you care about, prepare to gain valuable insights into the world of Lupus and equip yourself with the information to face it head-on. Lupus, a chronic autoimmune disease, affects millions of people worldwide. It is a complex condition that can have a significant impact on your daily life. Understanding the causes, symptoms, and treatment options for lupus is crucial in managing the condition effectively.

Causes
Genetic Factors
Research suggests that lupus can have a genetic component, meaning that certain genes may increase the likelihood of developing the disease. However, it is important to note that genetics alone cannot determine the onset of lupus. Other factors, such as environmental triggers, play a significant role as well.
Environmental Triggers
Environmental triggers, including exposure to certain medications, infections, and hormonal changes, may contribute to the development of lupus. Ultraviolet (UV) light from the sun is also known to be a common trigger for lupus flares. It is essential to be mindful of these triggers and take necessary precautions to minimize their impact.
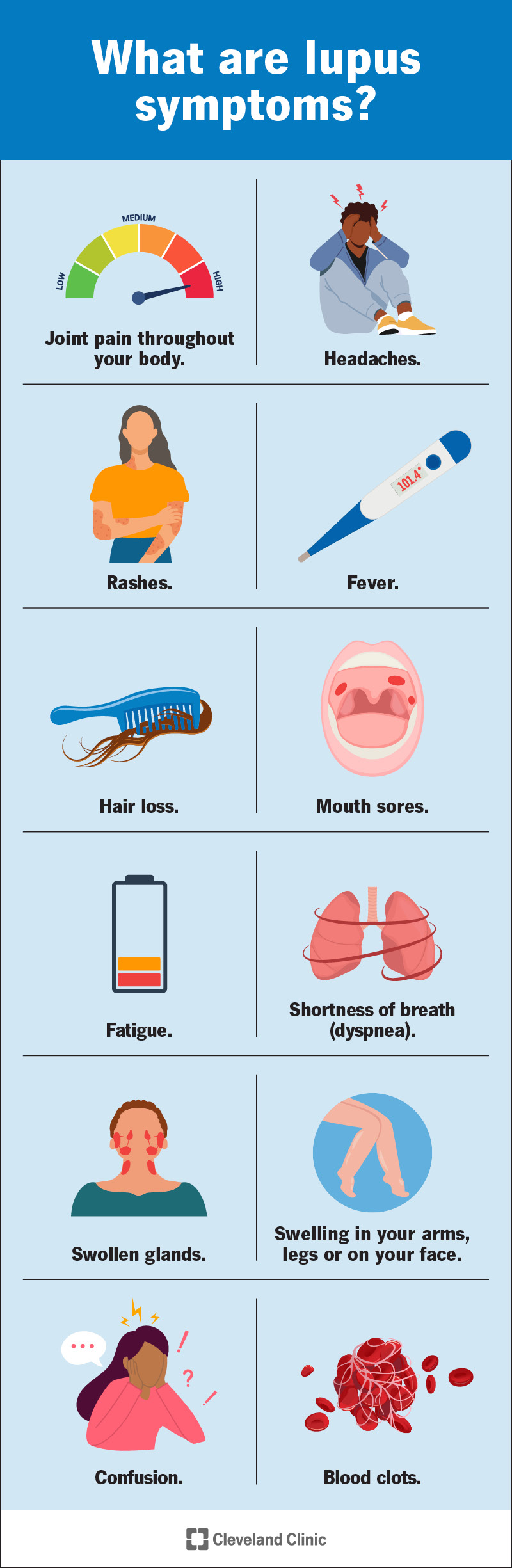
Symptoms
Butterfly Rash
One of the hallmark symptoms of lupus is a butterfly-shaped rash across the cheeks and nose, known as a malar rash. This rash is usually red or purple in color and may be accompanied by itching or pain. It is important to note that not all individuals with lupus will experience this rash, and its presence can vary from person to person.
Joint Pain
Many individuals with lupus experience joint pain and stiffness, often resembling symptoms of arthritis. This pain can affect various joints in the body, including the hands, wrists, knees, and ankles. Regular exercise and appropriate medication can help manage this symptom and improve overall joint function.
Fatigue
Fatigue is a common symptom of lupus and can range from mild to severe. This persistent feeling of exhaustion can significantly impact your daily life. It is important to listen to your body and take breaks when needed. Prioritizing rest and maintaining a healthy lifestyle can help combat fatigue.
Diagnosis
Medical History
To diagnose lupus, your doctor will first conduct a thorough medical history evaluation. They will ask questions about your symptoms, their duration and intensity, and any relevant family history. Providing detailed and accurate information during this stage is crucial in formulating an accurate diagnosis.
Physical Examination
A physical examination will be conducted to assess your overall health and any visible symptoms or signs of lupus. This may include examining your skin, joints, and overall physical appearance for any specific lupus-related findings.
Laboratory Tests
Laboratory tests are essential in diagnosing lupus. Blood tests can detect certain antibodies commonly found in individuals with lupus, such as antinuclear antibodies (ANA) and anti-double stranded DNA antibodies (anti-dsDNA). Other tests may be ordered to assess kidney and liver function as well.
Imaging Tests
In some cases, imaging tests such as X-rays, ultrasounds, or MRI scans may be conducted to assess any specific organ involvement or damage. These tests help evaluate the extent of the disease and guide treatment decisions.
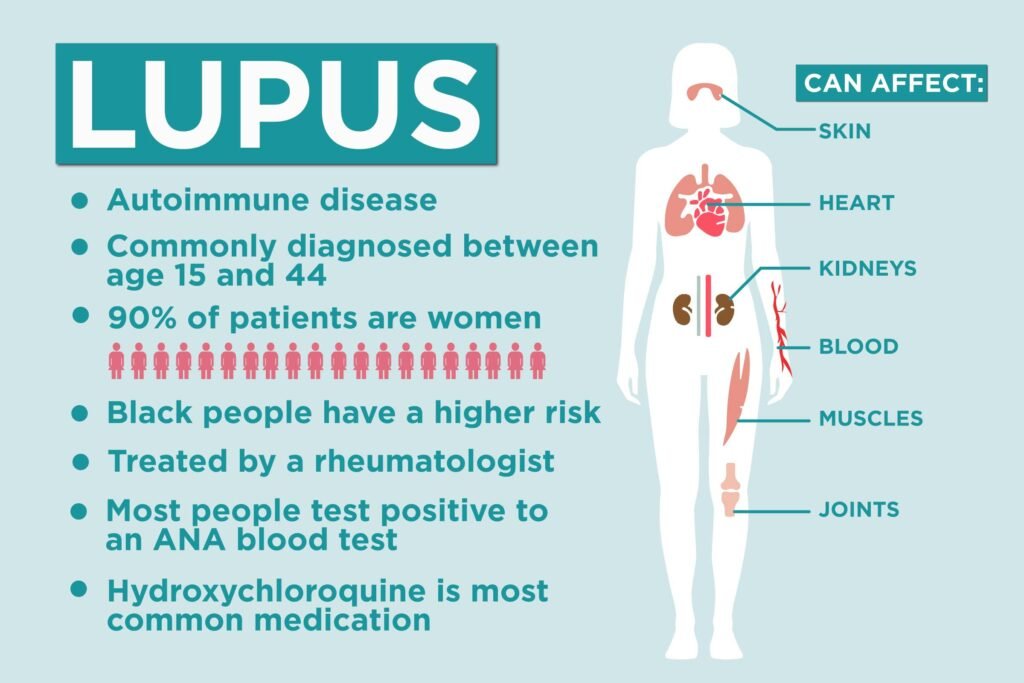
Types of Lupus
Systemic Lupus Erythematosus (SLE)
Systemic Lupus Erythematosus is the most common and severe form of lupus. It can affect multiple organ systems, including the skin, joints, kidneys, heart, and lungs. SLE symptoms can be diverse and vary significantly from person to person.
Discoid Lupus Erythematosus (DLE)
Discoid Lupus Erythematosus primarily affects the skin, causing characteristic disc-shaped rashes, usually on the face, scalp, and ears. This form of lupus is generally less severe than SLE, but it can still cause discomfort and impact one’s self-esteem.
Subacute Cutaneous Lupus Erythematosus (SCLE)
Subacute Cutaneous Lupus Erythematosus primarily affects the skin and is often triggered by exposure to sunlight. It is characterized by distinct rashes, typically in sun-exposed areas such as the upper back, shoulders, and chest.
Drug-Induced Lupus Erythematosus (DILE)
Drug-Induced Lupus Erythematosus is a form of lupus that develops as a side effect of certain medications. Symptoms usually resolve once the medication is discontinued. Common drugs associated with DILE include hydralazine, procainamide, and certain anti-seizure medications.
Complications
Kidney Damage
Lupus can cause inflammation in the kidneys, leading to kidney damage or failure if left untreated. Regular monitoring and early intervention can help manage kidney complications effectively.
Heart and Lung Problems
Inflammation in the heart and lungs can occur in individuals with lupus, leading to various complications such as pericarditis, myocarditis, and pleurisy. Maintaining a healthy lifestyle and monitoring these organs regularly can reduce the risk and impact of such complications.
Central Nervous System Issues
Some individuals with lupus may experience neurological symptoms, such as headaches, seizures, cognitive impairments, and mood disorders. Prompt recognition and appropriate management of these symptoms are crucial to minimize their impact on daily functioning.
Pregnancy Complications
Pregnancy can pose additional challenges for individuals with lupus. It is essential to consult with your healthcare provider if you are planning a pregnancy, as lupus can increase the risk of complications such as pre-eclampsia and preterm birth. Close monitoring and appropriate management can help ensure a healthy pregnancy.
Treatment
Medications
Medications are typically the cornerstone of lupus treatment. Nonsteroidal anti-inflammatory drugs (NSAIDs) and corticosteroids are commonly used to manage symptoms such as joint pain and inflammation. Immunosuppressants and antimalarial drugs are also prescribed to control the immune response and reduce disease activity.
Lifestyle Changes
Making certain lifestyle changes can complement medical treatment and help manage lupus effectively. Sun protection is crucial in preventing flares, as UV light can trigger symptoms. Regular exercise can improve joint flexibility and overall well-being. Adopting a healthy diet rich in fruits, vegetables, and omega-3 fatty acids can support immune function and reduce inflammation.
Alternative Therapies
Some individuals with lupus find alternative therapies helpful in managing their symptoms. Acupuncture, herbal supplements, massage therapy, and mind-body techniques such as meditation and yoga are some examples. However, it is essential to consult with your healthcare provider before incorporating these therapies into your treatment plan.

Coping with Lupus
Seeking Support
Living with lupus can be challenging, both physically and emotionally. Seeking support from friends, family, or support groups can provide a valuable network of understanding and encouragement. Sharing your experiences and learning from others who have faced similar challenges can help you cope more effectively.
Managing Stress
Stress management plays a vital role in managing lupus symptoms. High levels of stress can trigger flares and worsen symptoms. Engaging in activities that reduce stress and promote relaxation, such as mindfulness exercises, hobbies, and deep breathing techniques, can significantly improve overall well-being.
Self-Care Practices
Taking care of yourself is essential when living with lupus. Prioritizing rest and getting enough sleep can help manage fatigue and allow your body to heal. Setting realistic goals and pacing yourself are also crucial in balancing your energy levels. It is important to listen to your body and take breaks when needed.
In conclusion, understanding lupus, its causes, symptoms, and treatment options is key to effectively managing the disease. By working closely with healthcare professionals, making necessary lifestyle changes, and seeking support, individuals with lupus can lead fulfilling lives despite the challenges posed by this chronic condition.