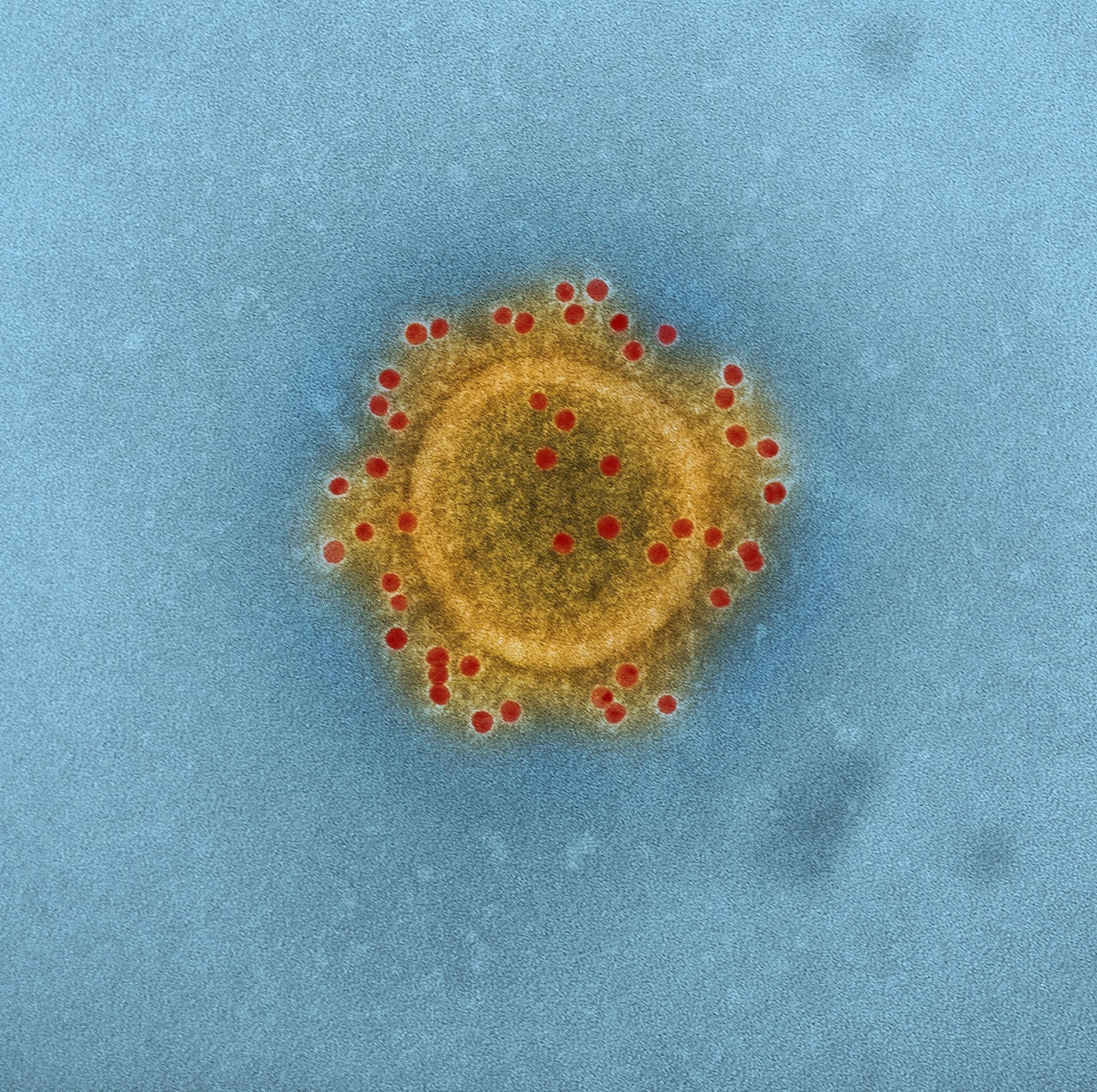
In this article, you will gain a deeper understanding of the Middle East Respiratory Syndrome Coronavirus (MERS-CoV) and its impact on the world. As a prevalent virus that emerged in the Middle East, MERS-CoV has raised concerns amongst health professionals and individuals worldwide. By shedding light on its characteristics, symptoms, transmission, and prevention methods, this article aims to empower you with knowledge about this infectious disease and help you stay informed and prepared.
Overview of Middle East Respiratory Syndrome Coronavirus
Middle East Respiratory Syndrome Coronavirus (MERS-CoV) is a viral infection that was first identified in 2012 in Saudi Arabia. It belongs to the family of coronaviruses, which also includes Severe Acute Respiratory Syndrome Coronavirus (SARS-CoV) and the more recent coronavirus causing COVID-19. MERS-CoV is a zoonotic virus, meaning it primarily infects animals but can be transmitted to humans. The disease caused by MERS-CoV is known as Middle East Respiratory Syndrome (MERS).
Definition
Middle East Respiratory Syndrome (MERS) is a respiratory illness that is caused by the coronavirus MERS-CoV. It is characterized by severe acute respiratory symptoms, including fever, cough, and shortness of breath. MERS can lead to complications such as pneumonia, kidney failure, and even death.
Symptoms
The symptoms of MERS can vary from mild to severe. Common symptoms include fever, cough, and shortness of breath. Some individuals may also experience muscle aches, headache, sore throat, and diarrhea. In severe cases, MERS can lead to respiratory failure, kidney failure, and other organ complications.
Transmission
MERS-CoV can be transmitted from animals to humans and between humans. The primary mode of transmission is through close contact with infected camels or consumption of raw camel products. Human-to-human transmission is possible through close contact with an infected person, especially in healthcare settings. It is important to note that MERS is not highly contagious and typically requires close and prolonged contact for transmission to occur.
Prevention
Preventing MERS involves several key measures. Avoiding close contact with camels and their bodily fluids is crucial, especially for individuals at high risk, such as camel handlers and those working in slaughterhouses. Practicing good respiratory hygiene, such as covering the mouth and nose when coughing or sneezing, can also help prevent the spread of the virus. In healthcare settings, strict infection control measures, including the use of personal protective equipment, are essential in preventing transmission.
History and Origin of Middle East Respiratory Syndrome Coronavirus
Discovery of MERS-CoV
MERS-CoV was first identified in September 2012 when a patient in Saudi Arabia developed severe respiratory symptoms. Further investigation identified the novel coronavirus as the causative agent. The World Health Organization (WHO) declared MERS-CoV a public health emergency in 2013, highlighting the urgency for research and control measures.
First Outbreak
The first outbreak of MERS occurred in Saudi Arabia in 2012 with a cluster of cases linked to a healthcare facility. The source of the outbreak was traced back to camels, which are known reservoirs of MERS-CoV. This initial outbreak raised concerns about the potential global spread of the virus and the need for effective control measures.
Geographical Spread
Since its discovery, MERS-CoV has been reported in several countries across the Middle East, with the majority of cases originating from Saudi Arabia. There have also been sporadic cases reported in other regions, including Europe, North America, and Asia, often associated with travel to or from the Middle East. However, the overall incidence of MERS remains low compared to other respiratory viruses.
Characteristics of Middle East Respiratory Syndrome Coronavirus
Virus Structure
MERS-CoV is a member of the coronavirus family, characterized by its crown-like appearance under an electron microscope. It has a lipid envelope, which makes it susceptible to disinfectants and detergents, and it contains a single-stranded RNA genome. The virus is relatively stable and can survive for a short time on surfaces.
Genetic Makeup
The genome of MERS-CoV consists of approximately 30,000 nucleotides and contains several genes that encode various proteins involved in viral replication and interactions with the host immune system. Genetic sequencing has provided valuable insights into the origin and evolution of MERS-CoV and has aided in the development of diagnostic tests and potential vaccines.
Host Range
While the primary reservoir for MERS-CoV is camels, the virus can infect a range of mammalian species, including humans. The virus has shown the ability to bind to receptors in the respiratory and gastrointestinal tracts, allowing it to enter and invade host cells. Understanding the host range of MERS-CoV is essential for controlling its transmission and preventing future outbreaks.
Clinical Presentation of Middle East Respiratory Syndrome
Incubation Period
The incubation period for MERS ranges from 2 to 14 days, with an average of 5 to 6 days. This is the time between infection with the virus and the onset of symptoms. During this period, individuals may be asymptomatic, making it challenging to identify and isolate cases early.
Common Symptoms
The most common symptoms of MERS include fever, cough, and shortness of breath. These respiratory symptoms can range from mild to severe, with some individuals requiring hospitalization and intensive care. Additional symptoms may include muscle aches, headache, sore throat, and diarrhea. It is important to note that symptoms may vary among individuals.
Severe Complications
In severe cases, MERS can lead to complications such as pneumonia, acute respiratory distress syndrome (ARDS), kidney failure, and multiple organ failure. The mortality rate for MERS is estimated to be around 35%, although this can vary depending on the healthcare infrastructure and the quality of supportive care available.
Diagnostic Procedures for Middle East Respiratory Syndrome
Laboratory Testing
Laboratory testing is essential for diagnosing MERS. This includes collecting samples, such as respiratory secretions, blood, and stool, from suspected cases and testing them for the presence of MERS-CoV. Several laboratory techniques, including molecular assays and viral culture, can be used to detect and confirm the infection.
RT-PCR Analysis
One of the most common diagnostic methods for MERS-CoV is the reverse transcription polymerase chain reaction (RT-PCR) analysis. This test detects the viral RNA in patient samples by amplifying and identifying specific regions of the genome. RT-PCR is highly sensitive and specific and can provide rapid results for timely patient management and control measures.
Serological Assays
Serological assays are used to detect antibodies produced by the immune system in response to MERS-CoV infection. These tests can help determine if an individual has been previously infected with the virus. However, serological assays are not useful for diagnosing acute infections, as it takes time for the immune system to produce detectable levels of antibodies.
Transmission Dynamics of Middle East Respiratory Syndrome
Reservoirs of MERS-CoV
Camels are considered the primary reservoirs for MERS-CoV, as they can carry the virus without showing symptoms. Direct or indirect contact with infected camels, their bodily fluids, or contaminated environments contributes to the transmission of MERS.
Modes of Transmission
Human-to-human transmission of MERS can occur through close contact with an infected individual, particularly in healthcare settings. Respiratory droplets and close contact with respiratory secretions are the main routes of transmission. However, MERS is not highly contagious, and sustained community transmission has not been reported.
Hospital Outbreaks
Hospital outbreaks of MERS have been reported, often linked to insufficient infection control practices. Healthcare workers who come into close contact with infected patients are at a higher risk of acquiring MERS. Implementing strict infection control measures, including isolation of suspected cases and appropriate use of personal protective equipment, is crucial in preventing hospital transmission.
MERS-CoV Treatment and Management
Antiviral Therapy
There is currently no specific antiviral therapy for MERS. However, experimental drugs, such as remdesivir, have shown promise in inhibiting the replication of MERS-CoV in laboratory studies. Clinical trials are ongoing to evaluate the effectiveness of these antiviral agents in treating MERS.
Supportive Care
Treatment for MERS primarily involves supportive care aimed at relieving symptoms and managing complications. This may include oxygen therapy, intravenous fluids, and the use of ventilators for severe respiratory distress. Prompt medical attention and comprehensive care are crucial in improving patient outcomes.
Infection Control Measures
Preventing the transmission of MERS-CoV in healthcare settings requires strict adherence to infection control measures. This includes proper hand hygiene, wearing personal protective equipment (e.g., masks, gloves, gowns), and implementing respiratory hygiene and cough etiquette. Isolation of suspected cases and appropriate disinfection of surfaces are also important in reducing the risk of transmission.
Global Epidemiology of Middle East Respiratory Syndrome
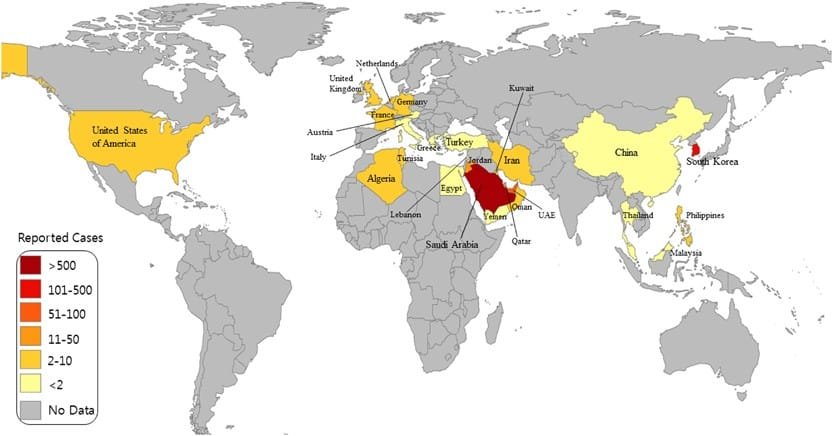
Countries Affected
As of [date], MERS cases have been reported in [number] countries across the Middle East and beyond. The majority of cases are concentrated in Saudi Arabia, where the virus was first identified. Other countries in the region, including [list countries], have also reported cases, often linked to travel or contact with infected individuals.
Case Fatality Rate
The case fatality rate for MERS varies depending on several factors, including the quality of healthcare and the underlying health of the individual. On average, the mortality rate is estimated to be around 35%, but this can range from 20% to 40% in different outbreaks. Prompt diagnosis, appropriate treatment, and supportive care are crucial in reducing the risk of fatal outcomes.
Trends in Infections
Since its emergence, MERS has demonstrated sporadic outbreaks with a relatively low incidence compared to other respiratory viruses such as SARS-CoV and the coronavirus causing COVID-19. While the overall number of cases remains relatively low, vigilance and surveillance are still necessary to detect and contain new outbreaks promptly.
Public Health Response to Middle East Respiratory Syndrome
Surveillance and Reporting
Surveillance systems play a critical role in monitoring the spread of MERS and identifying new cases. Health authorities in affected countries, as well as international organizations like the WHO, collaborate to collect and analyze data on MERS cases and outbreaks. This information is essential for guiding public health strategies and interventions.
Quarantine and Isolation
Quarantine and isolation measures are employed to prevent the spread of MERS. Suspected cases are isolated and tested, while close contacts are placed under quarantine to monitor for symptoms. These measures help contain the virus and prevent further transmission within communities and healthcare settings.
Research and Vaccine Development
Research efforts are ongoing to better understand the epidemiology, transmission dynamics, and clinical aspects of MERS. This includes studying the genetic makeup of the virus, conducting clinical trials for potential treatments, and developing vaccines. While no licensed vaccine is currently available, promising candidates are being evaluated for their safety and efficacy.
Comparisons with Other Coronavirus Outbreaks
SARS-CoV
MERS-CoV shares several similarities with SARS-CoV, which caused the Severe Acute Respiratory Syndrome (SARS) outbreak in 2002-2003. Both viruses are zoonotic in origin, with bats identified as the primary reservoirs. They also exhibit respiratory symptoms and can lead to severe complications. However, MERS has a higher case fatality rate compared to SARS.
COVID-19
COVID-19, caused by the coronavirus SARS-CoV-2, is another respiratory illness that has caused a global pandemic. While both MERS and COVID-19 belong to the same family of viruses, their transmission dynamics and clinical presentations differ. COVID-19 has a higher transmission rate but a lower case fatality rate compared to MERS. The impact of COVID-19 on global health and economies has been far-reaching.
Lessons Learned
The outbreaks of MERS, SARS, and COVID-19 have highlighted the need for robust surveillance systems, rapid response mechanisms, and global cooperation in managing emerging infectious diseases. Lessons learned from previous outbreaks, such as the importance of infection control measures and research collaborations, can inform future preparedness and response efforts to mitigate the impact of similar viruses.