Lymphogranuloma Venereum, also known as LGV, is a sexually transmitted infection that is rapidly gaining attention due to its increasing prevalence. This article aims to provide a comprehensive understanding of LGV, including its symptoms, transmission, and treatment options. By shedding light on this often overlooked infection, we hope to equip you with the knowledge necessary to protect yourself and others from the potential risks posed by LGV.
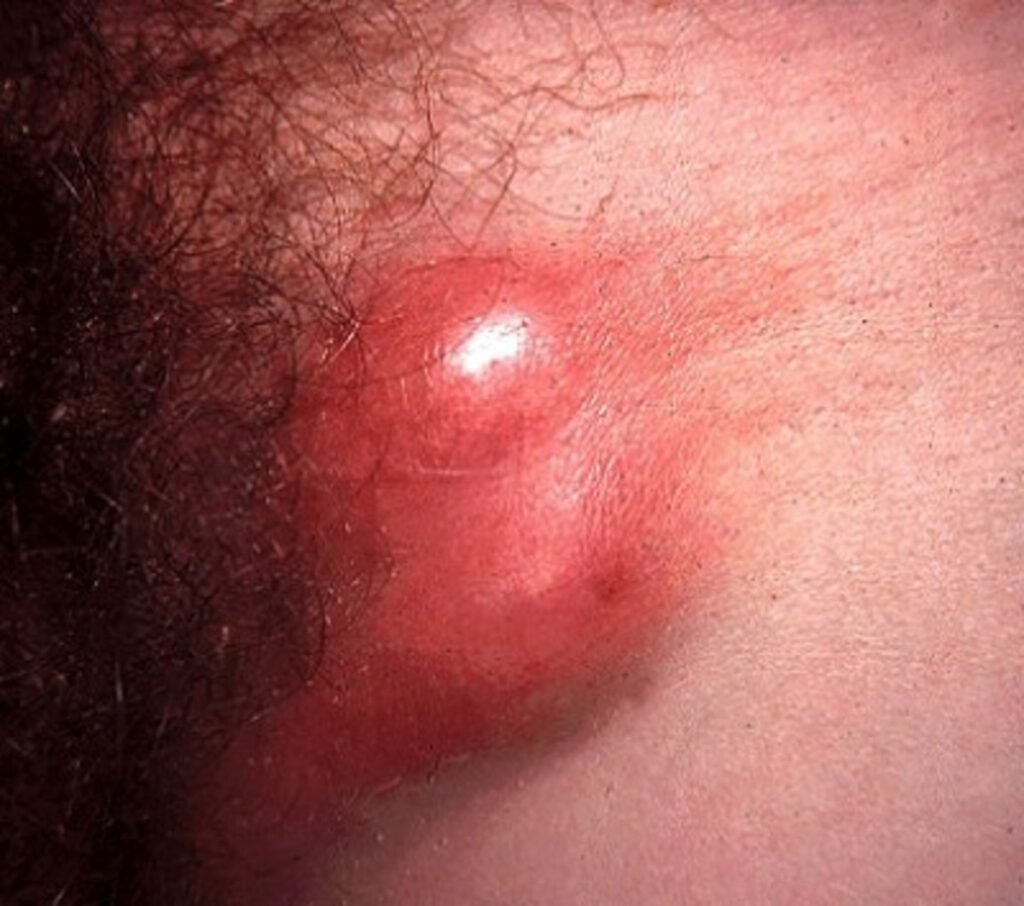
Symptoms of LGV
Initial symptoms of LGV
The initial symptoms of LGV can be quite mild and easily overlooked. They often appear within three to 30 days after exposure to the bacteria that cause the infection. One of the most common early symptoms is the presence of small, painless sores or ulcers on the genitals or around the anus. These sores may go unnoticed and heal on their own.
Later symptoms of LGV
If left untreated, LGV can progress to more severe symptoms. This usually occurs a few weeks after the initial infection. Swollen lymph nodes in the groin or pelvic area are a characteristic feature of LGV. These swollen nodes may be painful, warm to the touch, and can sometimes break open, forming painful abscesses. Other symptoms that may develop include fever, fatigue, muscle aches, and a general feeling of being unwell.
Complications of LGV
Without proper treatment, LGV can lead to serious complications. One of the most significant complications is the scarring and narrowing of the lymphatic vessels in the genital area. This can cause long-term damage and chronic swelling known as lymphedema. In some cases, LGV can also affect other organs, such as the rectum or intestines, leading to complications like rectal strictures or fistulas.
Causes and Transmission of LGV
Causes of LGV
LGV is caused by a specific type of bacteria called Chlamydia trachomatis. This bacterium has different strains, and those associated with LGV are known as L1, L2, and L3. These strains are usually transmitted through sexual contact, including vaginal, anal, or oral sex. It is important to note that LGV is relatively uncommon in regions where routine screening and treatment for sexually transmitted infections (STIs) are accessible.
Transmission of LGV
LGV is primarily transmitted through sexual contact with an infected individual. Unprotected intercourse, including vaginal, anal, or oral sex, can all lead to the transmission of LGV. It is also possible to contract LGV through contact with contaminated objects, although this method of transmission is less common. It is important to practice safe sex to prevent the spread of LGV and other sexually transmitted infections.
Diagnosis of LGV
Physical examination and medical history
When diagnosing LGV, healthcare professionals will typically start by conducting a physical examination and reviewing the patient’s medical history. During the physical examination, they will look for any signs of swollen lymph nodes or other symptoms associated with LGV. It is crucial to provide accurate information about any sexual encounters, including the number of partners and the type of sexual activity involved, to assist in making an accurate diagnosis.
Laboratory tests for LGV
Laboratory tests are often necessary to confirm the diagnosis of LGV. These tests may include the collection of samples from the affected area, such as swabs from genital ulcers or rectal swabs. These samples are then sent to a laboratory to be tested for the presence of Chlamydia trachomatis DNA or antigens. Additional blood tests may also be performed to check for antibodies against the bacteria.
Testing for LGV in specific body parts
If LGV is suspected in a specific body part, additional testing may be required. For example, if LGV is suspected to affect the rectum, a proctoscopy may be performed. This procedure involves inserting a thin tube with a camera into the rectum to examine the area for any signs of infection or damage. Testing for LGV in specific body parts helps ensure an accurate diagnosis and appropriate treatment.
Treatment of LGV
Antibiotics for LGV
The primary treatment for LGV is a course of antibiotics. The specific antibiotics prescribed will depend on the severity and stage of the infection. Doxycycline or azithromycin are commonly used to treat LGV. It is essential to take the prescribed antibiotics for the full duration as directed by the healthcare provider to ensure the complete eradication of the bacteria.
Duration of treatment
The duration of treatment for LGV can vary. Typically, a course of antibiotics lasts for at least three weeks. In some cases, treatment may be extended to several months, especially if complications or delay in diagnosis has occurred. It is crucial to complete the full course of antibiotics as prescribed, even if symptoms improve or disappear, to prevent recurrence and the development of antibiotic-resistant strains.
Follow-up testing and monitoring
After completing treatment for LGV, follow-up testing is essential to ensure the effectiveness of the antibiotics and to detect any potential complications or re-infections. It is recommended to undergo testing approximately three months after completing the treatment. Regular monitoring and follow-up also help in assessing the healing progress and preventing any long-term consequences.
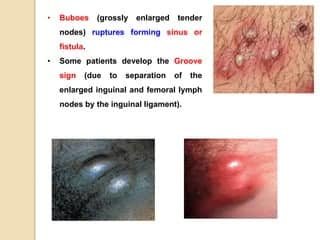
Prevention of LGV
Safe sexual practices
Practicing safe sex is crucial in preventing the transmission of LGV and other sexually transmitted infections. This includes consistently and correctly using condoms during sexual intercourse, whether it is vaginal, anal, or oral sex. Limiting the number of sexual partners and getting tested regularly for STIs can also significantly reduce the risk of contracting LGV.
Vaccination for LGV
Currently, there is no specific vaccine available for LGV. However, routine vaccination against other strains of Chlamydia trachomatis, such as those causing genital chlamydia, can indirectly help in preventing LGV transmission. It is essential to discuss vaccination options with a healthcare provider to ensure protection against other sexually transmitted infections.
Risks and Complications of LGV
Long-term complications of LGV
LGV can lead to various long-term complications if left untreated or poorly managed. As mentioned earlier, one of the significant complications is the scarring and narrowing of the lymphatic vessels, which causes chronic swelling and discomfort. Other potential long-term complications include damage to the rectum, intestines, or genitals, leading to strictures, fistulas, or chronic pain.
Increased risk of HIV transmission
Individuals infected with LGV may have an increased risk of HIV transmission. The presence of LGV can cause inflammation and ulcers in the genital area, which can facilitate the entry and transmission of the HIV virus. It is crucial for individuals diagnosed with LGV to take appropriate precautions to prevent any additional infections, including HIV.
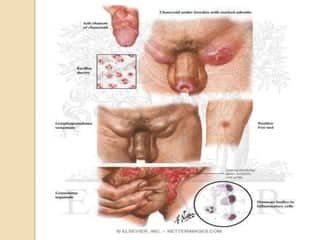
LGV in Specific Populations
LGV in men who have sex with men (MSM)
LGV is of particular importance in men who have sex with men (MSM) due to the increased risk of transmission within this population. MSM are more likely to engage in unprotected anal intercourse, which is a higher-risk activity for the transmission of LGV. Therefore, it is crucial for MSM to be aware of the symptoms of LGV and seek prompt medical attention if any signs or symptoms arise.
LGV in women
While LGV is often associated with men, it can also affect women. The symptoms of LGV in women can resemble other sexually transmitted infections, making it challenging to diagnose. It is essential for women to undergo regular check-ups, discuss any symptoms, and provide accurate information about sexual history with their healthcare providers. Early diagnosis and treatment are crucial in preventing complications.
LGV in immunocompromised individuals
Immunocompromised individuals, such as those living with HIV/AIDS or those undergoing immunosuppressive treatment, may be more susceptible to LGV and its complications. These individuals should work closely with their healthcare providers to ensure regular monitoring, early detection, and appropriate treatment. Adhering to antiretroviral therapy and immune-boosting measures can help reduce the risk of LGV in this population.
Public Health Measures for LGV
Surveillance and reporting
Public health officials play a crucial role in monitoring, surveillance, and reporting cases of LGV. These measures help identify any patterns or outbreaks and guide public health interventions. Healthcare providers are required to report cases of LGV promptly to local health departments to facilitate appropriate public health responses.
Partner notification and contact tracing
Partner notification and contact tracing are vital in controlling the spread of LGV. When a case is diagnosed, healthcare providers or public health officials work with the affected individual to identify and notify any recent sexual partners. These partners can then receive testing and treatment to prevent further transmission. Confidentiality and sensitivity are essential during this process to encourage cooperation and prevent stigma.
Health education and awareness
Health education and awareness initiatives are fundamental in preventing LGV and promoting overall sexual health. Public health agencies, healthcare providers, and community organizations play a critical role in educating individuals about the risks, symptoms, and prevention methods of LGV. Increasing awareness of available testing, treatment, and prevention options can empower individuals to make informed decisions and protect themselves and their partners.
Resources and Support for LGV
Medical resources for LGV
Various medical resources are available for individuals seeking information and support for LGV. Local healthcare providers, clinics specializing in sexual health, and public health agencies can provide accurate and up-to-date information on LGV. These resources can help individuals understand the disease, access appropriate testing and treatment, and connect with healthcare professionals experienced in managing LGV.
Support groups for individuals with LGV
Support groups can be invaluable for individuals diagnosed with LGV. These groups provide a safe and understanding environment where individuals can share experiences, receive emotional support, and access practical advice. Online forums, community-based organizations, and specialized helplines are some sources that offer support to those dealing with the physical and emotional aspects of LGV.
Conclusion
Lymphogranuloma Venereum (LGV) is a sexually transmitted infection caused by certain strains of Chlamydia trachomatis. It can cause a range of symptoms, from mild ulcers to severe swelling of the lymph nodes. Without proper treatment, LGV can lead to long-term complications and an increased risk of HIV transmission. However, with early diagnosis and appropriate antibiotics, LGV can be effectively treated. Practicing safe sex, seeking regular STI testing, and raising awareness about LGV are vital in preventing its spread. By understanding the symptoms, causes, and prevention methods, individuals can take control of their sexual health and minimize the impact of LGV on their lives.